How do you feel when you wake up in the morning? How do you feel between 2 and 3 pm each day? Do you feel “awake” during the day, or do you feel brain fogged, tired, or like you’re dragging your feet? Do you rely on caffeine to “wake up” in the morning?
If you answered “tired” or “yes” to any of these questions, then you are most likely experiencing fatigue.
Fatigue was the most debilitating symptom I experienced with Hashimoto’s. It started eight years before I was finally diagnosed in 2009, after I had contracted mono (the Epstein-Barr virus) in college. I needed to sleep for 12 hours each night to be able to function… and by “function,” I mean after hitting the snooze button on my alarm clock for two hours (ask my poor husband), I would drag myself out of bed and then had to drink 4 to 6 cups of caffeine every day to keep myself awake. I often had Red Bull and Pepsi for breakfast, and was the epitome of “wired but tired.”
I saw numerous doctors, and I was offered antidepressants and stimulant medications used for narcolepsy and ADHD, but no one thought to check my poor little thyroid. I then came across “chronic fatigue syndrome,” which seemed to fit my symptoms, and was discouraged that there was “no cure” (at least not according to conventional medicine). I slept half of my early twenties away thinking that I had better just deal with it, since no one could help me anyway.
When I was finally diagnosed with Hashimoto’s, part of me was relieved. I thought that I would finally get more energy. But this was not the case. Sure, the thyroid medication helped; instead of sleeping for 12 hours, I only needed 11 hours of sleep. But I didn’t stop there. At the time of my diagnosis, I was working as a consultant pharmacist and had become accustomed to researching emerging healthcare information. Finding a way to get myself better became my mission.
It took me almost three years after my Hashimoto’s diagnosis to get my energy back, and I hope that some of the strategies that I used will help you get yours back too.
If you are dealing with Hashimoto’s fatigue, I’d like to share a few tips with you:
- The optimal TSH number for fatigue resolution
- The one nutrient that can restore energy in three days (if deficient)
- The thyroid hormone that can block energy production
- The three types of fatigue–inducing anemia your doctor may miss
- Supplements that can reduce thyroid fatigue
Strategies to Address Fatigue
Fatigue and low energy are common symptoms of hypothyroidism. In general, this can be caused by hormonal imbalance (low levels of thyroid hormone) and a slowed metabolism, but it may be linked to a number of other factors. I suggest considering the list below to get to the root cause(s) of your fatigue.
1. The Importance of an Optimal TSH
Conventional endocrinologists often refer to the TSH test as the “gold standard” test for diagnosing and treating thyroid conditions. So, it’s important to make sure that your TSH is within the range of a healthy person without thyroid disease (not within the range of an elderly person or someone with subclinical thyroid disease).
TSH stands for Thyroid Stimulating Hormone, which is produced in the pituitary gland in your brain. [1] The pituitary gland tells your thyroid to make and release thyroid hormones into your blood. A TSH test measures how much of this hormone is in your blood. In advanced cases of Hashimoto’s and primary hypothyroidism, this lab test will be elevated. (Read my post about interpreting your TSH test for more information.) In the case of Graves’ disease and hyperthyroidism, the TSH will be low. Keep in mind, however, that people with Hashimoto’s and central hypothyroidism may have a normal reading on this test.
The National Academy of Clinical Biochemists indicates that 95 percent of individuals without thyroid disease have TSH concentrations below 2.5 μIU/mL. However, as of 2017, the official TSH reference range in most U.S. labs, runs from approximately 0.5 to 4.5 or 5.0 μIU/mL. A patient with TSH levels within this range is considered to have normal thyroid function.
However, some labs have not adjusted that range in the reports they provide to physicians, and have kept ranges as lax as 0.2-8.0 μIU/mL. And, many physicians only look for values outside of the “normal” reference range provided by the labs. They may not be familiar with the new guidelines. This is one reason why patients should always ask their physicians for a copy of their lab results. Despite some lab tests stating that a TSH of 8 or 5 μIU/mL is “normal,” most people feel best with a TSH between 0.5 and 2 μIU/mL. [2]
You may also be interested to know that of the 2,000+ people who took part in a survey I conducted, thyroid patients reported that optimizing their TSH helped improve their energy. Seventy-seven percent of my readers with a TSH level under 1 μIU/mL saw improvement in energy from medication interventions, and 72 percent with a TSH between 1 and 2 μIU/mL saw improvement in their energy levels.
From a personal perspective, I felt like a sloth when my TSH was within the “normal” range at 4 μIU/mL.
In 2001, the results of the Basel Thyroid Study conducted at the end of the 1990s were published, and this study revealed that tiredness and fatigue often remained in people with hypothyroidism, despite thyroid hormone therapy. [3] An editorial in Thyroid, written by Peter Andreas Kopp in 2014, found that patients remain symptomatic (that is, they may experience symptoms like fatigue) despite having “normal” thyroid hormone levels. [4]
Similar to the opinion of Kopp, Mary H. Samuels, a professor at the Oregon Clinical and Translational Research Institute, stated: “It is a common clinical observation that some otherwise healthy patients with hypothyroidism continue to complain of fatigue, poor mood, inability to concentrate, and vague cognitive difficulties (often described as ‘brain fog’) despite normal TSH levels.” [5]
2. The Impact of Low T3/High Reverse T3
Beyond TSH, I also recommend additional thyroid hormone testing to feel our best.
Triiodothyronine, or T3, is a hormone produced by the thyroid gland that is essential for keeping our metabolism going. T3 is the main “energy” hormone produced by the thyroid. When our cells see T3, they produce more energy, so it’s very important to ensure that we have adequate levels of active T3, as T3 tells our body to grow hair, boost metabolism, and create more energy.
It’s also important to avoid having a high level of reverse T3, which is a molecule related to T3 that blocks thyroid receptors in cells instead of activating them. When cells see this molecule, they slow down energy production. [6]
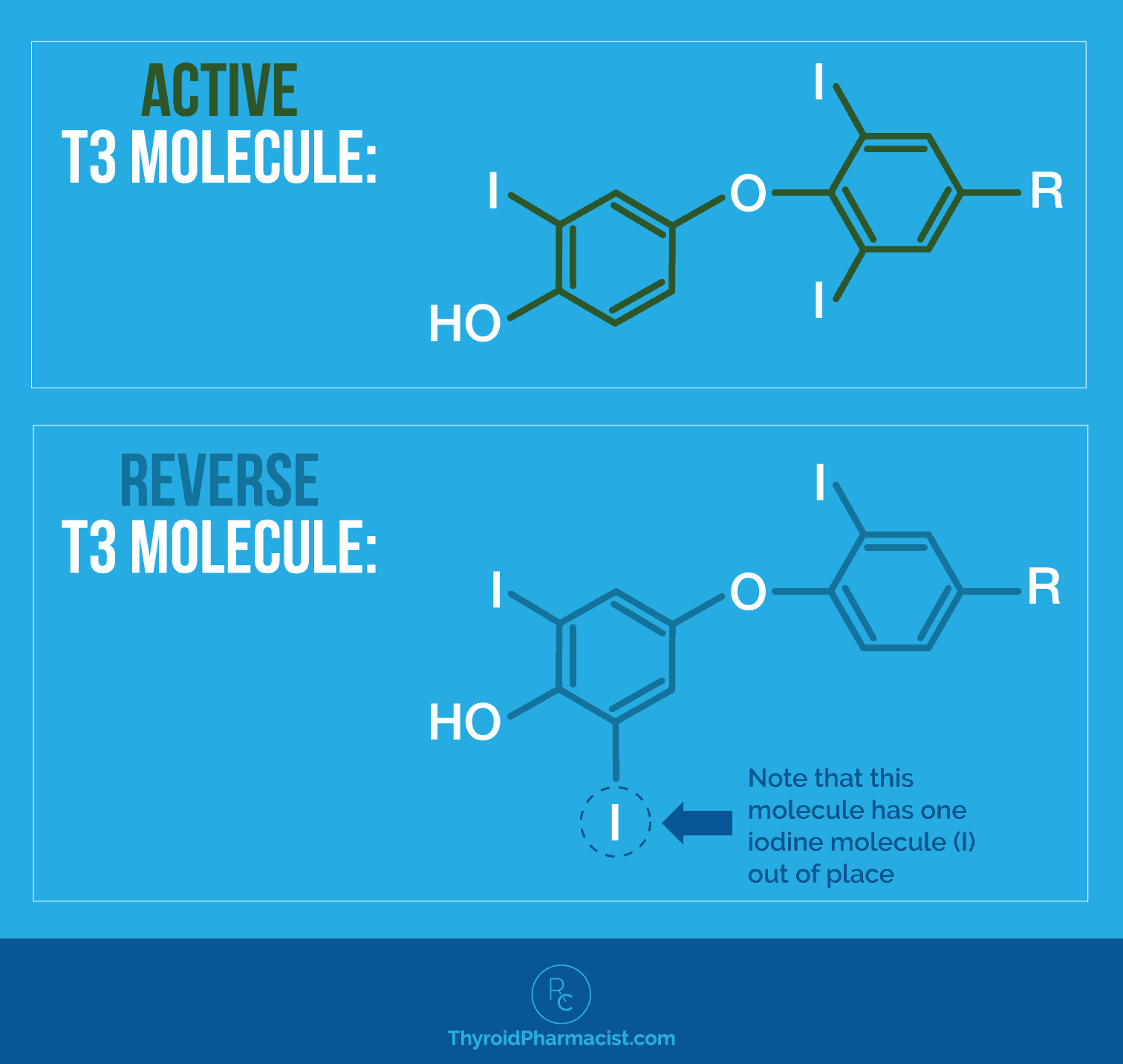
Synthroid® or levothyroxine (a synthetic version of T4) is the most commonly prescribed thyroid medication, but only contains T4, a precursor to T3, our main “energy” hormone. T4 is converted to T3 in the body, but this doesn’t always happen, due to numerous factors such as stress, nutrient deficiencies, and others… so we often continue to feel exhausted despite having normal T4 levels. [7]

Ulta Labs is a great online resource for ordering a free T3, free T4, and TSH test, as well as for checking your reverse T3 levels, without needing to get a thyroid lab request from your doctor.
You may also be able to submit them to your insurance for reimbursement (be sure to check with your individual insurance to make sure they allow this), and I love using it to get a discount on lab tests with my high-deductible insurance plan.
If you continue to be fatigued while on medications, you can have your practitioner test your free T3 levels. (In some cases, testing reverse T3 may also be helpful, although it’s not always necessary.)
In the case that your T3 is low, or in the bottom part of the reference range, or if you’re still symptomatic with T4 medications alone, you may benefit from adding a T3-containing medication such as Cytomel (liothyronine) to your current medication regimen, or switching to a T4/T3 combination medication such as Armour Thyroid* or compounded T4/T3. (Other combination options include WP Thyroid and Nature-Throid, however, these medications are currently unavailable following a voluntary recall in 2020.)
In my survey of over 2,000 readers, 76 percent reported improved energy while taking compounded T3/T4, 74 percent while taking Armour Thyroid*, 74 percent with Cytomel, and 72 percent with Nature-Throid. Only 52 percent saw improved energy levels with Synthroid, the most commonly prescribed thyroid medication.
The takeaway from the survey showed that getting on the right thyroid medication helps many people get their energy back. For further information, you can read my article about thyroid medications.
Also, be sure to download my FREE eBook on optimizing your thyroid medications!
*Note: While Armour Thyroid does not have any gluten-containing ingredients, it is not tested for gluten content, and cannot be certified as gluten-free. Armour Thyroid does contain sodium starch glycolate, which can be derived from wheat or corn.
3. Is Anemia Stealing Your Energy?
Many people think of iron deficiency as the cause of anemia. But in my experience, there are actually three types of nutrient deficiencies that can lead to anemia and are common in people with Hashimoto’s – iron, B12, and folate.
Testing for Anemia
To look for anemia, your practitioner will usually run a blood test to check for hemoglobin and hematocrit. While helpful for advanced cases of anemia, this test may miss some subtle cases of anemia that can leave us feeling exhausted.
In addition to testing hemoglobin and hematocrit, I recommend testing ferritin, B12, and folate. Always be sure to get a copy of your lab tests. Just as the “normal” (conventional) ranges for TSH may not be optimal, the “normal” lab values for B12 and ferritin may not be in what functional practitioners (including myself) would consider an ideal range either.
B12
B12 is an essential vitamin that is required for protein synthesis, cell reproduction, and normal growth. [8] It also helps with the production of melatonin and serotonin, which promote restful sleep and positive moods. [9] However, it can become depleted, especially in times of high stress. [10]
Normal levels of vitamin B12 are between 200-900 pg/mL; however, levels under 350 pg/mL are known to be associated with neurological symptoms. [11] In my experience, you can have symptoms if your levels are below 700 pg/mL, and you may still benefit from a supplement.
In a study regarding the prevalence of vitamin B12 deficiency among patients with thyroid dysfunction, it was found that autoimmune thyroid disease is also associated with the autoimmune disorder pernicious anemia, which may lead to malabsorption of vitamin B12. [12]
The study concluded that in order to ensure proper treatment, vitamin B12 screening is recommended upon initial diagnosis of autoimmune thyroid disease, and periodically thereafter.
As some people may have a difficult time absorbing B12 orally due to conditions like pernicious anemia, SIBO, or H. pylori infections, practitioners may choose to megadose vitamin B12 orally or give B12 injections to ensure proper absorption. A less known route of administration that I have found to be as effective is B12 sublingual (under the tongue) drops or lozenges. (Some people can have a difficult time with absorption from pills due to various reasons, including pernicious anemia.) [13]
In addition, a methylcobalamin or hydroxocobalamin version of B12 (rather than a cyanocobalamin version) is absorbed better by most. [14]
I have found the liquid B12 5000 supplement by Pure Encapsulations to be very helpful for my clients. In my survey of 2232 of my readers with Hashimoto’s, 88 percent saw improvement in energy from B12 supplementation. You can read more about the thyroid and B12, as well as the optimal sublingual dosing regimen that may help you avoid B12 shots.
Ferritin
Ferritin is the name given to your body’s iron reserve protein. “Normal” ferritin levels for women are between 12 and 150 ng/mL. [15] However, in my practice, I’ve observed that the optimal ferritin level for thyroid function is between 90 and 110 ng/mL.
Ferritin is one of the most common deficiencies I see in people with Hashimoto’s, and in addition to fatigue, ferritin deficiency can also contribute to shortness of breath, restless leg syndrome, hair loss, insomnia, strange food cravings, elevated levels of reverse T3, and mood swings. [16]
While ferritin is likely to be deficient in up to 50 percent of women of childbearing age, as well as up to 80 percent of women who are pregnant or who are recently postpartum, I don’t recommend supplementing unless you’ve been tested to be deficient in ferritin. [17] Too much iron/ferritin can also be a problem!
According to my survey, ferritin/iron supplementation improved energy levels for 82 percent of those who responded. While most iron supplements can cause digestive disturbances, two potential options may be better tolerated:
- OptiFerin-C contains ferritin and has helped many of my clients boost their ferritin levels. Calcium ascorbate, a natural, water-soluble version of vitamin C, is added to increase intestinal absorption.
- Thorne Iron Bisglycinate is an iron supplement that is more gentle on the stomach and less likely to cause constipation.
I recommend testing for ferritin before supplementing, and retesting your levels within 1 to 3 months, to ensure that you are supplementing enough (but not too much!).
Folate
Vitamin B9 is a necessary nutrient that naturally presents itself as folate, which plays a vital role in the formation of DNA and cell growth. [18] In some cases, you may test normal or high for folate, but you could still be deficient in the right kind of folate for your body.
This is the case with the MTHFR gene variation, which can impact how well your body metabolizes folate. [19] Both folate and folic acid are forms of vitamin B9, required for numerous critical bodily functions. However, folic acid is synthetic, while folate occurs naturally in foods, such as broccoli, lamb, beets, and quinoa.
Some people, including some individuals with Hashimoto’s, have the MTHFR gene variation that prevents them from properly processing the folic acid that may be present in less expensive supplements and processed foods. Some professionals claim this type of folic acid may even cause a build-up in the body, leading to toxicity. [20]
Likewise, the MTHFR gene produces an enzyme necessary to process vitamin B9 properly. This enzyme is also important for converting homocysteine to methionine, which the body needs for proper muscle growth and energy. [21]
Those who may have adrenal fatigue, those who are often stressed, and those with the MTHFR gene variation and high homocysteine levels, may benefit from an activated or methylated version of folate, mainly because food alone does not provide sufficient levels. I have formulated MTHFR Pathways, which contains all of the above-mentioned ingredients and may be helpful in maintaining healthy homocysteine levels.*
Read more about MTHFR and Hashimoto’s here.
4. Discover Your Food Sensitivities
Fatigue can be experienced from ingesting a food you are sensitive to. Food sensitivities are very different from food allergies, and many people are sensitive to specific food groups which can result in fatigue. I’ve found that people with Hashimoto’s often present with gluten, dairy, soy, egg, corn, and nut sensitivities. In fact, I find two of the most common food sensitivities in people with Hashimoto’s are gluten and dairy.
Gluten is the main reactive protein found in wheat, and casein is the main reactive protein found in dairy. Growing evidence has shown that food sensitivities can negatively impact our bodies and trigger a wide range of symptoms, such as asthma, arthritis, mood disorders, and autoimmune disorders. [22]
My own clinical and personal experience has shown that non-celiac gluten sensitivity is one of the biggest triggers in Hashimoto’s.

Changing my diet helped with fatigue, and I regained my energy. It also helped me eliminate bloating, symptoms of irritable bowel syndrome, anxiety, congestion, and carpal tunnel!
In my survey of people with Hashimoto’s, 75 percent reported improvement in energy from the Autoimmune Paleo diet, and another 78 percent saw improvement in energy from the Paleo diet.
Of course, it is important to find a diet that works for you and is free of foods that you are sensitive to. (Check out my article on tailoring your diet to your specific needs here.)
Food sensitivity testing may be helpful in some cases. Not all tests are created equally, but I have found the food sensitivity testing through Alletess to be the most accurate. The company offers food sensitivity testing (96 and 184 food panels) for people to self-order. I started with the 96 food panel, which was enough to pinpoint most of my food triggers, and I now repeat the 184 food panel on an annual basis to be sure that I’m staying on top of potential triggers, as our food sensitivities and reactions to foods tend to change with time.
5. Balance Your Blood Sugar
Blood sugar imbalances can wreak havoc on our energy levels as well as cause anxiety. People with blood sugar imbalances will often have times of the day where they feel especially tired, weak, and/or anxious, such as “morning fatigue” or the “afternoon slump.” Those who have adrenal fatigue may also suffer from blood sugar imbalances. [23]
That’s why balancing blood sugar levels should be one of the top priorities for anyone who is hoping to overcome fatigue. Balancing my blood sugar made a big difference for me, helping me feel more energetically balanced and less anxious throughout the day. Plus, many of my clients and readers with Hashimoto’s have reported that their thyroid antibody levels dropped when they balanced their blood sugar!
Before I balanced my blood sugar, I would get “hangry” (hungry + angry) multiple times per day.
I found that the high-carbohydrate foods I was eating were causing huge blood sugar swings, and I didn’t realize these swings were causing a spike in my thyroid antibodies and weakening my adrenals.
Practitioners, like myself, who focus on reversing Hashimoto’s, often describe blood sugar imbalances as adding fuel to the fire in autoimmune thyroid disease. I wasn’t aware that I had blood sugar issues when I was first diagnosed (despite being a self-admitted sugar addict).
Researchers in Poland found that up to 50 percent of patients with Hashimoto’s have an impaired tolerance to refined or simple carbohydrates, like processed sugar or refined grains that have had the nutrients removed. [24] This means that after consuming carbohydrate-rich foods, their blood sugar goes up too high, too quickly, which leads to a rapid, and often extreme release of insulin. These insulin surges can cause low blood sugar (reactive hypoglycemia), which in turn can cause troublesome symptoms like lightheadedness, nervousness, anxiety, and fatigue.
However, eating a low glycemic index diet can help you feel fuller longer. It can also help to improve cholesterol and blood sugar levels, enhance cognitive performance, improve energy, alleviate symptoms of adrenal fatigue, promote weight loss, and reduce acne. The diet can lower your risk of developing diabetes, heart disease, and some cancers as well. [25]

6. Enhance and Optimize Digestion
The digestive process is an energy-intensive one. Studies have shown that people with Hashimoto’s and hypothyroidism often do not have adequate levels of stomach acid, and some don’t produce ANY stomach acid, making protein digestion inefficient and even more draining of our energy. [26]
Discovering that I had a deficiency of stomach acid was a huge “aha” moment for me! I couldn’t believe how energetic I became when I started taking Betaine with Pepsin with my protein-containing meals.
My 10-year-long debilitating fatigue was lifted practically overnight, and I went from sleeping for 11 to 12 hours per night, to 8 hours — just because I started digesting my food better. I felt like Bradley Cooper in the movie Limitless after I started taking Betaine with Pepsin. Finally having enough energy gave me the confidence that I could overcome Hashimoto’s and my long list of health struggles. It even helped with my brain fog, and I was able to come up with all kinds of clever words much more quickly. My humor came back.
I started writing my first book about overcoming Hashimoto’s the morning after I took a dose of Betaine with Pepsin. The restored energy gave me hope that I would be able to devote myself to research and find the root cause of my condition, then share that knowledge to help others.
Betaine with Pepsin promotes healthy digestion and supports the absorption of various nutrients, such as protein, calcium, vitamin B12, and iron. [27] I have found it to be very beneficial for anyone seeking enhanced digestive function.
Out of 627 of my readers who took Betaine HCI and Pepsin, 59 percent said it made them feel better and saw improved energy levels, 33 percent said it made them feel worse, while 7 percent saw no difference in their symptoms. These results lead me to estimate that 50-70 percent of people with Hashimoto’s are likely to have a deficiency in stomach acid, and the 33 percent of those who felt worse were likely not deficient in stomach acid. Those who did not see any improvement may not have been dosed adequately, as the dosage of Betaine with Pepsin should be individualized.
If you have a thyroid condition and continue to struggle with fatigue, check out my article on low stomach acid.
7. Sunshine Deficiency
A lack of sunshine can lead to fatigue, due to two very specific reasons: vitamin D deficiency and light deficiency.
Vitamin D deficiency is rampant and very common. It is estimated that some 30-50 percent of children and adults in North America, Europe, Australia, New Zealand, and Asia are deficient. Even in regions that receive plenty of sunlight, deficiency may be common if there is a lack of sun exposure to the skin. [28]
(So in my view, pretty much anyone who is not a full-time lifeguard in Southern California is at risk of being deficient in vitamin D! ;-))
A low-fat diet, vegetarian/vegan diets, and medical conditions related to fat malabsorption can increase the risk of vitamin D deficiency. Low levels of vitamin D are also associated with fatigue, hypothyroidism, and autoimmunity. [29] We can get vitamin D from sunshine, certain foods, and supplements, but it’s not always easy to ensure you are getting enough.
Vitamin D deficiency is more commonly found in people with Hashimoto’s — 68 percent of my readers with Hashimoto’s reported also being diagnosed with vitamin D deficiency, and 67 percent saw improvement in energy from increasing their vitamin D levels. Research done in Turkey found that 92 percent of Hashimoto’s patients were deficient in vitamin D, and another 2013 study found that low vitamin D levels were associated with higher thyroid antibodies and worse disease prognosis. [30]
I’ve personally found that most of my clients who are in remission from Hashimoto’s keep their levels of vitamin D between 60 to 80 ng/mL (150 to 200 nmol/L). This is especially true for those who have a history of contracting the Epstein-Barr virus (EBV).
My top ways to restore optimal vitamin D levels are through sun exposure and oral vitamin D3 supplements. Tanning beds are also another way to increase vitamin D levels, and some of my clients in colder climates with autoimmune issues swear by them in helping symptoms during the winter. However, tanning beds are very controversial, so I am hesitant in recommending them, due to their connections with skin cancers. [31] Other good sources of vitamin D are foods like wild salmon and cod liver oil.
Another thing I recommend is a beach vacation. (Please print this and show it to your boss or spouse whenever necessary — I know I have to remind my husband every winter!) But if you can’t get to the beach just yet, the recommendations below should work even in the darkest and coldest of winters!
Vitamin D advocates recommend 15 minutes of unexposed skin without sunscreen around noon. Perhaps you can go for a walk during lunchtime? If you are fair-skinned and not used to the sun, you may need to start a bit slower. Be careful not to overexpose yourself to prevent getting a sunburn.
I also recommend blue light therapy boxes. Clinically proven to boost energy and mood naturally, as well as fight the winter blues, blue light therapy boxes allow you to get the light you need wherever you live or work. [32]
For best results, I suggest using the box daily for at least 30 minutes. It may take a week or so before you begin to feel your energy return. I generally recommend using the box first thing in the morning as you’re getting ready for work, as well as in the early afternoon, to give yourself another energy boost. I don’t recommend using the light too close to bedtime, unless you’re planning to stay up late!
I have personally used this type of light preventatively during cloudy weather, as well as whenever I feel like I need an energy boost and can’t get outside or to the beach.
8. Is Your Liver Congested?
The liver’s function is to remove toxins from our bodies. These toxins can come from various external sources, such as molds, or from internal sources like an imbalance of gut bacteria or pathogens. [33] Some of us may be exhausted because we cannot process the toxins that are present in our bodies. The toxins saturate our liver enzymes, making us feel fatigued.
Some of the most common toxins in the environment include:
- Pesticides
- Herbicides
- Heavy metals
- Food additives
- Formaldehyde
- Solvents/cleaning materials
It’s a good idea to reduce your exposure to toxins in your environment. A few ideas include the use of an air purifier, drinking filtered water, stopping the use of cosmetics and related products that contain petrochemicals, avoiding preservatives and additives, stopping the use of harsh cleaning agents and aerosols, and eliminating molds in your home.
I have also found N-Acetyl-Cysteine, a supplement that supports liver detox capabilities, to be worth considering. [34]
You can also read about how supporting the liver is key to recovering from thyroid disease. [35] You’ll find signs and causes of toxic overload, how liver impairment is related to Hashimoto’s, who is most at risk, and so much more.
9. Boost Thiamine and Boost Your Energy
I have found that people with Hashimoto’s are often deficient in the B vitamin, thiamine (vitamin B1).
Thiamine is essential for energy production and carbohydrate digestion. Our bodies need thiamine to make adenosine triphosphate (ATP), which our cells use for energy, and it plays a key role in supporting the nervous system. [36] B1 is thought to strengthen the immune system and help our bodies withstand stressful situations. But, in order to absorb enough thiamine into our bodies, we also need adequate supplies of B6, B12, and folate.
What’s really exciting is that I’ve found that taking 600 mg of thiamine per day can restore energy levels in as little as three days! That’s great news for someone who suffers from fatigue. I have written about the thyroid and thiamine connection in my blog posts, and I still get hugs from people I meet at conferences who have reported that thiamine has changed their lives.
I recommend Rootcology Benfotiamine and Benfomax from Pure Encapsulations for best results. They are both non-GMO, gluten-free, and vegan… and are some of the highest-quality thiamine supplements on the market.
10. L-Carnitine for Thyroid Fatigue
L-carnitine is an amino acid that is naturally produced in the body. It helps transport fatty acids into the mitochondria where they can be burned up and used as fuel. [37]
L-carnitine levels may be decreased in hypothyroidism, potentially due to reduced synthesis of L-carnitine while we are in a hypothyroid state. Taking a thyroid medication can boost the production of L-carnitine, but it can also work as a vacuum, taking the L-carnitine from the body and resulting in an overall deficiency. [38]
The results of a recent study regarding L-carnitine supplementation for the management of fatigue in patients with hypothyroidism found that L-carnitine may be useful in alleviating fatigue symptoms in hypothyroid patients, especially in those younger than 50 and those who have hypothyroidism due to a thyroidectomy. [39]
In the study, 60 patients who were experiencing fatigue were given L-carnitine for 12 weeks. A dose of 1,980 mg was given to 30 people who were taking thyroid hormones (either due to Hashimoto’s or post-thyroidectomy), while 30 people received a placebo.
After 12 weeks, the researchers noted that the group receiving L-carnitine did indeed show improvements in fatigue, with the most significant improvements seen in “brain fatigue.”
I have personally seen people “awaken” with the use of L-carnitine.
L-carnitine, combined with eating a low glycemic index diet, can also help to establish proper blood sugar balance in the body. As we discussed above, blood sugar balance is crucial to help overcome fatigue. Studies in both humans and animals have shown that carnitine supplementation resulted in an improvement of glucose tolerance, in particular during insulin-resistant states. [40]
Red meat is the richest source of L-carnitine, but some individuals may not eat enough red meat to meet their carnitine requirement, or may not properly extract the nutrient. [41] For this reason, I created Rootcology’s Carnitine Blend, which combines 400 mg L-carnitine and 100 mg acetyl-L-carnitine in one convenient capsule.
Both L-carnitine and acetyl-L-carnitine can help to increase carnitine levels in the body; however, each form may have its own specific benefits. L-carnitine (2 grams per day) has been reported to resolve Hashimoto’s-related fatigue and has also been found to support antioxidant activities in the body, while acetyl-L-carnitine has unique brain-supportive properties and has been shown to help to reduce mental fatigue (and improve cognitive function) in various studies (bye bye brain fog!). [42]
Mitochondrial function is often impaired in Hashimoto’s, and over the last few years, studies have come out on using targeted mitochondrial supportive nutrients, including carnitine, to restore energy and brain function in people with hypothyroidism.
Taking care of our mitochondria is one of the best things we can do for fatigue, and it’s one of the main strategies I outline in my book, Adrenal Transformation Protocol. We focus on reducing inflammation and oxidative stress, and using supplements like L-carnitine to help restore optimal mitochondrial function. This strategy supports energy levels on a cellular level, to help you create true, sustained energy now and in the future.
11. Is Adrenal Fatigue Getting You Down?
Adrenal fatigue can make you feel like you are dragging around 50 pounds of concrete, especially in the later phases of adrenal fatigue when your cortisol becomes depleted. I have found that adrenal fatigue is one of the major reasons we feel exhausted despite taking thyroid medications.
With optimal adrenal function, in the morning, cortisol spikes, giving you a natural jolt to get you out of bed. Those with advanced levels of adrenal fatigue won’t make enough cortisol in the morning and may find themselves having difficulty getting up in the morning and sustaining good energy throughout the day. Common patterns I often see are “the afternoon person” — someone who struggles in the morning and evening, and has just a few good hours in the afternoon; or the “tired night owl,” a person who feels tired most of the day then gets a second wind at bedtime when the day’s cortisol is released.
Without sufficient cortisol levels, we may be more at risk of becoming overly dependent on caffeine.
Caffeine boosts cortisol levels temporarily, which may contribute to weakened adrenals in the long term. Drinking too much caffeine can create a vicious cycle of unrestful sleep, fatigue, and needing more caffeine.[44]
Since caffeine can alter cortisol responses, getting out of the cycle of dependency on caffeine by weaning off it (notice I didn’t say to stop cold turkey), as well as getting adequate sleep, can help with rebalancing the adrenals.
Hot lemon water first thing in the morning is a great substitute for caffeine and helps to provide relief from fatigue. Another great option is Dandy Blend, which is an instant herbal beverage made with dandelion. It’s a gluten- and caffeine-free alternative to coffee, that does not lead to withdrawal symptoms. I also like Four Sigmatic’s low caffeine and mushroom coffee options which provide you a little boost, but without the jitters, crashing, or stomach issues that regular coffee products can cause.
I have found that the ABCs of adrenals can be incredibly helpful for supporting the adrenals and energy levels:
A – Adrenal adaptogens
B – B vitamins
C – Vitamin C
I created Adrenal Support from Rootcology, which contains a blend of the ABCs. You should see improvements in your energy levels and resilience within a few days of starting Adrenal Support.
In some cases, additional adrenal testing and protocols may be indicated, but I know it’s often challenging to find a practitioner who will test for adrenal dysfunction, yet alone a practitioner who can give you a proper protocol for recovering your stress response. This is exactly why I created my Fatigue and Brain Fog Fix in Six (Thyroid and Adrenal Edition) program, and why I wrote my book, Adrenal Transformation Protocol, which takes readers through my tried and true process to transform their adrenals in just four weeks.
The protocol doesn’t require adrenal testing. Instead, we focus on the most frustrating symptoms of adrenal dysfunction, including brain fog, fatigue, anxiety, and trouble sleeping. We address these symptoms on a cellular level by providing mitochondrial support, bringing down inflammation, eating a nutrient-dense diet, and supporting our circadian rhythm.
In fact, 89 percent of people who completed the program reported a reduction in fatigue! Additionally, 92 percent experienced less mental fog, 86 percent reported reduced anxiety, and 81 percent said they slept better.
Here’s what one of my participants, Amy, had to say:
“I have more energy to approach my day. Many of my body aches have diminished. I’m getting quality sleep every night for the whole night! This program has helped me feel better than I’ve felt in over a decade.”
Based on years of personal experience, client experience, and research, my Adrenal Transformation Protocol is a comprehensive program designed to boost your energy and help you get your life back.
The Takeaway
Many people endure the exhausting symptoms of fatigue every day. I know firsthand how tiredness and fatigue can impact everyday life and leave you exhausted. Overcoming Hashimoto’s fatigue is an important step in regaining your energy and getting on with life, and the interventions listed above may help with that. You have the power to take back your health.
If you’re looking for more tips, I have a FREE eBook that includes a summary of the most helpful strategies to overcome fatigue in a simple and easy-to-read format. Sign up below to join my mailing list and download the eBook today:
If you suspect that your adrenals may be at the root of your fatigue, I highly recommend exploring my Adrenal Transformation Protocol. The protocol has helped over 80 percent of people who completed it reduce their brain fog, reduce fatigue, reduce anxiety, and improve their mood, to name just a few of the incredible changes.
I hope that this information helps you to get your energy back soon!
P.S. I love interacting with my readers on social media, and I encourage you to join my Facebook, Instagram, TikTok, and Pinterest community pages to stay on top of thyroid health updates and meet others who are following similar health journeys. For recipes, a FREE Thyroid Diet start guide, notifications about upcoming events, and the Nutrient Depletions and Digestion chapter from my first book for free, be sure to sign up for my email list!
References
[1] Brownstein D. Overcoming Thyroid Disorders. West Bloomfield, MI: Medical Alternatives Press; 2008.
[2] Samuels MH. Effect of thyroid function variations within the laboratory reference range on health status, mood, and cognition in levothyroxine-treated subjects. Thyroid. 2016;26:1173–1184.
[3] Meier C. TSH-controlled L-thyroxine therapy reduces cholesterol levels and clinical symptoms in subclinical hypothyroidism: a double blind, placebo-controlled trial (Basel Thyroid Study) J. Clin. Endocrinol. 2001;86:4860–4866.
[4] Kopp PA. Commentary on: guidelines for the treatment of hypothyroidism. Thyroid. 2014;24:1667–1669.
[5] Samuels MH, Kolobova I, Smeraglio A, Niederhausen M, Janowsky JS, Schuff KG. Effect of Thyroid Function Variations Within the Laboratory Reference Range on Health Status, Mood, and Cognition in Levothyroxine-Treated Subjects. Thyroid. 2016;26(9):1173-1184. doi:10.1089/thy.2016.0141
[6] Shahid MA, Ashraf MA, Sharma S. Physiology, Thyroid Hormone. In: StatPearls. Treasure Island (FL): StatPearls Publishing; May 8, 2022.
[7] Saravanan P. Psychological well-being in patients on ‘adequate’ doses of l-thyroxine: results of a large, controlled community-based questionnaire study. Clin. Endocrinol. 2002;57:577–585.; Wekking E.M. Cognitive functioning and well-being in euthyroid patients on thyroxine replacement therapy for primary hypothyroidism. Eur. J. Endocrinol. 2005;153:747–753.; Winther KH. Disease-specific as well as generic quality of life is widely impacted in autoimmune hypothyroidism and improves during the first six months of levothyroxine therapy. PLoS One. 2016;11.; Walsh JP. Small changes in thyroxine dosage do not produce measurable changes in hypothyroid symptoms, well-being, or quality of life: results of a double-blind, randomized clinical trial. J. Clin. Endocrinol. 2006;91:2624–2630.
[8] Stabler SP, Allen RH. Vitamin B12 deficiency as a worldwide problem. Annu Rev Nutr. 2004;24:299-326. doi:10.1146/annurev.nutr.24.012003.132440; Office of dietary supplements – vitamin B12. NIH Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/VitaminB12-HealthProfessional/. Published March 9, 2022. Accessed July 20, 2022.
[9] Mayer G, Kröger M, Meier-Ewert K. Effects of vitamin B12 on performance and circadian rhythm in normal subjects. Neuropsychopharmacology. 1996;15(5):456-464. doi:10.1016/S0893-133X(96)00055-3
[10] Stough C, Simpson T, Lomas J, et al. Reducing occupational stress with a B-vitamin focussed intervention: a randomized clinical trial: study protocol. Nutr J. 2014;13(1):122. Published 2014 Dec 22. doi:10.1186/1475-2891-13-122
[11] Hanna S, Lachover L, Rajarethinam RP. Vitamin b₁₂ deficiency and depression in the elderly: review and case report. Prim Care Companion J Clin Psychiatry. 2009;11(5):269-270. doi:10.4088/PCC.08l00707; Serin HM, Arslan EA. Neurological symptoms of vitamin B12 deficiency: analysis of pediatric patients. Acta Clin Croat. 2019;58(2):295-302. doi:10.20471/acc.2019.58.02.13; Jatoi S, Hafeez A, Riaz SU, Ali A, Ghauri MI, Zehra M. Low Vitamin B12 Levels: An Underestimated Cause Of Minimal Cognitive Impairment And Dementia. Cureus. 2020;12(2):e6976. Published 2020 Feb 13. doi:10.7759/cureus.6976
[12] Collins AB, Pawlak R. Prevalence of vitamin B-12 deficiency among patients with thyroid dysfunction. Asia Pac J Clin Nutr. 2016;25(2):221-6. doi: 10.6133/apjcn.2016.25.2.22.
[13] Anemia: Vitamin B12-Deficiency. National Heart, Lung, and Blood Institute. Updated March 24, 2022. Accessed August 30, 2022. https://www.nhlbi.nih.gov/health/anemia/vitamin-b12-deficiency-anemia
[14] Paul C, Brady DM. Comparative Bioavailability and Utilization of Particular Forms of B12 Supplements With Potential to Mitigate B12-related Genetic Polymorphisms. Integr Med (Encinitas). 2017;16(1):42-49.
[15] Mishra AK, Tiwari A. Iron overload in Beta thalassaemia major and intermedia patients. Maedica (Bucur). 2013;8(4):328-332.
[16] Knovich MA, Storey JA, Coffman LG, Torti SV, Torti FM. Ferritin for the clinician. Blood Rev. 2009;23(3):95-104. doi:10.1016/j.blre.2008.08.001; Schulte EC, Kaffe M, Schormair B, Winkelmann J. Iron in Restless Legs Syndrome. Mov Disord Clin Pract. 2014;1(3):161-172. Published 2014 Jun 12. doi:10.1002/mdc3.12047
[17] Breymann C, Römer T, Dudenhausen JW. Treatment of Iron Deficiency in Women. Geburtshilfe Frauenheilkd. 2013;73(3):256-261. doi:10.1055/s-0032-1328271
[18] Crider KS, Yang TP, Berry RJ, Bailey LB. Folate and DNA methylation: a review of molecular mechanisms and the evidence for folate’s role. Adv Nutr. 2012;3(1):21-38. doi:10.3945/an.111.000992
[19] Arakawa Y. Association of polymorphisms in DNMT1, DNMT3A, DNMT3B, MTHFR and MTRR genes with global DNA methylation levels and prognosis of autoimmune thyroid disease. Clinical and Experimental Immunology. 170:194–201.
[20] Servy EJ, Jacquesson-Fournols L, Cohen M, Menezo YJR. MTHFR isoform carriers. 5-MTHF (5-methyl tetrahydrofolate) vs folic acid: a key to pregnancy outcome: a case series. J Assist Reprod Genet. 2018;35(8):1431-1435. doi:10.1007/s10815-018-1225-2
[21] Aledo JC. Methionine in proteins: The Cinderella of the proteinogenic amino acids. Protein Sci. 2019;28(10):1785-1796. doi:10.1002/pro.3698
[22] Allergy vs intolerance: Allergy UK: National Charity. Allergy UK | National Charity. https://www.allergyuk.org/about-allergy/allergy-vs-intolerance. Accessed July 20, 2022.; Coucke F. Food intolerance in patients with manifest autoimmunity. Observational study. Autoimmun Rev. 2018;17(11):1078-1080. doi:10.1016/j.autrev.2018.05.011
[23] Fritschi C, Park C, Quinn L, Collins EG. Real-Time Associations Between Glucose Levels and Fatigue in Type 2 Diabetes: Sex and Time Effects. Biol Res Nurs. 2020;22(2):197-204. doi:10.1177/1099800419898002; Askani E, Rospleszcz S, Lorbeer R, et al. Association of MRI-based adrenal gland volume and impaired glucose metabolism in a population-based cohort study. Diabetes Metab Res Rev. 2022;38(5):e3528. doi:10.1002/dmrr.3528
[24] Kozacz A, Assis GG, Sanocka U, Ziemba AW. Standard hypothyroid treatment did not restore proper metabolic response to carbohydrate. Endocrine. 2021;71(1):96-103. doi:10.1007/s12020-020-02334-0
[25] Martínez García RM, Jiménez Ortega AI, López Sobaler AM, Ortega RM. Estrategias nutricionales que mejoran la función cognitiva [Nutrition strategies that improve cognitive function]. Nutr Hosp. 2018;35(Spec No6):16-19. Published 2018 Sep 7. doi:10.20960/nh.2281; Jones JL, Fernandez ML, McIntosh MS, et al. A Mediterranean-style low-glycemic-load diet improves variables of metabolic syndrome in women, and addition of a phytochemical-rich medical food enhances benefits on lipoprotein metabolism. J Clin Lipidol. 2011;5(3):188-196. doi:10.1016/j.jacl.2011.03.002; Szypowska A, Regulska-Ilow B. Significance of low-carbohydrate diets and fasting in patients with cancer. Rocz Panstw Zakl Hig. 2019;70(4):325-336. doi:10.32394/rpzh.2019.0083; Larsen TM, Dalskov SM, van Baak M, et al. Diets with high or low protein content and glycemic index for weight-loss maintenance. N Engl J Med. 2010;363(22):2102-2113. doi:10.1056/NEJMoa1007137
[26] Divyanshoo Rai Kohli MD. Achlorhydria clinical presentation: History. Achlorhydria Clinical Presentation: History. https://emedicine.medscape.com/article/170066-clinical. Published October 6, 2021. Accessed July 21, 2022.
[27] Yago MR, Frymoyer AR, Smelick GS, et al. Gastric reacidification with betaine HCl in healthy volunteers with rabeprazole-induced hypochlorhydria. Mol Pharm. 2013;10(11):4032-4037. doi:10.1021/mp4003738; Russell RM. Factors in aging that effect the bioavailability of nutrients. J Nutr. 2001;131(4 Suppl):1359S-61S. doi:10.1093/jn/131.4.1359S
[28] Hovsepian S, Amini M, Aminorroaya A, Amini P, Iraj B. Prevalence of vitamin D deficiency among adult population of Isfahan City, Iran. J Health Popul Nutr. 2011;29(2):149-155. doi:10.3329/jhpn.v29i2.7857
[29] Office of Dietary Supplements. Vitamin D – Health Professional Fact Sheet. National Institutes of Health. https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/. Updated August 12, 2022. Accessed August 26, 2022.; Mackawy AM, Al-Ayed BM, Al-Rashidi BM. Vitamin d deficiency and its association with thyroid disease. Int J Health Sci (Qassim). 2013;7(3):267-275. doi:10.12816/0006054
[30] Tamer G, Arik S, Tamer I, Coksert D. Relative vitamin D insufficiency in Hashimoto’s thyroiditis. Thyroid. 2011;21(8):891-896. doi:10.1089/thy.2009.0200
[31] 10 Surprising Facts About Indoor Tanning. American Academy of Dermatology Association. Updated July 11, 2022. Accessed August 29, 2022. https://www.aad.org/public/diseases/skin-cancer/surprising- facts-about-indoor-tanning
[32] Tuunainen A, Kripke DF, Endo T. Light therapy for non-seasonal depression. Cochrane Database Syst Rev. 2004;2004(2):CD004050. doi:10.1002/14651858.CD004050.pub2; Chandra P, Wolfenden LL, Ziegler TR, et al. Treatment of vitamin D deficiency with UV light in patients with malabsorption syndromes: a case series. Photodermatol Photoimmunol Photomed. 2007;23(5):179-185. doi:10.1111/j.1600-0781.2007.00302.x; Maruani J, Geoffroy PA. Bright Light as a Personalized Precision Treatment of Mood Disorders. Front Psychiatry. 2019;10:85. Published 2019 Mar 1. doi:10.3389/fpsyt.2019.00085
[33] Trefts E, Gannon M, Wasserman DH. The liver. Curr Biol. 2017;27(21):R1147-R1151. doi:10.1016/j.cub.2017.09.019
[34] Mokhtari V, Afsharian P, Shahhoseini M, Kalantar SM, Moini A. A Review on Various Uses of N-Acetyl Cysteine. Cell J. 2017;19(1):11-17. doi:10.22074/cellj.2016.4872
[35] Malik R, Hodgson H. The relationship between the thyroid gland and the liver. QJM. 2002;95(9):559-569. doi:10.1093/qjmed/95.9.559
[36] Lonsdale D. A review of the biochemistry, metabolism and clinical benefits of thiamin(e) and its derivatives. Evid Based Complement Alternat Med. 2006;3(1):49-59. doi:10.1093/ecam/nek009
[37] WebMD. L-CARNITINE: Uses, Side Effects, Interactions and Warnings. WebMD. https://www.webmd.com/vitamins-supplements/ingredientmono-1026-L-CARNITINE.aspx. Accessed March 2, 2018.; Tejani AM, Wasdell M, Spiwak R, Rowell G, Nathwani S. Carnitine for fatigue in multiple sclerosis. Cochrane Database of Systematic Reviews. 2012;5. DOI: 10.1002/14651858.CD007280.pub3.; Tomassini V, Pozzilli C, Onesti E, Pasqualetti P, Marinelli F, Pisani A, et al. Comparison of the effects of acetyl L- carnitine and amantadine for the treatment of fatigue in multiple sclerosis: results of a pilot, randomised, double- blind, crossover trial. Journal Neurological Sciences. 2004; 218(1-2):103–8.
[38] Flanagan JL, Simmons PA, Vehige J, Willcox MD, Garrett Q. Role of carnitine in disease. Nutr Metab (Lond). 2010;7:30. Published 2010 Apr 16. doi:10.1186/1743-7075-7-30
[39] An JH, Kim YJ, Kim SH, et al. L-carnitine supplementation for the management of fatigue in patients with hypothyroidism on levothyroxine treatment: a randomized, double-blind, placebo-controlled trial. Endocr J. 2016;63(10):885-895.
[40] Ringseis R, Keller J, Eder K. Role of carnitine in the regulation of glucose homeostasis and insulin sensitivity: evidence from in vivo and in vitro studies with carnitine supplementation and carnitine deficiency. Eur J Nutr. 2012 Feb;51(1):1-18. doi: 10.1007/s00394-011-0284-2.
[41] Office of Dietary Supplements. Carnitine – Health Professional Fact Sheet. National Institutes of Health. https://ods.od.nih.gov/factsheets/Carnitine-HealthProfessional/ Updated March 29, 2021. Accessed August 26, 2022.
[42] Kuratsune H, Yamaguti K, Takahashi M, Misaki H, Tagawa S, Kitani T. Acylcarnitine deficiency in chronic fatigue syndrome. Clin Infect Dis. 1994;18 Suppl 1:S62-S67. doi:10.1093/clinids/18.supplement_1.s62; Smeland OB, Meisingset TW, Borges K, Sonnewald U. Chronic acetyl-L-carnitine alters brain energy metabolism and increases noradrenaline and serotonin content in healthy mice. Neurochem Int. 2012;61(1):100-107. doi:10.1016/j.neuint.2012.04.008; Benvenga S, Feldt-Rasmussen U, Bonofiglio D, Asamoah E. Nutraceutical Supplements in the Thyroid Setting: Health Benefits beyond Basic Nutrition. Nutrients. 2019;11(9):2214. Published 2019 Sep 13. doi:10.3390/nu11092214
[43] Cioffi F, Giacco A, Goglia F, Silvestri E. Bioenergetic Aspects of Mitochondrial Actions of Thyroid Hormones. Cells. 2022;11(6):997. Published 2022 Mar 15. doi:10.3390/cells11060997; An JH, Kim YJ, Kim KJ, et al. L-carnitine supplementation for the management of fatigue in patients with hypothyroidism on levothyroxine treatment: a randomized, double-blind, placebo-controlled trial. Endocr J. 2016;63(10):885-895. doi:10.1507/endocrj.EJ16-0109; Virmani MA, Cirulli M. The Role of l-Carnitine in Mitochondria, Prevention of Metabolic Inflexibility and Disease Initiation. Int J Mol Sci. 2022;23(5):2717. Published 2022 Feb 28. doi:10.3390/ijms23052717
[44] Lovallo WR, Farag NH, Vincent AS, Thomas TL, Wilson MF. Cortisol responses to mental stress, exercise, and meals following caffeine intake in men and women. Pharmacol Biochem Behav. 2006;83(3):441-447. doi:10.1016/j.pbb.2006.03.005; O’Callaghan F, Muurlink O, Reid N. Effects of caffeine on sleep quality and daytime functioning. Risk Manag Healthc Policy. 2018;11:263-271. Published 2018 Dec 7. doi:10.2147/RMHP.S156404; Ryu KY, Roh J. The Effects of High Peripubertal Caffeine Exposure on the Adrenal Gland in Immature Male and Female Rats. Nutrients. 2019;11(5):951. Published 2019 Apr 26. doi:10.3390/nu11050951
Note: Originally published in May 2015, this article has been revised and updated for accuracy and thoroughness.


 Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Hi,
what does high level of reverse T3 mean? Is there a good range?
Thanks
Best regards
Boo – thank you for reaching out. Reverse T3 is an inactive molecule related to T3 but without any physiological activity—it is a dud that just takes up space! Under stressful situations, T4 gets converted to reverse T3 instead of T3. You can find more information on Reverse T3 in my book Hashimoto’s Root Cause. Here is an article you may find helpful as well:
STRATEGIES TO OVERCOME HASHIMOTO’S FATIGUE
https://thyroidpharmacist.com/articles/strategies-overcome-hashimotos-fatigue/
Wow! So much info! Which supplements should I take? How to know? Insurance doesn’t cover the testing that you talk about and I can’t afford it out of pocket. Depressing.
Kathy – thank you for reaching out! I understand how overwhelming this can all be. <3 Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO'S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year
Thank you so much for your informative articles!
Do you have any suggestions for someone taking NDT, and their FT3 and FT4 are in the low end of normal range, but their TSH is very low at .02?
Vicky – you are very welcome! <3 I am so sorry to hear you are struggling with this. Most people feel best with a TSH of around 1 or lower and with a Free T4 and Free T3 in the upper half of the range. It is expected that your TSH will be very suppressed when optimal on NDT medication. How much thyroid replacement therapy is needed is unique and different for each person, so it's important to work with a functional medicine practitioner or a doctor, who can closely monitor your dosage and your progress. Every six weeks is usually a good schedule for testing your thyroid hormones. Here are some articles you might find helpful:
TSH
https://thyroidpharmacist.com/articles/what-to-do-if-your-tsh-is-normal-and-you-are-anything-but/
TOP 6 THYROID TESTS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests
ARE YOU GOING CRAZY OR IS IT JUST YOUR THYROID?
https://thyroidpharmacist.com/articles/are-you-going-crazy-or-is-it-just-your-thyroid/
Hi Isabella,
I have eaten red meat once a week for a few years, but was veg for the 20 years prior. Is there a test or a symptom that can tell me if I am L- carnitine deficient? Thank you for the work you do. I follow your research habitually!
Sky – thank you for reaching out and sharing. <3 Here is another article where I discuss L-carnitine that you might find helpful:
VEGAN DIETS AND HASHIMOTO'S
https://thyroidpharmacist.com/articles/vegan-diets-and-hashimotos/
Is there a Canadian brand of betaine with pepsin? I would really like to try this but they don’t ship to Canada. ?
Melanie – thank you so much for your interest in my Rootcology products! I’m sorry we are not able to ship internationally. Please email my team at info@rootcology.com and they will be happy to give you an alternative.
Dear Isabella;
I’m perplex; my thyroid was removed in 2009; I took a T4 supplementation: Levothyrox 125, then 112,5. Then I had several problems (fatigue, insomnia, pain, fibromyalgia etc, altogether 32 symptoms from the hypothyroidism symptom list. I was unable to take T3 (that generated a lot of heart palpitations).
The antibody tests don’t work for me (thyroid surgically removed); would that be possible for you to suggest another method for Hashimoto diagnostic? I would then hopefully meet a specialized health care pratictioner here in Paris (any recommendation?).
In France 95% of endicronologist just read the TSH results and are not interested in patient’s symptoms, they simply conclude that you are in a very good health; some are not lucky and are sent in psychiatry.
I went to Belgium to see a good MD specialist; he diagnosed in 2017 that I had [infra] clinical hypothyroidism since my infancy! (I am 72).
Thank you for your help!
Madeleine – thank you so much for reaching out and sharing your journey. I am so sorry you are struggling with all of this. Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism, it’s an autoimmune disease that needs to be managed. Whether you have all, part or no thyroid, the autoimmunity still persists in most cases. We need to re-balance the immune system which begins in the gut. With the exception of discussing proper thyroid medication dosing, the majority of my website and book’s focuses on balancing the immune system. The info I present is based on my own research and journey overcoming my autoimmune thyroid condition.
Here are some articles I think you might find helpful:
IMPORTANCE OF GUT HEALTH
https://thyroidpharmacist.com/articles/importance-gut-health/
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
Thank you so much for your story and information! I am going through this exact situation. I was diagnosed with Lupus first, then when that was taken off the board, i was told Celiac. Most recently though is IGG of the pancreas. I have lost my large intestine to I.B.S. and i have a J Pouch now. I am going to see a G.I doctor in October for more information. Im on a steroid because everything i eat goes straight through me. Its helping, but not completely. Im not digesting my food properly. So with that being said, do you think your supplements will help me? I dont want to hinder any future testing, but i cant live like this anymore! I am crawling out of bed, and have lost so much strength! My latest lab tests say my thyroid levels are borderline. I will be rechecked in 4 to 6 months. I am not even sure i will absorb them, but im at the end of my rope, and just want some answers. Im following you and praying for a end to this. I just got my first B12 shot, but havent felt an improvement yet.Ive been sick for a long time. But i just keep pushing through it. Sorry this is so long, i just feel like im going crazy! xoxo
Maribeth – thank you so much for reaching out and sharing your journey with me. <3 We know that intestinal permeability (aka leaky gut) is present in every case of autoimmunity and often precedes the development of Hashimoto’s. Symptoms of leaky gut may include bloating, diarrhea, constipation, stomach aches, acid reflux and irritable bowel syndrome. According to the Institute of Functional Medicine, many people develop IBS 5-10 years before an autoimmune diagnosis. I was one of them and didn’t take my gut health as seriously as I should have. Gut problems are often caused by infections like H. pylori, parasites like Blasto, SIBO, an imbalance of bacteria, and enzyme deficiencies or food sensitivities (especially to gluten, dairy, and/or soy). Even stress can be a factor in gut permeability. Gut healing is a journey; you may need various interventions like removing reactive foods and infections, taking enzymes and probiotics, and balancing nutrients. Remember, be kind to yourself and learn to listen to your body so that you can support and feed it properly! You are worth it! You may find this article helpful as well!
WHAT'S CAUSING YOUR LEAKY GUT
https://thyroidpharmacist.com/articles/whats-causing-your-leaky-gut/
SUPPLEMENTS ACTUALLY HELP HASHIMOTO’S
https://thyroidpharmacist.com/articles/which-supplements-actually-help-hashimotos/
I believe that everyone needs to find a practitioner as well, that will let her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It’s a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
COMPOUNDING PHARMACIES
https://thyroidpharmacist.com/database-recommended-compounding-pharmacies/
This is incredible! I received my first Iron IV and blood transfusion last year, due to chronic anemia. Yet my symptoms never stopped. Doctors did the basic thyroid test like x3 already. My first test showed, low Ferratin, Low Haemoglobin, low B12, low D3… Early this year i went for more extensive test – Blood gas, Doppler test, etc. Up until today i still have no clue whats wrong with me. Yet after listening to your interview with Dr G, I just had to review your page. Whats the chances hey.
What kind of test over and above the normal Thyroid test can i request to be done to confirm my diagnosis? I have copies of my test and will review the results as per the above advise. However, i will need need new test to be done. Will appreciate your time to review and advise. Thank you so much.
Jacky – thank you for reaching out and sharing your journey. <3 Here are the tests you need for diagnosis. Most endocrinologists don't run them all so you will have to request them.
¨ TSH
¨ TPO Antibodies
¨ Thyroglobulin Antibodies
¨ Free T4
¨ Free T3
¨ Reverse T3 (optional)
¨ Thyroid Ultrasound (optional)
Here are some research articles which might help further:
TOP 10 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
Most Common Nutrient Deficiencies
https://thyroidpharmacist.com/articles/most-common-nutrient-deficiencies-hashimotos/
Hi, I was just recently diagnosed with hypothyroidism and I read in my own search on the web to stop taking L-Carnitine but here you say it is helpful so now I’m confused LOL! I loved taking it but thought it was more harmful than helpful for hypothyroidism? Can you tell me why some say to avoid it? I’d really love to start taking it again but don’t want to make my condition worse. Thank you for all you do, I’m reading everything I can by you 🙂
Jennifer – thank you for reaching out. I generally recommends L-carnitine to people with Hashimoto’s to help overcome thyroid fatigue. She has personally seen people “awaken” with the use of L-carnitine. L-carnitine helps transport fatty acids into the mitochondria where they can be burned up and used as fuel. L-carnitine levels may be decreased in hypothyroidism, potentially due to reduced synthesis of L-carnitine while we are in a hypothyroid state. Taking a thyroid medication can boost the production of L-carnitine, but it can also work as a vacuum, taking the L-carnitine from the body and resulting in an overall deficiency of it. The results of a recent study regarding L-carnitine supplementation for the management of fatigue in patients with hypothyroidism found that L-carnitine may be useful in alleviating fatigue symptoms in hypothyroid patients, especially in those younger than 50 and those who have hypothyroidism due to a thyroidectomy. In the study, 60 patients who were experiencing fatigue were given L-carnitine for 12 weeks. A dose of 1,980 mg was given to 30 people who were taking thyroid hormones (either due to Hashimoto’s or post-thyroidectomy), while 30 people received a placebo. After 12 weeks, the researchers noted that the group receiving L-carnitine did indeed show improvements in fatigue, with the most significant improvements seen in “brain fatigue.” I recommend you consult with your doctor to see if L-carnitine supplementation is right for you.
Hi – Thank you for this great article! What can cause waking up during the night and not being able to get back to sleep? Is that a blood sugar issue or adrenal? It happens to me almost every night and then I’m so tired throughout the day. I usually don’t drink more than 1-2 caffeine drinks per day and the latest is between 12 and 3 pm.
Thank you
Angie – thank you for reaching out. <3 I am so sorry you are having trouble staying asleep. Caffeine is known to interfere with sleep, and because most of our liver detoxifying and healing takes place when we’re sleeping, we want to avoid anything that may interfere with sleep. We want to give the body every opportunity to heal. Additionally, caffeine weakens the adrenals and can increase gut permeability. Tea is problematic because of fluoride content, while coffee has the potential to contain mold or cross-react with gluten.
Research has also shown that when people with autoimmune thyroid disease took magnesium citrate for six weeks, they reported feeling better with more energy, better sleep, less anxiety, and less constipation. These patients also had reductions in TSH! Magnesium citrate and magnesium glycinate are great sources of oral magnesium supplements.
Here are some articles I hope you find helpful:
ARE YOUR ADRENALS SABOTAGING YOUR HEALTH?
https://thyroidpharmacist.com/articles/are-your-adrenals-sabotaging-your-health
NEW STUDIES ON MAGNESIUM AND THYROID HEALTH
https://thyroidpharmacist.com/articles/new-studies-on-magnesium-and-thyroid-health
CONTROVERSY COFFEE AND YOUR THYROID
https://thyroidpharmacist.com/articles/controversy-coffee-bad-thyroid-myths-truths/
I’m really confused on the iron thing. My iron bloodwork is on the high end but my ferritin is on the low end. What’s the difference between the two? I’m afraid to supplement with the wrong thing.
Gina – thank you for reaching out. I am so sorry you are struggling with this. <3 Ferritin is our iron storage protein. Hashimoto's and low iron go together as leaky gut makes it hard to absorb iron from your diet. These are the ferritin levels from my book, page 83. Normal ferritin levels for women are between 12 and 150 ng/mL. Ferritin levels of at least 40 ng/ml are required to stop hair loss, while levels of at least 70 ng/ml are needed for hair regrowth. The optimal ferritin level for thyroid function is between 90-110 ng/ml. Here are some resources you might find helpful:
7 MOST IMPORTANT NUTRIENT DEFICIENCIES IN HASHIMOTO'S
https://thyroidpharmacist.com/articles/6-important-nutrient-deficiencies-hashimotos/
HAIR LOSS AND YOUR THYROID
https://thyroidpharmacist.com/articles/hair-loss-and-thyroid
I have a couple of things that I have an issue with. First one is the worst, I wake up feeling like crud. I cannot figure out why not. Also, the other thing is I will feel good and then all of a sudden I feel like crap for like 5 days and I can’t figure out what I did wrong. I think the biggest thing I would like to fix is waking up in the morning feeling so bad. I would love it if anybody has any input on that. I cannot seem to find the answer.
Jo – thank you so much for sharing. I’m so sorry you are struggling with all of this. <3 Hashimoto’s is often a combination of food sensitivities, nutrient deficiencies, adrenal issues, gut issues as well as an impaired ability to get rid of toxins. Any of those things would prevent a person from getting better.
Hashimoto's is very much an individual condition. While there are root cause commonalities, each person will have their own or in some cases, more than one root cause. You will have to start with the simplest modifications, by removing triggers, followed by repairing the other broken systems to restore equilibrium, allowing the body to rebuild itself. You will need to dig down to why the immune system is imbalanced in the first place and this will tell you how you begin to finally feel better, reduce your thyroid antibodies and even take your condition into remission.
You will have to create your own health timeline. Look back at your overall history as far back as you can remember. Look for infections, periods of severe stress, the use of medications (especially antibiotics, antacids, and oral contraceptives), accidents, and exposure to toxins. These are events that may have contributed to Hashimoto's. Once you do, you will know what types of changes you need to implement to make yourself feel better.
If you need further support, please check out the list of lab tests inside the “Testing” chapter of my book, Hashimoto’s Root Cause. I also offer a 12-week program, Hashimoto's Self Management Program. Here are some resources I hope you find helpful as well.
BUILDING YOUR OWN HEALTH TIMELINE
https://thyroidpharmacist.com/sample-health-timeline/
Hashimoto’s Self-Management Program
https://thyroidpharmacist.com/enroll-in-hashimotos-self-management/
ROOT CAUSE RESET
https://thyroidpharmacist.com/enroll-in-root-cause-reset/
How does the Hashimoto’s Self-Management Program differ from following the Hashimoto’s Protocol?
Christine – thank you for reaching out. ❤️ The Hashimoto’s Self-Management Program was born from my Hashimoto’s Protocol book. What I love about this program, specifically, is that it caters to all learning styles with the workbooks, videos, and audio recordings that are included within it. The best way to describe the difference between the book and the program is that it’s similar to owning a textbook versus actually being in a class with the teacher. I was limited as to the information I could put into a specific amount of pages in the book; not so in the program! Here are a couple resources I hope you find helpful:
HASHIMOTO’S SELF-MANAGEMENT PROGRAM
https://thyroidpharmacist.com/enroll-in-hashimotos-program/
HASHIMOTO’S PROTOCOL
https://www.amazon.com/Hashimotos-Protocol-Reversing-Thyroid-Symptoms/dp/006257129X?tag=thyroipharma-20&geniuslink=true
There’s something I’ve been scratching my head on for a while. You quite rightly call out the problems with petrochemicals. Isn’t mineral oil a petrochemical? It’s one of the fillers in NP Thyroid. Would someone with a known sensitivity to petrochemicals be better off switching to a different option?
Hi Heather, You’re right, mineral oil is derived from petroleum and is considered a petrochemical. It is used as an inactive ingredient in some thyroid medications, including NP Thyroid. For most people, this ingredient does not cause issues, but for those with a known sensitivity to petrochemicals, it may trigger reactions. If you suspect this could be a problem for you, it’s important to discuss alternatives with your practitioner. They can help determine if a different thyroid medication without that ingredient might be a better fit for your health and sensitivities.