People who are newly diagnosed with Hashimoto’s are often confused about the symptoms they are experiencing. Personally, I was shocked to have been diagnosed with hypothyroidism and not hyperthyroidism. I was thin, anxious, irritable, and had heart palpitations in addition to feeling cold, forgetful, and tired — all symptoms that are typically associated with hyperthyroidism.
What I didn’t know at the time, is that 90-97 percent of cases of hypothyroidism are caused by Hashimoto’s, an autoimmune attack on the thyroid — and Hashimoto’s has a unique set of symptoms compared to non-autoimmune hypothyroidism.
I’ve come to understand that Hashimoto’s can look very different from person to person. No two people will present with the exact same list of symptoms, and some people have more mild versions, while others can be completely debilitated. I have witnessed people with uncontrolled Hashimoto’s who can work an 80 hour week, run a household, become elite body builders, and/or run marathons, while others can barely drag themselves out of bed in the morning.
Hashimoto’s and its symptoms cover a broad spectrum — and in this article, I’d like to bring awareness to how different the condition can look from person to person. We’ll discuss:
- The differences between hypo- and hyperthyroidism
- Symptoms associated with Hashimoto’s
- Common root causes
- Steps you can take to address your root causes today
Do you Swing Back and Forth from Hypothyroidism to Hyperthyroidism?
The thyroid gland is an important endocrine organ that produces hormones to regulate our metabolism. When the thyroid is not functioning properly, there may be an excess or lack of thyroid hormone production, which can lead to hyper or hypothyroidism, respectively.
Hyperthyroidism is characterized by an overactive thyroid gland that produces and releases an excess of thyroid hormone into the body. It is often caused by hyperfunctioning (overactive) thyroid nodules, an attack on the immune system (as is the case in the autoimmune condition Graves’ disease), a viral infection, or the consumption of foods or medications that contain high levels of iodine.
Conversely, hypothyroidism is associated with a lack of thyroid hormone that can occur as a result of a variety of different factors (including iodine deficiency, surgical removal of the thyroid, or damage to the thyroid).
Symptoms of Hyperthyroidism
Hyperthyroidism, or an overabundance of thyroid hormone, has a stimulatory effect. Classical symptoms include:
- Weight loss
- Palpitations
- Anxiety
- Eye bulging
- Tremors
- Irritability
- Infrequent menstrual periods
- Fatigue
- Heat intolerance
- Increased appetite
- Hair loss
- Enlarged thyroid gland
- Sweating
- Frequent bowel movements
- Infertility
- Soft nails
- Warm, moist palms
- Finger tremors
- Insomnia
- Muscle weakness
- Nervousness
Symptoms of Hypothyroidism
Some of the more common symptoms of hypothyroidism, or deficiency of thyroid hormone, include:
- Slower metabolism leading to weight gain
- Forgetfulness
- Feeling cold or cold intolerance
- Depression
- Fatigue
- Dry skin
- Constipation
- Loss of ambition
- Dry, coarse hair
- Muscle cramps
- Stiffness
- Joint pain
- A loss of the outer third eyebrow
- Heavy menstrual periods
- Infertility
- Muscle aches
- Puffy face
- Slow heartbeat
- Brittle nails
- Arthritis
These symptoms may be present in any combination in people with thyroid disorders, but the degree to which they impact an individual can vary greatly as well. For example, one person with hypothyroidism may find themselves putting on a great deal of weight, despite eating a healthy diet and exercising regularly, while another person may stay within a normal weight range most of the time, with minimal effort. Additionally, the symptoms a person experiences can change, disappear, and reappear over time.
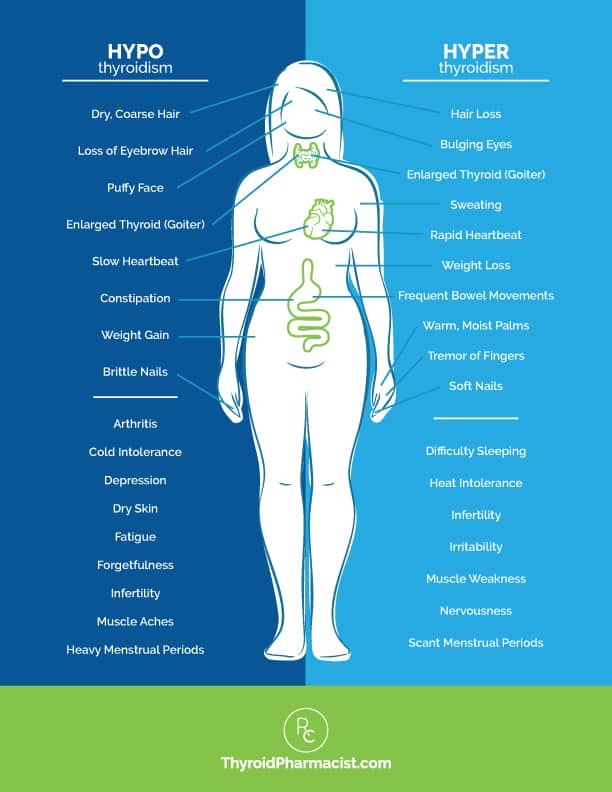
Hashimoto’s Symptoms
If you’re reading this, you’re likely thinking, what about Hashimoto’s?
Hashimoto’s is an autoimmune condition that results in the immune system damaging the thyroid, which leads to a lack of thyroid hormone production. Most cases of hypothyroidism in the United States, and other countries that add iodine to their salt supply, are caused by Hashimoto’s.
While Hashimoto’s is the leading cause of hypothyroidism, there is a difference between Hashimoto’s and hypothyroidism. A person can have one, and not the other.
Most cases of pure hypothyroidism can be remedied by taking thyroid hormones. However, given that 97 percent of cases of hypothyroidism are due to advanced Hashimoto’s, people will still have Hashimoto’s and the autoimmune attack will remain, even when proper levels of thyroid hormone are restored with medications, unless we find and treat the root cause of the autoimmune attack.
People with Hashimoto’s may experience BOTH hypothyroid and hyperthyroid symptoms because, as the thyroid cells are destroyed, stored hormones are released into circulation, causing a toxic level of thyroid hormone in the body. This is known as thyrotoxicosis, or Hashitoxicosis. Eventually, the stored thyroid hormones may become depleted, and due to thyroid cell damage, the body may no longer be able to produce enough hormones. This is when hypothyroidism develops.
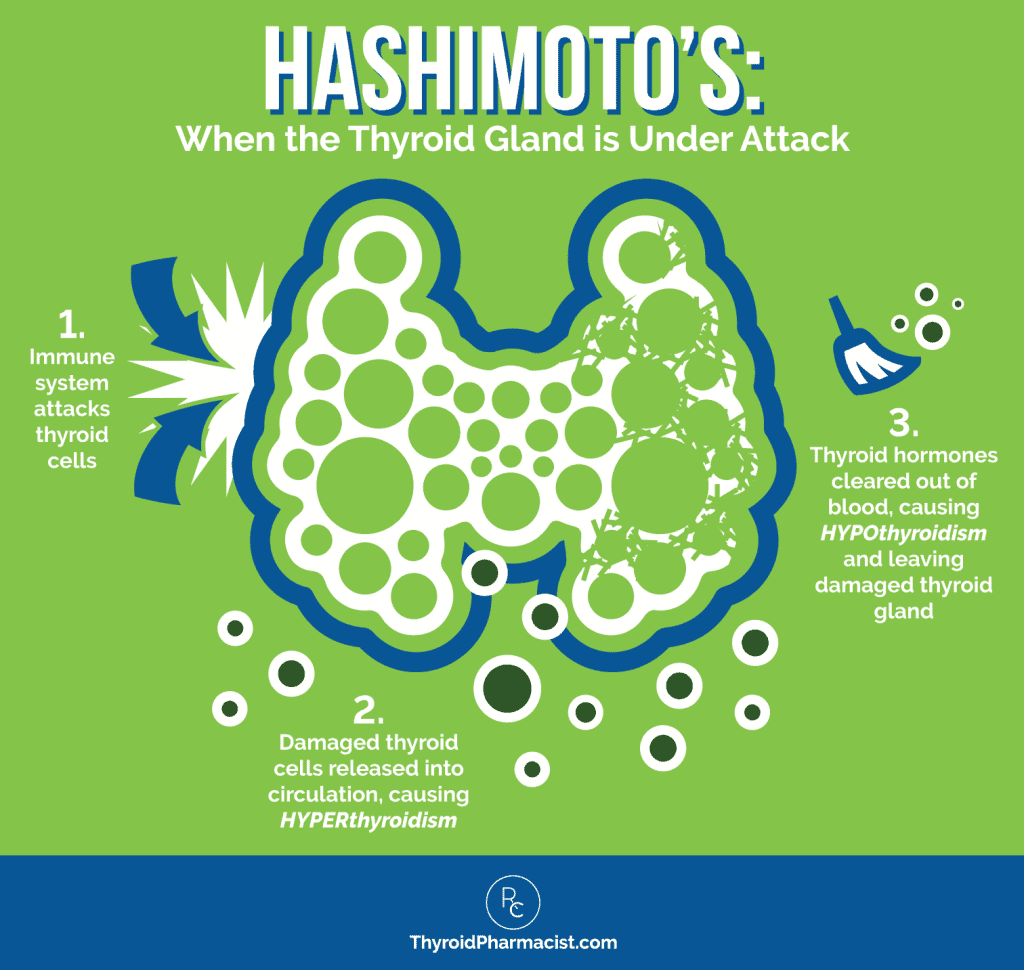
This explains why we see both symptoms of hyper- and hypothyroidism in people with Hashimoto’s, in addition to a few symptoms that are typical of Hashimoto’s — especially those related to gastrointestinal distress, like irritable bowel syndrome (IBS), acid reflux (GERD), diarrhea, constipation, and bloating.
It also explains why the condition can look so different from person to person, as the symptoms are broad and frequently shifting.
In addition to many of the symptoms we frequently see associated with hyper- and hypothyroidism, Hashimoto’s commonly presents with:
- Anxiety
- Depression
- Weight gain
- Mood swings
- Fatigue
- Brain fog
- Cold hands and feet
- Gastrointestinal issues
- Food sensitivities
I personally experienced irritable bowel syndrome (IBS), anxiety, and advanced carpal tunnel in both hands, which required me to wear wrist braces. Despite my symptoms, however, I looked fine (except for some bloating). I had hair on my head (despite losing much of it) and I didn’t need crutches (although I experienced leg and muscle pain). When I came home from work, all I could do was eat, watch TV, and fall asleep on the couch. I was living proof that thyroid symptoms may affect someone, even though they may look fine on the outside!
Some of these symptoms may have been directly related to insufficient thyroid hormone. Others may have been due to related issues (i.e. gut infections), which are seen in many people with Hashimoto’s. That’s why it’s important to identify the root causes of YOUR Hashimoto’s, so you can take the first steps toward healing!
Identifying and Addressing Your Root Cause(s)
Most doctors dismiss autoimmune conditions as the result of certain genes and believe that once present, they cannot be reversed. However, leading pediatric gastroenterologist and researcher, Dr. Fasano, has proven otherwise. He has come up with a concept which he calls the “three-legged stool of autoimmunity.”
According to his research, three factors need to be present for an autoimmune condition to develop:
- A genetic predisposition
- An external trigger
- Intestinal permeability, also known as leaky gut (a condition that involves “holes” in the intestinal lining, which allows toxins and food particles to pass through and further damage our gut)
Dr. Fasano found that, upon removing the intestinal permeability and/or trigger, an autoimmune condition will go into remission. For this reason, I believe in addressing the root causes of Hashimoto’s symptoms to reverse the condition. (And yes, remission is possible with Hashimoto’s!)
Those with Hashimoto’s often share similar triggers and root causes. Though the list of potential triggers is long, the ones we see the most often are:
1. Food sensitivities: The most common food sensitivities found in people with Hashimoto’s are gluten, dairy, soy, grains, nightshades (potatoes, tomatoes, and peppers), nuts, and seeds. When someone is first setting out to change their diet, I always recommend removing gluten, dairy, and soy.
In surveying my readers and clients, I’ve found that about 93 percent have felt better on a gluten-free diet. Another 75 percent reported feeling better on a dairy-free diet, 73 percent felt better grain-free, and another 60 percent said they felt better soy-free. Egg and nightshade-free diets were helpful 40 percent and 35 percent of the time, respectively. One of the easiest ways to begin identifying your own food sensitivities is with an elimination diet. You can also read my article about food sensitivities for more information to help you get started.
2. Nutrient depletions: Micronutrient deficiencies are common in people with Hashimoto’s. This could be due to a lack of sufficient thyroid hormones, as such a state makes nutrient extraction from food more difficult and less efficient. Nutrient deficiencies can also occur as a result of eating nutrient-poor foods, following a calorie-restricted diet, having inflammation from infections or food sensitivities, taking certain medications, or having an imbalance of gut bacteria.
These nutrient deficiencies contribute to the development of Hashimoto’s, as well as many of its symptoms. Restoring one’s nutrient levels through nutrient-dense foods, supplementation, and optimizing digestion, are some of the fastest ways to feel better with Hashimoto’s!
3. Impaired stress response: Stress affects so many different bodily functions, including metabolism, hormone production, immune system regulation, and emotional response. It can also decrease thyroid function, as the body attempts to preserve energy to deal with whatever issue is at hand — whether you are being chased by a bear or stuck in traffic. The adrenal glands cannot decipher what is happening when in a “fight or flight” response, so it reacts the same way. “Fight or flight” mode can save us from danger and help us tackle the challenging situations in life.
However, problems arise when this type of stress is ongoing and the body is constantly suppressing thyroid function to preserve its resources. Additionally, high or low cortisol levels, caused by chronic stress to the adrenal glands, can cause hypoglycemia (low blood sugar) and hyperglycemia (high blood sugar).
If left unmanaged, these blood sugar imbalances can lead to hypothyroid symptoms. An increase in cortisol will also disrupt the balance of the HPT (hypothalamic-pituitary-thyroid) axis, which the body relies on to keep thyroid levels steady.
You can begin incorporating a few simple steps to reduce your stress load, such as making time for self-care (massage is a favorite option!), taking a yoga class, or beginning a daily meditation practice.
My article on adrenal fatigue has more ideas for lowering your stress levels and supporting your adrenals.
4. Toxins: It can be nearly impossible to escape from toxins because they are everywhere — cosmetics, skin products, pesticides, exhaust fumes — whatever we inhale, ingest, and absorb into our skin eventually ends up circulating in our body. In fact, in 2006, the Centers for Disease Control reported that the average American has 116 out of 148 commonly used synthetic compounds in their body!
We are frequently exposed to xenoestrogens (found in BPA, soy, phthalates, parabens, etc.), which may increase TSH and perpetuate the autoimmune attack on the thyroid. Other toxins such as triclosan (recently banned by the FDA and found in antibacterial soap, toothpaste, deodorant, hair spray, and many other personal care products) have structures that can resemble the thyroid and have been found to cause thyroid toxicity.
There are also toxins called halogens (i.e. bromide, chloride, and fluoride), which can compete with receptor sites in the thyroid gland and build up in our thyroid tissue, leading to inflammation and thyroid cell death. Fluoride, in particular, can wreak havoc on the thyroid and is included in an array of products — bottled beverages, toothpaste, black and red tea, canned foods, certain medications, and even our drinking (tap) water!
You can begin reducing your toxic exposure by replacing personal care products with safer choices, and installing a home water filtration system to eliminate harmful chemicals from your drinking water. To learn more about reducing your toxic burden, please read my article on liver support.
5. Bacterial, fungal and parasitic infections: Chronic infections (such as small intestinal bacterial overgrowth (SIBO), Blastocystis hominis, Candida overgrowth, and H.pylori) have all been identified as triggers of Hashimoto’s, and identifying and treating them can result in complete remission. In 2015, 80 percent of my clients who hit a plateau with nutrition and took the gut tests I recommended, tested positive for at least one gut infection. If you feel you have also hit a wall and feel that an underlying infection might be your root cause, I encourage you to read more about Hashimoto’s and infections to learn how to eradicate them once and for all.
6. Leaky gut: As I mentioned earlier, intestinal permeability (leaky gut) is one of the factors that must be present for autoimmunity to occur. A leaky gut has gaps in the gut lining that allow irritating molecules and substances to escape from the digestive system and enter into the bloodstream. In a leaky gut, infections, viruses, and food particles that find their way into the body through the intestinal wall can cause food sensitivities and a host of other symptoms.
This irritation can interrupt the immune system’s ability to regulate itself and put the body into a perpetual “attack mode” that is counterproductive to healing. Even those who have no apparent gastrointestinal symptoms may have a leaky gut, and addressing gut function might be the best place to start to bring healing to the body. If we can reverse leaky gut, we can prevent or reverse autoimmunity altogether.
While there are many possible root causes of Hashimoto’s, everyone’s will be different. Some people may just have one or two, while others may have a combination of food sensitivities, underlying infections, nutrient depletions, and more.
You can read more about the top root causes of Hashimoto’s, and the dietary and lifestyle interventions that I recommend to address them, in this article. You can also check out my article on the conventional versus Root Cause approach to dig for your own root cause(s). I also recommend finding a functional medicine practitioner who can help guide you on your health journey.
The Takeaway
Through my own journey with Hashimoto’s, I have learned that this condition has many different faces and will, therefore, require an individualized approach for each person.
In my own case, the symptoms of acid reflux, bloating, and IBS that I experienced, were my first clues to the connection between gut health and autoimmunity — which set me on the path to healing my gut through the use of food and other lifestyle interventions.
You will need to dig to find your own root cause(s), but identifying food sensitivities, addressing nutrient depletions, removing toxins, supporting adrenal health, testing for infections, and healing a leaky gut are the most common areas that people with Hashimoto’s will need to address on their journey to healing. And now I have made it my mission to help you get there!
Because I know that this journey can feel overwhelming at times, I wrote my book Hashimoto’s Protocol to offer a clear, step-by-step path to identify your own root cause(s) and heal your own symptoms. I also created my own cookbook, full of delicious and easy recipes to support you on your path to healing using the power of nutrition.
You can pick up a copy of Hashimoto’s Food Pharmacology: Nutrition Protocols and Healing Recipes to Take Charge of Your Thyroid Health to help heal your gut and feel better today!
What has Hashimoto’s looked like for you? I’d love to hear your success stories — please share them in the comments below!
You can also download a free Thyroid Diet Guide, 10 thyroid-friendly recipes, and the Nutrient Depletions and Digestion chapter by signing up for my weekly newsletter. You will also receive occasional updates about new research, resources, giveaways, and helpful information.
For future updates, make sure to follow us on Facebook and Instagram!
Note: Originally published in October 2016, this article has been revised and updated for accuracy and thoroughness.


 Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Hi, I had my Thyroid checked 7years ago and my TSH was very low 0.07 and my T3 and T4 were on the high side but I did’t do anything about it just thought it was a fluke thing cuz I never had issues with my Thyroid before. I am going to see an Endo in October just to get it checked. I do have a lot of both hypo/hyper symtoms. Should I be concerned???
Norma – thank you for reaching out and sharing your journey here. <3 Did you know that if you live in the United States, Australia, Europe and most developed countries that add iodine to the salt supply and take thyroid medications, there’s a higher probability that you do have Hashimoto’s?Depending on the source, estimates are that between 90-95% of those with hypothyroidism have Hashimoto’s.But most doctors will never tell people that they have Hashimoto’s, or that their own immune system is attacking their thyroid. People are told that their “thyroid is sluggish,” and that these things happen with age and “Just take this pill, you’ll be fine.” I hope you check out these articles that I wrote.
ARE YOU DOING EVERYTHING FOR YOUR THYROID BUT NOT YET WELL?
https://thyroidpharmacist.com/articles/are-you-doing-everything-for-your-thyroid-but-not-yet-well/
DO YOU HAVE HYPOTHYROIDISM OR HASHIMOTO’S OR BOTH?
https://thyroidpharmacist.com/articles/do-you-have-hypothyroidism-or-hashimotos-or-both/Here are the tests you need for diagnosis.
Most endocrinologists don’t run them all, so you will have to request them. Make sure to request a copy of your labs as well.
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
It’s so crazy that you mentioned your symptoms, and THANK YOU FOR THAT! I have been going crazy wondering what’s wrong with me, I have the same symptoms: weight loss, hair loss, EXTREME fatigue and being cold to my core, as well as anxiety, and irregular cycles. I was told, at my one appointment with an Endo, that one side of my Thyroid was not producing hormones and to come back if I were still feeling poorly another treatment I had to go through…needless to say, I feel so bad some days I just want to cry, physically feeling poorly had led to my emotionally feeling poorly. It’s depressing when you don’t have the energy to do the things you love…and no one understands why because you LOOK fine. ?
Rachel – you are very welcome! <3 I'm so sorry you are struggling with all of this! You are not alone! I do suggest that you join one of the Hashimoto’s groups that are out there. Being able to share ideas of what has worked with one another and offer support for each other can be very helpful. A couple of years after my diagnosis, I found Hashimoto’s 411, a closed Facebook group run by Alice Berry McDonnell. This group is amazing! It is comprised of an army of highly motivated, smart, supportive women and men (now 50,000+ strong), and each of them sharing ideas of what worked for them, things they were planning to try, and offering support to one another.
https://www.facebook.com/groups/hashimotos411/
I have been diagnosed with Hashimotos for about 5.5 yrs. About 2.5 yrs ago I received the pneumovax 23 vaccine and had a terrible reaction.
I was confused because my initial symptoms were those of hyperthyroidism. But nothing ever showed up in my blood work and yet my symptoms were horrendous. My Endocrinologist was very little help during that time since my thyroid blood work appeared normal, (felt very abandoned), not sure if she checked my antibodies. Is it common for the thyroid levels to not show a major flare? Or could this have been something unrelated? The only problem is that I have experienced these same cluster of symptoms as flares through the years but it was exponentially worse after the vaccine. Your explanation of what happens when the thyroid gland is initially attacked makes a lot of sense as to what may have happened to me. But curious about the blood work.
I have been working with a functional medicine doctor and am doing much better, but it has taken 2.5 years with no major explanations of what happened to me.
Thanks for all that you do for the Hashimotos community, it was partly you and your book that gave me hope during a very dark time.
Janet – thank you so much for sharing your journey. <3 I'm so happy to hear you have found a practitioner and are feeling much better. <3 I hope you will continue to keep me posted on your progress.
Dr.wentz
I have Hashimoto’s. I experience hyper and hypo constantly. My antibodies was a 900 and my T3 free Was a little high but everything else was normal my other antibodies I believe was the three which it was high also. Do you have any recommendations?
Sharon – thank you for reaching out. Graves and Hashimoto’s are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto’s, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people)-Hashimoto’s results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually, people with Graves have hyperthyroidism, and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own, and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. Here are the links to my books:
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Wendy- There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
Brenda- Here is an article you may find interesting! 🙂
THE COMMON ROOT CAUSE OF HASHIMOTO’S, HIVES AND IBS
https://thyroidpharmacist.com/articles/the-common-root-cause-of-hashimotos-hives-and-ibs
Dr. Wentz,
I wish so bad that YOU were my doctor. I’ve learned more from your books and online works than I’ve learned from any of the doctors I’ve seen over the last 7 months when my symptoms first started. I initially had a tsh of 23.67. I was put on levothyroxine and gradually increased to 100 McG that I’m on now. I’m trying to focus on my gut health and mental health as well. I have Hashimoto’s and a lot of those standard hypothyroid symptoms, weight gain, hair loss, fatigue, GI issues. But my main problem remains heart palpitations that occur completely out of the blue and result in bad chest pain. These started only in the middle of the night but they now come on as they please, day or night. I am desperate for help. I’ve been to the ER four times in the last seven months convinced that I’m having a heart attack but all heart tests come back negative. I’m afraid these heart palpitations, beating over 100 BPM, may eventually cause real damage to my heart. Do you have any suggestions for how to treat this symptom? As it appears I’m clearly a person suffering from both hyperthyroid and hypothyroid symptoms. Any advice you have for these terrible heart palpitations would be so greatly appreciated.
Emily – thank you for following! I’m so happy to hear you are finding my books and research helpful! ❤️ Palpitations might be due to food sensitivities, as it is a common reaction associated with eating foods that one is reactive to. Doing an elimination diet would help you figure out which foods you are sensitive to, and eliminating those foods could cause your palpitations to stop. Other possible causes of palpitations include caffeine consumption, caffeine withdrawals, being overmedicated, and having high thyroid antibodies. Supplementing with selenium helps many people in the case of high thyroid antibodies. I recommend consulting with your practitioner to discuss your symptoms and possible underlying nutrient deficiencies that may be behind your palpitations. Here are a couple articles you might find helpful:
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos/
MEDICATIONS FOR HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/medications-for-hashimotos-and-hypothyroidism/
Hi. I have been on synthroid for 17 yrs. Recently, we have discovered a growth on my thyroid. It is growing very quickly. I have had numerous biopsies with non-cancerous results. 2 weeks ago my doctor took me off synthroid because my thyroid is now making too much thyroid hormone. It is better to just have my thyroid and tumor removed? I asl because 12 yrs ago my husband had papilllay carcinoma and his entire thuroid was removed and he managed really well.
Vanessa – thank you for following this page. Nodules and goiters are often the result of toxicity and/or the autoimmune process. So, doing interventions to reduce the autoimmune attack on the thyroid, and toxicity, can be helpful to reduce them. Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
It worked….never saw the rash again. What also worked for a mile was Dr Scholls athlete foot cream as it kills the fungus in the rash…..but the herbs and diet removed it permenantly.
Denny- Thank you so much for sharing! You may find this article interesting! 🙂
CANDIDA AND HASHIMOTOS CONNECTION
https://thyroidpharmacist.com/articles/candida-and-hashimotos-connection
PLEASE HELP!
Cori- You may like to check out the doctors that other patients recommend on this list:
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
Sara- I personally struggled with pain in the form of body aches and stiffness as well as carpal tunnel in both arms in 2010, when I was first diagnosed with Hashimoto’s. It was awful, I had to wear braces on both arms all day and even at night for about 6 months.
I took NSAIDs every day to deal with the pain so I could get through my workday.
I hope these articles help you get started.
PAIN AND HASHIMOTOS
https://thyroidpharmacist.com/articles/pain-and-hashimotos
PAIN HASHIMOTOS AND FIBROMYALGIA…
https://thyroidpharmacist.com/articles/pain-hashimotos-and-fibromyalgia/
TURMERIC FOR YOUR THYROID AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/turmeric-for-your-thyroid-and-hashimotos
Jean- There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
Lynn- Graves and Hashimoto’s are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto’s, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people)-Hashimoto’s results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually people with Graves have hyperthyroidism and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research in journey for overcoming my autoimmune thyroid condition.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
So, I have some questions. Is it right to treat hashitoxicosis as if it was regular hyperthyroidism, as far as medication is concerned? Do the same things apply concerning nutrition as in hashimoto hypo? Will changing my diet to the autoimmune protocol help save my thyroid before I go hypo? Also, I read that exposure to high tsh causes goiter, am i at risk or it had to be more than a couple months to cause me a problem? Should i always ask for a full check (including antibodies) or is it ok to check them once a year? Thank you for all the info!It will help my family understand a bit more about hashimoto’s and why I have these “inexplicable” mood changes.
Sofia- Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. Thyroid tissue can regenerate, but the rate at which it does is not always predictable. Thus, some are able to stop the autoimmune attack on their thyroid and regain normal thyroid function. Others can reduce the dose of medications, and others will need to stay on the medications indefinitely. I’m currently working on some protocols to help with tissue regeneration.
Reversing Hashimoto’s means different things to different people. For some, it means a reduction in symptoms and for others it means a reduction in your antibodies. I had both. Here a few articles that might be helpful for you 🙂
IS IT POSSIBLE TO RECOVER THYROID FUNCTION IN HASHIMOTO’S
https://thyroidpharmacist.com/articles/is-it-possible-to-recover-thyroid-function-in-hashimotos
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
I have been over weight since my thyroid was removed , I feel like some of my systems of RA, SS and thyroid are all the same . I would love to have the T3 test done,my Dr. Will not do it
Carol- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
April- Most conventional physicians use the TSH test to determine if one has a thyroid disorder and to dose thyroid medications.
However, this test can often times be misleading, as levels of circulating hormones may fluctuate at different times, such as in Hashimoto’s, the person affected may fluctuate between highs and lows.
Additionally, when scientists first set the “normal” ranges of TSH for healthy individuals, they inadvertently included elderly patients and others with compromised thyroid function in the calculations leading to an overly lax reference range.
This resulted in people with underactive thyroid hormones being told that their thyroid tests were “normal,” based on this skewed reference range.
WHAT TO DO IF YOUR TSH IS NORMAL AND YOU ARE ANYTHING BUT
https://thyroidpharmacist.com/articles/what-to-do-if-your-tsh-is-normal-and-you-are-anything-but
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well.
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests
Tasha- Here is an article you may find interesting! 🙂
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
Please help !
Dana- There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
Zola- Here is an article you may find interesting! 🙂
LYME AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/lyme-and-hashimotos
Karen- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Terri- There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
A little worried about this situation
Rebecca- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Tanya- These are the recommended labs from my book, page 32.
RECOMMENDED THYROID FUNCTION TESTS
TSH
TPO Antibodies
Thyroglobulin Antibodies
Free T4
Free T3
Reverse T3 (Optional)
Have you read my book, Hashimoto’s The Root Cause? Here’s the link in case you’re interested.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20

HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications
Jennifer- These are the recommended labs from my book, page 32.
RECOMMENDED THYROID FUNCTION TESTS
TSH
TPO Antibodies
Thyroglobulin Antibodies
Free T4
Free T3
Reverse T3 (Optional)
Have you read my book, Hashimoto’s The Root Cause? Here’s the link in case you’re interested.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20

HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications
All my antibodies are normal but i am feeling all the syptoms of hasimotos, heart palaps bowl problems, etc . My Tsh was at a 9.5 intailly, then moved to .5. I have reduced my medication from 50 mcg to 25 to 25 every other day. Is my thyroid healing?
Akshay – Thank you for following this page and sharing your journey. Please, understand that due to liability issues, I am unable to answer specific medical questions, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms. Here are some links which might help:
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
MY RECENT CHALLENGES AND FINDING DR. RIGHT
https://thyroidpharmacist.com/articles/my-challenges-and-finding-dr-right/
Sonya- Conventional cosmetics, potions and lotions are filled with petroleum by-products, phthalates, formaldehyde, hormone disruptors and other toxins, and as a pharmacologist, I can tell you that what you put on your skin definitely gets absorbed into your body! Here is an article you may find interesting! 🙂
ARE YOU SACRIFICING YOUR HEALTH FOR EXTERNAL BEAUTY?
https://thyroidpharmacist.com/articles/are-you-sacrificing-your-health-for-external-beauty
E- You may be interested in checking out the Root Cause Recipe Portal. It is full of autoimmune paleo and paleo recipes. You’re able to organize weekly shopping lists, meal planning, etc. Hope you check it out.
http://rootcauserecipes.com/
Carolyn- Thank you so much for sharing! Here is an article you may find interesting as well! 🙂
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
Sonya- Thank you for sharing! Here is an article you may find interesting! 🙂
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
Candelaria- Thank you so much for sharing! Here is an article you may find interesting! 🙂
WHY THYROID PATIENTS NEED CHANGE
https://thyroidpharmacist.com/articles/why-thyroid-patients-need-change
Amber- Most conventional physicians use the TSH test to determine if one has a thyroid disorder and to dose thyroid medications.
However, this test can often times be misleading, as levels of circulating hormones may fluctuate at different times, such as in Hashimoto’s, the person affected may fluctuate between highs and lows.
Additionally, when scientists first set the “normal” ranges of TSH for healthy individuals, they inadvertently included elderly patients and others with compromised thyroid function in the calculations leading to an overly lax reference range.
This resulted in people with underactive thyroid hormones being told that their thyroid tests were “normal,” based on this skewed reference range.
WHAT TO DO IF YOUR TSH IS NORMAL AND YOU ARE ANYTHING BUT
https://thyroidpharmacist.com/articles/what-to-do-if-your-tsh-is-normal-and-you-are-anything-but
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well.
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests
Rosa- Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
Risa- Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
Theresa- Here is an article you may find interesting! 🙂
ARE YOUR ADRENALS SABOTAGING YOUR HEALTH?
https://thyroidpharmacist.com/articles/are-your-adrenals-sabotaging-your-health
Cheryl- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Emily- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Mary- Did you know that if you live in the United States, the UK, Australia, Europe and most developed countries that add iodine to the salt supply and take thyroid medications, there’s a higher probability that you do have Hashimoto’s?
Depending on the source, estimates are that between 90-95% of those with hypothyroidism have Hashimoto’s.
But most doctors will never tell people that they have Hashimoto’s, or that their own immune system is attacking their thyroid. People are told that their “thyroid is sluggish”, and that these things happen with age and “Just take this pill, you’ll be fine.” I hope you check out these articles that I wrote.
ARE YOU DOING EVERYTHING FOR YOUR THYROID BUT NOT YET WELL?
https://thyroidpharmacist.com/articles/are-you-doing-everything-for-your-thyroid-but-not-yet-well
DO YOU HAVE HYPOTHYROIDISM OR HASHIMOTO’S OR BOTH?
https://thyroidpharmacist.com/articles/do-you-have-hypothyroidism-or-hashimotos-or-both/
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well.
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests
Roxanne- There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
Rebecca- These are the recommended labs from my book, page 32.
RECOMMENDED THYROID FUNCTION TESTS
TSH
TPO Antibodies
Thyroglobulin Antibodies
Free T4
Free T3
Reverse T3 (Optional)
Have you read my book, Hashimoto’s The Root Cause? Here’s the link in case you’re interested.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20

HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications
Chrissie- Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year/
Lisa- Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year/
Leonie- Here is an article you may find interesting! 🙂
INFECTIONS AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/infections-and-hashimotos
I was diagnosed with Hashimoto’s when I was 20 and have been on Synthroid since. I’m positive for antibodies and have two nodules. I also have been diagnosed with anxiety, depression, and ADHD and take medications to control everything. Lately I’ve noticed I can’t handle my alcohol intake, now at age 33, then I have in the past. I used to be able to drink 8 beers and be fine. Now, I have 4 beers and I blackout and have the worst hangover for 2 days. Is there a correlation between thyroid function levels and alcohol?
Elizabeth- Coffee, alcohol, and tea (except for herbal tea) may need to be avoided. Caffeine stimulates ACTH, which in turn stimulates the adrenals and cortisol production. You may find this article interesting! 🙂
ARE YOUR ADRENALS SABOTAGING YOUR HEALTH?
https://thyroidpharmacist.com/articles/are-your-adrenals-sabotaging-your-health
OH MY so I have gone from TSH from being 10.3 to 1.79 to my now 0.019. Seriously this yoyo ride has got to stop. SO now what. I see my doctor tomorrow. So tired of being this way. So very tried.
Sophie – thank you for following this page. 🙂
Dealing with Hashimoto’s is certainly frustrating, and my heart goes out to you. <3
Please, understand that due to liability issues, I am unable to answer specific medical questions.
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
I have no thyroid, ever since my hysterectomy my body will not balance thyroid hormones. I’m either really or really high or really low just can not attain a balance which is driving me nuts emotionally and physically. We have tried gluten free diet and medication change and nothing has worked any advice would be greatly appreciate.
Monica – thank you for following this page. My heart goes out to you. <3
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead,' or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
IS HASHIMOTO’S A SURGICAL DISEASE
https://thyroidpharmacist.com/articles/is-hashimotos-a-surgical-disease
so interesting that we can be both. I fit more signs of hyper but I’m far from the standard “thin” that most people think of as being hyper. As I learn more I almost want to throw up my hands and give up.
Carol – thank you for following this page.
Graves and Hashimoto’s are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto’s, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people)-Hashimoto’s results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually, people with Graves have hyperthyroidism, and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own, and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Dr Izabella I hope you can help. There is a lot of information coming and all very confusing. I seem to be a “medical mystery” but I can’t believe I am alone in this. When I initially went to an endo he ran all of the tests including uptake and another I can’t think of. TSH was non existent, free t4 2.84, free t3 7.9, TSI 370, TPO 55.5, Anti TG 188. I was diagnosed with Graves. Of course the Dr wanted to put me on meds to slow my thyroid but since I also had high anti-bodies for hashi, had symptoms of hyper and hypo, and I was in the process of watching your video series that didn’t sit with me. I went GF and started looking for an integrative DR. I did find one and they put me on LDN. This Dr took baseline blood work again and I was thrilled to see that my TSI was NORMAL just from being gf and even before taking the LDN. Other antibodies were still high so I started the LDN. After a month my antibodies, T4 and T4 are MUCH higher and TSH is still non-existent. t4 3.46, t3 8.7, TSI <89, TPO 262.1, Anti TG 616. I have symptoms of hyper (heart palps, heat intolerance) and hypo (constipation, weight gain, brittle hair and nails). I am at a loss of where to go for help now. The integrative dr said I am hyper but have hashi antibodies. I was surprised when I was told that they couldn't help me an that I need to go back to an endo. I don't understand why TSI is normal but everything else in elevated esp while taking LDN. Also don't understand how my thyroid is throwing out so many hormones yet have such high hashi anti-bodies. I am in the suburbs of Chicago and noticed a lot of you series was filmed here. Can you help me understand this and/or can you direct me to someone who can help?
Thank you,
Kim
Kim – thank you for following this page. I’m sorry to hear that you are struggling! 🙁
Graves and Hashimoto’s are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto’s, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people)-Hashimoto’s results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually, people with Graves have hyperthyroidism, and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own, and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hi Dr Izabella
I have been diagnosed hypotthyroid since 2009 and on thyroxine since then but have always had fluctuating but usually worsening TSH levels even as my dose has gradually increased over that time. Anti TPO results have come back clear though this has not been tested for a few years. Last year anti-thyroglobulin came back 252. The endo asked for this test. My doctor says it is not relevant and only TPO levels should be checked for Hashimotos. Could this result alone indicate hashimotos?
Carrie – thank you for following this page. These are the recommended labs from my book, page 32.
RECOMMENDED THYROID FUNCTION TESTS
TSH
TPO Antibodies
Thyroglobulin Antibodies
Free T4
Free T3
Reverse T3 (Optional)
Have you read my book, Hashimoto’s The Root Cause? Here’s the link in case you’re interested.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20

HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications
Hello and thank you for your expertise. I recently was tested with a TSH of 55-yes that is correct. With a thyroid underfunctioning to that degree I have gained no weight. Can anyone suggest why? I do fatigue very easily but no other hypo symptoms. My present med is a dessicated thyroid that I take sublingually so I would think most of the med is utilized in my body. Thanks
Stan – thank you for following this page and my research. Most people with Hashimoto’s will experience weight gain, and so of course that’s what gets the most focus, but some people actually experience weight loss, or they can’t keep their weight on. This is especially problematic when a person has multiple food sensitivities and needs to adhere to an autoimmune diet that restricts foods.
Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function!
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
WHAT’S CAUSING YOUR LEAKY GUT
https://thyroidpharmacist.com/articles/whats-causing-your-leaky-gut
Dr. Wentz, when you say that Hashimoto’s can lead to weight loss and hyper-like symptoms because of the attack on the thyroid, would this excess of thyroid hormone be detected by blood test as a low TSH or is it possible to have those kind of symptoms with a high TSH?
I have had Hashimotos Disease for 20 years. I started taking Selenium, Vitamin D, B12, Fish Oil, and a multi vitamin about 4 months ago. I have been on Synthroid for 20 years with 125 mcg dose most of the time. I had blood work done inMarch and I was hyper. My doctor decreased my Synthroid to 112 mcg. I went back this week and i was still Hyper. She decreased my Synthroid again, now to 75 mcg. Whats goin on with me? Please help!
Pamela – thank you for following this page. Graves and Hashimoto’s are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto’s, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people) – Hashimoto’s results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually people with Graves have hyperthyroidism and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine, the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The information I present is based on my own research, in my journey for overcoming my autoimmune thyroid condition.
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hello i am 19 years old Male, i just recently got diagnosed with hashimotos. When i started to feel crappy like in 2 to 3 days my whole right side of my body hurt i could not move my wrists or anything. than it just is not strictly on my right side of my body. i dont know how to explain it my right side of my body just feels different than my left. i also am experiencing termeros in my tremors hands is this normal? its mostly on my right side. im very scared.
Daniel – Thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Hello Dr Izabella,
I have Hashimoto, I was hypothyroid and on NDT. Since a few weeks I have gone hyperthyroid for the first time, I have the classic symptoms like the heart palpitations, shaky, etc. My question is, do I lower my NDT until the hyperthyroid goes back to hypo? Or stay on the same dose I was until my body sorts itself out? I have been trying to find information online, but I can’t find any. I hope you can help.
Best wishes from NZ, Maria.
Maria – thank you for following this page. People with Hashimoto’s may experience BOTH hypothyroid and hyperthyroid symptoms because as the thyroid cells are destroyed, stored hormones are released into the circulation causing a toxic level of thyroid hormone in the body, also known as thyrotoxicosis or Hashitoxicosis. Eventually, the stored thyroid may become depleted and due to thyroid cell damage, the person is no longer able to produce enough hormones. At this time, hypothyroidism develops.
I recommend that you refer back to your practitioner, who is familiar with your health history or that find a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Hi
I was dx hypothyroid 16 years ago and placed on Levothyroxine. Never felt healthy in that time, always run down, poor work attendance etc. Since having my youngest whose nearly 3 now I’ve got progressively worse, at my worst I was literally bedridden. Now dx with Hashimotos and taking T3 but still feel ill. Any advice?
Thanks
Michelle – thank you for following this page. There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication which you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
HOW THE DOSE OF YOUR THYROID MEDICATION CAN UNCOVER YOUR ROOT CAUSE
https://thyroidpharmacist.com/articles/the-dose-of-your-thyroid-medication-can-uncover-your-root-cause/
HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications/
I have been battling with doctors for two+ years as my list of symptoms continue to grow…in short, each year brings new symptoms. I have family history of hypo, thyroid cancer, goiters, IBS, Gastroparesis, B-12 deficiency, etc. etc. I myself have a nodule. I am self-pay so all the doctors were resistant to what they deemed as unnecessary expensive tests (TPO &Thyroglobulin) until I recently insisted. Most notably is that part of my field of vision in my left eye has gone blurry and they told me I am a mystery cause there tests couldn’t figure it out. I am no where close to a hypochondriac, have enjoyed great health most of my life. But as I see myself start to develop more and more symptoms similar to so many family members before me and concern for my children to follow suite…I am desperately trying to figure this out. Please advise, help, direction would be so appreciated!!! thanks
Cyndi
Cyndi -Thank you so much for following this page. Here is some information which you may find interesting.
Three things MUST be present in order for autoimmunity to occur…
1. Genetic predisposition
2. Environmental triggers
3. Intestinal permeability (leaky gut)
Developing autoimmunity is like a three-legged stool, all of these factors must be present for autoimmunity to occur! When you remove one of these, you can prevent or stop autoimmune disease. While we can’t change genes, if we know the trigger, we can remove it and we can heal the gut.
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm
IS HASHIMOTO’S HYPOTHYROIDISM GENETIC?
https://thyroidpharmacist.com/articles/is-hashimotos-genetic
Do you treat hashimotos the same during a hyperthyroid phase as you do in hypothyroid phases? I just discovered I have hashimotos but I am having hyperthyroid symptoms so taking more thyroid hormone doesn’t make sense to me.
Moriah – thank you for reaching out! Graves and Hashimoto’s are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto’s, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people)-Hashimoto’s results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually, people with Graves have hyperthyroidism, and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own, and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. Here are the links to my books:
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
I have Hyperthyroidism. I’m vegan and Gluten Free i do not take any animal food . I would like to folow your diet but can I replace animal protein with anything alse??
Irina – thank you for reaching out. Recovering from adrenal fatigue and hypothyroidism when following a vegetarian diet is very challenging, as vegetarian diets are often carbohydrate heavy. Vegetarian sources of protein such as legumes (beans), dairy, grains, soy and some seeds may be incompatible with trying to heal a leaky gut, which is almost always present with Hashimoto’s. Pea protein is an alternative that may be easier to digest and is less likely to cause food sensitivities.
I have created my own line of supplements, which also includes an Organic Pea Protein. Here’s the link: https://rootcology.com/collections/supplements/products/copy-of-purepaleo-protein-vanilla
Eggs, some seeds, and nuts would be the preferred sources of protein for vegetarians. However, some people with Hashimoto’s may be intolerant to those as well, especially in the early stages of starting a healing diet. Being a vegan is even more challenging, and nuts and seeds would be the go-to source of protein, which are usually too difficult to digest for many in the beginning of their thyroid healing journeys.
While vegan and vegetarian diets have been reported to be extremely helpful with autoimmune and chronic conditions, I have not been able to find reports of people recovering from Hashimoto’s by following a vegan diet. Even devout vegans who are nutritionally conscious still struggle with low body temperatures, hypothyroidism and Hashimoto’s.
Additionally, many former vegans have reported improved symptoms of Hashimoto’s following transitioning to a Paleo diet. Based on this, I believe that animal proteins must play an important role in building back the health of people with Hashimoto’s. That said, while meats and fats are important for healing, eating them exclusively will produce an acidic environment in the body, hindering healing, and thus the diet should be balanced with plenty of nutrient rich vegetables (suggested ratio may be 20% meat/80% veggie).
Additionally, vegan and raw vegan diets can be extremely helpful for cleansing and detoxifying, especially for those with persistent protein digestion issues. A vegan diet can be followed for a few days to a few weeks and may help the body detoxify. B12 and iron or ferritin supplements should be utilized at this time to prevent deficiency. Please know that I’m a big proponent of bio-individuality which honors the distinct nutritional needs of every human being. I’m not saying everybody needs to eat meat, but I am saying to listen to your body if it needs meat. Here are a few articles which might help:
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
ELIMINATION DIET FOR HASHIMOTO’S
https://thyroidpharmacist.com/articles/elimination-diet-for-hashimotos
I recently had my TSH level checked and my doctor said that I had such low amounts it was undetectable, which I now understand means hyperthyroidism. She’s not checking me for antigens and my t3 and t4 levels. She thinks it’s Hashimoto’s, but from everything I am reading Hashimoto’s causes hypothyroidism. Is that possible? I’m just not sure if it’s possible to have hyperthyroidism caused by Hashimoto’s. Can you clear this up for me? Thanks in advance.
Holly – thank you for reaching out. Graves and Hashimoto’s are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto’s, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people)-Hashimoto’s results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually, people with Graves have hyperthyroidism, and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own, and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. Here are the links to my books:
Hashimoto’s Root Cause
https://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
My dad is the hospital. He has many conditions (MS, heart disease, thyroid and more)… he’s a mess. He has been on thyroid medicine for probably 20 years. I noticed that the hospitalist decided to check his TSH likely because he is in afib. The same hospitalist a few years ago did this and took my completely off her levothyroxine 100 mg because it came back low. The thing is she didn’t do any of the other thyroid tests. And because of my mom’s situation no one tested her thyroid for a year and no surprise the TSH was in the 8’s. By the way I have Hashimoto’s. My dad’s test came back as .15. I would love to know your thoughts and whether I should try to intervene. With the afib I can see where they are coming from but he is also currently on the medicine to lower the TSH so you would definitely so it should be low. Thank you! I am so glad that I found your information.
Edit: His TSH is at .75
Riah – Thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms. Here are some links which might help:
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
MY RECENT CHALLENGES AND FINDING DR. RIGHT
https://thyroidpharmacist.com/articles/my-challenges-and-finding-dr-right/
Hello ,
I am 24 years old and just did my pharmacy master’s degree. Two years ago I started having health problems. It all started with swollen cervical lymph nodes which no doctor could explain. Three antibiotics after I became really sick and the nodes weren’t going away. I was constantly dizzy , had extreme fatigue , nausea and abdominal pain. Somehow I managed to get some tests and blood work. My antibodies were pretty high and I was diagnosed with Hashimoto’s . The problem was that TSH , T3 and T4 were all in the so called normal range. Doctors weren’t concerned because I was a young healthy 22 year old girl , tall and skinny. Than I was diagnosed with chronic gastritis and GERD and was told they cannot do anything else for me than prescribe me PPIs. For 2 years now I haven’t felt like myself for more than half a day. I still have all the symptoms , can’t eat properly because of leaky gut and constant abdominal pain , get dizzy and my brain doesn’t work as it used to. I just try to ignore my symptoms and go on with my life , but some days I feel like giving up.
I recently read ‘Root cause’ and plan to try some of your recommendations. I read above that you also weren’t the typical hypothyroid case (with no weight gain) and this is my main concern. Is there a possibility to have all those syptoms with my hormones in the normal range and with being skinny as I am or do I have to look for some other cause?
Thanks in advance. Sorry for the long post , but I hope sharing all the symptoms I have could help someone else in the same situation.
Velina – thank you for sharing your journey. Most conventional physicians use the TSH test to determine if one has a thyroid disorder and to dose thyroid medications. However, this test can often times be misleading, as levels of circulating hormones may fluctuate at different times, such as in Hashimoto’s, where the person affected may fluctuate between highs and lows.
Additionally, when scientists first set the “normal” ranges of TSH for healthy individuals, they inadvertently included elderly patients and others with compromised thyroid function in the calculations, leading to an overly lax reference range. This resulted in people with underactive thyroid hormones being told that their thyroid tests were “normal,” based on this skewed reference range.
WHAT TO DO IF YOUR TSH IS NORMAL AND YOU ARE ANYTHING BUT
https://thyroidpharmacist.com/articles/what-to-do-if-your-tsh-is-normal-and-you-are-anything-but/
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well.
TOP 10 THYROID TESTS AND HOW TO INTERPRET THEM
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
I have hashimotos! It’s been a night mare. Dizziness all the time on and off. Right now my biggest problem is my heart. My heart rate is going as low as 30. The cardiologist I’m seeing has said he thinks it’s depression and tried me on an antidepressant, but after 5 days I quit it because it made me feel terrible! My endocrinologist says my thyroid wouldn’t cause my heart to slow down that much. I’m feeling like I’m at the end of my ropes with this! I have went gluten free multiple times and nothing has seemed to help me. My thyroid goes from not working to over working and it causes other major issues. My last tpo was over 2000. ? where do I go from here?
Kay – thank you for following this page. Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. Here are the links to my books:
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hi Izabella,
I love your blog. It’s so helpful.
I have Hashmotis and have lived with it for over 10 years.
I usually manage variations in symptoms by getting blood tests and making minor changes in my throxine levels.
I’m a Naturopath and use supplements and acknowledge the necessity to keep on top of gut function with diet and supplements. I have recently come through a stressful phase which has left me with different symptoms than I usually experience when I am out of balance.
I’m thinking it may be a low level thyroid storm .
I would really like your help. I have been experiencing brain fag, bad memory and recall, overheating, anxiety, insomnia both onset and offset . Bowels, skin, muscles have been ok, energy levels high. Unable to nap and rest. Pressure behind my eyes and in my face. The thing that has really bothered me is the lack of sleep. I take my thyroxine at night and one night I noticed a real increase in alertness soon after taking it and didn’t sleep till after 2pm that night, this has been the pattern. The next night I decided not to take it and slept like a baby. Took it again , awake. Stopped, slept well..
blood tests are
16/3/18
TSH 3.5 (.04-4.0)
T4 21(10-20)
T3 (4-8)
I do best when my TSH is 1-1.5
So that’s hypo for me.
Symptoms are hyper and I am just uncertain as to how long I can stop taking the thyroxine so I can sleep and also get my TSH
back to where I work best. Any suggestions?
Madhu – thank you for following this page. People with Hashimoto’s may experience BOTH hypothyroid and hyperthyroid symptoms because as the thyroid cells are destroyed, stored hormones are released into the circulation causing a toxic level of thyroid hormone in the body, also known as thyrotoxicosis or Hashitoxicosis. Eventually, the stored thyroid may become depleted and due to thyroid cell damage, the person is no longer able to produce enough hormones. At this time, hypothyroidism develops.
THE MANY FACES OF HASHIMOTO’S
https://thyroidpharmacist.com/articles/the-many-faces-of-hashimotos/
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this. Sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. Here are the links to my books:
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
First, I can’t thank you enough for such a descriptive website with awesome content. Its surely a goldmine for people like me. I am writing a long post, hope you will read through it.
I am from India (Bangalore). My case is weird since so many doctors and specialist couldn’t figure out the symptoms that are mentioned across this site and it moves back to 2011 where my TSH was a little high (5.x) and it was ignored (found in routine annual medical health check). Then, following years also showed an increased cholesterol level (high range) and again TSH was silently ignored. (6.X) Its like the general physician never cared about it and I being ignorant about TSH just moved on. Parallelly I started having frequent stomach upsets and I just took the prescribed medicines for the cure. Eventually the stomach issues enlarged and after Colonoscopy, endoscopy etc. doctors told me that I have IBS. They asked me stop Whey protein and other supplements which I regularly took as a part of my gym routine and prescribed some medicines (which never helped).
It was during 2014 the IBS was at its peak, I was having severe bloating, diarrhea, acid reflux etc. and I started with a chest pain on the left side. Again, on my routine checkup I was told that I was having a pleural effusion. I went to the top doctors and most of them prescribed tuberculosis medicine without even running a diagnosis for TB. Finally, I went to a doc and asked him forcefully to run a series of tests on blood, sputum, drained liquid culture, skin test etc .and everything came back negative for tuberculosis. So, I never took TB medicine and eventually I cured myself by Ayurvedic medicines (which works for me 99% of the times). There were 2 doctors who were fair enough to go against the norms and tell me that, 1. It might be eosinophilic pleural effusion (eosinophil count = 4X in the culture and blood) 2. It’s happened because of the increased acid reflux while asleep, that it aspirated to lungs and caused an infection and finally, CT scan revealed a calcified granuloma of 1.3 mm in the left lung and the case was closed telling me go live with it!
After this incident, my symptoms like, knee/back pain, brain fog, insomnia, fatigue, anxiety etc. increased a lot. I can’t keep count on how many specialists I visited and most of them told me that I am taking too much of stress and I need to consult a psychiatrist. Its at this point I lost it with the so-called doctors and started doing my own research. Ayurvedic medicines have always helped me bring TSH down. I have already taken supplements that you have mentioned like Selenium, Magnesium, CoQ 10 etc. on and off, during these years.
I almost took control of my IBS by isolating many food items from my regular diet like Gluten for example and switching to A2 Milk and products, going Organic! (also following Ayurvedic detox methodology called Panchakarma). But I still suffer from diarrhea/constipation.
I finally managed to argue with an endocrinologist and get Anti TPO test done last year. Till then every single one of them told me that being a Male its OK to have TSH at levels of 6-8 and never come back again till it crosses 10.
My Anti TPO came at 800+ and the doctor prescribed me Thyroxine .25 mcg and didn’t say word more. I knew that this is the regular protocol and he won’t look beyond that.
Here is a brief history if you are interested in chronological order:
9/2010: T3: 1.03 ng/ml, T4: 6.95 ug/dl, TSH: 2.73
12/2011: TSH: 5.29
5/2012: T3: 0.80 ng/ml, T4: 6.07 ug/dl, TSH: 4.30
2/2013: TSH: 4.0, IBS Starting stage
2/2014: Pleural Effusion, Very High Eosinophils, Severe IBS
4/2015: TSH: 6.4, FT4: 1.51
2/2015: TSH: 7.75
6/2015: TSH: 5.3
12/2015: TSH: 4.99
4/2017: TSH: 6.02
11/2017: Anti TPO: 801, Prescribed Thyroxine .25mcg (didn’t start)
2/2018: T3: 73 ng/dl, T4: 5.10 mg/dl, TSH: 4.02 (Normal)
Others:
ANA: Negative, Cholesterol: Always just on the higher side, Uric Acid: Normal, S.Cretainine: Normal, Colonoscopy: Normal, Endoscopy: LES LAX, H.Pylori (Not seen), Stool routine: Bacteria: +, Cysts: Ascaris L
Blood pressure: Keeps varying Normal – High, CT Scan: Head/Neck: Normal, USG Neck: Normal, 3T MRI Whole Spine: Normal, USG Abdomen: Normal
Currently I am facing joint pains, high fatigue, severe anxiety / insomnia/depression issues.
Here are my questions and I really hope you will answer them:
1. Do I need any more tests to drill down to the exact issue?
2. Currently do I need to start with Thyroxine? Is this the reason for my anxiety?
3. Should I continue with supplements like Selenium, Magnesium etc.?
4. Should I continue taking Glutamine for healing leaky gut?
5. Are there any more tests that I need for my GI issues?
6. Dairy(A2 : Milk and Yogurt), Rice/pulses is something that is hard to exclude for me What’s your recommendation?
Thanks and Regards
Deepak – Thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms. Here are some links which might help:
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
MY RECENT CHALLENGES AND FINDING DR. RIGHT
https://thyroidpharmacist.com/articles/my-challenges-and-finding-dr-right/
Thank you Dr.Wentz for the reply. Though I visited these links before, if I am not wrong ASIAN countries are not covered yet (hopefully you will cover us and extend your knowledge and approach to India as well) so you are my best hope 🙂 In the mean time do let me know if you recommend any tests, and I will continue my search for doctors and the root causes on my own.
Thanks again for the great work.
Deepak – you are very welcome! I am sorry you are having difficulty finding a good practitioner. If you cannot find a Functional Medicine practitioner in your area, it is possible to work with an overseas practitioner remotely via Skype or some other online video platform. Here are some links you might find helpful:
http://www.thyroidpharmacistconsulting.com/europe1.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
I have a history of hypothyroidism in my family and recently found out that my mother was diagnosed with Hashimoto’s (she apparently knew but didn’t tell me). I have many of the symptoms related to hypothyroidism as well as being diagnosed with fibromyalgia (I read the article you referenced and saw how the symptoms overlapped) and Joint Hypermobility Syndrome. The fatigue kills me and I’ve constantly had my TSH and FT4 tested. I recently had my TSH, TT4, and FT3 tested and all came back within the “normal” range. Here are my test results:
TSH: 1.326 (0.300-3.00)
TT4: 10.8 (4.5-12.0) I’m also on birth control
FT3: 2.5 (2.3-4.4)
In the past, my TSH has been as high as 2.87 and my FT4 has been as low as 0.90 (0.78-2.19).
Is there anything specifically that I should bring up to my PCM? My numbers are within the accepted range, but they’re on the very low end.
Heather – Thank you for following this page. Most people feel best with a TSH of around 1 or lower and with a Free T4 and Free T3 in the upper half of the range. It is expected that your TSH will be very suppressed when optimal on NDT medication. How much thyroid replacement therapy is needed is unique and different for each person, so it’s important to work with a functional medicine practitioner or a doctor, who can closely monitor your dosage and your progress.Every six weeks is usually a good schedule for testing your thyroid hormones. Here is a research article which might help further:
TOP 10 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
I have hashimotos and I have heart palpitations whenever I exercise or get up suddenly. I noticed that my blood pressure goes from being slightly high to being normal again, which I don’t understand. I also have been having this weird issue with my left eye that has just gotten progressively worse ever since I was diagnosed. It protrudes more than the other eye, and I have a lot of pressure around it and headaches. Sometimes I’ll have pain in my upper teeth too. I thought maybe I had a sinus issue but I’ve been to several doctors about that and don’t have anything sinus related going on. Do you think these symptoms I’m having are related to hashimotos?
Olivia – Thank you for sharing your journey. Please, understand that due to liability issues, I am unable to answer specific medical questions, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms. Here are some links which might help:
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
MY RECENT CHALLENGES AND FINDING DR. RIGHT
https://thyroidpharmacist.com/articles/my-challenges-and-finding-dr-right/
I was diagnosed with hashimoto’s but am really confused, my TSH was normal for so long but I feel like I have hyper symptoms. Can dizziness be a classic sign of hashimoto’s?
Maddie – thank you for reaching out. Vertigo or dizziness can be common symptoms seen in people with thyroid disease. In one research study, 52% of Hashimoto’s patients showed an alteration of Vestibular function, which can affect balance and lead to vertigo and nausea. Getting your thyroid antibodies down will, of course, help vertigo, but in the meantime, I wanted to share a new advancement with you:
https://denver.cbslocal.com/2012/04/23/colorado-doctor-finds-way-to-treat-common-vertigo/
I hope this helps!
I recently went to my GP because I was experiencing symptoms of both Hypo and Hyperthyroidisms and my TSH was slightly elevated; 4.20. I’m 38 and honestly thought I was starting premature menopause because of the hot flashes and other symptoms I was experiencing. A number of the symptoms I have been experiencing started a few years ago; persistent fatigue and brain fog, but others started within the past 4/5 weeks; rapid heart rate, hot flashes, sensitivity to cold, insomnia, irritability, tremors in my hands, not to mention that this is the first time in more then a decade that I have missed a period. No, I am not pregnant. The GP thought that I might have Hashimoto’s and decided to order labs for TPO and Free T4. Well, those labs have come back “normal”; TPO = 1 and Free T4 = 1.18. I haven’t had any other labs done so far, but I have an appointment to see an endocrinologist in January. Needless to say, Hashimoto’s has been ruled out. I am really confused about whats going on with me and dreading the month and a half long wait to see a specialist while feeling as horrible as I do.
Lydia – thank you for sharing your journey. I am so sorry to hear you are struggling with all of this. <3 Graves and Hashimoto's are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto's, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people) Hashimoto's results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually, people with Graves have hyperthyroidism, and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own, and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this. Sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. Here are the links to my books:
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
I have Hashimoto’s and think I have been fluctuating between Hyper and Hypo symptoms (fatigue, cold, no appetite, anxiousness, muscle weakness, moments of sweating, etc.). My levels are normal, but he said because they could be fluctuating, he wanted to start me on Synthroid. I now feel like the Hyper symptoms have gotten more frequent. Ive only been on it for 3 weeks, so my questions are 1. Even if your levels are showing normal, can they be off and can medication “level” them out? and 2. I called my Endo to tell him I think I am having hyper symptoms (I lost 10 lbs in a week) but he said to give it more time to level out. Is that normal??
Kelli – thank you so much for sharing your journey. <3 Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism, it's an autoimmune disease that needs to be managed. Whether you have all, part or no thyroid, the autoimmunity still persists in most cases. We need to re-balance the immune system which begins in the gut. With the exception of discussing proper thyroid medication dosing, the majority of my website and book's focuses on balancing the immune system. The info I present is based on my own research and journey overcoming my autoimmune thyroid condition. Here are some articles you might find helpful:
Here are some articles I think you might find helpful:
IMPORTANCE OF GUT HEALTH
https://thyroidpharmacist.com/articles/importance-gut-health/
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
Hi, I just went to the Dr because I was experiencing some of the symptoms of both hypo and hyperthyroidism. Hair loss, rapid heart beat, sweating; but then also weight gain, heavy periods, constipation. My TSH levels are so low they are untraceable, and my T4 was on the high end of normal. So, how do they treat this, as hyper or hypothyroidism? Could it be hashimoto’s?
Heidi – thank you for reaching out and sharing your story. <3 I am so sorry to hear you are struggling with all of this. Graves and Hashimoto's are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto's, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people) Hashimoto's results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually, people with Graves have hyperthyroidism, and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own, and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. I hope this helps! You may find these resources helpful as well.
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Food Pharmacology
https://www.amazon.com/Hashimotos-Food-Pharmacology-Nutrition-Protocols/dp/0062571591?tag=thyroipharma-20
I’ve been diagnosed with Hashimotos and Thyroid cancer. Not sure how much you read your comments but it feels like when I start eating right I get seriously fatigue by the 7th day. I’ve done without gluten /dairy /soy. Then I’ll be like ok maybe alittle more gluten (not feeling well) seems to work and then it’s back to how it feels. It’s like a circle game -add eggs then don’t add eggs. It seems for me after so many days I don’t feel good no matter what I’m trying – Wondering where I can get your cook books . I also notice cardio -nothing major but by the 3rd day of simple fast past walking -I’m bed ridden. AnY pointers on the exercise part?– or is that something that comes after getting your gut cleaned out and what not? It’s just very frustration cause I’ve heard so many things about the eating and it’s like who do you believe ? Hope to hear from you. 🙂
Vanessa – thank you for reaching out and sharing your journey with me. I’m so sorry you are struggling with all of this. <3 My heart goes out to you. Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to rebalance the immune system to prevent this. Sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
IMPORTANCE OF GUT HEALTH
https://thyroidpharmacist.com/articles/importance-gut-health/
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
When if comes to exercise, I would recommend anyone embarking on a program of exercise starts slowly and progresses at their own pace. Exercise can be very healthy, but for people with Hashimoto’s it can create stress. Stress causes our adrenals to pump out extra hormones, and shifts our body from a relaxing, digesting, healing state to a fight or flight state.
The body’s energy is shifted from doing “useless” things like growing beautiful hair, metabolizing, making hormones, digesting and repairing itself, and instead, all of the body’s resources are reserved to make cortisol and adrenaline that is pumped through our veins so that we can keep going. Eventually, we run out of nutrients that are required for proper adrenal function and we get to a state of adrenal fatigue. This is when our body is no longer able to heal itself and we feel drained. Here is an article you might find interesting:
ARE YOUR ADRENALS SABOTAGING YOUR HEALTH?
https://thyroidpharmacist.com/articles/are-your-adrenals-sabotaging-your-health
I have always gotten migraines from the heat in the summers, but last year, my migraines were severe, and my symptoms were more heat exhaustion/stroke. I play slowpitch tournaments. I drink 2 full water bottles a game, i have added gatorades to my mix, go in the shade when i can and no matter what i do, i cannot stop the migraines and getting sick. Is there anything else i can do as the tournament season is starting soon? I have hashimotos, have half a thyroid left, and have celiac disease. I eat GF and have worked to heal my leaky gut. Thanks for any help!
Tammy – thank you for reaching out. Working with people with Hashimoto’s, I have found that most people will experience pain on some level. For some, it may manifest as a chronic condition, such as migraines or joint pain. Here are a some articles you may find helpful:
PAIN AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/pain-and-hashimotos
NEW STUDIES ON MAGNESIUM AND THYROID HEALTH
https://thyroidpharmacist.com/articles/new-studies-on-magnesium-and-thyroid-health
ELECTROLYTES FOR HASHIMOTO’S
https://thyroidpharmacist.com/articles/importance-electrolytes-hashimotos/
Hello, I have been a hypothyroid pt. since I was 12 and I am now 66. Hashimoto’s labs always negative. I have been on Synthroid up until almost a year ago, when I switched to NP Thyroid. I have always had the same “low thyroid” s/s since I have been on Synthroid but always told my bloodwork is fine. I saw an Endocrinologist a few years back stating despite being on Synthroid I still don’t feel good. He agreed my # are fine.
It wasn’t until I went to see a Dr for bio identical hormone replacement and she recommended trying NP Thyroid. I switched over and labs for a yr were good. I felt better and lost a few pounds. All my life I have been struggling with my weight. All of a sudden I developed binocular double vision went to ER and had a work up. All was negative except we found T3-T4 were normal but TSH below 1.0. Repeated labs after dose lowered by one pill a week. My TSH has come up a little after my dose was decreased from 90 daily to 90 5 days a week and 1/2 tab 2 days divided within the week. I feel fine other than visual problem mostly towards end of the day. MG labs in progress, and I will see a Neuro ophthalmologist coming up.
From your experience, how long does it take to show a higher TSH after my dose was lowered? Can I have Hashimoto’s despite my antibodies being normal. In addition to Hypothyroidism, I was diagnosed with RA last year. I have mild HTN and elevated cholesterol on statins. I know you can’t diagnose me but from your experience, I wondered your thoughts
Judy, Thank you so much for sharing your story, and I’m honored that you’ve reached out. It is possible to have Hashimoto’s even if your thyroid antibodies are negative. This can happen in seronegative Hashimoto’s, where the autoimmune damage is present but not reflected in antibody levels. In these cases, diagnosis may be supported by ultrasound findings or clinical presentation over time. Regarding TSH response, it can take about 6–8 weeks after a medication adjustment to see a significant change in TSH levels, though some people may respond sooner or later depending on their individual metabolism and overall health. You’re clearly being proactive and thoughtful about your care, working with a knowledgeable practitioner and continuing to monitor how you feel is key. I’m wishing you continued progress and answers as you navigate the vision symptoms and autoimmune overlap. Sending you healing thoughts! 💛