While I have a lot of stories of people who recovered their health through removing reactive foods, adding in healing foods, and taking the appropriate supplements, I personally did not get my Hashimoto’s into remission by following those steps.
Sure, I felt much better, and my thyroid antibodies significantly dropped with the help of nutrition, but eventually my health problems began creeping back in. All of a sudden, I became sensitive to nuts, bananas, eggs, and all of the “nutrient-dense” Paleo foods that I began eating once I found out I was gluten and dairy sensitive.
I later learned that this was because I was unknowingly walking around with four different gut infections, including Helicobacter pylori, which is connected to both Hashimoto’s and Graves’ disease and can cause new onset food sensitivities!
I was shocked and in complete disbelief that I had all of those issues (this was after two years of eating a gluten-free/dairy-free diet). I began treating my gut infections one by one, and steadily saw improvement in how I felt, along with a reduction in thyroid antibodies.
At first, I was really embarrassed to speak publicly about having “gut infections,” as it sort of grossed me out. But when I began working with people with Hashimoto’s, I realized I wasn’t the only one, and that it was important for me to get past the ick factor to spread awareness.
In this article, I’ll dive a little bit deeper into:
- How infections can act as Hashimoto’s triggers
- The role of gut infections in autoimmunity
- How H. pylori affects Hashimoto’s
- Testing for H. pylori
- Treatment options for H. pylori
Hashimoto’s and Infections
Chronic infections are the Hashimoto’s triggers that get the least amount of attention, yet identifying and treating them can result in a complete remission of Hashimoto’s. (1) Additionally, some of the infections can be progressive, leading to more and more symptoms if not identified and treated accordingly. Thus, I want to make you all aware of them whenever I can.
Infections can live in our gums, sinuses, thyroid gland, stomach, intestines, and anywhere in our bodies. These infections can contribute to the development of autoimmunity through various mechanisms, depending on where they “live” (i.e. via molecular mimicry outside of the thyroid gland, or via the bystander effect inside of the thyroid gland). (2-7)
Infections that live in the gut, gums, or sinuses can also contribute to intestinal permeability directly, as they are connected to the digestive system.
Molecular Mimicry
Molecular mimicry is one of the leading theories of autoimmune disease. (8) In very simple terms, this theory hypothesizes that our immune system begins to attack our own thyroid gland because we are infected with a pathogenic organism (like a bacterium, parasite, or virus), that looks similar to components of the thyroid gland.
The immune system remembers isolated protein sequences on the pathogen (rather than the entire DNA sequence of the pathogen) and then looks for similar looking proteins as targets for an attack. If the proteins on the thyroid match the proteins the immune system remembers, then the thyroid will be targeted for attack as well. Therefore, the immune system attacks the thyroid gland due to a case of mistaken identity, when it is actually trying to attack an infection!
Bystander Effect
Another popular autoimmune theory that explains how infections can trigger autoimmunity, is known as the bystander effect theory. (9) This theory proposes that an infection inside the actual target organ leads the immune system to attack the “home” of the infection. In the case of Hashimoto’s, the infection is inside thyroid cells, and thus the immune system attacks the thyroid gland.
Scientists have noted that in people with the right genetic sequence, an infectious agent that resembles the thyroid gland can trigger Hashimoto’s. (8,9)
Gut Infections and Autoimmunity
In 2015, 80 percent of my clients who hit a plateau with nutrition and took the gut tests I recommended, tested positive for at least one gut infection. (You can read more details about my analysis of gut tests in this article.)
We know that the three-legged stool of autoimmunity consists of a genetic predisposition, one or more triggers, and intestinal permeability (otherwise known as leaky gut). (10) All three are required to be present for an autoimmune condition to manifest. Eliminating the triggers and addressing the leaky gut are keys to getting autoimmune thyroid disease into remission.
While conventional medicine ignores the gut in relation to thyroid health, natural medicine also often misses the point in gut health by solely focusing on supportive and maintenance care of the gut, such as taking gut support supplements and probiotics, consuming nourishing foods such as bone broth, and removing reactive foods.
Of course, all of those steps are essential in restoring gut health when someone is nutrient depleted or has a strong reaction to a particular food (like gluten), but they do not get to the underlying root cause of most cases of intestinal permeability… gut infections!
Thus, I recommend a three-pronged approach to healing the gut:
- Kill off any infections that may be irritating the gut wall and causing you to have a leaky gut.
- Remove foods that have a large particle size (and are more difficult to digest) for 30 to 90 days, such as gluten, dairy, soy, grains, nightshades, nuts, and seeds.
- Add supplements that accelerate gut healing.
As I try not to adhere to a dogma of “there’s only one right way to healing,” my infection protocols will include supportive foods, herbs, and medications (and sometimes a combination of all of the above), to properly get rid of an infection.
Why Isn’t There More Focus on Infectious Origins of Autoimmune Disease?
Scientists have found a great deal of evidence which suggests that Hashimoto’s is caused by an infectious pathogen. (2-7) Many Hashimoto’s patients have received positive blood tests indicating a past or current exposure to an infection, and studies have shown that certain birth months when infections are more prevalent, produce more cases of Hashimoto’s.
One extensive research study showed that most people diagnosed with autoimmune diseases are born in April, while the fewest are born in October. (11) Many environmental factors, such as lack of sunlight (vitamin D), seasonal allergens, availability of certain foods, and the prevalence of specific pathogens, can all impact a person’s development in utero and play a role in determining future health conditions. (12)
Scientists have yet to say that Hashimoto’s is caused by an infection because they’re looking for “ONE” single infection in every person with Hashimoto’s… but it’s not a black and white issue.
It’s too simplistic to say that for an infection to be at the root cause, every person with the disease should have the same infection, and that every person without the disease will be infection-free.
Numerous infectious pathogens may have protein sequences similar to the thyroid gland, possess the ability to infect the thyroid gland, and cause leaky gut. (13,14)
Some new research even suggests that our friendly bacteria (Lactobacillus species) has a similar protein sequence to the thyroid gland, so in the case of leaky gut, the good bacteria can get into our bloodstream through tiny holes in a compromised gut and cause an immune response, which can potentially cross-react with thyroid tissue. (15,16)
There are many different scenarios that are potential mechanisms for how various infections could lead to developing autoimmune disease. Studies often fall short because they assume that one infection only applies to one condition.
In my observation, the equation is more akin to advanced calculus, rather than simple math. It looks more like this: genes combined with infection A, and perhaps infections B, C, and even D, in the absence of nutrients and beneficial bacteria, leads to the development of an autoimmune condition.
Now, let’s focus on one of the most common infections seen in Hashimoto’s, H. pylori.
Helicobacter Pylori Infections
Helicobacter pylori (H. pylori) is a gram-negative spirochete-shaped bacteria that burrows into our stomach lining and secretes urease, which neutralizes stomach acid. (1) The byproduct of the urease and stomach acid is toxic to epithelial cells (lining the surface), as are the other chemicals produced by this bacterium, leading to damage to cells, a disruption of tight junctions, and inflammation.
This bacterium is transmitted orally, from person to person, as well as potentially between people and their pets (who can resist doggie kisses, right?). It can trigger an immune response and has been implicated in numerous autoimmune conditions, including Hashimoto’s and Graves’ disease. (2-7)
H. pylori has also been implicated in ulcers and can contribute to low stomach acid, leading people to improperly digest their foods. In turn, the poorly digested foods are not broken down properly, and the person ends up with multiple food sensitivities as a result of this infection.
Marshall and Warren, the Original Root Cause Rebels
The story behind the discovery of H. pylori being the root cause of ulcers is one of my favorite stories and inspires me to keep doing what I’m doing, despite a lack of acceptance of a root cause approach to Hashimoto’s in conventional medicine.
As early as 1899, Professor Walery Jaworski of the Jagiellonian University in Krakow (one of the oldest surviving universities in the world that also happens to be on my bucket list as a place for future studies), found spiral bacteria in gastric washings of humans, and was the first to suggest that these bacteria may cause gut issues. He published his research in a medical handbook on addressing gastrointestinal issues, but as the handbook was only available in Polish, the research went largely unnoticed for almost a century!
In the 1980s, two young scientists from Australia named Barry Marshall and Robin Warren were convinced that H. pylori caused ulcers. However, their colleagues ridiculed them, as the conventional thought in those days was that no bacteria could survive the acidic environment of the stomach.
Furthermore, ulcers were “obviously” caused by stress and spicy food, as time and time again, a stressed out person was more likely to come down with an ulcer. (Of course, we know what happens when we are stressed out: our bodies become more susceptible to infections, as the microbes that we have living inside of us receive signals from our stress responses, showing them that we are weak, and giving them an opportunity to take over.)
Most “serious” ulcer researchers were focusing on optimizing ulcer repair surgeries, not looking for bugs in a place where bugs couldn’t grow! But Marshall and Warren kept going, though they had trouble growing the bacteria in Petri dishes… until one of them accidentally left the dishes in the incubator over the Easter weekend.
Marshall was so convinced of his work that he actually drank a beaker of cultured H. pylori and became ill with nausea and vomiting several days later. He was found to have gastritis (inflammation of the lining of the stomach) and H. pylori. He then showed that taking antibiotics to treat the H. pylori could reverse gastritis.
Finally, in 1994, the National Institutes of Health stated that most ulcers were in fact caused by H. pylori, and recommended the use of antibiotics for the treatment of ulcers.
This big news was newly emerging research in 2002 when I started pharmacy school, 20 years after their initial discovery.
Eventually, the rest of the world caught up. Drs. Marshall and Warren were awarded the 2005 Nobel Prize in Medicine (23 years later), and slowly, physicians began to test for H. pylori in people with ulcers. (17-21)
I have seen plenty of recent research connecting H. pylori to autoimmune thyroid disease, but in my experience, most conventionally trained physicians are not aware of this connection, how to detect the infection, or how to treat it with anything other than super intensive antibiotics.
This is one of the reasons why, when I scour the medical databases for current research on Hashimoto’s, I look for articles not just in English, but also in Polish, Russian, Spanish, and Portuguese, and why I’m also super excited about my Hashimoto’s books being translated into those languages! (Please note: We are currently working on restocking the Portuguese edition of Hashimoto’s Protocol on Amazon.) With each passing year since I started my work on the root causes of Hashimoto’s, I’ve seen more and more proof that Hashimoto’s can be reversed by addressing root causes. 🙂
Symptoms of H. pylori Infections
While some individuals may be asymptomatic, there are various symptoms that can be associated with H. pylori, including:
- Acid reflux/GERD
- Food sensitivities
- Anemia, as in low iron or low B12
- Low stomach acid and/or a need for digestive enzymes
- Heartburn
- B12 deficiency
- Difficulty tolerating meat
- Nausea
- Belching
- Bloating
- Prolonged fullness after eating
- Feeling full soon after eating
- Past or current history of ulcers
- Period of high stress recently/around diagnosis
- Thyroid nodules
- TPO/TG antibodies over 500
- Hyperthyroidism
- Pernicious anemia
- Headaches or migraines
- Histamine issues
- Hair loss
- Belching or burping after taking certain supplements
- Muscle pains or weakness
- History of/existing reactive hypoglycemia
- Waking up at night hungry
If you have tested positive for H. pylori on a stool test or have a family or personal history of stomach cancer or ulcers, I encourage you to look into H. pylori. I also encourage you to do so if you have a family member who has been diagnosed with H. pylori or SIBO, has a history of Graves’ disease, has TPO (thyroid peroxidase) antibodies over 500 IU/mL, has developed symptoms after a period of high stress (H. pylori thrives in stress!), has had previous mold exposure, or has taken acid-suppressing medications.
Note: The above list is based on assessments and observations from my clients. While these symptoms can be good indicators of an H. pylori infection, testing can be helpful to confirm that a person has H. pylori (read on for more information about testing for H. pylori).
How Common is H. pylori?
While only a small percent, perhaps 5-10 percent of those infected, will develop an ulcer with H. pylori, it is thought to affect as many as 50 percent of people worldwide. Many of these people may be considered “asymptomatic,” yet they may have acid reflux, Hashimoto’s, migraines, Graves’, or other conditions that conventional doctors seem to believe are unrelated, but that will disappear and/or improve once the H. pylori is treated. (2-7)
I believe that similar to all autoimmune triggers, H. pylori is part of the perfect storm in a genetically susceptible and vulnerable individual.
A 2013 Chinese study found a rate of H. pylori infection in 66 percent of people with Graves’ disease and 37.7 percent of people with Hashimoto’s. (6) As the rate of H. pylori in controls was 32 percent, the researchers concluded that H. pylori was not likely a causative factor for Hashimoto’s – but of course, they did not perform deeper tests such as genetic tests on the controls to determine if the controls had the correct genetic predisposition to develop Hashimoto’s after an infection.
After all, we know that autoimmunity develops due to a combination of genes and triggers. Additionally, the researchers didn’t perform antibody studies, conduct before and after studies of thyroid function, nor test for autoimmune markers after treating H. pylori in those with Hashimoto’s… Deeper studies have found cross-reactive antibodies with Hashimoto’s and H. pylori. (22)
These deeper studies also found better absorption of thyroid hormones, a reduction of thyroid antibodies, and in some cases, improvements in TSH, following the eradication of H. pylori! (2-5) I’ll share more about this later in this article, but for now, I wanted to mention that this is why I look at hundreds of studies and patient cases before I dismiss a trigger after just one study. 😉
Interestingly, I saw a similar rate of H. pylori when I reviewed around 300 GI-MAP stool pathogen tests that I conducted with my clients and readers with Hashimoto’s over a three year period. I found H. pylori tests to be positive in 21 percent of people.
I previously would only recommend treating H. pylori if someone had a positive test result for it. However, as I began speaking to other clinicians about this test, I learned that some clinicians treat any detected levels of H. pylori with more natural, gentle protocols (instead of antibiotics). The GI-MAP test reports on the various bugs that live in our stools and will mark a test as positive when the threshold of the DNA of the particular bug is above a lab determined marker, but will also let clinicians know if any DNA of H. pylori is present.
When looking at the results of people who had any level of H. pylori on the GI-MAP (not just what the lab showed to be positive), it ended up being 33 percent of people that had the pathogen present.
I’ve had H. pylori a few times myself. Treating it has helped me reduce my thyroid antibodies, reduce acid reflux and food sensitivities, eliminate voice hoarseness, and get rid of headaches.
In my own practice, I’ve also had numerous readers and clients with Hashimoto’s report that their symptoms were greatly improved following the treatment of an H. pylori infection. Most of them showed a reduction in thyroid antibodies following the eradication of H. pylori; a few even put their Hashimoto’s into remission!
Here are some messages from my readers and clients:
- “I have been reading your book and decided to tackle any infections in my body… through this investigation I found I had H. pylori and two tooth infections. I have taken care of these infections to the best of my knowledge… a few weeks later my hair-loss is at an all time low!! Yessss… and with the addition of T3 my hair texture feels better too. I wouldn’t have known to look into this so thank you! On I go to the next step of healing my gut now!”
- “Dr. Izabella, I think you are on the right track… I have had Hashimoto’s for 20 years… recently I found out I had H. pylori. I have done the antibiotic treatment and my TPO just came back 17 kU/L! I think the antagonist has been killed off! Haven’t felt this good in 20 years!”
- “I have an exciting update! Last week I finished the H. pylori protocol you recommended and am now migraine free for almost two months! My joint pain is gone too! I just tested my antibodies, and they’ve gone from 953 to 366 kU/L!”
- “After 20 years of having Hashimoto’s, I was treated for H. pylori. I feel better than ever; my TPO antibodies are in the normal range, and my doctor just reduced my medication!”
Studies on Antibodies and H. pylori
Antibodies produced in response to H. pylori can cross-react with many normal tissue antigens, such as gastric cells and even thyroid tissue.
Studies have shown antibodies to H. pylori were found in 46.5 percent of patients with Hashimoto’s in a small study in Iran, compared to just 11 percent in the general population. (1)
Research has shown that the level of TPO antibodies was higher in people with Hashimoto’s with H. pylori, compared to those without H. pylori, though there was no correlation between TG (thyroglobulin) antibodies and those with H. pylori. (4,5)
In another study, researchers tested 25 patients with TPO antibodies greater than 700 kU/L (or 700 IU/mL). Of the participants, 72 percent tested positive for H. pylori via a urea breath test. (23) (So if those antibodies of yours are >700 IU/mL, get checked for H. pylori STAT!)
Researchers in Italy identified 10 patients with Hashimoto’s and H. pylori. They treated half of the patients with medications to eradicate the infection, and did not treat the other half. The results were astonishing – the people who were treated for H. pylori saw a 50-78 percent reduction in TPO antibodies, as well as a significant reduction in symptoms! (23)
One patient with H. pylori who started with a TPO antibody count of 4745 kU/L and TG antibody count of 1783 kU/L, was able to see a reduction in TPO antibodies, from 4745 to 45 kU/L, over the course of 21 months; and TG levels from 1783 to 94 kU/L, with treatment for the infection.
The person was tested a total of six times — at the start of treatment, three months in, then nine, 14, 16, and 21 months after eradication. A pattern of reduction was seen within three months, and between month 16 and 21, the TPO count dropped from 100 kU/L to 45 kU/L, while TG dropped from 283 kU/L to 94 kU/L.
The other patients in the treatment group also showed patterns of reduction in TPO and TG antibodies. Reduction in TPO antibodies ranged from 50 to 99 percent, while reduction of TG antibodies ranged from 31 to 95 percent over the course of 17 to 22 months. (23)
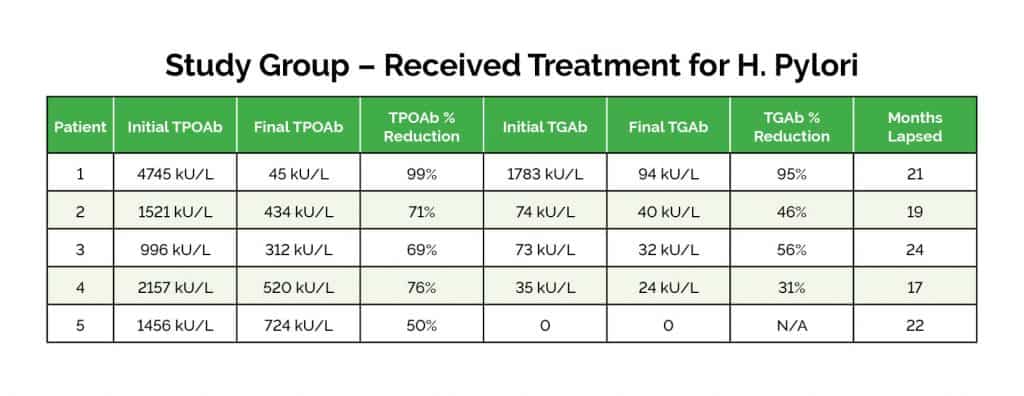
(Source: Bertalot et al, 2004)
The five patients with Hashimoto’s and untreated H. pylori continued to have high TPO and TG levels. One person’s TPO antibodies stayed the same, another person’s decreased, while the three others had theirs decreased between 5 to 26 percent. Three people saw an increase in TG antibodies from baseline, and the other two saw a decrease of 6 percent and 16 percent over the course of 9 to 28 months.
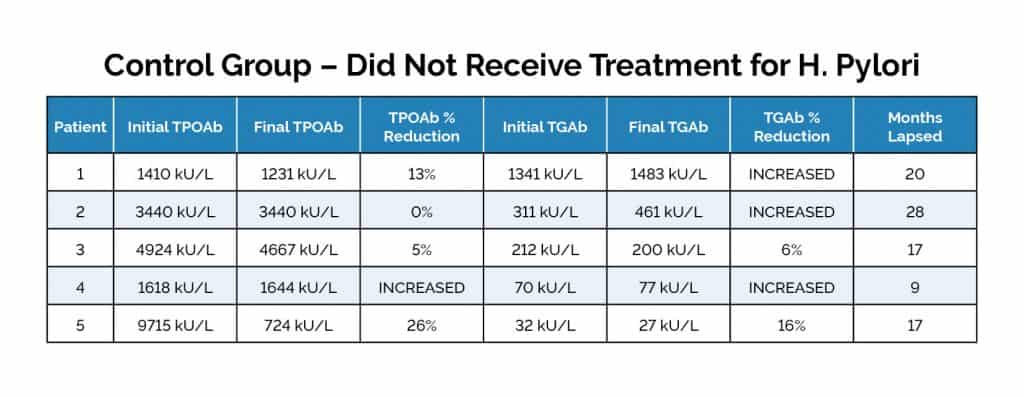
(Source: Bertalot et al, 2004)
The treatment used in this study was known as the triple antibiotic therapy:
- Amoxicillin – 1000 mg twice per day, for 7 days
- Clarithromycin – 500 mg twice per day, for 7 days
- Esomeprazole – 20 mg twice per day, for 7 days
(If you’re wondering why the researchers did not treat everyone, it turns out that the five controls all refused H. pylori treatment! Four did not have symptoms, and one was allergic to antibiotics.)
Autoimmune Gastritis, Hashimoto’s, and H. pylori
Autoimmune gastritis is a chronic inflammatory condition that often results in B12 and iron deficiency, low stomach acid, cancerous gastric lesions, and the destruction of parietal cells of the corpus and fundus of the stomach. Parietal cell antibodies (PCA) are the self-antibodies that are produced in autoimmune gastritis. (24)
This condition was previously reported to affect 10 to 40 percent of people with Hashimoto’s. (25) A 2014 study looked at the co-occurring rates of autoimmune gastritis in people with Hashimoto’s, as autoimmune gastritis may contribute to the malabsorption of thyroid medication and require a person to need a higher dose of thyroid hormone. (26)
Fifty-five people with Hashimoto’s had their B12, ferritin (iron storage protein), and PCA levels measured. Of these people, 12.9 percent were found to have PCA, and all of them had an H. pylori infection. Interestingly, six months after these patients were treated for H. pylori, their PCA antibodies reversed, and they no longer met the diagnostic criteria for autoimmune gastritis.
The researchers thought it was peculiar that all of the PCA antibodies were due to an H. pylori infection and probably not due to “per se” autoimmune gastric damage. I think they missed the forest for the trees, as H. pylori has been implicated as a trigger for autoimmune thyroid disease!
I can’t locate the reference at the moment, but another study found autoimmune gastritis (AIG) to be present in 33.3 percent of people with autoimmune thyroid disease. In this study, around 40 percent of the patients had an H. pylori infection. Anti-parietal cell antibodies were correlated with TPO antibodies, and parietal cell antigens in the stomach are very similar to the thyroid peroxidase enzyme. I always recommend investigating H. pylori in AIG and B12 deficiency!
Testing for H. pylori
If you have Hashimoto’s and elevated thyroid antibodies and/or signs of autoimmune gastritis, there is a high possibility that you have an underlying H. pylori infection. You have a few different testing options available to you, which include the following:
- Blood tests: Blood tests are available for antibodies to H. pylori, but they may not always differentiate between past and current infections.
- Breath tests: Conventional doctors may recommend an H. pylori breath test, but a positive result will only be found in severe cases.
- Stool antigen tests: I prefer stool antigen tests like the GI-MAP test, which can uncover many additional low-grade infections. Such advanced functional medicine tests often require the ordering practitioner to have an account set up with them. You can order them through a functional medicine practitioner, or self-order them through options such as Direct Labs, MyMedLab, or Rupa Health. (Note: self-order options are generally not insurance reimbursable.)
H. pylori Protocols
When it comes to treating an H. pylori infection, pharmacological and natural treatment options are available.
Pharmacologic Treatments
Pharmacologic treatments are generally based on using acid-suppressing medications combined with two to three antibiotics – or as I like to call them, “the big guns.” Multiple drugs are used due to the issue of antibiotic resistance.
- Triple Therapy Option 1: omeprazole, amoxicillin, and clarithromycin (OAC) for 10 days, as directed by your doctor and pharmacist
- Triple Therapy Option 2: bismuth subsalicylate, metronidazole, and tetracycline (BMT) for 14 days, as directed by your doctor and pharmacist
- Triple Therapy Option 3: lansoprazole, amoxicillin, and clarithromycin (LAC), which has been approved for either 10 days or 14 days of treatment, as directed by your doctor and pharmacist
- Quadruple Therapy: Proton pump inhibitor, bismuth, tetracycline, and metronidazole, as directed by your doctor and pharmacist
Please note: Most doctors will prescribe triple therapy or quadruple therapy to address this pathogen in the presence of a positive breath test and symptoms.
The above-mentioned treatments can take a toll on your gut health, leading to further dysbiosis. Adding an S. boulardii supplement to this treatment can increase the rates of eradication, and reduce the rates of dysbiosis from the use of antibiotics.
Natural alternative protocols are also effective for suppressing H. pylori. They may take longer, but are more gentle on your gut flora. Of course, the choice is between you and your doctor as to which path to take.
Natural Treatment Options
Some physicians may not recommend antibiotic treatments when H. pylori is found through a stool antigen test, or when a person is asymptomatic – but you may benefit from the use of herbal protocols to address such an infection.
There is a vast variety of natural treatments and remedies that can be used for H. pylori.
The most well known protocol used by functional medicine practitioners is focused on using mastic gum and DGL. (31)
- Mastic gum has been used traditionally to help treat stomach pain, and modern research has shown it to be effective against multiple strains of H. pylori. (32)
- Deglycyrrhizinated Licorice (DGL) is a well-researched botanical that coats and soothes the intestinal lining and also promotes the healing of ulcers, a common complication attributed to H. pylori. (33,34)
I’ve personally had excellent results with many clients and the first time I cleared out H. pylori in myself, using a 60-day natural protocol involving mastic gum, DGL, and S. boulardii.
- S. boulardii is a beneficial yeast that I like using to raise our own body’s immune defenses, and can be helpful in the body’s fight against various infections, including H. pylori. While using it by itself won’t take care of an H. pylori infection, I often like to add it to H. pylori protocols. (35)
I have also used the following research-backed natural therapies for H. pylori, sometimes alone, sometimes in combination, depending on the needs of the client.
- Aloe – One 2014 study in Italy sought to evaluate the antibacterial activity of aloe vera inner gel against both susceptible and resistant Helicobacter pylori strains. (30) The inner gel of leaves of a 5-year-old plant of aloe was extracted and tested against 15 different strains of H. pylori. Fifty percent of the strains were inhibited in their growth by the addition of aloe vera, and researchers determined that aloe vera inner gel expresses antibacterial properties against both susceptible and resistant Helicobacter pylori strains.
- Andrographis – This is an herb often used for immune support, and may also help with fighting Helicobacter pylori. (36)
- Berberine – Berberine has been shown effective in treating Helicobacter pylori strains, including those resistant to antibiotics. (37)
- Black seed oil – This is a natural herb that is being shown in more and more studies to help eradicate H. pylori infections. Black seed oil is derived from the plant Nigella sativa, and has historically been used as a remedy for a variety of health conditions — most notably, for inflammation, cardiovascular health, infections, and skin issues. (38) The antibacterial properties of black seed oil may play a role in the treatment of H. pylori. Thymoquinone (TQ), one of the active compounds found in black seed oil, acts as a biofilm disruptor, meaning that it can break free from the protective coating that H. pylori uses to protect itself, allowing antibacterial components to reach the H. pylori bacteria and eradicate it. (39) What’s more is that black seed oil has been shown to be gastro-protective in both human and rat studies. One rat study specifically looked at gastritis in rats with hypothyroid function, and found that low thyroid function can be a trigger for gastritis. It also found that black seed oil can play a therapeutic role by inhibiting free radical generation and increasing levels of antioxidants that protect against oxidative stress in gastric tissue. (38,39) Most studies on the use of black seed oil to treat various conditions, including infections, have found a dose of two grams per day to be effective. (28,29,40)
- Broccoli sprouts – These have been found helpful in the treatment of H. pylori. (41,42) I recommend checking out your local health food store for broccoli sprouts, or taking a supplement like BroccoProtect by Designs for Health. (Taking broccoli sprouts in supplement form can help ensure your body absorbs glucosinolates and other nutrients properly.) I also like Sungarden’s BrassiPeak broccoli sprouts, which come in a convenient powder form that can be added to your smoothies (and you can use code DRWENTZ to save 5% off your order). In addition to helping with H. pylori, I love recommending broccoli sprouts to boost our detoxification pathways.
- Cabbage juice – I have found cabbage juice, being rich in glutamine, can also help support gut healing and suppress the H. pylori bacteria, allowing the gut to heal and clear the infection. Simply place the cabbage in a masticating juicer and drink four ounces of cabbage juice daily to suppress H. pylori.
- Cranberries – Cranberries (and their juice) have been studied for their abilities to treat H. pylori. Cranberry juice has been the focus of several studies for its ability to inhibit the growth of H. pylori and other bacteria (E. coli and Streptococcus) and for its anti-adhesion activity, which allows the pathogens to be cleared from the digestive tract more easily. (43-47)
- Fish oils – Fish oils have in vitro antibiotic activity against H. pylori, and have also been studied for their anti-inflammatory activity and ability to protect against ulcer formation. (48)
- Herbs and spices – A 2005 paper which reviewed 25 plants concluded that these eight spices had the strongest bactericidal effects against H. pylori (in declining order): turmeric, cumin, ginger, chili, borage, black caraway, oregano, and licorice. The study also showed that turmeric, borage, and parsley, in extract form, prevented the adhesion of H. pylori to the stomach. (49)
- Methylmethionine Sulfonium (MMS) – This is a derivative of the amino acid methionine that is found in raw cabbage. Raw cabbage juice has long been used to treat ulcers. It helps to support the mucosa throughout the gastrointestinal tract. (50,51)
- Oil of Oregano – Supplemental forms of oil of oregano can be helpful with killing H. pylori since it promotes intestinal cleansing and a healthy balance of gut bacteria. It also contains high levels of antioxidants, which may be beneficial for supporting the immune system and the body’s inflammatory response. I often like to use oil of oregano because it’s also helpful for SIBO and yeast, common co-occurring conditions with Hashimoto’s. (52,53)
- Probiotics – I generally use them in conjunction with other protocols (especially antibiotics), as they play an important role in creating a healthy gut environment and may crowd out the mean H. pylori buggers. 😉 (54,55)
- Propolis – Derived from bee pollen, propolis is an interesting option that has shown promise with inhibiting H. pylori. (56)
- Turmeric supplement – Taking a turmeric supplement may help with slowing down the growth of H. pylori. (57)
- Zinc Carnosine – Research has shown zinc to be effective in combating H. pylori, supporting the mucosal layer, and protecting against ulceration. When zinc is combined with the amino acid L-carnosine, the zinc can more effectively penetrate irritated tissue in the gut. (58,59)
- Vitamin C has anti-H. pylori activity and can help with tissue regeneration, in the case of ulcers. (60)
Thyme, mint, purple coneflower, and chamomile are examples of plants which seem to demonstrate anti-H. pylori activity, and plenty of other herbs could offer protection due to their antibacterial properties, although I have personally not used them as standalone treatments. (27)
I also recommend biofilm busters like Systemic Enzymes and NAC. These can also be helpful in addressing a healthy microbial balance because they break up the bacterial colonies. (61,62)
Another thing to keep in mind is that H. pylori can be spread between family members (even furry ones), as well as through breast milk, and we can even get reinfected by using our old toothbrushes! Thus, if you are someone undergoing an H. pylori protocol, it is imperative to throw away your old toothbrush (every two weeks or weekly while you are on the protocol), and even test/treat your family members.
Natural Protocol Options/Dosing
If you’re looking for an option that combines several of the natural therapies in one bottle, I am excited to share that I developed HP Restore for my Rootcology supplement line, which is a combination product that uses therapeutic doses of mastic gum, methylmethionine sulfonium, DGL, zinc carnosine and vitamin C, which support a healthy microbial balance and a healthy gut lining.*
Rootcology HP Restore is designed to provide comprehensive gut support and can be a tool when addressing H. pylori naturally.* I recommend taking two capsules, twice per day, between meals (at least 90 minutes after eating and 45 minutes before eating). Remember to take them 30-60 minutes away from thyroid medications.
This product, like all natural H. pylori protocols, should ideally be used for 8 weeks.
If you prefer standalone products, here are a few options:
Three supplement 60-day protocol:
- Mastic Gum (500 mg): Take two capsules, three times per day (breakfast, lunch, dinner). (It’s available on Fullscript. If you don’t have a Fullscript account, you can sign up with my credentials here.)
- DGL Plus: Take one capsule, three times per day (breakfast, lunch, dinner).
- S. Boulardii: Take two capsules, three times per day (with or without food). S. boulardii is a probiotic yeast that can help eradicate H. pylori. Studies show that it can help balance levels of opportunistic bacteria and yeast in the gut, which can be a side effect from treatments like antibiotics.* (35,63)
Children/Nursing Moms/Those Unable to Tolerate Other Protocols:
Potential options for children/nursing moms and others who can’t tolerate the other protocols include MegaGuard, which contains ginger, artichoke, and licorice, PyloGuard, which supports gut health by using probiotics to rebalance the gut flora, and black seed oil. I suggest trying them individually, or using a combination of the three. MegaGuard and PyloGuard provide doses on the package. For black seed oil, doses as low as one drop per day have been helpful in children, but I recommend checking with your practitioner. (39,64-67)
I have personally used black seed oil for the two additional flares of H. pylori I had after the birth of my son. I’ve always considered childbirth to be an important Hashimoto’s trigger and exacerbating factor, and boy, do I now know why! Here are some alternative protocols I had to seek out for myself while nursing my son.
Flare #1
Around four months after the birth of my son, I started to experience hair loss and new food sensitivities. I also found that my voice was becoming more hoarse. I tested my thyroid antibodies and they were elevated above 100 IU/mL — my Hashimoto’s was no longer in remission! (Under 100 IU/mL is considered in remission by many professionals.)
While the antibodies weren’t as high as they were when I first started my journey (at over 2000 IU/mL), I was concerned. I wasn’t sure if the Hashimoto’s was flaring up, or if it was postpartum thyroiditis. Luckily, I knew a thing or two about reducing Hashimoto’s antibodies and getting Hashimoto’s back into remission (the same principles apply to postpartum thyroiditis).
At that point, I tested myself with the GI-MAP test and found that I had H. pylori. I was excited because I knew that treating this infection usually results in a reduction of thyroid symptoms and thyroid antibodies, but wasn’t sure about which protocol I would use, as many of the treatments I would typically use for H. pylori are not safe to take while breastfeeding. I reached out to my friend and colleague Dr. Maya Shetreat-Klein, and learned that black seed oil could be used against H. pylori. Within a few weeks, my hoarse voice was gone, my hair stopped falling out, and my follow-up tests showed no more H. pylori.
Flare #2
I had a flare of H. pylori during the initial 2020 quarantine period. This time I found myself waking up at night with burning in my throat, headaches, acid reflux (for the first time since 2011, when I cut out dairy, and an overall feeling that I just wasn’t digesting my foods). I decided to try black seed oil again. However, this time I used a gel capsule, instead of a liquid, and this helped my symptoms somewhat, but not all the way. I went back to the liquid version, and added zinc carnosine and DGL.
While it’s ultimately up to you and your practitioner as to the right protocol to choose, I generally advise my clients to think about their symptoms, past reactions to antibiotics, and health timeline when choosing a treatment approach. For example, if someone had a prior negative reaction to antibiotics, they may want to consider the alternative route; and if someone felt an urgent need to address their infection due to severe symptoms, taking antibiotics may be a faster and more appropriate approach.
Monitoring Your Thyroid Hormones When Taking Herbal Supplements
Whenever you start a lifestyle or complementary intervention to address Hashimoto’s, I encourage you to work with your doctor to monitor your thyroid symptoms, thyroid hormones, and thyroid antibodies. This is a great idea for any lifestyle intervention, but a must for lifestyle changes that could impact your TSH, especially if you are already taking thyroid medications.
Mastic gum may help with reducing H. pylori-induced malabsorption of thyroid hormones, and may result in lowered requirements of thyroid hormones. (68) Similarly, berberine, aloe, and black seed oil can have thyroid-modulating activity and may result in needing to adjust thyroid medications. (69-72)
So as you move forward with supplementation, please look out for the following symptoms of being overmedicated: rapid or irregular heartbeat, nervousness, irritability or mood swings, muscle weakness or tremors, diarrhea, heat intolerance, menstrual irregularities, hair loss, weight loss, insomnia, chest pain, and/or excessive sweating.
I recommend testing thyroid hormone levels every six to 12 weeks to ensure your thyroid medication dosage is optimized, or sooner, if you are showing any of the above symptoms. Thyroid medications are goldilocks hormones – they need to be used in just the right dose!
Testing TSH, T4, T3, and the two most common Hashimoto’s antibodies (TPO and TG antibodies – you can read more about thyroid tests here) is an important part of ensuring that the lifestyle changes you are making are both safe and helpful. 🙂
If your doctor is ordering these thyroid labs for you, be sure to request a copy so that you can see them for yourself and ensure that they are interpreted correctly. If you aren’t able to use your physician for ordering, you may also wish to self-order your own thyroid monitoring labs. I recommend the Ulta Labs thyroid panel for monitoring your progress, which can be ordered anywhere in the U.S. (Some, but not all, insurance companies may reimburse you for self-ordered labs, so please be sure to check with your plan.)
The Takeaway
Gut infections lie at the root of many cases of Hashimoto’s, and eliminating the source of these infections can bring a relief of symptoms — and even remission — to many people. H. pylori is one of the most common infections that we see in those with thyroid conditions, and studies show that even those that are asymptomatic may still be harboring the infection.
The good news is that, once identified, H. pylori can be eradicated through a combination of antibiotics, or through more natural herbal treatments, and health is usually greatly improved!
For more information on treating H. pylori and other gut infections, I encourage you to pick up a copy of my book Hashimoto’s Protocol.
I’d love to hear from you! Have you been tested for H. pylori? What has your experience been?
P.S. You can download a free Thyroid Diet Guide, 10 thyroid-friendly recipes, and the Nutrient Depletions and Digestion chapter of my first book for free by signing up for my newsletter. You will also receive occasional updates about new research, resources, giveaways, and helpful information.
For future updates, make sure to follow me on Facebook, Instagram, TikTok, and Pinterest too!
References
- Aghili R, Jafarzadeh F, Bhorbani R, et al. The association of Helicobacter pylori infection with Hashimoto’s thyroiditis. Acta Med Iran. 2013;51(5):293-6.
- Bassi V, Marino G, Iengo A, Fattoruso O, Santinelli, C. Autoimmune thyroid diseases and Helicobacter pylori : The correlation is present only in Graves’s disease. World Journal of Gastroenterology. 2012;18(10):1093-7. doi:10.3748/wjg.v18.i10.1093.
- Bassi V, Santinelli C, Iengo A, Romano C. Identification of a correlation between Helicobacter pylori infection and Graves’ disease. Helicobacter. 2010;15(6):558-62. doi:10.1111/j.1523-5378.2010.00802.x.
- de Luis D, Varela C, de La Calle H, et al. Helicobacter pylori infection is markedly increased in patients with autoimmune atrophic thyroiditis. Journal of Clinical Gastroenterology. 1998;26(4):259-63. doi:10.1097/00004836-199806000-00008.
- Franceschi F, Satta M, Mentella M et al. Helicobacter pylori infection in patients with Hashimoto’s thyroiditis. Helicobacter. 2004;9(4):369. doi:10.1111/j.1083-4389.2004.00241.x.
- Shi W, Liu W, Zhou X, Ye F, Zhang G. Associations of Helicobacter pylori infection and cytotoxin-associated gene A status with autoimmune thyroid diseases: A meta-analysis. Thyroid. 2013;23(10):1294-300. doi:10.1089/thy.2012.0630.
- Arslan M, Ekiz F, Deveci M et al. The relationship between cytotoxin-associated gene A positive Helicobacter pylori infection and autoimmune thyroid disease. Endocrine Research. 2015;40(4):211-214. doi:10.3109/07435800.2015.1015727.
- Rojas M, Restrepo-Jiménez P, Monsalve DM, et al. Molecular mimicry and autoimmunity. J Autoimmun. 2018;95:100-123. doi:10.1016/j.jaut.2018.10.012
- Pacheco Y, Acosta-Ampudia Y, Monsalve DM, Chang C, Gershwin ME, Anaya JM. Bystander activation and autoimmunity. J Autoimmun. 2019;103:102301. doi:10.1016/j.jaut.2019.06.012
- Fasano A. Leaky gut and autoimmune diseases. Clin Rev Allergy Immunol. 2012;42(1):71-78. doi:10.1007/s12016-011-8291-x
- Disanto G, Chaplin G, Morahan JM, et al. Month of birth, vitamin D and risk of immune-mediated disease: a case control study. BMC Med. 2012;10:69. Published 2012 Jul 6. doi:10.1186/1741-7015-10-69.
- Ferrari SM, Fallahi P, Antonelli A, Benvenga S. Environmental Issues in Thyroid Diseases. Front Endocrinol (Lausanne). 2017;8:50. Published 2017 Mar 20. doi:10.3389/fendo.2017.00050
- Kharrazian D, Herbert M, Vojdani A. Immunological Reactivity Using Monoclonal and Polyclonal Antibodies of Autoimmune Thyroid Target Sites with Dietary Proteins. J Thyroid Res. 2017;2017:4354723. doi:10.1155/2017/4354723
- Knezevic J, Starchl C, Tmava Berisha A, Amrein K. Thyroid-Gut-Axis: How Does the Microbiota Influence Thyroid Function?. Nutrients. 2020;12(6):1769. Published 2020 Jun 12. doi:10.3390/nu12061769
- Yu M, Zhang R, Ni P, Chen S, Duan G. Efficacy of Lactobacillus-supplemented triple therapy for H. pylori eradication: A meta-analysis of randomized controlled trials. PLoS One. 2019;14(10):e0223309. Published 2019 Oct 2. doi:10.1371/journal.pone.0223309
- MIHAI CĂTĂLINA. Lactobacillus reuteri – an alternative in the first-line of helicobacter pylori eradication. FARMACIA. 2019;67(5):871-876. doi:10.31925/farmacia.2019.5.17
- Hellstrom PM. This year’s Nobel Prize to gastroenterology: Robin Warren and Barry Marshall awarded for their discovery of Helicobacter pylori as pathogen in the gastrointestinal tract. World J Gastroenterol. 2006;12(19):3126-3127. doi:10.3748/wjg.v12.i19.3126
- Konturek JW. Discovery by Jaworski of Helicobacter pylori and its pathogenetic role in peptic ulcer, gastritis and gastric cancer. J Physiol Pharmacol. 2003;54 Suppl 3:23-41.
- Charisius, Hanno. When Scientists Experiment on Themselves: H. pylori and Ulcers. Scientific American. July 5, 2014. Accessed August 8, 2022. https://blogs.scientificamerican.com/guest-blog/when-scientists-experiment-on-themselves-h-pylori-and-ulcers/
- Helicobacter Pylori in Peptic Ulcer Disease. National Institutes of Health Consensus Development Conference Statement, February 7-9, 1994. National Institutes of Health. Accessed August 8, 2022. https://consensus.nih.gov/1994/1994HelicobacterPyloriUlcer094html.htm
- Pincock, Stephen. Nobel Prize winners Robin Warren and Barry Marshall. The Lancet. October 22, 2005. Accessed August 8, 2022. https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(05)67587-3/fulltext
- Choi YM, Kim TY, Kim EY, et al. Association between thyroid autoimmunity and Helicobacter pylori infection. Korean J Intern Med. 2017;32(2):309-313. doi:10.3904/kjim.2014.369
- Bertalot G, Montresor G, Tampieri M, et al. Decrease in thyroid autoantibodies after eradication of Helicobacter pylori infection. Clin Endocrinol (Oxf). 2004;61(5):650-652. doi:10.1111/j.1365-2265.2004.02137.x
- Neumann WL, Coss E, Rugge M, Genta RM. Autoimmune atrophic gastritis–pathogenesis, pathology and management. Nat Rev Gastroenterol Hepatol. 2013;10(9):529-541. doi:10.1038/nrgastro.2013.101
- Cellini M, Santaguida MG, Virili C, et al. Hashimoto’s Thyroiditis and Autoimmune Gastritis. Front Endocrinol (Lausanne). 2017;8:92. Published 2017 Apr 26. doi:10.3389/fendo.2017.00092
- Toh BH. Diagnosis and classification of autoimmune gastritis. Autoimmun Rev. 2014;13(4-5):459-462. doi:10.1016/j.autrev.2014.01.048
- Malm, A. et al. Anti-Helicobacter pylori activity in vitro of chamomile flowers, coneflower herbs, peppermint leaves and thyme herbs – a preliminary report. Pharm. Med. Sci. 2018; 28(1): 30-32. doi: 10.1515/cipms-2015-0038
- Farhangi M, Dehghan P, Tajmiri S, Abbasi M. The effects of Nigella sativa on thyroid function, serum Vascular Endothelial Growth Factor (VEGF)-1, Nesfatin-1 and anthropometric features in patients with Hashimoto’s thyroiditis: a randomized controlled trial. BMC Complementary and Alternative Medicine. 2016; 16: 471. doi: 10.1186/s12906-016-1432-2
- Bakathir HA, Abbas NA. Detection of the antibacterial effect of Nigella sativa ground seeds with water. African Journal of Traditional, Complementary and Alternative Medicine. 2011;8(2):159–164.
- Cellini L, Di Bartolomeo S, Di Campli E, Genovese S, Locatelli M, Di Giulio M. In vitro activity of Aloe vera inner gel against Helicobacter pylori strains. Lett Appl Microbiol. 2014;59(1):43-48. doi:10.1111/lam.12241.
- Al Mofleh IA. Spices, herbal xenobiotics and the stomach: friends or foes?. World J Gastroenterol. 2010;16(22):2710-2719. doi:10.3748/wjg.v16.i22.2710.
- Pachi VK, Mikropoulou EV, Gkiouvetidis P, et al. Traditional uses, phytochemistry and pharmacology of Chios mastic gum (Pistacia lentiscus var. Chia, Anacardiaceae): A review [published correction appears in J Ethnopharmacol. 2021 Jun 12;273:113961]. J Ethnopharmacol. 2020;254:112485. doi:10.1016/j.jep.2019.112485
- Murray MT. Glycyrrhiza glabra (Licorice). Textbook of Natural Medicine. 2020;641-647.e3. doi:10.1016/B978-0-323-43044-9.00085-6
- Setright R. Prevention of symptoms of gastric irritation (GERD) using two herbal formulas: An observational study. Informit. https://search.informit.org/doi/10.3316/INFORMIT.950298610899394. Published June 2017. Accessed August 11, 2022.
- Namkin K, Zardast M, Basirinejad F. Saccharomyces Boulardii in Helicobacter Pylori Eradication in Children: A Randomized Trial From Iran. Iran J Pediatr. 2016;26(1):e3768. doi:10.5812/ijp.3768
- Mo ZZ, Wang XF, Zhang X, et al. Andrographolide sodium bisulphite-induced inactivation of urease: inhibitory potency, kinetics and mechanism. BMC Complement Altern Med. 2015;15:238. Published 2015 Jul 16. doi:10.1186/s12906-015-0775-4
- Zhang D, Ke L, Ni Z, et al. Berberine containing quadruple therapy for initial Helicobacter pylori eradication: An open-label randomized phase IV trial. Medicine (Baltimore). 2017;96(32):e7697. doi:10.1097/MD.0000000000007697
- Ahmad A, Husain A, Mujeeb M, et al. A review on therapeutic potential of Nigella sativa: A miracle herb. Asian Pac J Trop Biomed. 2013;3(5):337-352. doi:10.1016/S2221-1691(13)60075-1
- Hashem-Dabaghian F, Agah S, Taghavi-Shirazi M, Ghobadi A. Combination of Nigella sativa and Honey in Eradication of Gastric Helicobacter pylori Infection. Iran Red Crescent Med J. 2016;18(11):e23771. Published 2016 Jun 21. doi:10.5812/ircmj.23771
- Yimer EM, Tuem KB, Karim A, Ur-Rehman N, Anwar F. Nigella sativa L. (Black Cumin): A Promising Natural Remedy for Wide Range of Illnesses. Evid Based Complement Alternat Med. 2019;2019:1528635. Published 2019 May 12. doi:10.1155/2019/1528635
- Chang YW, Jang JY, Kim YH, Kim JW, Shim JJ. The Effects of Broccoli Sprout Extract Containing Sulforaphane on Lipid Peroxidation and Helicobacter pylori Infection in the Gastric Mucosa. Gut Liver. 2015;9(4):486-493. doi:10.5009/gnl14040.
- Brunner S. Helicobacter Pylori Can Be Defeated With Broccoli Sprouts And Thus Preventing Stomach Cancer. Medical News Today website. https://www.medicalnewstoday.com/articles/145177#1. Published April 6, 2009. Accessed August 5, 2020.
- Matsushima M, Suzuki T, Masui A, et al. Growth inhibitory action of cranberry on Helicobacter pylori. J Gastroenterol Hepatol. 2008;23 Suppl 2:S175-S180. doi:10.1111/j.1440-1746.2008.05409.x
- Li ZX, Ma JL, Guo Y, et al. Suppression of Helicobacter pylori infection by daily cranberry intake: A double-blind, randomized, placebo-controlled trial. J Gastroenterol Hepatol. 2021;36(4):927-935. doi:10.1111/jgh.15212
- Hisano M, Bruschini H, Nicodemo AC, Srougi M. Cranberries and lower urinary tract infection prevention. Clinics (Sao Paulo). 2012;67(6):661-668. doi:10.6061/clinics/2012(06)18
- Jensen HD, Struve C, Christensen SB, Krogfelt KA. Cranberry Juice and Combinations of Its Organic Acids Are Effective against Experimental Urinary Tract Infection. Front Microbiol. 2017;8:542. Published 2017 Apr 4. doi:10.3389/fmicb.2017.00542
- Sethi R, Govila V. Inhibitory effect of cranberry juice on the colonization of Streptococci species: An in vitro study. J Indian Soc Periodontol. 2011;15(1):46-50. doi:10.4103/0972-124X.82271
- Drago L, Mombelli B, Ciardo G, De Vecchi E, Gismondo MR. Effects of three different fish oil formulations on Helicobacter pylori growth and viability: in vitro study. JChemother. 1999;11(3):207-210. doi:10.1179/joc.1999.11.3.207
- O’Mahony R, Al-Khtheeri H, Weerasekera D, et al. Bactericidal and anti-adhesive properties of culinary and medicinal plants against Helicobacter pylori. World J Gastroenterol. 2005;11(47):7499-7507. doi:10.3748/wjg.v11.i47.7499
- Cheney G. Rapid healing of peptic ulcers in patients receiving fresh cabbage juice. Calif Med. 1949;70(1):10-15.
- Cheney G. Vitamin U therapy of peptic ulcer. Calif Med. 1952;77(4):248-252.
- Korona-Glowniak I, Glowniak-Lipa A, Ludwiczuk A, Baj T, Malm A. The In Vitro Activity of Essential Oils against Helicobacter Pylori Growth and Urease Activity. Molecules. 2020;25(3):586. Published 2020 Jan 29. doi:10.3390/molecules25030586
- Leyva-López N, Gutiérrez-Grijalva EP, Vazquez-Olivo G, Heredia JB. Essential Oils of Oregano: Biological Activity beyond Their Antimicrobial Properties. Molecules. 2017;22(6):989. Published 2017 Jun 14. doi:10.3390/molecules22060989
- Homan M, Orel R. Are probiotics useful in Helicobacter pylori eradication?. World J Gastroenterol. 2015;21(37):10644-10653. doi:10.3748/wjg.v21.i37.10644
- Ji J, Yang H. Using Probiotics as Supplementation for Helicobacter pylori Antibiotic Therapy. Int J Mol Sci. 2020;21(3):1136. Published 2020 Feb 8. doi:10.3390/ijms21031136
- Baltas N, Karaoglu SA, Tarakci C, Kolayli S. Effect of propolis in gastric disorders: inhibition studies on the growth of Helicobacter pylori and production of its urease. J Enzyme Inhib Med Chem. 2016;31(sup2):46-50. doi:10.1080/14756366.2016.1186023
- De R, Kundu P, Swarnakar S, et al. Antimicrobial activity of curcumin against Helicobacter pylori isolates from India and during infections in mice. Antimicrob Agents Chemother. 2009;53(4):1592-1597. doi:10.1128/AAC.01242-08
- Ibrahim N, El Said H, Choukair A. Zinc carnosine-based modified bismuth quadruple therapy vs standard triple therapy for Helicobacter pylori eradication: A randomized controlled study. World J Clin Cases. 2022;10(1):227-235. doi:10.12998/wjcc.v10.i1.227
- Hewlings S, Kalman D. A Review of Zinc-L-Carnosine and Its Positive Effects on Oral Mucositis, Taste Disorders, and Gastrointestinal Disorders. Nutrients. 2020;12(3):665. Published 2020 Feb 29. doi:10.3390/nu12030665
- Hussain A, Tabrez E, Peela J, Honnavar P Dr, Tabrez SSM. Vitamin C: A Preventative, Therapeutic Agent Against Helicobacter pylori. Cureus. 2018;10(7):e3062. Published 2018 Jul 30. doi:10.7759/cureus.3062
- Li X, Kim J, Wu J, Ahamed AI, Wang Y, Martins-Green M. N-Acetyl-cysteine and Mechanisms Involved in Resolution of Chronic Wound Biofilm. J Diabetes Res. 2020;2020:9589507. Published 2020 Jan 27. doi:10.1155/2020/9589507
- Roy R, Tiwari M, Donelli G, Tiwari V. Strategies for combating bacterial biofilms: A focus on anti-biofilm agents and their mechanisms of action. Virulence. 2018;9(1):522-554. doi:10.1080/21505594.2017.1313372
- Szajewska H, Horvath A, Kołodziej M. Systematic review with meta-analysis: Saccharomyces boulardii supplementation and eradication of Helicobacter pylori infection. Aliment Pharmacol Ther. 2015;41(12):1237-1245. doi:10.1111/apt.13214
- Fahey JW, Stephenson KK, Wallace AJ. Dietary amelioration of Helicobacter infection. Nutr Res. 2015;35(6):461-473. doi:10.1016/j.nutres.2015.03.001
- Raveendra et al. Evidence-Based Complementary and Alternative Medicine 2012, Article ID 216970, 9 pages, 2012.
- Puram et al. Evidence-Based Complementary and Alternative Medicine 2013, Article ID 263805, 8 pages, 2013.
- Holtmann G, Adam B, Haag S, Collet W, Grünewald E, Windeck T. Efficacy of artichoke leaf extract in the treatment of patients with functional dyspepsia: a six-week placebo-controlled, double-blind, multicentre trial. Aliment Pharmacol Ther. 2003;18(11-12):1099-1105. doi:10.1046/j.1365-2036.2003.01767.x
- Dabos KJ, Sfika E, Vlatta LJ, Giannikopoulos G. The effect of mastic gum on Helicobacter pylori: a randomized pilot study. Phytomedicine. 2010;17(3-4):296-299. doi:10.1016/j.phymed.2009.09.010
- Caron P, Grunenwald S, Persani L, Borson-Chazot F, Leroy R, Duntas L. Factors influencing the levothyroxine dose in the hormone replacement therapy of primary hypothyroidism in adults [published online ahead of print, 2021 Oct 20]. Rev Endocr Metab Disord. 2021;1-21. doi:10.1007/s11154-021-09691-9
- Castellana M, Castellana C, Giovanella L, Trimboli P. Prevalence of gastrointestinal disorders having an impact on tablet levothyroxine absorption: should this formulation still be considered as the first-line therapy?. Endocrine. 2020;67(2):281-290. doi:10.1007/s12020-019-02185-4
- Han Z, Cen C, Ou Q et al. The Potential Prebiotic Berberine Combined With Methimazole Improved the Therapeutic Effect of Graves’ Disease Patients Through Regulating the Intestinal Microbiome. Front Immunol. 2022;12. doi:10.3389/fimmu.2021.826067
- Metro D, Cernaro V, Papa M, Benvenga S. Marked improvement of thyroid function and autoimmunity by Aloe barbadensis miller juice in patients with subclinical hypothyroidism. J Clin Transl Endocrinol. 2018;11:18-25. doi:10.1016/j.jcte.2018.01.003
Note: Originally published October 14, 2016, this article has been revised and updated for accuracy and thoroughness.

 Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Dear Izabella! Thank you very much! I dmire you!
Could you please clarify- for natural H.pillory protocol, we should use any of three options, or it need to use all of them ttogether?
Thank you in advance.
Kate- It’s ultimately up to you and your practitioner as to the right protocol to choose, I generally advise my clients to think about their symptoms, past reactions to antibiotics and timeline when choosing a treatment approach. For example, if someone had a prior negative reaction to antibiotics, they may want to consider the alternative route, and if someone felt an urgent need to address the infection due to severe symptoms, taking antibiotics may be a faster and more appropriate approach. Here is an article you may find interesting as well! 🙂
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
Dr. Izabella,
Thank you for all your hard work. I do have a comment. Kate asked you to clarify your statement about the natural protocol, instead you proceed to tell her you could not advice her on any individual medical advice.
Under antibiotic protocols, you wrote 5 different treatments, yet under natural treatments you bundle them all up. Perhaps the description article is not clearly written. Are you saying all 3 natural products are used or are you implying to choose one? Can you please be a little more specific? IMO, Kate did not ask you for personal advice, she asked to clarify part of your article.
Yes, I am very thankful for all your hard work which benefits many people including myself. God Bless you,
Jeannette
Jeannette – thank you for your question. Any time an individual asks any question about what they personally should eat or take as far supplements or medications and I respond that legally becomes direct personal medical advice and jeopardizes my license. I hope you understand. I have to be very careful and responsible. The advice of a skilled personal medical practitioner is always best.
Kate – thank you for following this page. I am not able to give out any direct personal medical advice here. I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
If one has an “gut infection” one should definitely not treat it with conventional antibiotics.
Melissa – thank you for following this page.
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Hi, I have a question. I have recently been told that my Hashimoto antibodies are present at a 340 level. My thyroid is working fine and the hormone output levels are normal. I know the antibodies were triggered due to allergies. I have cut out gluten, dairy and nightshades. I wanted to detoxify my body and started eating lots of fruit, by making fruit juices in a blender. Everytime I have the juice, I get a migraine, I found in your book that you mentioned that there might be an issue with the processing of carbs. I cant tolerate potato or white rice. Please can you let me know if when I am healed, I will be able to tolerate fruit in large quantities, or will I forever have to reduce fruit and carb intake? I also have permanent brain fog, do you think it will ever go away, if i implement your eating regime (protein and fats throughout the day)? thank you so much
Jane – thank you for following this page. Here are a few articles related to diet that hopefully help you get started. Diet is a very individual intervention and will be different for each of us. It’s great that you have discovered some of your food sensitivities so you can avoid them. Here are a few articles related to diet that hopefully help you get started.
LOOD SUGAR IMBALANCES AND HASHIMOTOS
https://thyroidpharmacist.com/articles/blood-sugar-imbalances-and-hashimotos
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
GUT, BRAIN, AND AUTOIMMUNE DISORDERS: THE ROLE OF FOOD
https://thyroidpharmacist.com/articles/gut%C2%A0%C2%A0brain%C2%A0and-autoimmune-disorders
Hello Izabella,
Could you please post the link how I can order tests through your website. I also have troubles to register(it suggests only to change the password, but there is no link to register) even though I am on your email list.
my pilory antibodi is 150 is that normal have infected 10 years ago
t – I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Hi, do you have links/article for a greater explanation of a natural protocol treatment for H Pylori that you can share to help more fully explore that option? I’ve searched before and it’s difficult to find FULL information on what that protocol entails. I think people are interested in exploring but can’t easily find info. Thanks.
Kathy – thank you for following this page. I can understand your frustration. 🙁
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Thanks so much for posting this information. A quick question: For the natural H. Pylori protocol, would someone take the S. Boulardii instead of their regular probiotic supplement (something like https://www.purerxo.com/thyroidpharmacist/rxo/products/product_details.asp?ProductsID=1058) or in addition to other probiotics?
Yvonne – thank you for following this page. I cannot tell you specifically what you can and cannot do over the internet as I could be held liable for what would happen to you.
These articles may be of help!
TOP 4 PROBIOTICS FOR HASHIMOTO’S
https://thyroidpharmacist.com/articles/the-four-best-probiotics-for-hashimotos
USING ENZYMES TO OVERCOME HASHIMOTO’S
https://thyroidpharmacist.com/articles/using-enzymes-to-overcome-hashimotos
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Free Chapter on Depletions and Digestion, Thyroid Diet Quick Start Guide and 10 Nutrient Dense Gluten Free recipes:
https://thyroidpharmacist.com/gift
Dear Izabella,
Thank you so much for the links; they’re really helpful. And thank you so much for all your awesome work!
In the past, I experienced some strong side-effects from and allergies to antibiotics. Therefore, I want to try the natural protocol first and avoid taking antibiotics, if possible.
Thanks for providing all this information on alternative and functional approaches. I wouldn’t know where else to get this help. Your Root Cause book and the Thyroid Secret documentary have given me new hope after ten years of being told that not feeling good would be the new normal for me. (Going gluten free has already helped a lot – with the unexplained IBS symptoms in particular.)
Btw, I also can’t wait to read your new book. It’s been pre-ordered and on its way. 🙂
Dear Izabella!
What is the best way to use Mastic Gum? Just before the meal or earlier, an hour before the meal? Can I take the Mastic Gum and the Probiotic in the same time?
Thank you,
Anna
Hello Dr. Wentz:
Thank you so much for this article.
I’ve been suffering with ulcers and H. Pylori infections for almost 50 years.
Unfortunately, I am unable to take antibiotics except for Cipro and have not had much success at eliminating this horrible infection.
Would you suggest I use the 60 day protocol (I’ve been taking both Mastic Gum and DGL for about a year now and it seems to help, but not at the levels you have suggested.) I also use a 10 billion probiotic daily + make my own coconut yogurt and use 10 billion in a 2 cup batch. Do you think increasing the Mastic Gum, DGL, and taking the s. boulardii would be beneficial in my case?
Your input would be so valuable.
I have both the Root Cause and the Hashimoto Protocol and am in the process of reading them.
Thank you in advance for any advice you could offer.
Blessings,
Louise
Louise – thank you for following this page and for your support. <3
Please, understand that due to liability issues, I am unable to answer specific medical questions.
I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
I’d just like to share my husband’s experience with h.pylori. A friend recommended mastic gum. He personally had had duodenal ulcers, had read about mastic gum and asked his consultant if he could do a trial of mastic gum. The consultant agreed, saying he would examine him again in three months. Anyway, three months later the h.pylori was cleared, and the consultant was impressed. I think the friend continued with a maintenance dose.
So…..when this friend heard that my husband had h.pylori, he felt he could recommend mastic gum.
After using mastic gum, my husband’s breath test still showed positive, which was disappointing. However, apparently if there is atrophic gastritis, which there was (caused by the h.pylori) then there can be a false positive with a breath test. The stool test showed the infection cleared, and then biopsies taken taken during a gastroscopy were also clear. Hope this information helps someone.
Vivien – Thank you for following this page and for sharing. Happy to hear that your husband’s labs were clear!
Hello, what was the dose of Mastic gum daily to clear HPylori? And was it the brand recommended by Dr Wentz?
About 11 years ago I found I had H pilori and was treated with antibiotics. I now have delayed pressure urticaria which doctors have no known cause. I had Graves and had my thyroid destroyed around 2000. They think it is my antibodies attacking my immune system. I am trying to follow the AIP diet and seem to do better. I take Allegra and Singular daily to control welts and have been able to cut dose in half. Have you had any success with DPU?
Marianne – thank you for following this page.
You may be interested in reading…
THE COMMON ROOT CAUSE OF HASHIMOTO’S, HIVES, AND IBS
https://thyroidpharmacist.com/articles/the-common-root-cause-of-hashimotos-hives-and-ibs
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
I would love to see a similar post on SIBO! There is not enough available information right now and understand it’s an underlying cause of Hashimotos.
Oh my.. Passed by kissing? So if I get rid of the h. Pylori I need to ask all future kissing partners for a stool sample first? How do you get around this? ?
As a clinical nutritionist (40+ years) and a “health detective,” I have found that jawbone infection(s) caused by a root canal(s) is very common in cases of Hashimoto’s / Grave’s and other autoimmune conditions. Just curious if you do dental histories on your patients. I have found this to be extremely useful in my practice, particularly after my own root canal nightmare. Dental histories have revolutionized my practice.
Thanks for the outstanding work you’re doing. I will implement your guidelines & experience with H. Pylori and autoimmune conditions / Hashimoto’s in my practice….immediately. I never made this connection although it’s been obvious to me that infection is a leading trigger for autoimmune conditions.
Hi Jim – Thank you for following this page and your support.
Here is some information you may find interesting.
Three things MUST be present in order for autoimmunity to occur…
1. Genetic predisposition
2. Environmental triggers
3. Intestinal permeability (leaky gut)
Developing autoimmunity is like a three-legged stool, all of these factors must be present for autoimmunity to occur! When you remove one of these, you can prevent or stop autoimmune disease. While we can’t change genes, if we know the trigger, we can remove it, and we can heal the gut.
REVERSING AUTOIMMUNITY AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
IS HASHIMOTO’S HYPOTHYROIDISM GENETIC
https://thyroidpharmacist.com/articles/is-hashimotos-genetic
CARRIE’S DENTAL PROCEDURE TRIGGERED HER HASHIMOTO’S
https://thyroidpharmacist.com/articles/carries-dental-procedure-triggered-her-hashimotos
PERIODONTITIS
https://thyroidpharmacist.com/articles/periodontitis-a-trigger-for-hashimotos
Greetings, This is all very interesting information. I not only have hashimoto disease but equally now have developed fibromyalgia, another auto-immune chronic disease. I suspect my fibro arose after an infection. I don’t know about the hashimoto ( which I have for about 15 years) Would you know if one is related to the other? How could I receive treatment for both? I heard I can possibly treat fibro with antibiotics as well. Your help and advice would seriously make a difference in my daily life. I not only live with the symptoms of thyroid disease but equally deal with chronic pain which is at times, debilitating.
Looking forward to your suggestions.
Regards,
Anna
Anna – thank you for following this page. While I only work with patients with Hashimoto’s, oftentimes patients will have additional autoimmune conditions. Most autoimmune conditions have common root causes, and a lot of times the things that are recommended for one autoimmune condition will help with others. Conditions that I have found to respond really well to the Hashimoto’s protocols have been rheumatoid arthritis, lupus, Celiac disease, irritable bowel syndrome, eczema, asthma, Graves’, premature ovarian failure, psoriasis, Alopecia Areata, and Sjogrens. I have also seen the protocols help with Fibromyalgia, chronic fatigue syndrome, PCOS, as well as Type 2 diabetes, Crohn’s, and Ulcerative colitis.
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Where is a good clean resource to buy mastic gum and DGL?
Kathleen – here a couple links to the mastic gum and DGL that I recommended in the article.
DGL
https://www.purerxo.com/thyroidpharmacist/rxo/products/product_details.asp?ProductsID=132
S. boulardii
https://www.purerxo.com/thyroidpharmacist/rxo/products/product_details.asp?ProductsID=1000%E2%80%9D
Mastic Gum
https://www.amazon.com/Allergy-Research-Group-Mastica-Mastic/dp/B001IAEIXG/ref=sr_1_1_a_it?ie=UTF8&qid=1479756922&sr=8-1&keywords=mastica&th=1
Dear Dr. Izabella Wenz,
Regarding the alternative protocol, can I ask you if those three can be taken together at same time since taking each one on an empty stomach (or with 15/20 min difference between) it will be quite impossible for me (it means I can eat basically)?
Thank you very much in advance!
Maria – thank you for following this page. For questions pertaining to the protocols please contact my team at info@thyroidpharmacist.com and they will be happy to help you. 🙂
Dr. Izabella,
I’ve heard you on a few podcasts with Dave aspery, fascinating work that you are doing. I don’t think I have hashimotos, sometimes I seem to have hyperthyroidism, I have trouble sleeping, am always hot, but my lab work always seems to come back normal for thyroid. I was just diagnosed with pylori. Started an herbal route with dgl, mastic gum, bismuth, but my Dr really recommended the triple therapy. Unfortunately my symptoms are significantly worse after antibiotics, serious fatigue which I only felt when I was taking a ppi, now it’s constant. Have you heard of these therapies affecting the thyroid and creating other thyroid issues? I mostly have hot flashes / short of breath / and fatigue issues. My heart rate seems to be about 5-10bpm higher after antibiotics, my resting rate was in the mid 40s, now never below 53. Would love to know your thoughts, maybe a candida overgrowth after antibiotics?
Sam – thank you for following this page. I wish I could give you more direct advice but, each person will react differently. I would advise you to ask your personal pharmacist or a trusted clinician who’s care you are under. I am not able to respond directly to these types of questions here. Graves and Hashimoto’s are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto’s, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people) Hashimoto’s results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually, people with Graves have hyperthyroidism, and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own, and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Here is an article you might also find helpful.
CANDIDA AND HASHIMOTOS CONNECTION
https://thyroidpharmacist.com/articles/candida-and-hashimotos-connection/
Dr. Izabella,
When dealing with H.pylori or SIBO in your opinion is it necessary to take a food allergy test for finding out what specific foods are causing inflammation?
Valerie – thank you for following this page. About 50% of the people with hypothyroid were found to have SIBO in one study, so it’s likely that if you have a thyroid condition, you also have SIBO. While I always prefer to test and not guess, some functional medicine clinicians do recommend treatment based on symptoms alone! This can save time and money, however, the drawback of not testing would be treating something that you didn’t need to treat! The herbal protocol is a long process with a lot of supplements to take. If that doesn’t deter you, then I’d suggest at least testing at the end of treatment to ensure that the SIBO is eradicated. The way that you want to address infections is by starting with the highest infection in your body first. H. pylori is typically found in the stomach (it can also be in the upper part of the small intestine), so that’s going to be the first infection you want to treat. A lot of times, when you treat H. pylori, the SIBO will go away as well. Next would be the parasite. If, after the H.pylori and parasite protocols you still have SIBO, you would treat it at this time. The yeast would be addressed last, if needed. Sometimes when you use the parasite protocol along with the SIBO protocols, the yeast issue is taken care of as well. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
https://www.amazon.com/Hashimotos-Protocol-Reversing-Thyroid-Symptoms-ebook/dp/B01HXK6GVQ/ref=sr_1_1?ie=UTF8&qid=1505933035&sr=8-1&keywords=hashimotos+protocol+izabella+wentz
Hi Dr. Izabella,
Thank you so much for these useful and very interesting information. I have hashimoto disease and currently taking levothyroxine. I’m also H.pylori positive. My question is: Do mastic gum supplement and levothyroxine contradict? and How to use them together.
Many thanks.
Olinka – thank you for reaching out. I wish I could give you more direct advice but, each person will react differently. I would advise you to ask your personal pharmacist or a trusted clinician who’s care you are under. I am not able to respond directly to these types of questions here. I also don’t recommend starting multiple supplements all at once. I recommend starting one at a time, and then adding another a week or so later once it has been confirmed that the first supplement is not causing any harm.
I do have a full supplements chapter in my book. Have you checked it out? Not everyone should be taking every supplement and the book will help uncover your root cause. This will help you figure out your supplementation.
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8…
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hi Izabella,
I have been following your recipes. I have peroxidase antibodies of 43.6 the top of the range is 35. I have tsh of 3.32. This was tested 13th of August. I had a hpylori infection discovered the 18th of August (because I had stomach pain for 2 years and I thought it was connected to the raised antibodies). I retested on 23rd October. H pylori specific ag. (stool) Negative No evidence of active H pylori infection.
I had burning pain and hair loss from everywhere for 21 months. Still suffering from hair loss and massive hair thinning/fine. Have lost 70% of hair still going.
I am gluten free.
1. How long after this eradication should I wait to retest my thyroid?
2. Do you think there is a possibility it will decrease my antibodies?
3. How much do you think it could decrease it by?
4. Will a decrease in antibodies then cause the TSH to decrease to close to 1? Does it have an impact on tsh levels dropping to optimal levels as well or only antibodies?
I live in the UK and they won’t give me any treatment not bad enough in their opinion.
2 years ago in the first week of February I got swine flu for a week lost a stone of weight in a week. 3 weeks prior had huge stress levels. Hair that I noticed falling out started 24th May. But the hair condition changed completely in February 2016 (tangled dry).
I didn’t go for any testing until (was first apt I could get) June 2016, they tested my tsh and t4 Serum free T4 level 19.4 Pmol/l 12.0-22.0
Serum TSH level 3.18 mU/l 0.3-4.5
This test was 4 months after the flu.
The flu affected only my throat. could not swallow. could not move. extremely painful for the week. was hoarse for 2 weeks. took at least 2-3 months to put the weight back on and get appetite back.
5. Do you think this may have been sub acute thyroiditis before hashimitos?.
I am not sure but I probably noticed the stomach pain around feb/march 2016 time as well.
other tsh and t4 tests between june 2016 and aug 2017 were:
Test Date 21st October 2016 3.19pm (GP)
Serum free T4 level 14.9 Pmol/l 12.0-22.0
Serum TSH level 5.24 mU/l 0.3-4.5
Test Date 6th January 2017 3.33pm (GP)
Serum free T4 level 15.6 Pmol/l 12.0-22.0
Serum TSH level 2.07 mU/l 0.3-4.5
Test Date 11th May 2017 at 3pm (GP)
Serum free T4 level 16.3 Pmol/l 12.0-22.0
Serum TSH level 2.13 mU/l 0.3-4.5
thank you.
jay – thank you for reaching out. I am sorry I am not able to respond directly to these types of questions here. I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
I had h pylori for 2 years. treatment I had, 5 days of amoxicillin 3 times a day plus ppi. followed by triple therapy for 7 days. I also took probiotic once a day and 2 mastic gums 3 times a day. also took aloe vera. hope this helps anyone going through it. 6 weeks after treatment I am clear. stomach pain is gone no more burning, I eat regular and a lot more. I had vomiting and diahrea during the treatment but it was fine I could eat straight after I was sick.
However, I have recent pain in my kidney areas both sides. had flu injection a week ago first felt this pain 2 days after it, so I wonder if it is connected. going to monitor it.
I had a scan on kidney’s 6 weeks before when first went to hospital about the stomach pain, I had white blood cells in urine. they thought I may have a kidney infection. they did a cat scan and said I had no kidney stones. pain was only in one side then so not sure if they would have done both kidneys. they gave me one antibiotic then for it. pain at the moment is in both. I have clear urine when I go to the toilet at the moment. am drinking lemon juice and water to help flush them out. not sure if pain is kidneys but will monitor and ask Dr to check on Monday and advise what tests they may want to do if it is still here then.
Hi Izabella – thank you for this information! Can I ask how you treated your own h pylori infection?
Thanks!
Kerri
Kerri – thank you for following this page. Here is an article you may find interesting.
MY HASHIMOTO’S AND HYPOTHYROIDISM JOURNEY
https://thyroidpharmacist.com/articles/my-hashimotos-and-hypothyroidism-journey
Hi I m Akshay.I am 29 years old.Since 15+ years,I have constipation or could I say Obstipation, and irregular,(IBS-C) incomplete bowel movement.
I m diagnosed with Hypothyroidism since 3 years.
Recently diagnosed with Antral Gastritis and duodenitis.
Stool antigen test for H Pylori is negative.When I brush my teeth all the Brush covers with toothpaste+spit.My spit always forms strings.
I have bloating,fatigue,burping,yawning and cramps all over body.
Should I take Masticgum+DGl+…?
Which other tests shd I do for Bacteria and fungus?
Some antibiotics used for Cough are useful for relieving constipation for me,in short term.
Please help!!
Akshay – Thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms. Here are some links which might help:
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
MY RECENT CHALLENGES AND FINDING DR. RIGHT
https://thyroidpharmacist.com/articles/my-challenges-and-finding-dr-right/
Could you provide the link to the italian study that reduced antibody levels?
Thomas – thank you for following this page. At the bottom of each article, there are several references listed where I collected my information from. I would encourage you to check them out!
I’m trying, but it is quite hard to figure out which one is the Italian one. Just let me know that.
if someone has hashimotos and h pylori do you treat the h pylori first and foremost ignoring that alot of the natural means to irradicate h pylori is not good for the thyroid/hashimotos and for how long is it safe to do so…i.e. cabbage juice, broccoli sprouts, etc….thanx for the reply
John – thank you for reaching out! Most goitrogens are okay, with the exceptions of soy and millet as I mention in my article on goitrogens, as most people with Hashimoto’s are not iodine deficient, especially those in developed countries. So, those you mentioned should be fine for you if you have Hashimoto’s. Here is an article you may find helpful as well: https://thyroidpharmacist.com/articles/what-are-goitrogens-and-do-they-matter-with-hashimotos/
H. pylori is a stubborn infection. I’ve found that some clients are successful in treating their H. Pylori by using a combination of herbal products such as Mastic Gum, DGL, S. Boulardii, and Rootcology Amino Support, among other products. You might also appreciate my book, Hashimoto’s Root Cause. The book has an entire section dedicated to infections and the various options for treatment. This 380-page guide helps people figure out their own root cause. It covers birth control, gut infections, the thyroid, adrenals, hormones, toxins, food sensitivities, medications, diet, tests/assessments you can do, etc. It will save you a lot of time and frustration, and so far it has helped a lot of people to feel better. You may also want to check out my new book Hashimoto’s Protocol, a more step by step in-depth plan that streamlines the most effective interventions. ?
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hello people, I follow Dr. Wentz a lot, got her book, recipes, read her articles, etc. I recently came positive for H. Pylori, which is why I am writing here today.
All I wanted to say is, if some of you follow the natural protocol for this, it would real nice for other people to read about your experience, detailed steps and results.
Well, that’s just my opinion anyway.
Thanks and take care!
Sara – thank you so much for sharing your journey with me! <3 I understand how hard this can be. H. pylori is a stubborn infection. I’ve found that some clients are successful in treating their H. Pylori by using a combination of herbal products such as Mastic Gum, DGL, S. Boulardii, and Rootcology Amino Support, among other products. You might also appreciate my book, Hashimoto’s Root Cause. The book has an entire section dedicated to infections and the various options for treatment. This 380-page guide helps people figure out their own root cause. It covers birth control, gut infections, the thyroid, adrenals, hormones, toxins, food sensitivities, medications, diet, tests/assessments you can do, etc. It will save you a lot of time and frustration, and so far it has helped a lot of people to feel better. You may also want to check out my new book Hashimoto’s Protocol, a more step by step in-depth plan that streamlines the most effective interventions. ?
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
What are your thoughts on Matula Tea for H. Pylori?
Brenna – thank you for reaching out. <3 That is a very interesting question. I haven't seen any papers on this topic yet but I will add it to my research list.
Hi. I was directed here by The Hashimotos 411 Facebook group because I have been diagnosed Hashimoto’s/with graves antibodies. I’m on the AIP diet and I have been doing really well. However I have now also been diagnosed with H pylori. So, I ordered these supplements . Now I’ve had a reaction to one of them. I’m thinking it’s the DGL plus. I started having heart palpitations last night as I lay down and I could not sleep. 🙁 What could it be?
Jann – thank you so much for reaching out and sharing your journey. I’m glad you have found support with the Hashimoto’s Facebook group and are feeling better with the diet changes. I would recommend that you stop the supplements and contact your practitioner who’s care you are under for advise on continuing. <3 Graves and Hashimoto's are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto's, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people) Hashimoto's results in hypothyroidism and is usually treated with Synthroid and replacement hormone. The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually, people with Graves have hyperthyroidism, and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own, and these people end up on Synthroid as well. Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. I hope this helps! You may find these resources helpful as well.
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Food Pharmacology
https://www.amazon.com/Hashimotos-Food-Pharmacology-Nutrition-Protocols/dp/0062571591?tag=thyroipharma-20
My TPO antibodies test results have been >1300 since I was diagnosed. They have not dropped since eliminating gluten, sugar or diary. Since dietary changes, I have commenced LDN for 18 months and also switched to a T3/T4 NDT combo…
I was diagnosed with H.Pylori and have had two treatments of triple antibiotic therapy – however, no improvement of TPO antibodies.
I have also tried black seed oil and probiotics, to no avail.
What else can I do??
Elle – thank you for reaching out and sharing your journey.❤️ I understand how hard this is. Hashimoto’s is often a combination of food sensitivities, nutrient deficiencies, adrenal issues, gut issues as well as an impaired ability to get rid of toxins. Any of those things would prevent a person from getting better. Hashimoto’s is very much an individual condition. While there are root cause commonalities, each person will have their own or in some cases, more than one root cause. You will have to start with the simplest modifications, by removing triggers, followed by repairing the other broken systems to restore equilibrium, allowing the body to rebuild itself. You will need to dig down to why the immune system is imbalanced in the first place and this will tell you how you begin to finally feel better, reduce your thyroid antibodies and even take your condition into remission. You will have to create your own health timeline. Look back at your overall history as far back as you can remember. Look for infections, periods of severe stress, the use of medications (especially antibiotics, antacids, and oral contraceptives), accidents, and exposure to toxins. These are events that may have contributed to Hashimoto’s. Once you do, you will know what types of changes you need to implement to make yourself feel better. If you need further support, please check out the list of lab tests inside the “Testing” chapter of my book, Hashimoto’s Root Cause. I also offer a 12-week program, Hashimoto’s Self Management Program. Here are some resources I hope you find helpful as well.
BUILDING YOUR OWN HEALTH TIMELINE
https://thyroidpharmacist.com/sample-health-timeline/
Hashimoto’s Self-Management Program
https://thyroidpharmacist.com/enroll-in-hashimotos-self-management/
Thank you for this wonderful article – very thorough and informative!
I had one GI-MAP test 3 years ago- which actually you might have used for your study! At the time, there was no H.Pylori virulence factor but H.Pylori was present. I did not seek medical advice and thought I was in the clear (so wrong)!
After a new GI-MAP with similar results a few months ago (H.Pylori present but no virulence factors), I consulted with a naturopath and he – as you mentioned quite a few do – decided to treat the H.Pylori nonetheless (due to all my symptoms). My two-month treatment was Candibactin AR/BR + Klaire Labs Interfase Plus + Microbiome Labs Mega IgG + Gastromend HP + Calcium D Glucarate. I did have some improvement after treatment – my runny and stuffed nose was getting clearer overall. I did have a couple of drinks on holiday and did not react to it (I usually sneeze and have a runny nose within 15 minutes and for the whole night) but otherwise no major improvement in the big categories (brain fog/concentration, energy or constipation).
I also was interested in the studies you mentioned about the decrease of TPO. Mine are elevated due to my Hashimoto’s but did not decrease one bit after treatment: 73 before and after. I wonder why? It’s also interesting to see that you can have TPO in the “remission” zone and still have H.Pylori on stool tests.
I’m due to have a follow-up GI-MAP to check if the H.Pylori is gone soon so I can update if anyone is interested. If still there, I am thinking about trying Matula tea as an alternative and wondered if you have had any personal or clinical experience with it? Or anyone reading this?
I have black seed oil – as I bought it after reading your article about it but never had the chance to try it out but definitely will.
I’m not sure if you’re familiar with the various studies about the link between H.Pylori in the mouth and the gut because they seem to suggest that it might be the reason for re-occurence. I looked into it as I once had antibodies and symptoms of Sjogren’s disease (yes, past tense!). One of them:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4123373/
It’s hard to eradicate in the mouth (I’m planning to use Corsodyl while doing the treament again (if H.Pylori is not gone – Corsodyl’s main active ingredient chlorhexidine digluconate has been proven to erradicate H.Pylori in the mouth though CAUTION the mouthwash can stain teeth and the other ingredients are not “friendly”) but I’m wondering if a double approach “mouth + gut” would not yield better, long-lasting results AND/OR a regular “course” of mouthwash once or twice a year would prevent re-occurence….I would love to know your thoughts on the matter but I know you can reply to every single message so no worries.
Thank you again for your hard work! And happy holidays x
Elle, thank you so much for sharing your journey and what has worked best for you. When it comes to Matula tea and Corsodyl, I have not researched these so I do not have information to share at this time. About 95% of people with Hashimoto’s have elevated Thyroid Peroxidase Antibodies, while 80% will have elevated Thyroglobulin Antibodies. They can both be important in monitoring the autoimmune attack on the thyroid, and can both be used to monitor the effect of interventions. Some interventions will lower TPO antibodies more, while others will have a greater effect on TG antibodies. This can depend on the individual and their body’s response.
Some people with Hashimoto’s test negative for thyroid antibodies because their overall immune health is so weak, they do not produce enough antibodies. I tested negative for antibodies several times. Now, I insist on a thyroid ultrasound. A thyroid ultrasound can be used to detect changes in the thyroid, associated with Hashimoto’s. Given that Hashimoto’s is one of the leading causes of hypothyroidism worldwide, it’s best to be certain, one way or another. I have written several articles about how to best decrease thyroid antibodies.
Here are some articles I think you might find helpful:
HASHIMOTO’S AND THYROID ANTIBODIES: PART 1
https://thyroidpharmacist.com/articles/hashimotos-and-thyroid-antibodies/
HASHIMOTO’S AND THYROID ANTIBODIES: PART 2
https://thyroidpharmacist.com/articles/part-2-mechanisms-reduce-thyroid-antibodies/
Hi Isabella,
You are amazing! Thank.ypu so much for this information.
I have 2 questions for you.
When you say remission of Hashimotos with the antibodies below 100, are you still on thyroid medicine? I’m just looking for some clarification on the meaning of remission.
2. Did your husband treat for H Pylori too since he could have it too and reinfect you after treatment? I ask this because I have a feeling that my husband and kids may have H Pylori as well and I don’t want them to reinfect me after treatment.
Thank you so much,
Jen
Jen – thank you for reaching out! I’m so glad you are finding my research helpful. I recommend that you discuss your concerns about your children and husband having H Pylori with your practitioner so that you can all be treated at once if needed. When it comes to remission, thyroid tissue can regenerate, but the rate at which it does is not always predictable. Thus, some are able to stop the autoimmune attack on their thyroid and regain normal thyroid function. Others can reduce the dose of medications, and others will need to stay on the medications indefinitely. Reversing Hashimoto’s means different things to different people. For some, it means a reduction in symptoms, and for others, it means a reduction in your antibodies. I had both. Here a few articles that might be helpful for you:
IS IT POSSIBLE TO RECOVER THYROID FUNCTION IN HASHIMOTO’S
https://thyroidpharmacist.com/articles/is-it-possible-to-recover-thyroid-function-in-hashimotos
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
I was just diagnosed with Hashimoto’s 9 months ago. Just recently I had to have a colonoscopy and endoscopy due to a family history of cancer in these areas. Through a biopsy I was informed that I had h pylori. I started to do some research and found articles, such as yours, suggesting these two conditions could be related. My doctors have not acknowledged the link between the two. And I have a follow up with my endocrinologist in two weeks, so I’m hopeful to gather more information. I just recently experienced “an attack” and I’m trying to work my way back to normal via new meds and altering my diet to gluten free. Thank you for your research. I just had a feeling that the two were somehow intertwined and I’m hopeful that by the time I finish the triple antibiotics that I will start to feel better. But I’m definitely curious if I will need to be tested for h pylori in the future. What do you think?
Erin – thank you for reaching out. <3 H. pylori is a stubborn infection so retesting after treatment may be necessary. You would want to discuss this with your practitioiner. I share my recommendations in the article above for natural treatments as well as some help with gut health.
Hello, I would like some piece of advice or guidance. I’ve been on AIP almost 4 months, but I also have h. pylori, and yesterday I went to see the gastro because I want to eliminate this bacteria, otherwise I will not have a healthy gut and my hashi won’t improve.
I already tried before, (when i wasn’t gluten free and others) to eliminate it with antibiotics and also with natural treatments, they all failed.
Now I trust that everything I have done will help with the treatment, however I am scared because he told me that he will put me on a second line treatment with two antibiotics and something else for 14 days. Do you think this treatment is worth it?
considering the previous treatments, including the natural one.
Laura – thank you for reaching out. ❤️ Some people’s antibodies greatly reduce and sometimes actually go away, once H. Pylori is properly treated. You can’t always get rid of this nasty bug on the first try. Another thing to think about is that sometimes H. Pylori can actually co-occur with blastocystis hominis, which is a protozoan infection I often see in people with Hashimoto’s. Gut healing is a journey; you may need various interventions like removing reactive foods and infections, taking enzymes and probiotics, and balancing nutrients. Remember, be kind to yourself and learn to listen to your body so that you can support and feed it properly! You are worth it! I’m so glad you have found a practitioner to help you and I hope you will keep me posted on your progress. Here are a couple articles you might find helpful:
A COMMON ROOT CAUSE OF HASHIMOTO’S, HIVES AND IBS
https://thyroidpharmacist.com/articles/the-common-root-cause-of-hashimotos-hives-and-ibs
IMPORTANCE OF GUT HEALTH
https://thyroidpharmacist.com/articles/importance-gut-health/
Hello Dr. Wentz, should we take care of infections first or leaky gut?
Helen – thank you for reaching out. ❤️ Gut problems are often caused by infections like H. pylori, parasites like Blasto, SIBO, an imbalance of bacteria, and enzyme deficiencies or food sensitivities (especially to gluten, dairy, and/or soy). Even stress can be a factor in gut permeability. We know that intestinal permeability (aka leaky gut) is present in every case of autoimmunity and often precedes the development of Hashimoto’s. Symptoms of leaky gut may include bloating, diarrhea, constipation, stomach aches, acid reflux and irritable bowel syndrome. According to the Institute of Functional Medicine, many people develop IBS 5-10 years before an autoimmune diagnosis. I was one of them and didn’t take my gut health as seriously as I should have. Here is an article you might find interesting.
6 DIFFERENT ROOT CAUSES
https://thyroidpharmacist.com/articles/6-different-hashimotos-root-causes/
Helen – thank you for reaching out. ❤️ Gut problems are often caused by infections like H. pylori, parasites like Blasto, SIBO, an imbalance of bacteria, and enzyme deficiencies or food sensitivities (especially to gluten, dairy, and/or soy). Even stress can be a factor in gut permeability. We know that intestinal permeability (aka leaky gut) is present in every case of autoimmunity and often precedes the development of Hashimoto’s. Symptoms of leaky gut may include bloating, diarrhea, constipation, stomach aches, acid reflux and irritable bowel syndrome. According to the Institute of Functional Medicine, many people develop IBS 5-10 years before an autoimmune diagnosis. I was one of them and didn’t take my gut health as seriously as I should have. Here is an article you might find interesting.
6 DIFFERENT ROOT CAUSES
https://thyroidpharmacist.com/articles/6-different-hashimotos-root-causes/
Oh how I wish I had come across this years sooner! I had heard a bit about h pylori and the connection to Hoshimoto. I love how thorough you are with studies, etc. I appreciate the effort you put in, as I know its a great amount. My question is this – I was just recently diagnosed with h pylori through a microbiome test. I was told my partner and children (due to their age- younger) should be treated as well, as they are also most likely infected as well. If they dont get treated I will most likely be be infected with h pylori again from my exposure to them. What are your thoughts on this? Also, if someone were to choose the route of antibiotics, what concoction would you recommend? Also, if one uses antibiotics, how would you recommend using pre and probiotics in conjunction (before/after/during)? Just wanting to pick your brain, as you seemingly are quite verse on the subject. So many doctors seem, well, are just completely uninformed and seemingly don’t care. As a woman, I appreciate your considerations and incredible efforts, as we must advocate for our health. Thank you.
Melynda – thank you for reaching out. ❤️ H Pylori is a bacterium that is transmitted orally, from person to person. Whether your family members should be tested/treated is something you would want to discuss with your practitioner. In the article above I do offer some general recommendations, however, please understand I am not able to recommend a specific antibiotic or treatment without a comprehensive health assessment. As for a probiotic, adding an S. boulardii supplement to your treatment can increase the rates of eradication, and reduce the rates of dysbiosis from the use of antibiotics. I hope this helps.
Thank you so much, Izabella! I have just started taking DGL, mastic gum, and s. boulardii 3 times a day along with oil of oregano once a day. I just started taking them in the last week. For some reason I have a significant headache last night and this morning and I’m wondering if it’s due to one of these. Do you have any thoughts on what would cause it?
Thank you!!
Liz – thank you for following!❤️ It could be a few things. I recommend stopping them until your symptoms subside and then discuss with your practitioner whether you should resume. If the symptoms persist please see your practitioner.
Hi Izabella! Through my functional
Doctor I did a stool test and it showed dysbiosis and h pylori. She has me taking Biocidin drops. Would you say this is equivalent of your protocol you mention above for the herbal way to treat? I have constipation with alternating diarrhea when it seems I eat dairy (recent finding). Thank you.
Christine – thank you for following! I’m so glad to hear you have found a practitioner to help you! ❤️ I recommend discussing the two protocols with them as they know your health history and are better able to help you determine what would work best for you. Please keep me posted on your progress.
Hello doctor. I’m a man with hypothyroid caused by stress and then got ulcer/burning in stomach.
I think the burning sign of h pylori, is it ok to drink cabbage juice with my hypothroid? Cause i heard that cabbage is harmful to thyroid.
Thanks in advance.
Fransos – thank you for following! Cabbage juice is rich in glutamine and can help support gut healing and suppress H. pylori, allowing the gut to heal and clear the infection. As for whether it is safe for hypothyroid, there is a myth that foods known as goitrogens, such as cruciferous vegetables ie cabbage, are not good for those with Hashimoto’s. Iodine deficiency is not widespread in people with Hashimoto’s, and so eating cruciferous vegetables (unless you are sensitive to them) is perfectly healthy for people with Hashimoto’s and should not impact thyroid function. In the case that a person does have hypothyroidism due to iodine deficiency, he/she can still enjoy crucifers as long as they are cooked or fermented. Cooking/fermenting will break down the iodine blocking content. You can read more about the breakdown of the science behind the thyroid and goitrogens here:
WHAT ARE GOITROGENS AND WHY DO THEY MATTER WITH HASHIMOTO’S?
https://thyroidpharmacist.com/articles/what-are-goitrogens-and-do-they-matter-with-hashimotos
Hello Izabella! Thank you for this article. It’s very helpful. I have been trying to heal Hashimoto’s since 2014 and it’s a constant battle seems like. I’m hoping I conquer this soon!
While I have not tested for H.pylori before, I recently developed a very debilitating acid reflux that keeps me up at night (that’s after I went through 2 rounds of antibiotics for the treatment of the UTI). Now to think of it, I think I had acid reflux before, it just wasn’t this prominent. I’m very interested in incorporating the natural protocol you listed. I’m hoping if not h.pylori, it could help acid reflux.
My question tho is about black seed oil – how much did you take for treatment and eradication of h.pylori?
Thank you for your help and all the information you provide!
Margarita – thank you for reaching out.❤️I’m so glad you found my article helpful. I have found as well as the studies that 2 grams per day is effective. Here is an article you might find interesting as well: https://thyroidpharmacist.com/articles/black-seed-oil-and-hashimotos/
Hi Dr. Izabella Wenz,
Thank you for your website.
I have Hashimoto’s. I’m diagnosed by H pylori. I have a low blood sugar (65 with A1c 4.9) and pressure ( 9/5.6). Most of the herbal medicines cause low blood sugar like Berberine, Black seed. Any command?
Thank you.
Azita – thank you for reaching out. ❤️Please understand, I am unable to advise which supplements might work best for you without a comprehensive health assessment. I recommend that you discuss these options with your personal doctor so they can help you determine what would work best for you and your health condition.
Dear Izabella,
I’ve been following you since your Thyroid Secret series in 2014 which I am so thankful to have found you and your work, thank you. I’ve been diagnosed with Hashimoto’s in 2009 at 17 y-o and my lifestyle has evolved so much since then (positively despite challenging). Recent diagnosis with H. Pylori through GI-MAP with very high zonulin. Currently being treated with Pyloguard, Black cumin seed oil (in soft gels), mastic gum, Mega IgG, Megasporebiotics, Biofilm defense and Butyrate. When you mentioned that you’ve found Black cumin seed oil to be less effective in gel capsules than its oil form, I got interested because I’m currently using the gel capsules.
May you please share more details as to why the oil would be more efficient if you would still suggest to opt for the oil instead of capsules? The protocol is already soooo expensive that I wouldn’t want to have to start over because the Softgels form was not strong enough. I was still prescribed 2g (1000mg twice daily).
Thank you <3
Karel – thank you so much for following. I have recently created my own Black Cumin Seed Extract softgels, making sure that their potency and purity would be optimized in order to be highly effective. That said, everyone is different and it’s ultimately up to you and your practitioner as to the right supplement to choose. I generally advise my clients to think about your symptoms, reactions to supplements, and your health timeline when your looking for a treatment option. ❤️
Dr. Wentz,
I have Grave’s disease and after reading Hashimoto’s Protocol, I took a GI map test. My test not only came back positive for H-pylori, but several other things like E-coli, Eschericia, enterobacter, firmicutes, chilomastix, blastocystis hominis, and several microbes. Is that common to have that many all at the same time? Would treating the H-pylori also irradicate all of the other issues? Thank so much for sharing all of your amazing knowledge via books and website. I’ve been in this battle for 5.5 years and finally feel like I’m making headway!
Krysten – thank you for reaching out. ❤️ It’s hard to say, everyone is different. I do recommend discussing all of this with your practitioner to help you come up with a plan to start healing your gut. Just keep in mind that gut healing is a journey; you may need various interventions like removing reactive foods and infections, taking enzymes and probiotics, and balancing nutrients. Remember, be kind to yourself and learn to listen to your body so that you can support and feed it properly! You are worth it! You may find this article helpful as well!
IMPORTANCE OF GUT HEALTH
https://thyroidpharmacist.com/articles/importance-gut-health/
Hello so much great information here, how do I start? How dio I find someone where I live to help with this journey? Endocrinologist not willing to do anything other than rx and standard protocol
Was Graves, RI and normal for years then started to get hyper again (allergic to PTU – white BC too low) thyroidectomy (regret) then hypo and Hashi…struggles with High BP, want to try natural thyroid and anything that will help
Any advice would be greatly apprecaited
Daphne – thank you for following! I believe that everyone needs to find a practitioner that will let them be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It’s a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! I also have articles on my page with information on where to start that you might find helpful. Here are some links to some resources that I hope help.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
COMPOUNDING PHARMACIES
https://thyroidpharmacist.com/database-recommended-compounding-pharmacies/
Hi Izabella! Firstly, thank you for all that you do. Your books have been a life saver for me, and I’m currently in line at my local library for your newest book on adrenal health.
My question is, I recently started the mastic gum approach and I’m surprised that I have no die-off symptoms whatsoever! Is this common? I noticed the bottle expires in about 1 month and I’m concerned that maybe the mastic gum isn’t potent enough anymore?
Thank you.
Lisa – thank you for reaching out. I’m so glad to hear you have found my books helpful. H. pylori is a stubborn infection. and the time it takes to kill H. Pylori is different for everyone. I recommend testing again after you complete the protocol and if the H. Pylori has not been eradicated, then to repeat the protocol again under the guidance of your practitioner.
I found this study regarding the efficacy of Artemisinin on H. pylori.
https://pubmed.ncbi.nlm.nih.gov/22687518/
Charlie, thank you so much for sharing this with me!
This is wonderful information! I wish I had researched Hashimoto’s root causes sooner but I trusted the traditional medical model for my son with Downs. He’s now 12 and hyper and super skinny. I am getting pushback now from both the endocrinologist and his pediatrician to keep his thyroid dosage high enough to keep his TSH in the “normal” range. But he has zero evidence of hypothyroidism, in fact the opposite. Have you come across any functional medicine research for pediatric and/or Down Syndrome TSH recommended range? Thanks.
Jenny – thank you for reaching out. I do recommend finding a Functional practitioner like Dr. Sheila Kilbane, a wonderful integrative pediatrician, who has worked with children and teens who have Hashimoto’s, to help them thrive. I have a couple articles I am going to share with you below and there are resources in those that I hope are helpful as well.
THYROID AND DOWN SYNDROME CONNECTION
https://thyroidpharmacist.com/articles/thyroid-down-syndrome-connection/
PHARMACISTS IN FUNCTIONAL MEDICINE
https://thyroidpharmacist.com/articles/pharmacists-functional-medicine/
Hi,
I’m on your 60 day protocol and was wondering when can I retest for helicopter . Do I have to wait a certain time after the protocol or can I retest before the end of the protocol?
Thanks, any help appreciated 😊
Gillian – thank you for reaching out. You can consider retesting once you have completed the protocol for the H.pylori, to ensure you’ve eradicated the infection. If you haven’t then you would want to continue the protocol for 30-60 days and then retest again. If you have any other questions about the protocols, please email my team at info@thyroidpharmacist.com and they will be happy to help.
Hi Dr. Izabella Wentz,
I just finished my second round of Mastica with cabbage juice & olive oil and I’m hoping this time I finally got the bacteria numbers down!
How long should someone wait after treatment before doing another stool test?
Thanks!
Lisa – thank you for following. Once they finish the course of the protocol, you can retest. Please feel free to email my team at info@thyroidpharmacist.com if you have any questions about the protocols.
Once we eradicate h. pylori, what are your recommendations for healthy-maintenance and preventing an infection again?
Ruth – thank you for following. Keeping in mind that H. pylori is transmitted orally, from person to person, as well as potentially between people and their pets, it’s really important to be mindful of that. So, not using the same tooth-brush or glass, washing hands, resisting your dog’s kisses, washing dishes, silverware, etc. and with hot water can help.
Hi, thank you for the updated article. Overall, I continue to feel better using your programs, and the information you provide has been invaluable. I have been working to eradicate H Pylori going on 2 years and so far no luck. I change my toothbrush frequently, stopped kissing my husband 🫤 from the start and am not seeing success. My practitioner has me on Pylo Guard by Microbiome Labs. Have you had any experience with this supplement? Thank you!
Ellie, You’re welcome! Pylo Guard is a good option and can be used on it’s own or in conjuction with antibiotics. I hope you will keep me posted on your progress.
My ND prescribed Interfase Plus (Biofilm Disruptor) followed by Candibactin AR & BR 2x day for 3 months to treat H.Pylori along with Giardia and Candida. Do you think this protocol will work to eradicate H.Pylori? I read that Candibactin AR/BR may not be the best treatment route for H.Pylori. Please advise!
Valerie, thank you for sharing. I’d recommend discussing your concerns about Candibactin AR/BR with your practitioner, as they’ll be most familiar with your specific health situation. For H. pylori, there are several options, including mastic gum, DGL, Matula tea, or antibiotic-based triple/quadruple therapy. It can be a stubborn infection to clear. Candibactin BR is one herbal approach I often recommend for SIBO. Keep in mind that many people with thyroid issues have multiple gut-related concerns. Here are a couple of articles that might be helpful for you:
https://thyroidpharmacist.com/articles/sibo-prevent-remission-hashimotos/
https://thyroidpharmacist.com/articles/fundamental-gut-health-protocol/
Please help! My daughter, 15, had been diagnosed with hashimotos. We are finally getting results back from stool sample and mold, bloodwork;etc. She tested positive for mold and H pylori. While addressing these we are trying to get some relief besides a steroid cream for an itchy, red rash on her neck primarily under her thyroid. Anything you can recommend?? We have tried everything and are desperate!! We think it may be caused by one of the above or high antibodies which we are working to fix.
Maggie, thank you for sharing your daughters struggle. I’m so sorry. I highly recommend working with a functional medicine clinician who has experience working with children/teens. It’s an entire medical specialty dedicated to finding and treating underlying root causes and preventing serious chronic disease rather than treating individual disease symptoms. Check out this article:
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Recommended Compounding Pharmacist list
https://thyroidpharmacist.com/database-recommended-compounding-pharmacies/
Hi Izabella – thanks for your great article regarding H Pylori and Hashimoto’s. My wife does have H Pylori currently and was have a 1.5 year old also. Would you ever treat the son or have him go through a protocol?
Tanner, H. pylori can be transmitted within households, so it’s wise to consider testing family members, especially if they’re showing symptoms like reflux, stomach pain, or feeding issues. I do suggest that you work with a functional medicine doctor that is familiar with working with children.
Here are some resources that I hope are helpful as well.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Thank you, Dr. Wentz. I’ve seen two studies where ground black seeds to eradicate H pylori. What dose and duration of treatment have you seen to be effective?
Valentina, In my research and clinical experience, Nigella sativa (black seed oil) shows promise as part of a natural approach to addressing Helicobacter pylori. Its active compound, thymoquinone, may help disrupt biofilms and support the body’s ability to reduce bacterial overgrowth, while also offering gastroprotective and anti-inflammatory benefits. Most studies have used a dose of around 2 grams per day, typically for a short-term protocol (a few weeks) when used in the context of H. pylori. That said, I generally do not recommend relying on black seed oil as a standalone treatment. Instead, I use it as part of a comprehensive, personalized protocol that may include additional targeted antimicrobials, gut lining support, and follow-up testing to confirm eradication. For more info on Black Seed oil, you can review my article here:
https://thyroidpharmacist.com/articles/black-seed-oil-and-hashimotos/