Iodine is a controversial topic with regard to thyroid health. While I’ve discussed the dangers of high doses of iodine for Hashimoto’s in my books, I wanted to address the topic in an article and make sure that the conversation doesn’t turn into a debate about a single nutrient, as Hashimoto’s is a multi-factor and full body condition.
While some thyroid advocates will propose that taking high doses of iodine is helpful for everyone with Hashimoto’s, unfortunately, I have not found that to be the case for most.
As a pharmacist, I am often reminded that “the only difference between a medicine and a poison is the dose.” This is a wise old quote from Paracelsus, who is credited as the father of modern toxicology.
Thus, not surprisingly, while physiological doses of iodine can benefit thyroid function, research has shown that excessive doses of iodine can trigger (and worsen) Hashimoto’s in people who are genetically predisposed to Hashimoto’s and may have certain “vulnerabilities”, such as a selenium deficiency.
Furthermore, temporary iodine restriction may actually improve and even normalize thyroid function, in some individuals.
Because I see the question over iodine come up so often, I’d like to address the topic in this article, where I’ll cover:
- The controversy around iodine
- How iodine affects Hashimoto’s
- The sweet spot for iodine
- What to do if you suspect you have excess iodine
- The low iodine diet approach
The Iodine Controversy
Iodine is an essential mineral that is found in the earth’s soil and water, and is used by the body to produce thyroid hormones. Iodine is typically consumed through seafood (fish and vegetables), iodized salt, or through supplementation.
Thyroid cells are the only cells in the body which can absorb iodine, and it is the role of the thyroid gland to combine iodine and the amino acid tyrosine, and convert them into thyroid hormones: thyroxine (T4) and triiodothyronine (T3).
Because it is a necessary nutrient for thyroid health, some people have assumed that supplementing with high doses of iodine can help the body make more thyroid hormone, thereby improving hypothyroidism and Hashimoto’s; and it is often recommended by many conventional health books and doctors. However, what they do not understand is that iodine is what pharmacists call a “Goldilocks” nutrient, meaning that, while low levels are necessary for thyroid health, higher levels can have a negative effect.
In my own practice, I have seen iodine harm people with Hashimoto’s, so I feel the need to caution people about supplementing with high doses of this nutrient, unless they have a known deficiency. However, even in the case of deficiency, taking too much at once can be toxic.
One reader wrote in to tell me:
I was given Iodine for a short spurt and my TSH went up to 98 and my antibodies up to 9800 after about 3 months. I think it can be deceiving. I would only do it with a doctor who understands the delicate balance with selenium. I regret that time in my journey now. It was with someone who did the simple iodine test on the hand and determined the dosage by muscle testing. I would not advise that for others.
Any supplement can have an adverse reaction in an individual, and I wish this was a one time report, but I have received countless messages like the one above, and have seen many similar reports in clients who came to me after trying high dose iodine on their own, or with other practitioners.
Initially, a person given iodine may experience more energy, but they then crash and feel worse. This is because iodine, given to a subset of people with Hashimoto’s, can make the thyroid produce more hormone initially, but unfortunately, in doing so without having enough selenium and antioxidants on board, the increased hormone production creates lots of free radicals, which can flare up the attack on the thyroid gland.
Iodine needs to be processed by the thyroid gland, and when the thyroid is inflamed, the processing of iodine will likely produce more inflammation. If you give an angry and overwhelmed organ more work to do, you’ll likely see it become even angrier!
A person may feel more energetic when first starting an iodine supplement, but lab tests will reveal that their “new energy” is coming from the destruction of thyroid tissue, which dumps thyroid hormone into the circulation. Reports will show an elevated TSH, elevated thyroid antibodies, and in some cases, low levels of active thyroid hormones.
This is why I don’t generally recommend iodine supplements to people with Hashimoto’s. I don’t believe that the short-term artificial boost in energy is worth destroying your thyroid gland!
I’ve heard the argument that the Japanese population consumes a high level of iodine, due to their seafood-heavy diets, therefore everyone should be taking high doses of iodine. After all, some of the healthiest subpopulations in the world live in Japan.
However, this argument fails to account for a couple of different factors. The first is that different ethnicities may have genetic predispositions for developing Hashimoto’s, and we can’t look at one group of people and make a generalization across all ethnicities, particularly when we know that genetics are a factor in developing an autoimmune condition.
For example, one recent meta analysis found that one particular gene variation, the PTPN22 R620W polymorphism, is associated with elevated autoimmune thyroid disease risk in Caucasians, but not in Asians.
Furthermore, Dr. Alan Christianson, author of The Thyroid Reset Diet, has noted that the Japanese do, in fact, have the highest levels of Hashimoto’s in the world. After all, Dr. Haraku Hashimoto, who the condition is named after (as he was the first to discover it), was a Japanese doctor. 😉
In my role as a researcher and writer, I focus my work on outcomes data, by looking at patterns that are present in a large majority of people with Hashimoto’s.
My goal as a medical professional is always to first do no harm. While a minority of people may indeed be iodine deficient and benefit from supplementing with iodine, that has not been the case for most of my clients.
As a clinician, I focus on each person as an individual, with individual needs, and I encourage everyone to work with a knowledgeable practitioner as well, so that they can find the course of treatment that is best for them.
Iodine, Hypothyroidism and Hashimoto’s
In the past, iodine deficiency used to be a major health concern worldwide. As recently as 1990, people in only a small percentage of countries were getting enough iodine, and 112 countries were categorized by the World Health Organization (WHO) as “severely iodine deficient.”
To address this issue, global health organizations came together and began adding iodine to salt and other fortified foods, and the iodine status of the world’s countries changed over the next two decades. By 2014, the number of nations considered severely iodine deficient plummeted to zero. This was considered a clear win, however we now know that iodine has a narrower range of safety than any other nutrient. Meaning, it is easy to get too much iodine.
As levels of iodine rose in countries around the world, the WHO recognized that excessive iodine can trigger thyroid disease.
According to the WHO, the following levels of daily iodine intake correlate with these conditions:
- <20 mcg: Endemic (native) goiter, congenital hypothyroidism
- 20-49 mcg: Pediatric goiter, low rate of adult disease
- 50-99 mcg: Lowest disease rate and reversal of autoimmune thyroid disease
- 100-199 mcg: Low thyroid disease rate
- 200-299 mcg: Iodine-induced hyperthyroidism, autoimmune thyroid disease, goiter, hypothyroidism
- >300 mcg: Hypothyroidism, goiter, autoimmune thyroid disease
This global spike in iodine consumption over the past two decades, exactly parallels the skyrocketing increase in thyroid diseases such as hypothyroidism, Hashimoto’s, and thyroid cancer. While correlation doesn’t equal causation, the research has supported the theory that excess iodine can lead to thyroid dysfunction.
This has to do with the way that iodine is processed in the body. Iodine from foods and supplements is processed by the thyroid gland so that the body can properly use it. During this process, hydrogen peroxide, a free radical, is released.
In cases when the body has adequate levels of selenium and it is used properly, the selenium neutralizes the hydrogen peroxide. However, in cases of iodine excess, excess hydrogen peroxide can cause oxidative damage to the thyroid gland. When not enough selenium or glutathione is present to neutralize the hydrogen peroxide, oxidative damage, which leads to inflammation and autoimmunity, can occur.

Studies have shown that excess iodine causes thyroid injury by generating reactive oxygen species, which leads to premature damage and programmed cell death in thyroid tissues. These iodine-overloaded cells then release the danger (or damage)-associated molecular patterns (DAMPs), which turn on the autoimmune process in a person with the right genetic predisposition and intestinal permeability.
When we think about this from an evolutionary, adaptive, or even innate body wisdom stance, it makes sense that the body would want to stop the production of excess thyroid hormones that would result from too much iodine. (Read my article on my Safety Theory that explains how hypothyroidism may act as a protective mechanism.)
Research on Excess Iodine and Thyroid Disease
The effects of excess iodine on those with thyroid disease has been studied by researchers. In Germany, for example, a low dose of potassium iodide (250 mcg) was given to 40 people who tested positive for anti-thyroid (TPO) antibodies or had a thyroid ultrasound showing a hypoechogenic (more dense tissue) pattern consistent with Hashimoto’s. A group of 43 subjects with similar characteristics served as a control group.
Nine patients from the iodine group developed thyroid abnormalities, compared with only one person from the control group. Of the nine patients in the iodine arm, seven developed subclinical hypothyroidism, one became hypothyroid, and another hyperthyroid. Positive changes were also seen in TPO antibody levels as well as on the thyroid ultrasound. Three of the seven subclinical hypothyroid patients and the hyperthyroid patient regained normal thyroid function after iodine withdrawal.
Research on Salt Iodization and Thyroid Health
Researchers in Iran were able to document the rates of thyroid peroxidase antibodies (TPOAb) and thyroglobulin antibodies (TgAb) before and after a national salt iodization program started in 1994. In 1983-84, positive TPOAb and positive TgAb were found in 3.2 percent and 4 percent, respectively, of the 465 adults selected for random sampling in Tehran. This sampling was repeated with 1,426 adults in Tehran in 1999-2000, this time showing 12.5 percent positive for TPOAb and 16.8 percent positive for TgAb. The addition of iodine quadrupled the rate of Hashimoto’s within a six-year span!
Iodine does seem to have a dose-responsive effect. A Slovenian study followed the rates of thyroid disorders after the amount of potassium iodide added to the Slovenian salt supply was increased from 10 mg/kg of salt to 25 mg/kg in 1999. This increase resulted in a significant change in the incidence of thyroid disorders. While there was a marked decline in the incidence of iodine deficiency hypothyroidism, the rates of Hashimoto’s more than doubled from the baseline after the increase.
In another study, researchers from the Mayo Clinic in Minnesota tracked the rate of Hashimoto’s thyroiditis in patients from 1935 to 1967. Within two years, the doctors saw an increase in autoimmune thyroid disease caused by iodine fortification in table salt and processed food. Starting with the first decade after iodine fortification, they documented a 2,500 percent increase in Hashimoto’s disease. The earliest rates were 2.1 per every 100,000 persons; by the end of the study, it was up to 54.1 for women under 39, and 94.1 for those over 40.
Research on the Effects of a Low Iodine Diet
The potential benefits of a low iodine diet were demonstrated by one study after researchers observed an interesting phenomenon. When using radioactive iodine as a tool for determining thyroid health in a Radioiodine Uptake Test (a test that may help diagnose hyperthyroidism, hypothyroidism and goiters), doctors have found that the procedure works best when the thyroid is “hungry” for that iodine. As such, they have their patients go on low-iodine diets for several weeks so that their thyroid will take in as much of the radioactive iodine as possible before the procedure.
Researchers have discovered that many people see their thyroid function improve during this period, and wondered if it were just a coincidence or if there was a correlation. They launched clinical trials in which people with significant thyroid disease were put on low-iodine diets and were compared against others with the same degree of thyroid disease who were not on a low-iodine diet. Neither group was given thyroid medication, or any other treatment.
The studies all showed that nearly everyone who was not on the diet saw no improvement to their thyroid function or got worse, while up to 80 percent of those who were on the low-iodine diet experienced normal thyroid function within three to six months.
So, Should You Avoid Iodine Completely?
Given the known effects of excess iodine on thyroid health, the question arises… should we stay away from all sources of iodine? Let’s look at the research.
While there is a bit of controversy about whether people with Hashimoto’s should take iodine or avoid it altogether, a 1999 study in 377 people with Hashimoto’s followed for over 800 days, found that when combined with thyroid hormone therapy, a daily iodine dose of up to 200 mcg/day was able to reduce the patients’ TgAb and the TPOAb antibody levels.
However, the same study also enlisted a group of 375 people without thyroid disease and gave them either 200 mcg per day of iodine, or 1.53 milligrams of iodine, per week. The group that took 200 mcg per day did not have a significant increase in rates of Hashimoto’s. However, the group that got the large dose of iodine/week presented a distinct increase of TgAb as well as TPOAb antibodies, and the incidence of Hashimoto’s thyroiditis was four-fold higher than in the two other subgroups!
This study showed that a low dose of iodine (i.e. below 200 mcg) on a daily basis, is usually not going to be problematic for most people with Hashimoto’s, and in fact may be beneficial. (We’ll talk more about low iodine diets, further on in this article!)
Testing for Iodine Deficiency
While testing a low iodine diet can be helpful to many people, and iodine deficiency is relatively rare in those with Hashimoto’s, it’s important to note that for some people, addressing an iodine deficiency may actually be key to improving one’s thyroid health. (As such, it’s important to know whether you have excess or low levels of iodine.)
Some potential factors that may lead me to suspect an iodine deficiency include: eating a vegan diet, eating a diet low in seafood, having fibrocystic breasts (though this could be caused by magnesium deficiency), having low reverse T3 on a lab test, or a experiencing a negative reaction to selenium (which is very rare).
I often get the question about testing for iodine deficiency — do blood tests, urine tests or “spot” tests (where you paint yourself with iodine until it disappears) actually work? Are they accurate? Unfortunately, these tests are not able to reveal an iodine deficiency or excess, rather they will be reflective of your recent iodine intake.
That said, iodine testing can be helpful in order to determine if your average diet and lifestyle contains excess iodine. The most helpful test involves checking one’s urinary iodine to creatinine ratio. The amount of iodine in your urine is compared against the amount of a normal kidney protein, called creatinine.
This urinary iodine to creatinine ratio is tested with a urine collection and can be done at home and mailed in for convenience. The test will not tell you how much iodine you are taking in, but if you are working to reduce iodine levels to help your thyroid function, it can help you determine if you have eliminated enough hidden sources of iodine.
The urinary test results are reported as a mcg of iodine per gram of creatinine, abbreviated as mcg/G. If your levels are over 100 mcg/G, you have not eliminated enough hidden sources of iodine. The goal is to be under 100 mcg/G. The higher your scores are above this range, the more iodine you are still ingesting. You can use this as a clue that you need to find and eliminate other sources of iodine in your diet or personal care products.
In the case of a deficiency of iodine, I do recommend iodine supplements but only in the dose range found in multivitamins (like Nutrient 950 by Pure Encapsulations) and prenatal vitamins (most contain between 150 mcg–220 mcg), rather than in megadoses of iodine.
Recommended Daily Iodine Intake
That said, for both those with excess iodine and iodine deficiency, I would caution against using a dose above 200 mcg/day unless breastfeeding or pregnant (the general recommended daily allowance of iodine is 150 mcg for non-pregnant persons; 220 mcg and 290 mcg for pregnant and breastfeeding women, respectively). This includes your intake from supplements as well as high iodine-containing foods like seaweed, kelp, spirulina, or chlorella.
If exposed to these high doses of iodine, it may be helpful to take a selenium supplement (up to 600 mcg per day) to negate the negative effects of the iodine excess.
What About Cases of Excess Iodine? Can Thyroid Function Normalize with a Low Iodine Diet?
As mentioned above, iodine deficiency is rare, and most people with Hashimoto’s and issues related to iodine, actually have excess levels of this nutrient. As such, let’s discuss how to address excess iodine levels.
Excess iodine can definitely be a trigger for Hashimoto’s and hypothyroidism for some individuals. I have had a few clients where in looking at their health timelines, their Hashimoto’s was preceded by a high intake of iodine; for others, a high intake of iodine worsened their Hashimoto’s.
For one of my clients with new onset Hashimoto’s after a period of eating a lot of seaweed for general health benefits, a short-term low iodine diet was all that was needed to normalize her thyroid function and thyroid antibodies.
According to Dr. Alan Christianson, consuming the wrong amount of iodine is a primary driver of all types of thyroid disease and many thyroid growth abnormalities. Too little iodine, too much iodine, or fluctuations in iodine intake, can all disrupt thyroid function.
From test tube studies, we have seen that too much iodine slows down the thyroid and causes the immune system to attack it. From epidemiologic (population group) studies, we know that populations that increase their iodine intake, go on to develop more thyroid disease as a group. Meanwhile, interventional trials (clinical studies) have shown that people who are given more iodine develop thyroid conditions, while reducing people’s iodine intake can often reverse thyroid disease.
One recent clinical study showed that high doses of iodine supplementation slowed thyroid function, but even small doses were harmful. In the study, 256 adults who were free of thyroid disease, were given either a dose of supplemental iodine or a placebo. The iodine doses ranged from as little as 100 mcg to as high as 2000 mcg. No changes were observed in the placebo group, but many of those taking 100 mcg of iodine saw thyroid disease develop within four weeks. Of those taking 2000 mcg of iodine, 31 percent developed thyroid disease.
In another study to evaluate the tolerability of iodine supplementation, a group of adults were given 200 mcg of iodine or a placebo, for 12 months. Over 10 percent of those given iodine developed thyroid disease, but no one taking the placebo did. When the iodine was discontinued, the thyroid function of those who had been taking iodine normalized.
This is exciting news, indicating that we can use the restriction of iodine to reverse thyroid disease!
In another exciting human study, people with hypothyroidism caused by Hashimoto’s, were assigned to eat either a low-iodine diet or their normal diet. (These patients were significantly hypothyroid, as normal TSH scores were defined in this study as 0.41 to 4.43 IU/mL, and these patients’ TSH scores started as a group average of 14.28 IU/mL.)
Within three months of only regulating their iodine intake, nearly all their scores were normal, with the average coming down to 3.18 IU/mL! Those whose TSH levels did not return to normal, nevertheless saw improvements, typically by 50 percent or more. For example, one such patient started with a TSH score of 200 IU/mL, which was reduced to 100 IU/mL on the low iodine diet — still far from ideal, but significant progress in a short period of time!
Of those on the low-iodine diet, 78.3 percent were considered to no longer have Hashimoto’s, within three months. Meanwhile, the study’s control group didn’t see any change in TSH levels.
One interesting point from this study was that the baseline iodine intake was not different between the responders and the non-responders. Meaning, iodine regulation helped those who had average intakes of iodine, just as much as it helped those with high intake. This is one of the reasons Dr. Christianson notes that he doesn’t ask people to test their iodine levels before starting The Thyroid Reset Diet. If someone does not respond, iodine tests can then be helpful to make sure there was no hidden source of iodine that was holding back improvement.
Dr. Christianson’s new book makes the balanced iodine approach very straight-forward and easy to implement. While the iodine approach may not be the answer for every person with Hashimoto’s, it may be a part of the solution for some of us.
Furthermore, I want to clarify that Dr. Christianson’s approach focuses primarily on addressing TSH levels, but it does not focus on other triggers and root causes, nor does it focus on lowering Hashimoto’s antibodies. In my research into Hashimoto’s over the last decade, I’ve noticed that normalizing thyroid function and normalizing thyroid antibodies each require their own interventions, and I believe that both are important. Elevated thyroid antibodies have been linked to numerous issues including, but not limited to, recurrent miscarriage, anxiety, and even brain inflammation.
How to Restrict Iodine Intake
For some people with elevated thyroid antibodies and/or an elevated TSH, a temporary restriction of iodine may be beneficial.
As mentioned above, in some cases, following a low iodine diet and lifestyle has been helpful in reducing the autoimmune attack on the thyroid gland and in normalizing thyroid function, in people with iodine-induced Hashimoto’s. In this case, a person would temporarily restrict iodine to <100 mcg per day for a period of 1-3 months.
The thyroid gland needs approximately 52 mcg per day of iodine. This is usually present in thyroid hormones, which contain a small amount of iodine in them. (For example, 100 mcg of T4 medications will contain 52 mcg of iodine.)
Dr. Christianson has designed a diet plan that aims to provide between 57-107 mcg of iodine per day, and reports that within the first 28 days, people should start seeing an improvement in thyroid function, and most see the full benefits in three to six months.
According to Dr. Christianson, in order to reverse thyroid disease, in those who already have it, the optimal amount of iodine is 50-99 mcg per day. Dr. Christianson reports that with this approach, many individuals may be able to lower their dose of thyroid medications, while some may even be able to wean off thyroid medication completely (under the supervision of their physicians).
It’s important to note that many hidden sources of iodine can add up to create an iodine excess, and you will want to look for iodine exposure beyond supplements.
Common sources of iodine include:
- High iodine foods (kelp, dulse, spirulina, chlorella, seaweed, fish, shellfish, egg yolks, dairy products, and commercial baked goods)
- Iodized table salt
- Iodine in skin care products such as shampoo, conditioner, sunscreen, facial moisturizer, and skin creams (watch out for ammonium iodide, potassium iodide, sodium iodide, iodoform, PVP-iodine, hydroxypropyl bistrimonium diiodide, TEA-hydroiodide, ethiodized oil, iodopropynyl butylcarbamate, and the following seaweed extracts: Fucus vesiculosus extract, Laminaria digitata extract, kelp extract)
- Supplements, including multivitamins, prenatal vitamins and some supplements marketed as “thyroid support” blends
- Medications (many oral, topical, and injectable drugs contain iodine)
- Oral medications: amiodarone, benziodarone, calcium iodide, diiodohydroxyquin (Yodoxin), R-Gen, echothiophate iodide ophthalmic solution (phosphine), hydriodic acid syrup, iIodochlorhydroxyquin (Entro-Vioform), iodinated glycerol (Iophen), idoxuridine ophthalmic solution (Herplex), isopropamide iodide (Darbid), potassium iodine (KI), Mudrane, Lugol’s Solution, niacinamide hydroiodide, Ponaris nasal emollient, supersaturated potassium iodide (SSKI)
- Injectable solutions: sodium iodide
- Topical antiseptics: diiodohydroxyquin cream (Vytone), iodine tincture iodochlorhydroxyquin cream (Vioform), Cellasene, iodoform gauze (NuGauze), povidone-iodine (Betadine)
- Radiology contrast agents: diatrizoate meglumine sodium (Renografin), iodized oil, iopanoic acid (Telepaque), ipodate (Oragrafin), iothalamate (Angio-Conray), metrizamide (Omnipaque), ethiodized oil (Lipiodol)
To help determine your current level of iodine intake, you will want to check the labels on personal care products, medications, and supplements, as well as calculate your daily dietary consumption based on foods you commonly eat. The table below lists the iodine content of some common foods:
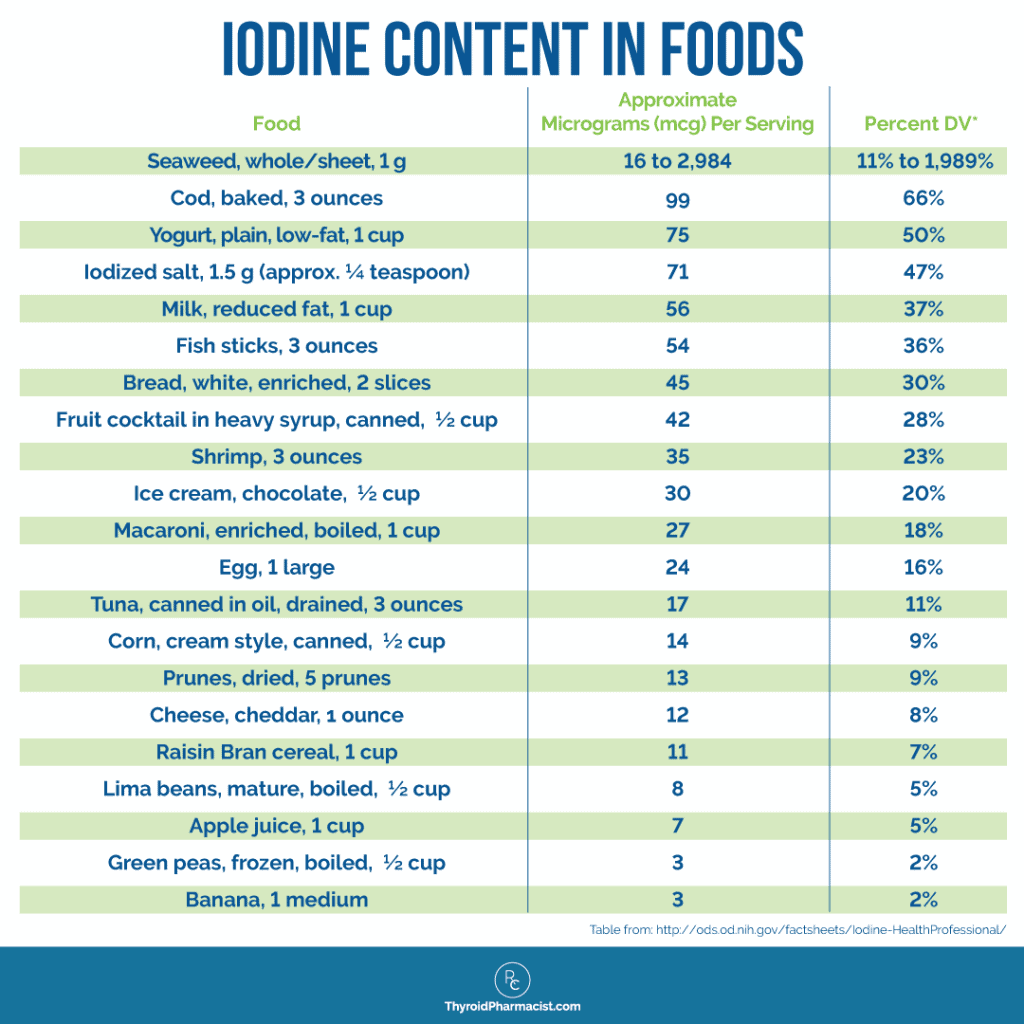
Here’s an example of how to do the math to determine your iodine intake, starting with a breakfast that is considered “healthy” by S.A.D. (Standard American Diet) standards.
Breakfast
1 cup milk = 56 mcg of iodine
Raisin Bran cereal = 11 mcg of iodine
Banana = 3 mcg of iodine
Lunch
Yogurt = 75 mcg of iodine
Bread (2 pieces) = 90 mcg of iodine
Cheddar cheese = 12 mcg of iodine
Canned tuna = 17 mcg of iodine
That’s 264 mcg of iodine before dinner…
What if you took a multivitamin?
A Centrum® multivitamin contains 150 mcg of iodine. Now you are up to 414 mcg.
What about those of us who add iodized table salt to our food?
Every ¼ teaspoon of iodized salt adds 71 mcg… so now we are at a total of 485 mcg of iodine.
What about going out for sushi?
Combining seaweed and fish can easily bring your iodine intake to 1,000 mcg, if not more.
And how about the personal care products that contain iodine that is absorbed through your skin?
Your facial moisturizer may contain as much as 54,000 mcg of iodine… 2,430 mcg (4.5 percent) of which may be absorbed into your system!
What if you wanted ice cream for dessert?
You get the picture. The Standard American Diet exceeds the threshold of safe iodine consumption for those with autoimmune thyroid conditions. By calculating the iodine content in the foods, supplements, medications, and personal care items that you consume and use in a day, you’ll gain a clearer understanding of your average daily intake and can decide if reducing iodine containing products would be beneficial for you.
Real World Experience with Iodine
Out of my Root Cause Readers that were surveyed back in 2015, 356 tried high dose iodine. Out of that group, 25 percent said that high dose iodine made them feel better, 28 percent said that it made them feel worse, and 46 percent saw no difference in how they felt… although this doesn’t mean that their thyroid markers weren’t affected.
The takeaway from this survey is that more people felt worse on high dose iodine than felt better. On the other hand, iodine restriction made 31.7 percent feel better and 7 percent feel worse.
In contrast, taking a selenium supplement helped 63 percent feel better, 34 percent saw no difference, while 3.5 percent felt worse. Going gluten free helped 88 percent of people feel better, 11.16 percent saw no difference, and 0.73 percent felt worse. (Check out my articles on the benefits of supplementing with selenium and going gluten free to learn more.)
As you can see, there are many safer and much more effective interventions than iodine supplementation in Hashimoto’s, which is why I have chosen to focus on the interventions that are helpful to most and least likely to result in harm. While some doctors are devout advocates of prescribing iodine to heal the thyroid, I treat iodine like a narrow therapeutic drug and recommend caution when using it in Hashimoto’s, as everyone is unique and may respond to iodine therapy differently.
A Client’s Experience with Iodine
To illustrate the need for caution when supplementing with iodine, and how addressing Hashimoto’s requires a root cause approach, I’d like to share with you a story from my client files.
Jenny is an athletic dog lover who worked part time at her family restaurant. She had been previously diagnosed with Hashimoto’s (TPO antibodies in the 800 IU/mL range) and subclinical hypothyroidism, with a slightly elevated TSH, and normal T4 and T3.
At her initial diagnosis, Jenny had many symptoms of hypothyroidism, including fatigue, excess weight gain, and hair loss.
She wanted to fix the condition in a natural way and found information about iodine being an effective treatment for hypothyroidism. She worked with an iodine advocate who did not have a medical background, but had seen improvement in her own thyroid function with iodine, although she herself had never been diagnosed with a thyroid condition. This advocate recommended that she start taking high doses of iodine to heal her thyroid.
After starting the high dose iodine, Jenny began to have more energy, but soon that energy became an anxious, irritable energy. She then became very tired, to the point where she stayed in bed for days.
Jenny’s husband became concerned about her health and urged her to stop working with the iodine advocate. She went to see an endocrinologist, who ran a thyroid antibody test — her thyroid antibodies had more than doubled to the 1800 IU/mL range, her TSH climbed to 100 IU/mL, and her T4 levels were undetectable! Her physician advised her to stop the high dose iodine immediately and prescribed synthetic thyroid medications.
After that point, Jenny came across my book and reached out to me for a case review. Her husband felt more comfortable with her consulting with me since I had a background in pharmacy and had also been diagnosed with Hashimoto’s.
I recommended that she restrict her intake of iodine from iodized salt, supplements, and food to less than 150 mcg of iodine per day for three months, and that she start the Paleo diet.
I also recommended that she start a selenium supplement, take probiotics, test her adrenals through a saliva test, and test for gut infections through a stool test. In addition, I advised her to speak to her doctor about adjusting her medications.
Within a few weeks of the new protocol, Jenny was starting to feel better. The anxiety and irritability improved, and her fatigue began to lift.
Once we received her test results back, we found that Jenny had stage 3 adrenal fatigue, and two gut infections: H. pylori and Blastocystis hominis.
We talked about the importance of self-care. I recommended that she reduce her responsibility levels, and that she start massage therapy treatments and a relaxing routine. We supported her adrenals through the use of adrenal adaptogens and a supplement called Moducare.
We also worked with her physician and treated her gut infections, starting with H. pylori, and then Blastocystis hominis. We then initiated a gut repair protocol.
Jenny reported that her gut symptoms, hair loss, and energy levels began to improve within two weeks on the H. pylori protocol. After she finished her protocol, her weight normalized, she reported that she had a “ton of energy,” and her hair began to grow back. Her thyroid medications had to be lowered slightly as she began to absorb them better once the infections were gone.
The last time we spoke was six months after her gut infection treatments, and she reported feeling happy, having great hair and great energy levels, and being back to being active and working out 4-5 days per week. Her TPO levels fell to under 100 IU/mL, and I anticipate that they will continue to improve as time goes on (TPO levels may take 3 to 18 months to decrease following H. pylori eradication).
Jenny’s story is a testament to how taking a root cause approach, which may include addressing iodine excess, can help improve thyroid health and reduce many of the symptoms of Hashimoto’s.
Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire. Adding iodine to the mix before putting out the fire and fixing the engine, may result in further damage to the thyroid. I have spent years researching this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first, and then add the fuel once we know that the engine is no longer on fire. 🙂
For more information on how to resolve your own triggers, I encourage you to check out my book Hashimoto’s Protocol.
The Bottom Line
Hashimoto’s is not a single nutrient condition, but rather the result of several underlying root causes. While iodine deficiency can cause thyroid issues in some people, most people get enough (or too much) iodine from their diet, and most people with Hashimoto’s are not iodine deficient.
Taking a high dose of iodine can exacerbate Hashimoto’s and accelerate thyroid cell destruction. The American Thyroid Association cautions against using doses of more than 500 mcg per day in the general public and noted that doses above 1100 mcg may cause thyroid dysfunction. These warnings are for the general population, but studies have found that people with Hashimoto’s may be sensitive to even smaller doses.
Excess iodine has been recognized as an environmental trigger for Hashimoto’s, and as such, I do not routinely recommend the use of iodine supplements outside of those found in multivitamins and prenatal vitamins (most contain between 150 mcg-220 mcg).
While I won’t deny that some people have certainly been helped by high doses of iodine, I feel that the risks outweigh the benefits for people with Hashimoto’s, and I caution people against the use of high dose iodine. In those who have been exposed to high doses, I may even recommend a short-term iodine restriction and selenium supplement to help reduce the hydrogen peroxide buildup and subsequent inflammation that may occur.
For more information about the low iodine approach to healing Hashimoto’s, please see my first book Hashimoto’s: The Root Cause and Dr. Christianson’s new book The Thyroid Reset Diet.
I do want to remind you that each one of us is a unique individual and has different nutrient deficiencies and needs. It is important to speak with a trusted medical professional to determine if supplementing with iodine or removing excess iodine from your lifestyle will be of benefit to you and your health journey.
To learn more about the nutrients that are helpful in Hashimoto’s, I encourage you to read my article on The 7 most common nutrient deficiencies in Hashimoto’s. In it, you’ll find useful information on the nutrients that are often a root cause for people with Hashimoto’s, and that I routinely recommend as part of a healing protocol.
I hope this information helps you on your journey!
What type of experience have you had with iodine?
P.S. Be sure to sign up to my weekly newsletter to get a free book chapter, recipes, Thyroid Diet Starter Guide, and notifications about upcoming events and my latest research.
For future updates, be sure to follow us on Facebook and Instagram too!
References
- Iodine deficiency. World Health Organization. https://www.who.int/data/nutrition/nlis/info/iodine-deficiency. Accessed December 2, 2021.
- Contempre B, Dumont J, Ngo B, et al. Effect of selenium supplementation in hypothyroid subjects of an iodine and selenium deficient area: the possible danger of indiscriminate supplementation of iodine-deficient subjects with selenium. J Clin Endocrinol Metab. 1991;73(1):213-215. doi:10.1210/jcem-73-1-213.
- Joung J, Cho Y, Park S, et al. Effect of iodine restriction on thyroid function in subclinical hypothyroid patients in an iodine-replete area: a long period observation in a large-scale cohort. Thyroid. 2014;24(9):1361-1368. doi:10.1089/thy.2014.0046.
- Rink T, Schroth H, Holle L, Garth H. Effect of iodine and thyroid hormones in the induction and therapy of Hashimoto’s thyroiditis. Nuklearmedizin. 2016;1999(38(5):144-9.
- Xu J, Liu X, Yang X, et al. Supplemental selenium alleviates the toxic effects of excessive iodine on thyroid. Biol Trace Elem Res. 2011 Jun;141(1-3):110-8. doi: 10.1007/s12011-010-8728-8.
- Zhao H, Tian Y, Liu Z, et al. Correlation between iodine intake and thyroid disorders: a cross-sectional study from the south of China. Biol Trace Elem Res. 2014;162(1-3):87-94. doi:10.1007/s12011-014-0102-9.
- Urinary Iodine Concentrations for Determining Iodine Status in Populations. World Health Organization. 2013.
- Chung JH. Low Iodine Diet for Preparation for Radioactive Iodine Therapy in Differentiated Thyroid Carcinoma in Korea. J Clin Endocrinol Metab. 2013;28(3):157-163. doi:10.3803/EnM.2013.28.3.157
- Park JT, Hennessey J V. Two-Week Low Iodine Diet is Necessary for Adequate Outpatient Preparation for Radioiodine rhTSH Scanning in Patients Taking Levothyroxine. Thyroid. 2004;14(1):57-63. doi:10.1089/105072504322783858
- Bhagwat S, Haytowitz DB, Holden JM. USDA Database for the Isoflavone: Content of Select Foods – Release 2.0. Beltsville, MD: USDA, 2008.
- Yoon SJ, Choi SR, Kim DM, et al. The Effect of Iodine Restriction on Thyroid Function in Patients with Hypothyroidism Due to Hashimoto’s Thyroiditis. Yonsei Med J. 2003;44(2):44-227
- Christianson, A. The Thyroid Reset Diet. Rodale Books; 2021.
- Sang Z, Wang PP, Yao Z, et al. Exploration of the Safe Upper Level of Iodine Intake in Euthyroid Chinese Adults: A Randomized Double-Blind Trial. Am J Clin Nutr. 2012;95(2):367-373. doi:10.3945/ajcn.111.028001.
- Kahaly G, Dienes HP, Beyer J, Hommel G. Randomized, Double Blind, Placebo-Controlled Trial of Low Dose Iodide in Endemic Goiter. J Clin Endocrinol Metab. 1997;82(12):4049-4053. doi:10.1210/jcem.82.12.4416.
- Kasagi K, Iwata M, Misaki T, Konishi J. Effect of Iodine Restriction on Thyroid Function in Patients with Primary Hypothyroidism. Thyroid. 2003;13(6):561-567. doi:10.1089/105072503322238827.
- Dellabella, H. Thyroid Peroxidase Antibody Positivity Linked to Reduced Live Birth Rate in Recurrent Pregnancy Loss. Endocrinology Advisor. https://www.endocrinologyadvisor.com/home/topics/thyroid/thyroid-peroxidase-antibody-positivity-linked-to-reduced-live-birth-rate-in-recurrent-pregnancy-loss/. Published October 17, 2010. Accessed January 7, 2021.
- Gutch M, Bhattacharjee A, Kumar S, Pushkar D. Hashimoto’s Encephalitis: Rare Manifestation of Hypothyroidism. Int J Appl Basic Med Res. 2017;7(3):193-195. doi:10.4103/ijabmr.IJABMR_256_16.
- Carta MG, Loviselli A, Hardoy MC, et al. The link between thyroid autoimmunity (antithyroid peroxidase autoantibodies) with anxiety and mood disorders in the community: a field of interest for public health in the future. BMC Psychiatry. 2004;4:25. Published 2004 Aug 18. doi:10.1186/1471-244X-4-25.


 Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
So is the advice the same then, for Graves disease? I find so much conflicting information about iodine for hypER, its not clear if its a positive or a negative.
Basically, avoid excess iodine?
Thanks for your time.
Anushka – thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions.
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
What is the Hashimotos Protocol?
Natalie – thank you for following this page. My new book Hashimoto’s Protocol is a step by step guide to the interventions that helped 80% of the people 80% of the time. I hope you check it out.
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
I am confused by your website discussion of Iodine intake for Hoshimoto’s patients. Can you summarize in 2 sentences indicating yes take iodine, or no avoid it, or other ? The studies referenced in totality point to…just go figure it out for yourself.
Bart
Bart – thank you for following. Small doses are generally safe (amount in prenatal vitamins and multivitamins), but above 400 mcg can be inflammatory.
You mentioned that the rise in iodized salt and iodine in general correlates with the rise in thyroid disease. What about the fact that bromide consumption and use, along with fluoride, also significantly increased at that time? Bromide occupies iodine receptors and is a thyroid toxin. In the absence of iodine, it is readily absorbed by the thyroid.
Lynda – thank you so much for sharing! Those are both toxins as well. Here is an article you might find interesting:
https://thyroidpharmacist.com/articles/the-many-faces-of-hashimotos/
I am so overwhelmed and confused! My 19 year old daughter, who has Hashimoto’s, Type 1 Diabetes, and Lupus, has been working with a FMD for almost 2 years now. She eats a paleo diet, for the most part and takes a ton of supplements! She is on 65mg NatureThroid and as of last month, her FMD also added something called Thyroid Px by Restorative Formulations to her arsenal. I just looked at the iodine dosage and it is 12mg!!! Thank goodness she has only been taking half that, but that’s still 6mg or 6000mcg!!!
I bought you Hashimoto’s Protocol book, but have yet had a chance to read it. My life has been consumed with all these docuseries (The Thyroid Secret, The Betrayal, The Truth about Vaccines, The Truth about Cancer, some food Summit – it’s all too much and I feel soooooo defeated and have no idea where to begin)!
My daughter’s case is extremely complex and I feel there is never going to be a way to find the root cause of her overall autoimmunity. At some point, her mental health (although compromised) has to take the forefront so that she can just live life like a somewhat normal college student.
Mandy – thank you for following this page. My heart goes out to you and your daughter. <3
A couple of years after my diagnosis, I found Hashimoto’s 411, a closed Facebook group run by Alice Berry McDonnell. This group is amazing! It is comprised of an army of highly motivated, smart, supportive women and men (now 45,000+ strong), and each of them sharing ideas of what worked for them, things they were planning to try, and offering support to one another. The comfort I received from knowing that there were others going through the same challenges as I, was enormous.
https://www.facebook.com/groups/hashimotos411/
Ask questions. Post your thoughts. Scan the files. It is an absolutely amazing resource. Best of all it’s kept private from spammers.
Thanks for all the great info! Your article sounds like it is specific to hashimotos. Would you say the same thing to someone who does not knowingly have hashimotos but whose thyroid numbers are off and who has been tested to be very low in iodine using a urine pre and post loading type test. Would you still caution against it when a good lab test shows you are low and your practitioner wants you to take a dose higher than you recommend? My cellular selenium levels are fine as well plus I take it it supplements.
Donna – thank you for following this page.
Did you know that if you live in the United States, Australia, Europe and most developed countries that add iodine to the salt supply and take thyroid medications, there’s a higher probability that you do have Hashimoto’s?
Depending on the source, estimates are that between 90-95% of those with hypothyroidism have Hashimoto’s.
But most doctors will never tell people that they have Hashimoto’s, or that their own immune system is attacking their thyroid. People are told that their “thyroid is sluggish”, and that these things happen with age and “Just take this pill, you’ll be fine.” I hope you check out these articles that I wrote.
ARE YOU DOING EVERYTHING FOR YOUR THYROID BUT NOT YET WELL?
https://thyroidpharmacist.com/articles/are-you-doing-everything-for-your-thyroid-but-not-yet-well/
DO YOU HAVE HYPOTHYROIDISM OR HASHIMOTO’S OR BOTH?
https://thyroidpharmacist.com/articles/do-you-have-hypothyroidism-or-hashimotos-or-both/
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well.
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
Thank you so much for your reply. I read the articles – thank you for supplying the links.
I’ve done most of the tests you mention. My results:
Thyroglobulin antibodies <1
Thyroid Peroxidase Antibodies <1
TSH 31.86 (very high)
Free T4 0.7 (listed as low)
Free T3 2.5 (in what they call normal range)
Also
Reverse T3 11 (in what they call normal range)
T3 uptake 27 (in what they call normal range)
T4 Total 4.6 (in what they call normal range)
As for my iodine test, doing a pre and post loading urine halides test from Doctor's Data, the %Excretion/24 hours was 30%, and I was told I should have it more like 90%, and that it means I'm low in iodine.
I have used sea salt as opposed to iodized salt for awhile, so that might be why I could be low. My doctor has me taking about 37 mg/day of iodine, which is 7.5mg as potassium iodide and 5mg molecular iodine per capsule. I have fairly good energy, and some of my symptoms like hair loss and being cold all the time have improved. It seems to me like I don't have Hashimotos, but taking that large of a dose of iodine does make me a little nervous when I read things that you and others write, so I wanted to get your opinion. I am going to a functional medicine practitioner and not just an allopathic doc so I believe he knows his stuff, but so many practitioners seem to have different ideas on certain particulars, so I thought it would be nice to hear from someone who specializes in thyroid.
Obviously I'm not your patient, but in your opinion should I question such a high dose of iodine, or under my circumstances might it be okay? If you don't feel you can comment, or don't have time, that's okay. But I appreciate your previous reply.
Donna – I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in both animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Thank you, for explination of the iodine’s impact on thyroid gland. I want to understand things thorougly, before I believe, or take action. Have heard that before,
yes, but without accurate knowledge and case studies, haven’t taken action this far, but now I’ll try restriction of my iodine input. Didn’t know that Spirulina and Chlorella have Iodine, using Kelp daily. Leaving now only 1 Kelp left and we’ll see- My case is a bit similar to the casestudy you told (Jenny? or sg) Anxiousness, hair loss, fatigue, dry skin. Not on medications, TSH 3.5, TPO 35, adrenal state 3.I bought your book on Amazon, now some difficulties in the delivery, hope I’ll get it sooooon. Thank you for your informative articles and HAPPY HOLIDAYS to you, you certainly have earned it. With best wishes Maija
Maija – thank you for following this page and for your support. <3 I'm sorry to hear that you are experiencing some delivery issues with your book order. :(
Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto's is a different mechanism. It's like pouring gas into an engine that's on fire... that's essentially what's happening in Hashi's, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let's fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
I read your article.
My comment is about the exposure to bromine and fluoride that rarely gets mentioned when talking about iodine. Nor have I seen those levels checked regularly.
They are a 3-legged stool and all need to be reviewed for a complete picture.
Mary – thank you for following this page.
I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Wow. Thank you for this info. I’m currently on 2 Xenostat (634 mcg) plus 3 prenatals (i’m not pregnant, just taking that supplement) and they contain 450 mcg MORE! i’ve had a friend who always warned me against taking iodine, but my functional med/endo said i needed it. i did feel better on it and have at times been up to 4 a day. Wow. He says my labs indicate i need more, but i’m thinking that i need to assimilate better what i already naturally get in foods and supplements and fix the root problem. i’m SO lost. where do i start. if i stop the idodine, i feel i’ll crash, but you’re saying that in taking it, i’m killing my thyroid!
Vit. D and iodine have been my “go tos” for feeling my best… guess it’s time to take a new route.
my symptoms are brain fog and irritability (and i have hashimotos). i don’t struggle with weight gain (and i’ve recently stopped raw milk and my bloating has gone down), i seem to do fine with homemade/raw yogurt). i do get tired at times, but it’s not bad AND i crave my “homemade/gf” desserts… HELP!
how dare i write you while you’re heading to vacation! thanks for your time. should i just look for a new doc? my idodine labs show i’m in good range right now. should i just get off the two Xenostats?
One last note, i can’t help but ask you to think beyond the common “evoluntionary” thinking that is so imposed on us, and in all your research see if you don’t actually see a Creator behind all the beauty, wonder, and irreducible complexities of life as we know it. God is good and i so hope you’ll know him as Creator and Savior.
I MUCH appreciate all you’ve done. i look forward to reading your book, but if you have any advice right quick, i’ll take it! thanks, elizabeth
Elizabeth – thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions.
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Your use of the wording high dose iodine is misleading. I have followed dr brownstein’s protocol for 18months. On the Facebook forum anything below 50mg is generally considered low. The low and slow approach is not encouraged, especially for those with Hashimoto’s. With many reporting they felt terrible on anything below 100mg. This was certainly the case for me, dr brownstein’s book iodine covers this exact point that hydrogen peroxide is created when the thyroid hormone is processed and how we need more iodine to have enough to produce an antioxidant effect to counter act this. He also gives references of studies showing that although antibodies can increase initially this only transitory and that they do soon reduce again. You seem not to have read his work or know what is regarded as low or high dose.
I have almost completed cured my fibrocystic breast with iodine not a result to be sniffed at considering the increased cancer risk of fibrocystic breasts. You have also not considered iodine anti cancerous effect.
I can’t follow your logic that the body would use destroying tissue as a way manage thyroid hormone levels. A more plausible theory is that autoimmunity is caused by an infective agent going deep into tissues and organs. What we see as our body attacking itself could merely be the collateral damage as the body tries to rid itself of the infection. Yes reducing iodine would weaken the body’s ability to attack the infection and reduce the antibodies but you are then not really treating the root cause of the Hashimoto’s, the infection. Leaving it dormant, merely in remission. The issues then is as we age and pick up more and more infections and environmental stressors they all add up until at some later date we reach a tipping point.
I can understand you counselling caution with iodine but please as so many people now follow your advice please become more educated on the pro iodine movement. It’s evident if you call 1mg a high dose when people are successful taking 100mg, 100 times more that you consider high, then you are not up to date. I loved your book and recommend it to others but as someone who has done all the diet and lifestyle modification and still it was not enough I can not condone your outdated stance on iodine.
Rachel – thank you for following this page and for sharing.
I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Thanks Rachel, I found your comment very helpful as I too have found that Lugol’s Iodine (working up to a high dose) helped me a lot and also decreased my fibrocystic breast tissue.
But I also had trouble with the high doses occasionally tanking my thyroid, but usually only for a few hours, and I have noticed some really interesting correlations which tie in with your theory about an infection or something deep in the thyroid that the Iodine helps rectify.
In my case- mould seemed to be really affecting me. When I was clearing my father’s mouldy house I had extremely bad auto-immune inflammation and pain (reactions to food). These reactions vanished as soon as I left the mouldy environment, and even once helped diagnose a hidden mould problem that I didn’t previously know about.
Anyway I noticed that using a Steam room to detox the mould, reduced my inflammatory symptoms overall, but straight afterwards (presumably when the toxins were still being eliminated from my system), that could also tank my thyroid.
Although the more steam detoxing I do- the more Iodine I could tolerate (and the more I seem to need). So at least in my case, it seems to be a delicate balancing act between all these different factors and getting the dosage right.
When I came off Iodine entirely my breast lumps came back, my hair worsened and then eventually when I tried Iodine again, I really felt the benefit. But I also can have too much!!
But if I detox in the steam room, I respond much better. It’s confusing. I wouldn’t want to stop Iodine entirely as I feel the benefit to my breast tissue is a significant aspect! I do not think my breasts are meant to be so lumpy, they were like concrete at one point.
I’m glad I found this article and website too as Dr Wentz seems very knowledgeable and it’s helping me get a grasp on what might be going on.
I really hope as more research occurs and awareness increases, the conversation around this gets clearer.
Rachel — thank you for your comments. I agree with you in that Dr. Wentz, for whom I have great respect, needs to get up to speed on iodine. I, too, read Dr. Brownstein’s book, and just a few months after starting on lugol’s iodine, my thyroid shrank to almost normal size after having been enlarged for 40+ years.
Hi Marsha, Thank you for sharing your experience. As said to Rachel, I am very cautious recommending iodine in Hashimoto’s. While iodine fuels the thyroid and helps in deficiency, Hashimoto’s involves a different mechanism. Many with Hashimoto’s already have adequate or high iodine, which can trigger thyroid inflammation, so it’s important to avoid excess and work with a practitioner before starting supplementation. I’m happy to hear you are seeing great results.
Enjoyed this iodine information. I am an OLD Hashimoto’s patient–not diagnosed until the late fall at 66! I guestimate after all I have read that I have likely had this for 20 years or more–but feel that I am doing everything I can to improve and continue to go through horrible days when I am not able to stay up for more than a few hours at a time. I was always active–working full time and a runner–now I am struggling. Taking NatureThroid and compounded liothyronine plus L glutamine powder, Lysine, selenium, probiotics, digestive enzymes and bone broth. What in the world else can I do? I am gluten free– 3 years now. Thank you.
Mary – thank you for following this page. I can understand your frustration. 🙁
A couple of years after my diagnosis, I found Hashimoto’s 411, a closed Facebook group run by Alice Berry McDonnell. This group is amazing! It is comprised of an army of highly motivated, smart, supportive women and men (now 45,000+ strong), and each of them sharing ideas of what worked for them, things they were planning to try, and offering support to one another. The comfort I received from knowing that there were others going through the same challenges as I, was enormous.
https://www.facebook.com/groups/hashimotos411/
Ask questions. Post your thoughts. Scan the files. It is an absolutely amazing resource. Best of all it’s kept private from spammers.
Dear Dr. Isabella, I enjoy reading your posts and I have your Hashimoto’s root cause book. I have also learned a lot from your free webinar.I don’t usually respond but had to today to say first of all I hope you really enjoy your vacation in Italy with your husband.It is hard to hear that you receive hate mail. Please know that there are many of us who greatly appreciate your help and benefit from it and may not send emails back to you. In the email above I can hear your frustration and hurt. keep up the awesome work and take good care in protecting yourself from negativity. Keep your vibration high. LOVE rules!!! Many blessings to you.
Gale – Thank you for following this page. Your kind words and support warmed my heart, and they were very much appreciated! <3
Then I wish to add my love and support too… and to thank you most sincerely for your guidance and for sharing all that you have learnt. Especially when it has been difficult and challenging, you have not given up.
You are an inspiration!
Thank you xxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxx
Mary – thank you for following this page and for your heartwarming words of support. <3 hugs <3
I have tried living with and without iodine in the context of my Hashi’s and a have found living with it to be much better. Everything is better with iodine, as long as there is enough selenium taken with it, in my experience. My energy is better, my allergies are better, my body’s tolerance for food is better and my body seems to heal better with it. The body needs iodine in order to function properly and using antibodies as a sole barometer for whether or not you should be using it, is a mistake in my opinion. I will be continuing to use it as I have found it to be highly beneficial.
Vanessa – thank you for following this page, and for sharing.
I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Dear Dr. Wentz
Thank you so much for this article. I have Hypothyroid, probably Hashis, and I use iodized sea salt when cooking. I guess it would be better for me to use the regular sea salt. Is it ok for other family members to use the same plain sea salt? I do not eat any of the other things mentioned by you which contain high amounts of iodine.
Also, I would like to ask you which oil can I use for cooking. I am allergic to coconut oil (which I leant the hard way after using coconut oil for cooking and consuming extra virgin coconut oil daily). Presently I am using olive oil (some brands don’t agree with me). Is it ok to cook with olive oil on high heat? What is the alternative oil that can be used for cooking for people with Hashimotos?
SS – thank you so much for following this page.
Did you know that if you live in the United States, Australia, Europe and most developed countries that add iodine to the salt supply and take thyroid medications, there’s a higher probability that you do have Hashimoto’s?
Depending on the source, estimates are that between 90-95% of those with hypothyroidism have Hashimoto’s.
But most doctors will never tell people that they have Hashimoto’s, or that their own immune system is attacking their thyroid. People are told that their “thyroid is sluggish”, and that these things happen with age and “Just take this pill, you’ll be fine.” I hope you check out my books:
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hi Izabella
I have found exactly this – that iodine causes inflammation in my whole body, including in my gut, my joints, my muscles and that I want to sleep all the time and I also now recognise that my antibodies went up (not sure of score though) as well as my TSH to over 200 and my T4 was 0.6! That was 3 years ago! I felt dreadful! Much the same story as Jenny in your blog. I’m happy that You have now confirmed my thoughts! Thank you! I’ve just received Hashimotos Protocol a couple of days ago so I’m avidly reading! I’m seeing the Endocrinologist tomorrow and I’m hoping to persuade her to test my gut for bacteria so I can rebalance my leaky gut for starters, and to test for all the thyroid markers. They usually only want to do TSH and T4! I live in the UK and their Protocol is STRICT and NARROW!!! Thanks for your wisdom and for sharing your knowledge for free…….best wishes
Lindsey
Lindsey – thank you for following this page, and you are most welcome. 🙂
These are the recommended labs from my book, page 32.
RECOMMENDED THYROID FUNCTION TESTS
TSH
TPO Antibodies
Thyroglobulin Antibodies
Free T4
Free T3
Reverse T3 (Optional)
Have you read my book, Hashimoto’s The Root Cause? Here’s the link in case you’re interested.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20

HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications
My nutritionist suggested I get a bottle of liquid iodine (about $2 at the drugstore) and paint a one inch patch on my thigh or stomach. My body will know how much iodine I need to absorb, so when the color goes away it’s time to paint my skin again. The first day I had to reapply it four times. Each day after, it got less and less until now I only need to apply it twice a week. I’ve never had a bad reaction to it.
Shirley – thank you for following this page and for sharing.
Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Thank you! Your email about supplementing with high does iodine came to me just in the nick of time. I just purchased a bottle of iodine and was ready to start the protocol. I was diagnosed with Hashi 20 years ago but apparently it has been in remission for many years after treating my adrenals.
Alvera – thank you for following this page.
Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
So if my iodine is only 10 but I have hashimotos and graves antibodies, what would I do?
Kari – thank you for reaching out. ❤️ If your iodine levels are low, I would recommend taking a multivitamin such as Nutrient 950 by Pure Encapsulations. A dose of up to 250 mcg of iodine per day (these levels are found in most multivitamins and prenatal vitamins) has been found to be helpful and beneficial in people with Hashimoto’s; however, doses above 300 mcg can be potentially inflammatory.
Thank you for the great article about iodine and Hashimotos.
I have two questions: What if your thyroid was removed due to nodules and you were diagnosed with Hashimotos. Is it O.K. to take low dose iodine? What if your thyroid was removed and you don’t have Hashimotos, should you take low dose iodine?
Try – thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions.
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Hi Izabella,
Thank you for the links. Unfortunately there are not any functional medicine doctors located near me. The ones that are far away, but close enough to travel to, appear to be very expensive and their fees are not clearly listed. I’m not going to give up though, I’ll keep searching.
My daughter and I did purchase your hard cover book, the Hashimoto’s Protocol, and I am currently in the process of reading it. So I’m sure it will have some answers for me.
Thank you for everything you do. My daughter and I really appreciate it. You have helped us immensely with our Hashimoto’s thyroid diets and our overall health and well being. My daughter is now completely gluten free (including her new gluten free thyroid medication) and as a result, she is feeling a lot better and her endocrinologist had to significantly reduce the dosage of her thyroid medication.
Try – you may be interested in my 12 week online program called Hashimoto’s Self-Management Program that covers all of the strategies that I go through with my one-on-one clients, in a self-paced format, so that participants have access to all of the things I’ve learned about Hashimoto’s without having to schedule costly consults with me or another practitioner. In addition, any person that goes through the program will get access to a Quick search Q&A Database of 1000+ questions asked by past program participants, Root Cause Assessment based on 100’s of my clients’ root causes and triggers, 2-week Meal Plans, recipes, and shopping lists to get you started on the following diets: Paleo, Autoimmune Paleo, SIBO, Candida. Also, Discounts on lab tests, high-quality supplements, and consultations and much more to support you in your journey! There are a few requirements that you should pay attention to, such as my book which is a required read.
Hashimoto’s Self-Management Program
http://hackinghashimotos.com/
I had a blood test and was found to be iodine deficient. I have been taking aproduct containing 145mcg of iodine daily for 5 months. My antibodies have fallen and my energy levels are improved. So low dose can help for some people. I supplement with selenium too. Thank you for all the information you provide.
Margot
Margot – thank you for following this page and for sharing.
I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hi your articles are all very interesting and extremely helpful.
I am wondering what your opinion is on Hashimoto’s and high cholesterol.
I have recently started on Crestor for high cholesterol. I also have arthritis in the hip and knees. I also work a job where I am standing and moving quickly for most of the day. This has always created some issues but now the pain at the end of the day has become excruciating. I now believe the statin medication is exponentially effecting the condition.
I now plan to stop the medication knowing that my cholesterol now at 9 will increase. I am careful with my diet and exercise daily but this seems to have little effect.
Any comments will be greatly appreciated.
Thank you
Leonie
Leonie – Thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
My understanding is that the high-dose iodine advocates also recommend selenium, magnesium, and other supplementation to protect the thyroid. Their argument is that iodine increases bromide and fluoride excretion, and that the symptoms of iodism are actually bromism arising from iodine causing bromide excretion. What are your thoughts on bromism, and the relevance to Hashimoto’s Dr Wentz? Bromide compounds have increased significantly in our environment and food supply at the same time as iodine levels have decreased. Is there another safer way for Hashimoto’s to detoxify bromide compounds?
Susan – thank you for following this page and for your support. 🙂
Have you read my book, Hashimoto’s The Root Cause? Here’s the link in case you’re interested. I cover toxins starting on page 259.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Thank you so much for this article and all of your research into Hashimotos. I have been on Thyroid meds for 35 to 40 years now. First synthroid then levothyroxine and now Armour. Being treated for low thyroid but not Hashimotos. I feel much better on the Armour. I was only tested for antibodies recently, diagnosed with Hashimotos and changed to Armour. My question is this. Looking back I believe I had Hashimotos as a teen. My parents fed us a lot of sea food as kids. Lots of shell fish and fish of all kinds. Could this have affected my thyroid with an over dose of Iodine? Thanks for all you do. Sandy
Sandy – Thank you so much for your support. Did you know that reactive foods trigger an inflammatory response in the GI tract, leading to malabsorption of nutrients (gluten sensitivity, in particular, has been implicated in causing a Selenium deficiency, a well-known risk factor for Hashimoto’s), and can also produce intestinal permeability whenever they are eaten?
Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts, and pain by eliminating the foods they are sensitive to. Some will also see a significant in thyroid antibodies! An additional subset of people will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
there is no question that my thyroid began its hashimotos journey after working with a nutritional detox dr who kept recommendeing i up my kelp when i kept telling him something is not right!! buyers beware when we consult with drs who do not truly understand your specific bodies language. we are all so unique and what helps one may destroy another. thank you Dr. Wentz for all your research, guidance , love and support, you are literallysavi g lives and quality of life for so many of us!
Chava – Thank you so much for your support. I’m looking forward to hearing your progress on this page.:)
Hi Isabella,
I had hashimotos (treated with a synthetic hormone replacement) for 20 years, lupus (on prednisone and cytotoxic mess) for 18 years, osterarthritis and osteoporosis for 1 year before discovering that I was severely iodine deficient. I started a moderate dose (400mcg) of nascent iodine daily and by body naturally started a toxic halide detoxification. (We have fluoride and chlorine in our tap water here in Western Australia.) I then developed a candida overgrowth and went onto a low carb diet which later morphed into the AIP diet. Over time my dependence on thyroxine decreased. I slowly reduced my dosage and I eventually stopped taking it altogether. I have also weaned off all my lupus and high blood pressure meds and am now completely prescription medication free. My TSH, T4 and free t3 are in normal range and my antiTPO is much improved.
I do not give iodine all the credit for my return to good health, as the AIP diet and other supplements have helped too, including magnesium, D3, selenium and K2, along with lifestyle changes, but adding iodine 3 years ago was the catalyst for change, the start of my detoxification from fluoride and chlorine and the beginning of my return to health.
* whoops, a couple of typos, firstly I was on cytotoxic “meds” not “mess” but that seems appropriate too haha 🙂 and also “my” body naturally started a toxic halide detoxification, not “by” body.
Cheers. Helen 🙂
I have also since discovered that I carry one of the MTHFR gene mutations, which may account for why I was so toxic to begin with and unable to detoxify the fluoride and chlorine without the iodine displacing them from my iodine receptors.
Kind regards, and thanks for all you do
Helen
Helen – thank you for following this page and for your support. 🙂
This article may be of interest.
MTHFR
https://thyroidpharmacist.com/articles/mthfr-hashimotos-and-nutrients
Helen – thank you for sharing your experience. Good job!
I am really hoping to build a database of testimonials to submit to a medical journal. I would very much love if you submitted your story. You would be helping so many. Would you consider doing this?
http://www.thyroidpharmacist.com/testimonial
What about “painting” iodine on a different part of body each day? This was incredibly informative. Thank you!
Kat – thank you for following this page and for your support. 🙂
I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
For those struggling with low energy, weight gain, hair loss…after a full thyroid removal do you have any suggestions or resources? Since surgery in 1998 I don’t know I have ever felt 100% on thyroid medication.
Beth – thank you for following this page.
Fatigue was the most debilitating symptom I experienced with Hashimoto’s. It actually started 8 years before I was finally diagnosed in 2009 after I got Mono (Epstein-Barr Virus) in college. I needed to sleep for 12 hours each night to be able to function, and by “function” I mean after hitting the snooze button on my alarm clock for two hours (ask my poor husband), I would drag myself out of bed and then had to drink 4-6 cups of caffeine everyday to keep myself awake. I often had Red Bull and Pepsi for breakfast, and was the epitome of “wired but tired”. I hope my articles help you get started 🙂
OVERCOMING THYROID FATIGUE
https://thyroidpharmacist.com/articles/top-10-tips-for-overcoming-hashimotos-fatigue
THIAMINE AND THYROID FATIGUE
https://thyroidpharmacist.com/articles/thiamine-and-thyroid-fatigue
Thank you so much for all the great info you provide. I have hashimotos which I believe was activated by my natural health dr prescribing me with iodine that was in way too high a dose. I felt terrible after about five days or so. She if cause denied that would have caused it but I still believe it did. I have no thyroid problems in my family of origin. So now I have this ongoing problem with autoimmunity. I am so upset. I have had it for around 12 years now. I often have very high general antibody levels also. I was able to get these down a lot through the autoimmune elimination diet. Now I am with a different integrative medicine dr who has just put me on iodine spray as my iodine levels are extremely Low and have been also for years. This was tested again recently with a spot urine test. I am now so confused as to whether I should be taking the iodine. I was told u obviously need it if your levels are that Low. I was told to take two sprays a day but maybe I will just take one. Which I had been doing just a few times a week before this latest test as I was worried about overdosing again. I am so confused.
Barb – thank you for following this page.
I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hello Dr. Wentz:
I have done many different tests for the thyroid, including TSH, Reverse T3 Free T3, the antibodies, etc., and they all came out within the normal range, so my endocrinologist hasn’t diagnosed me with hyper or hypothyroidism. But I have thyroid nodules and a goiter and my iodine level is 50 mcg/L. I think I should take a 150 mcg iodine pill to see if the nodules might get smaller. My vitamin D level is 27 ng/mL. Vitamin B12 is 497 pg/mL. My doctors say those levels are fine but I know they’re not. I have many other ailments and haven’t been able to work in years. I have been taking Prevacid for gastritis/esophagitis and I think that is causing some of my symptoms and vitamin and mineral malabsorption. Please let me know what you think. Thank you and have a nice trip to Italy!
Lily – thank you for following this page. My heart goes out to you. 🙁
Most conventional physicians use the TSH test to determine if one has a thyroid disorder and to dose thyroid medications.
However, this test can often time be misleading, as levels of circulating hormones may fluctuate at different times, such as in Hashimoto’s, the person affected may fluctuate between highs and lows.
Additionally, when scientists first set the “normal” ranges of TSH for healthy individuals, they inadvertently included elderly patients and others with compromised thyroid function in the calculations leading to an overly lax reference range.
This resulted in people with underactive thyroid hormones being told that their thyroid tests were “normal,” based on this skewed reference range.
WHAT TO DO IF YOUR TSH IS NORMAL AND YOU ARE ANYTHING BUT
https://thyroidpharmacist.com/articles/what-to-do-if-your-tsh-is-normal-and-you-are-anything-but
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well.
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
Thank you Dr. Wentz. I have done all the labs you recommend for the thyroid and the results were optimal, but I have many symptoms of hypothyroidism. The only thing that was low was the iodine (50 mcg/L). Would you recommend taking the daily recommended allowance of iodine to feel better? Maybe that could also get rid of my thyroid nodules and goiter.
Lilly – I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in both animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Thanks for another awesome article Izabella – they are always so informative and well researched. I greatly appreciate it. I hope you have a wonderful holiday- well deserved I say!
Allyson – thank you so very much for your support! I hope you will check out my books. 🙂 Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Great article! I used high doses of iodine for my masthopathy. It helped really good with that. Unfortunately my Thyroid got worse. I stopped the iodine and my masthopathy came back. Now I am thinking about topical application of iodine.
Do you have any thoughts on that?
Dani – thank you for following this page.
I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hi Izabella,
I always read and appreciate your insights into all things Hashimotos.
I use mostly self prescribed natural supplements due to confusion and conflicting advice from practitioners – few of who seem able to effectively treat this disease here in Queensland, Australia.
As I am unable to earn an income, I have limitations as to what I can afford.
My symptoms are often confused with the combination of 3 viruses – Ross River, Barmah Forest and Epstein Barr – that I was afflicted with some 10 years ago & lay dormant until increased stress re-ignites them.
Similarly my symptoms are often attributed to my post menopausal 60 years of age.
In the last 2 years I have suffered from anxiety & depression resultant of the tragic and unexpected death of my beautiful teenage son.
I meditate, do yoga, walk on the beach and have regular acupuncture & massage in an attempt to relieve the sadness, loss & stress around the continuing legal process.
Stress equates with my thyroid condition though this is something I will never get over and rather learn to adjust to & live with.
I take many supplements and believe I now take a good combination.
For the last 6 years I have taken between 1600-2000mcg of Nascent Iodine each morning.
I have been told that Nascent Iodine is closely aligned to the Iodine produced by our own thyroid gland.
My symptoms pre the Nascent Iodine included a debilitating weakness of the wrists, ankles and knees that left me falling over & unable to lift anything even like a saucepan.
Eventually I could not get out of bed.
If I do not take my Nascent Iodine for 3 days these symptoms return, indicating to me that my body needs this.
Whilst I cannot seem to drop the excess weight I carry, my other symptoms like hair loss, irritability, poor sleep and excessive tiredness have been substantially reduced.
I take a pure brown seaweed – 1000mcg of Laminaria extract – with my evening meal and have recently started taking 1000mg Hawaiian Spirulina with breakfast.
It sounds like so much Iodine in various forms yet I feel it beneficial and have not yet crashed like another of your clients mentioned.
Should I be fearful of this happening to me after so long on these products?
As you seem cautious about Iodine, I wondered what your thoughts are about this.
Your expertise would be valuable with regard to the different types of Iodine and why my body seems to resonate with these quantities.
One of the other supplements I find essential contains 149mcg of potassium Iodine & 75mcg of Selenium in addition to Tyrosine, Withania & Rhodiola which I take x 2 daily.
Perhaps they balance out the Iodine?
I take many other supplements, use quality Essential Oils specific to healing my thyroid and have been on a mostly Paleo diet for 15 years.
Interestingly, since using the E O’s the ‘thyroid line’ across my neck has all but disappeared.
Thank you so much Izabella.
Pamela – I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in both animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Spirulina and Chlorella have immune stimulating properties that can worsen autoimmunity and even cause new onset autoimmunity. Additionally, the iodine is problematic and can cause further thyroid damage. Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hi there so I am borderline Hashimoto and keep all my symptoms at bay through a Ketogenic diet. I do supplement with iodine but never iodized iodine only nascent iodine. There is a difference and I recommend you look into other forms of iodine. Maybe even tell people there is other kinds of iodine. Table salt is bad in general and I advise everyone to never ever use it. I am a big fan of Himalayan sea salt and there is a huge difference. I enjoyed your article but feel you need to more clear that there are other forms of iodine. Thanks for your health knowledge.
Laura – thank you for following this page and for the feedback.
I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Thank you so much for this information, Izabella. This makes a lot of sense to me now – especially when you mentioned how excess iodine could be an environmental trigger for people with Hashimotos. I noticed my condition definitely worsened after a few months of taking pure iodine and sea kelp, after reading different posts online that it might help my thyroid. There is a lot of conflicting, confusing information out there – I’m grateful for your research and expertise on the matter 🙂
Pamela – thank you for following this page and for sharing. I’m looking forward to hearing your progress on this page. 🙂
A nurse practitioner who specializes in bio-identical hormones told me several years ago that she recommends supplementing iodine for anyone with a thyroid disfunction. Because of her recommendation, I began taking an iodine supplement. Within a year my hypothyroidism had turned into Hashimoto’s. After learning about the problems created with iodine supplementation and thyroid disease, I took myself off iodine and my TSH normalized. The high was 37, if I remember correctly. I am 71 years old and have been on thyroid medication since I was in my early 20’s. Back then, doctors just looked at your symptoms because blood tests were not used. My mother and sister had goiters, my daughter has nodules and half of her thyroid was removed this year because of a cancer scare. I have Hashimoto’s. Thyroid disease is very prevalent in the women in my family. After learning of my Hashimoto’s diagnosis, I became gluten free for eight months, but I didn’t feel any different so I have not been back to being gluten free. I am thinking of trying it again because of my fatigue, which is now keeping me from doing normal duties around my home. Age and my Hashimoto’s is really making me tired. I appreciate Dr. Wentz and her study into this disease. I have gone round and round with a couple of doctors over my thyroid issues including staying on T3/T4 medication. My insurance won’t even pay for my Armour thyroid. My doctor says Synthroid is good enough for me, but I need the T3/T4 combination to feel better. Synthroid does nothing for me. You have to fight the whole medical community anymore over this issue.
Sand – thank you for following this page and for sharing. My heart goes out to you. <3
A couple of years after my diagnosis, I found Hashimoto’s 411, a closed Facebook group run by Alice Berry McDonnell. This group is amazing! It is comprised of an army of highly motivated, smart, supportive women and men (now 45,000+ strong), and each of them sharing ideas of what worked for them, things they were planning to try, and offering support to one another. The comfort I received from knowing that there were others going through the same challenges as I, was enormous.
https://www.facebook.com/groups/hashimotos411/
Ask questions. Post your thoughts. Scan the files. It is an absolutely amazing resource. Best of all it’s kept private from spammers.
Thanks for this. I appreciate the detail in this post explaining your position on a very controversial issue.
Sue – thank you for following this page and you are most welcome. 🙂
I had a very negative experience with iodine supplementation. I have Hashimoto’s (TPO’s usually around 300), and subclinical hypothyroidism. I tested very low in iodine. I tried taking high doses and gradually began to feel worse, then really awful. My THS had climbed to 98 after several months on iodine! Unfortunately my doctor didn’t test for antibodies, yet I could tell they were way high. I was taking selenium supplements the entire time. Stopping the iodine helped immensely.
Kathleen – thank you for following this page, and I’m glad you listened to your body.
I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Izabella,
What do you think of people who promote “nascent iodine” as opposed to the iodide that’s usually given for supplementation? Does it affect the thyroid less powerfully, as proponents of nascent iodine claim? Or can it be just as damaging as iodide?
Theresa I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
I have Hashimoto’s and was given a low dose of iodine via a kelp-based supplement from a Dr. After 3 months on the supplement (150mcg of iodine) my TSH went up by 1 point to 3.2 and my thyroid antibiodies went up by 100 to 470. My free T4 and total T4 levels remained constant but my free T3 dropped to 2.2 and my reverse T3 increased by 10 to 43. Of course, I didn’t know these levels at first, I just felt like a crazy person having major anxiety. When I got the lab results, it all made sense. Even a small dose of iodine harmed me. And I was taking selenium with it!
As a child , my parents were told that I was allergic to Iodine. So, my mother made sure that I didn’t get any in any shape or form (no salt).
When I was around 34, I was diagnosed with Hashimotos. I was told then there was no help. My thyroid tests were normal. My research suggested, then, there may be help using Vitamin D. My anti-body numbers began to reverse. My endo had never seen that before. I am now 60. Ten years ago a doctor had told me that , in fact, I was NOT allergic to Iodine, but allergic to scallops.I hadn’t had seafood in years. Over the last few years , I have taken Iodine and Vitamin D and feel great ! My question? If , having no iodine all my life, how does taking it now impact my thyroid negatively?
Ellen – thank you for following this page. I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Dr. Wentz,
Thank you for all of your informative articles. I have one question about this article. Should iodine be taken by a Hashimoto’s sufferer who has had a full thyroidectomy? Does not having a thyroid change the protocols? Thanks!
Denyce – thank you for following this page.
I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocolou for following this page.
Dear Dr. Izabella,
I have been following your webinars and posts for a little while now and they have been very illuminating and refreshing!! Most being that I no longer feel like a weak flower and that something is actually amiss. I am by no means in a horrible way, it’s more that I know I am not living as vibrant as I could. I have been working with functional and integrative docs for a while and finally got some thryroid panels done. As I have been put in the “subclinical” category I am working on lifestyle, diet, energy medicine, some tinctures, supplement (adb5 plus) However, all the posts that I have read from you however, state elevated TSH and normal T4/T3 readings for this category.. Mine seems to be reversed with normal TSH (1.3-1.8) and low T4/T3 (12; 1.1). (see below for further) Can you please comment on the difference and what that means, if anything? Also, the serum thyroglobulin test (done at NHS in London) , they keep saying it shouldn’t have been administered b/c its for people with thyroid cancer. I still question it though b/c its so high and out of range, but may be irrelevant.
Thank you!
Stephanie
31st March ’17 7th April ’17 Range
Thyroglobulin antibodies <10 iu/mL <10 iu/mL 0-115
Serum thyroglobulin 19.5 ug/L 0.-0.9
Thyroid Peroxidase Abs (TPO) 16 iu/mL 15.3 iu/mL 0-34
TSH 1.86 miu/L 1.33 miu/L .27-4.2
FT4 16.9 pmo/L 12.7 pmol/L 12 to 22
Total T4 72 nmol/L 59-154
FT3 2.8 pmol/L 3.1-6.8
Total T3 1.1 nmol/L 1.3-3.1
Reverse T3 19 ng/dL 10 to 24
Steph – thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions.
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Hi Isabella,
Thank you for all you do!
Could you share how I could get the adrenals saliva test?
I did not see it on the lists of tests from the lab.
All my best,
M
Michelle – thank you for following this page.
The test I recommend is the one at the top of the page after opening this link.
https://www.directlabs.com/thyroidrx/OrderTests/tabid/29159/language/en-US/Default.aspx
I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
I have a goiter, and the usual cause is low iodine intake. My diet had little to no iodine in it. I found when I took iodine I felt better, when I didn’t, I would get pains in my thyroid. However, I reached a point, with diet and exercise, where I no longer needed iodine supplement. Now I do the wrist test with food grade iodine – a drop or so on the wrist and see how long it takes to absorb. When I craved iodine, it was gone in seconds, when I don’t crave it, it may never fully absorb.
iGiwt – I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in both animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
I’ve been looking for information about the effects of iodine (Lugol’s at 5%, 8 drops daily) applied topically when mixed with DMSO which increases the effect. With Hashimoto’s and TPO at 260, I wonder if it will have an effect on my thyroid when it’s topical, not oral. I have your books, ‘Hashimoto’s Protocol’ and ‘Root Cause’ but I don’t see anything about the topical application of iodine. If you can direct me to any literature, that would be most helpful. Thank you.
Patricia – thank you for following this page. I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in both animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
IODINE AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/iodine-hashimotos/
I have not noticed Spirulina/chorella affecting me due to iodine. I have noticed iodine reviving me up too much. I don’t take iodine daily and get Se in nuts/supplements. I put iodine sometimes on precancer hoping it will help. My hair test says I am low in iodine.
Please could you give me some advice. I live in South Africa and there are not too many doctors who take thyroid problems seriously. A year ago I went to see a new doctor who specializes in weight problems, he ordered special blood tests as I have a very rare type of brain tumour which has been partially removed. I was at that stage suffering very badly with narcolepsy it was found that I had an under active thyroid and was put on medication which has helped the narcolepsy but nothing else. The weight is still the same and my hair is still thinning. I am allergic to shell fish of any kind. please could you give me some advice.
Erica – Thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
http://www.thyroidpharmacistconsulting.com/europe1.html
Dear Dr Wentz
I would like to know what you think about Alpha lipoic acid. I used to take 250 mg after my breakfast (my doctor told me it was good for energy of the cell) and then i found this article… https://www.ncbi.nlm.nih.gov/pubmed/1815532
Do think it’s like calcium or iron ? or should people taking thyroid medication avoid Alpha lipoic acid ?
Thank you
Hi i have so many questions because after reading your blog i am getting more confuse.
1. At first when i diagnosed my TSH level it was 9.33 then my doctor recommend me for Levothyroxin.
2. after taking it my TSH level came back within the normal range . and doctor fix the 50mg per day but the probelm was that i was not feeling normal as i had been feeling before diagnosing hypothyroid.
3. Then i changed my doctor and at that time he stopped my medication for one week and checked my blood with TPO.
At that time my TSH level increased with TPO but i got checked first time with TPO so that s why i could not tell you in starting it was also increased or not or just after stopping the medicine it got increased.
4. My new doctor said that take same medicine again 50mg and then we will do the test again so after taking the medicine my TSH became normal.
5. In your documents your are telling that iodine is not good for my case , if i will not take Levothyroxin my TSH will be again high ?
6. now you tell me what i have hypothyroid or hashimoto’s, i live in Germany but my doctor is general physician not a endocrinologist?
7. you mentioned that Cruciferous vegetables are not good for Hypothroid and hashimoto’s as well but here “Root Cause Autoimmune Paleo Diet Plan” you asked to use Brussels sprouts, can you please tell why so much confusion here ?
Thank you so much.
Regards
Momna
Momna – thank you for following this page. I understand how frustrating this can be. Here are some articles that you might find helpful.
GOITROGENS
https://thyroidpharmacist.com/articles/what-are-goitrogens-and-do-they-matter-with-hashimotos
TPO ANTIBODIES
https://thyroidpharmacist.com/articles/hashimotos-and-tpo-antibodies
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
thank you so much for your reply , if any one wants to make some consultation with you how it can be possible and please guide me about seaweed usage and more impaortant can i take Ashwagandha ?
Momna – Thank you for following this page. Seaweed should be avoided because it can exacerbate autoimmunity and may contain high doses of iodine; excess iodine can be toxic in Hashimoto’s. I do provide a limited number of consultations, however, my consultative schedule is all full at the moment. I have a 12 week online program called Hashimoto’s Self-Management Program that covers all of the strategies that I go through with my one-on-one clients, in a self-paced format, so that participants have access to all of the things I’ve learned about Hashimoto’s without having to schedule costly consults with me or another practitioner. In addition, any person that goes through the program will get access to a Quick search Q&A Database of 1000+ questions asked by past program participants, Root Cause Assessment based on 100’s of my clients’ root causes and triggers, 2-week Meal Plans, recipes, and shopping lists to get you started on the following diets: Paleo, Autoimmune Paleo, SIBO, Candida. Also, Discounts on lab tests, high-quality supplements, and consultations and much more to support you in your journey! There are a few requirements that you should pay attention to, such as my book is a required read. Hashimoto’s Self-Management Program http://hackinghashimotos.com/ I also have a team of consultants who I’ve personally trained on the protocols outlined in my books and program. Generally, the team will give priority for consultations to those who have read the book and completed the program. You can find out more about my team and consulting services here. https://www.thyroidpharmacistconsulting.com/pages/meet-the-thyroid-pharmacist-team
Thank you so much for your response . i really appreciate of your hard work but i am sometimes confuse because if L-thyroxin is not good for hashimoto’s then if they will stop taking the medicine then their TSH level will increase again and please tell me about Ashwagandha. I know you can not recommend me because you are not my doctor but i am just asking your suggestion as you told about seaweed .
Waiting for your response.
Momna – thank you for your support. Here are a some articles you might find helpful.
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
DORTHEA’S HEALING JOURNEY
https://thyroidpharmacist.com/articles/dortheas-hashimotos-healing-journey/
Hi doctor! Hashimotos patient here. Currently worried bc I am doing an FET fertility cycle and was forced to get a chest CT w iodine last week. My TSH two days after shot up to 10. It was .5. I’m getting retested again today but just curious if the iodine could have permanently messed with me or possibly just temporary. I’ve been taking a high dose of synthroid for 18 years and never had TSH above 5.
I’m consulting my doctor but this article was so great I wanted to ask your expert opinion.
Kat – thank you for reaching out. <3 I am so sorry you are going through all of this. Iodine excess has been recognized as a trigger to Hashimoto’s. This is true particularly in people who are genetically predisposed to Hashimoto’s and who may perhaps have certain vulnerabilities like a selenium deficiency. If you have been exposed to high doses of iodine, it may be helpful to take a selenium supplement. As always I recommend that you discuss this with your practitioner who's care you are under.
Here are come resources you may find helpful as well:
Selenium
https://thyroidpharmacist.com/articles/selenium-deficiency-and-hashimotos/
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hi I have hoshimotos. My functional medicine doctor recommed taking 3 drops of Lugols Aqueous which has 6mg per drop. That means 18000 mcg right. But you recommend 150mcg. So I’m scared of taking it. Actually I haven taken it yet. Please help. Thank you
Minda – thank you for following this page. I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in both animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Is it actually true that huge doses of iodine permanently destroy thyroid cells and what is your source for this?
Jim – I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in both animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Dear Dr. Wentz,
Thank you for your reply. I am asking, because I have a history of juvenile onset arthritis, if I am at higher risk of Hashimoto’s. I have used big quantities of nascent iodine topically before, and I have had unnatural tiredness, pain in the thyroid area, cold hand and feet. Does this mean in theory that I could have damaged my thyroid regarding these symptoms? I’m saying in theory so no liability issue could occur. We’re talking only hypothetically here.
I look forward to reading your book.
With best regards, Jim
Jim – thank you for following this page. I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in both animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hi Isabella,
In researching and looking at PE supplements, I found their multivitamin, which has 200 mcg of Selenium as well as Iodine in the formula. Knowing how you feel about Iodine – is there another multivitamin of quality you would recommend, or is the iodine content insignificant if I am taking the PE Thyroid Support with it? Love to know your thoughts.
Jessica – thank you for following this page. I commend you for doing your research and taking charge of your health! 🙂 As a pharmacist, my concern with multivitamins is that they throw everything together in one batch, so the absorption of the nutrients can’t be guaranteed. Some vitamins are best absorbed on an empty stomach; others require food, an acidic environment, etc. Additionally, different minerals can inhibit each other’s absorption. I recommend starting one at a time, and then adding another a week or so later once it has been confirmed that the first supplement is not causing any harm.
I do have a full supplements chapter in my book. Have you checked it out? Not everyone should be taking every supplement and the book will help uncover your root cause. This will help you figure out your supplementation.
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
I’m grateful for your article on iodine. I’m just beginning journey with Functional Dr. She has me on S-Acetyl Glutathione, Mitocore, HPA Adapt, Jigsaw Blend Multi-Mineral, Opti-Mag 125, Bergamot BPI, Progesterone creme and an Probiotic. Though I’ve been diagnosed with Hashimoto’s 14 years ago, since being on this protocol, I have had many heart palpitations which I have NOT had for 14 years. Anyway, any of these supplements sound like they may be a potential cause? Just wanting second opinion. I am seeing my naturapath tomorrow and she has told me to remove mitocore, glutathione and Hpa adapt. Any help would be so welcomed 🙂 Thanks so much!
Leslie – thank you for following this page. I wish I could give you more direct advice but, each person will react differently. I would advise you to ask clinician who’s care you are under. I am not able to respond directly to these types of questions here. I also don’t recommend starting multiple supplements all at once. I recommend starting one at a time, and then adding another a week or so later once it has been confirmed that the first supplement is not causing any harm.
I do have a full supplements chapter in my book. Have you checked it out? Not everyone should be taking every supplement and the book will help uncover your root cause. This will help you figure out your supplementation.
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8…
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
I will check that out, thank you so much!
Leslie – you are very welcome! 🙂
I was diagnosed with Hashimoto in 2015. Ever since, my doc only recommended me to take Levothyroxine. Now, I’m 8 weeks pregnant and my TSH levels went up a little bit (3.66). I went to see a doc (my doc is in holiday and doesn’t answer the phone) and she recommended me a higher dose of Levothyroxine (150 mcg instead of 100 mcg) and 100 mcg of iodine. She didn’t run any tests, in order to check my iodine level. I don’t know what to do, as I’m afraid taking the iodine will be such a bad idea. I’m afraid it will affect my baby. I also talked to my OB and she also said it’s a good idea to take iodine, as I need more in pregnancy. Now what to do ? I’m confused and scared..
Denise – thank you for following this page. In the case of a deficiency of iodine, I do recommend iodine supplements but only in the dose range found in multivitamins and prenatal vitamins (most contain between 150 mcg–220 mcg). If you are deficient in iodine, an iodine supplement will likely help your symptoms and may improve your outcomes, but it is not likely to be a cure-all! If you are pregnant or breastfeeding, I do recommend a prenatal vitamin that contains iodine.
Here are some articles you might find helpful.
PREGNANCY
https://thyroidpharmacist.com/articles/hashimotos-and-pregnancy
Hashimoto’s destroyed my thyroid, and I have pituitary damage. I do not produce TSH, or any thyroid hormones. I’m overweight, low energy, and everything inbetween. So how could iodine supplements hurt me now? I have been to an endocrinologist who has told me I’m just old and it’s normal to feel this way at my age just deal with it. Others tell me there is nothing to do, just take this little pill and everything will be just fine. But it’s not fine. How do people get to see you? But readers can’t? I’m very frustrated. I lay in bed depressed often. It’s not right to feel this way.
Kathi – thank you for following this page. I understand your frustration! When I was first diagnosed with Hashimoto’s, I felt so alone. My doctor didn’t think it was a big deal, and none of my friends or co-workers had it. It wasn’t until I started to research online that I found others who were going through the same thing.
A couple of years after my diagnosis, I found Hashimoto’s 411, a closed Facebook group run by Alice Berry McDonnell. This group is amazing! It is comprised of an army of highly motivated, smart, supportive women and men (now 45,000+ strong), and each of them sharing ideas of what worked for them, things they were planning to try, and offering support to one another. The comfort I received from knowing that there were others going through the same challenges as I, was enormous.
https://www.facebook.com/groups/hashimotos411/
Dear Izabella, Please can you recommend a good doctor for thyroid problems in children??? I am also very confused on the iodine issue. I have ASD kid with thyroid problems and I am a cancer survivor, I had chemo and radiation 4 years before I got pregnant. A doctor told me that I must have been very iodine deficient while pregnant and that was why my child has ASD. I was going to supplement iodine since my kid has all the symptoms. But I read this article and do not know what to do. Thank you very much!
Veronica – Thank you for following this page. My heart goes out to you and your child. <3 Please, understand that due to liability issues, I am unable to answer specific medical questions, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
My most recent labs results (drawn last week) show that I’m severely iodine deficient. I also have Hashimotos.
I was so disheartened by this news because I’ve been trying to get pregnant for 3 years. I finally did a cycle of IVF and I was planning to implant my embryo this month. My fertility doctor is concerned that my iodine levels are too low as this may cause miscarriages or worse. This deficiency in iodine can cause developmental problems and even mental retardation in my child. He is also concerned about me taking “too high” of a dose of daily iodine. My functional medicine doctor believes I need to take 25mg of iodine daily to get my iodine levels up before I become pregnant.
I’m already 42 and my window for getting pregnant is quickly closing. That said, I am afraid to get pregnant with such scary iodine levels. I of course want to give myself the best possible chance of having a successful and normal pregnancy, and giving birth to a healthy baby.
My fertility doctor doesn’t know what the best path is, concerning these issues, and my natural path doctor feels like I need to be on high dose iodine. He subscribes to Dr. Brownstein’s iodine protocol and believes that is the path I should take.
I’m completely overwhelmed. I keep reading conflicting information on the internet. Not to mention, all of my doctors seem to disagree with each other. I don’t know who to listen to anymore.
Tess – thank you for following this page. I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
IODINE AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/iodine-hashimotos/
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hi Dr. Wentz, I love your book. Thank you! Your book and website helped me immensely in the beginning of my journey. You had so many of the same health issues as me when I discovered them.
I have Hashimotos but I’ve been able to get off of all thyroid meds. I also have narcolepsy and I’m almost off my meds for that entirely. This is all due to figuring out my specific nutrient deficiences and methylation status and correcting with targeted nutrients.
I am IODINE Deficient. My health and energy have improved so much over the past couple years. My life was a disaster. I already spent years fixing the gut (had blastocystis hominis) and I’m gluten and dairy free. I do have Hashimotos but I was prescribed LDN and it SAVED ME and I’ve had no Hashis flareups since being on it (it’s been two years).
I have new health issues though. I have a history of cervical cancer. I had a hysterectomy. But, now I have a large cyst on my left ovary, I have very painful, fibrocystic dense breasts and nodules and cysts on the thyroid. Doctors, normal ones, don’t care. They put bandaids on problems and wait it out till it progresses. I have done extensive research and learned that these tissue changes, esp in the breasts, can lead to breast cancer if nothing is done to improve the situation. I also have a high risk genetic mutation which increases my chances of breast and other cancers. I need to be here for my son who has chronic health issues. I am the only person here to help him. So, out of desperation, I discovered the importance of IODINE and discovered through testing, that I am deficient.
I am going to be my own guinea pig. The max I’ve taken is 500-600mcg in one day for a few days and I’m already not feeling great from it. It’s hard to take much less because a drop is about 600mcg. I tried to use a qtip to take half away from that amount. Some people online say to take more to push through the initial period. But, I started having anxiety and throat tightening issues and a bit of shortness of breath. I feel like my life depends on getting my levels up. I am not taking very much. I take selenium, B6 and every other antioxidant you can imagine. I used to have this reaction from selenium alone…so I am wondering if that might be the case. I know I need selenium though. I may need to try a different type. I’m going to be closely monitoring and documenting how things go. In the coming months, I will be rescanned (ultrasound likely) for my large hemorragic cyst on the ovary. I will also have another thyroid ultrasound and breast MRI in 10 months. I want to see things improve by then. I hope I can safely take a normal amount without the side effects. I am not sure if I have a question for you, but I wanted to share my story. I also wanted to thank you so much. It’s because of you I learned of LDN and it totally saved my life. LDN, and the nutrients combined, I believe are the reason why I was able to get off all thyroid meds and almost all my narcolepsy medication. The biggest breakthrough miracle for me was being able to get off the thyroid medication.
Beth – thank you for sharing your journey. I am very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
IODINE AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/iodine-hashimotos/
AMAZON
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hi Dr. Wentz,
Do you still do case reviews? I really need help. No insurance and self treating. I have a goiter. I took iodine of all sorts for awhile and a lot of seafood at once. It seems I may have overdone it as I now am sensitive to iodine. Anytime I take it any form, even in multivitamins, I freeze. Not sure what that means but I’m trying to get rid of the goiter and it seems now the one thing that seems to do that I can not take anymore. I lean towards hypothyroidism: I have all the symptoms, very lean but have a lot of belly fat( with tons of exercise); usually cold even in the summer in Houston, ridged pinky and ring finger nails, and as of late very moody and melancholy and oh yeah been very fatigue but seemed to improve since changing a few things, and GERD. All are driving me crazy. I am trying to fix myself fast because I like everything to be done fast. VATA. But I am working on patience. But very low and slow. I take all the supps necessary for this situation, selenium, mag, vit c, NAC, zinc….still nothing in terms of goiter. Wondering if I should take NDT. I need help. I want to feel better. And be better
Christine – thank you very much for your inquiry. I do provide a limited number of consultations, however, my consultative schedule is all full at the moment. I have a 12 week online program called Hashimoto’s Self-Management Program, that covers all of the strategies that I go through with my one-on-one clients, in a self-paced format, so that participants have access to all of the things I’ve learned about Hashimoto’s without having to schedule costly consults with me or another practitioner. There are a few requirements that you should pay attention to before enrolling to this course, like reading my book. Here is the link to the program:
Hashimoto’s Self-Management Program
http://hackinghashimotos.com/
And here is the link to my book in case you haven’t read it already:
Hashimoto’s Root Cause
https://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol (this is my latest book)
https://www.amazon.com/Hashimotos-Protocol-Reversing-Thyroid-Symptoms-ebook/dp/B01HXK6GVQ/ref=sr_1_1?ie=UTF8&qid=1505933035&sr=8-1&keywords=hashimotos+protocol+izabella+wentz
What about the ingredient povidone in levothyroxine? I see my l-thyroxine contains it. Can this have a negative impact on your body?
Arlie – thank you so much for following this page. There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
HOW THE DOSE OF YOUR THYROID MEDICATION CAN UNCOVER YOUR ROOT CAUSE
https://thyroidpharmacist.com/articles/the-dose-of-your-thyroid-medication-can-uncover-your-root-cause/
HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications/
What about those of us with Hashi’s that have fibrocystic breasts and monthly breast pain/tenderness? Would you suspect an iodine deficiency here? I’ve been taking magnesium for years.
Tara – Thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms. Here are some links which might help:
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
MY RECENT CHALLENGES AND FINDING DR. RIGHT
https://thyroidpharmacist.com/articles/my-challenges-and-finding-dr-right/
Thank you for this article. I must be part of the very very sensitive to iodine… Diagnosed with Hashimoto in 1999 since i tried few times to take iodine because when you say you have hypothyroidism everybody tells you “you should take iodine”… Last time i tried was last week with trace element iodine. One cap equals 150 microgram. I took 12 drops wich is about 1/10 so 15mcg… The same day i felt great but the day after in the afternoon i started to feel really bad. I had to go to bed, i slept, i was cold and what i hate the most i was depress… It last for 5 days, today is better. I don’t understand why I react so violently to iodine. Before I could eat a little seaweed or gomasio algae it’s no longer possible. I was wondering if it’s partly because of the synthetic thyroxine (Tirosint) that I’m taking? Is thyroxine made from synthetic iodine? So it’s either too much or it has absolutely nothing to do with it? One thing i have to say is that the year before i was diagnosed i was craving for salt and algue and i remember having a whole bag of seaweed everyday for few days…
If we need iodine and iodine tests are not valid, how do I know if I have iodine deficiency?
Thank you
Marie = Thanks for reaching out! I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashimoto’s thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in both animal and human studies.
I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books:
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Thank you Izabella
I’ve read both your books and I’ve learned a lot. Since 2015 the antithyroid antibodies have begun to decline and by 2016 they were below the norm. By avoiding everything that generates inflammation and with probiotics among other things I have succeeded this exploit. For me Hashimoto is at rest but it seems that my immune system is always “unbalanced” because as soon as I take a product that stimulates the immunity or iodine it restarts… How do I get my immunity back to its original state?
Thank you
Marie – thank you for reaching out. I am very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. I hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
Here are the links to my books :
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
I was so happy to see you state that the introduction of Iodine supplementation be approached with caution. I have Hashimotos and after an extended time of supplementing with Selenium supplements my homeopathic doctor had me introduce Iodine. At the time, we knew that I was also Celiac, but did not realize that my long standing skin issues were a Celiac associated disorder referred to as Dermatitis Herpetiformis (DH). After adding Iodine to my regime, the DH exploded from just my scalp and neck to everywhere above the waist. To say that the experience was unpleasant would be a gross understatement. It took diligent study and research to realize what I had done to myself and diagnose the DH and then toss the Iodine. I still take Selenium, but watch the foods I eat that are high in Iodine and have not only been gluten free for 11 years, but have also gone grain free for 4 years, since the Iodine/DH episode. The DH is somewhat under control, but there are always uncomfortable outbreaks. At least, I know now what is going on, unlike the first 60 years of my life.
Catryna – thank you so much for sharing your journey with me! ❤️ i’m so happy to hear you are taking charge of your health and have been able to get this disorder under control. Please continue to keep me posted on your progress.
Hi Dr. Wentz,
What is the best test to find out accurately if a person is deficient in iodine? I had a blood test done, but have since read that those only indicate recent exposure. ?
Thanks!
Jen – thank you for following this page. Testing for iodine deficiency consists of blood tests, urine tests or “spot” tests (where you paint yourself with iodine until it disappears). Unfortunately, to the best of my knowledge, the tests are not able to reveal an iodine deficiency or excess, rather they will be reflective of your recent iodine intake. Some things that may lead me to suspect an iodine deficiency include: eating a vegan diet, eating a diet low in seafood, fibrocystic breasts (though this could be caused by magnesium deficiency), low reverse T3 on a lab test, or a negative reaction to selenium (which is very rare). You might find these articles helpful.
WHY WOMEN HAVE MORE THYROID DISORDERS
https://thyroidpharmacist.com/articles/women-thyroid-disorders/
NEW STUDIES ON MAGNESIUM AND THYROID HEALTH
https://thyroidpharmacist.com/articles/new-studies-on-magnesium-and-thyroid-health
Doctors have told me for years that my thyroid is normal in spite of hair loss, fatigue, brittle nails. I hit my head in a fall 9 months ago and the CT of my head and neck revealed a 1cm thyroid nodule. My MD checked T3 T4 TSH said all’s well. I did a little research on thyroid and decided to try high-dose iodine. Got the pro-Iodine books. Not sure, but I think I got up to 15 drops of 2% lugol’s per day. Felt better at first, hair seemed stuck in my scalp a little better, eyebrows grew back. At some point the results declined and at some point I stopped supplementing. After a few months the fatigue was terrible and I decided to resume the iodine slowly. I got up to taking 7 drops over a course of about 2 weeks when one night I discovered a grape-sized bump over my thyroid. Visible. Ultrasound this week says 2 cystic nodules with solids: 1cm and 2cm with indications of overall thyroid inflammation. Nodules mildly suspicious. I’m concerned that my naive playing with iodine has caused major damage.
Isidora Thanks for reaching out! I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashimoto’s thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in both animal and human studies.
I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books:
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Dr. Wentz,
I have Hashimoto’s thyroiditis. For that I am avoiding iodine, but taking Selenium+Zinc (100mcg of Selenium per tablet). I am also taking vitamin D spray (at that point 3000 units per day) and B12 spray as I am vegetarian. My blood tests in November (2017) show that my B12 is very high (1257 pmol/L; normal values are supposed to be 145-569). After that I stopped taking B12 and my blood tests in January (2018) show I still have high B12 (885 pmol/L). However, at that point I also had my Vitamin D checked and it was 47,2. After that I started taking 6000 units per day.
My question would be: is high B12 anyhow linked to Hashimoto? Isn’t B12 supposed to be water-soluble?
(I should probably add that I have Gilbert’s syndrome as well).
Thank you for your answer in advance.
Fond regards from Slovenia (Europe)
Mirjam
Mirjam – thank you for following this page. I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms.
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
You might find this article helpful as well.
MTHFR
https://thyroidpharmacist.com/articles/mthfr-hashimotos-and-nutrients/
Dear Izabella,
Thank you for all your work; it’s been a revelation and given me hope. Living in Greece, the general mentality is, “There’s nothing you can do. Your body is attacking your thyroid and, one day, there’ll be nothing left. Accept it and take the pill for the rest of your life. No, changing your diet won’t do anything. Gut is unrelated. Just go on a diet to keep your weight down.”
What I’d like to ask is whether using skin care products that contain normally iodine-rich ingredients, like seaweed oil or microalgae, should also be avoided. It seems impossible to determine whether such cosmetic ingredients have maintained any of the iodine, or how much of it would be safe to use. I’m asking this both as an aromatherapist and a Hashimoto’s warrior.
Thank you in advance for your time and input.
Kind regards,
Despina K.
Despina – Thank you for this question. I’ll add this to my list of future article possibilities. ♥ Our skin is a window to our internal health. It is the body’s largest elimination organ, and also a canvas where toxicities, nutrient deficiencies, food sensitivities and hormonal imbalances can show up. As a pharmacologist, I can tell you that what you put on your skin definitely gets absorbed into your body! Here are some articles you may find interesting! 🙂
ARE YOU SACRIFICING YOUR HEALTH FOR EXTERNAL BEAUTY?
https://thyroidpharmacist.com/articles/are-you-sacrificing-your-health-for-external-beauty
THE THYROID AND SKIN
https://thyroidpharmacist.com/articles/the-thyroid-and-skin You could also check out
You can also check out the website http://www.safecosmetics.org/ or search http://www.ewg.org/skindeep/search.php to see how your products compare.
I can not find which supplements you do recommend and dosage?
Lisa – thank you for reaching out. I currently use and recommend practitioner only brands that are free of fillers and
where the companies practice excellent quality control methods. Here are some article links which might help:
WHICH SUPPLEMENTS ACTUALLY HELP HASHIMOTO’S
https://thyroidpharmacist.com/articles/which-supplements-actually-help-hashimotos/
USING ENZYMES TO OVERCOME HASHIMOTO’S
https://thyroidpharmacist.com/articles/using-enzymes-to-overcome-hashimotos/
THE FOUR BEST PROBIOTICS FOR HASHIMOTO’S
https://thyroidpharmacist.com/articles/the-four-best-probiotics-for-hashimotos/
I have also created my own supplements brand, which is named Rootcology. Rootcology’s mission is to provide safe and effective supplement solutions for people struggling with autoimmune thyroid conditions. These supplements are composed of high-quality pesticide-free ingredients, do not contain soy protein, dairy, or gluten ingredients, and undergo third-party testing to ensure that the ingredients on the label match the ingredients inside each bottle. Here is a link to the website: https://www.rootcology.com/collections/supplements
Hello Izabella,
I could really use your advise.. When I started seeing a naturopath in April 2017 my thyroglobulin antibodies were .2 and (TPO) ab was 25. She said I didn’t have hoshimoto anymore, I just had hypothyroid. She started me on 12 drops of Lugol (2%) per day. Within 2 days I had all the symptoms and more. I couldn’t get out of bed. I thought I’m gonna die. I continued with it for 1 1/2 month since she convinced me this will heal my thyroid. After that 1.5 month we kept on reducing Iodine hoping my symptoms will go away. I reduced the iodine drops to 2 drops a day but my symptoms didn’t go away. We slowly kept increasing the iodine drops back again. 1 drop daily every 2-3 weeks. By first week of march 2018 I was on 13 -14 drops per day. After starting Iodine in April 2017 I went for my physical in October 2017. My blood platelet count was 836 and white blood cell count was 12, Neutrophils Absolute 9.1 and Comp. Metabolic Panel 14. So all these numbers were high. Before starting Iodine my platelet count along with other numbers have never been high. I rechecked my numbers in jan 2018 blood platelet was 810 but white blood cell count and all the other numbers were normal, CRP was less than .2. I started taking Curcumin 500mg twice daily. Increased my omega capsule and started taking MK7 300mg daily. Repeated the blood work on May 17, 2018 my platelet count is still 875, CRP was less than .3 and all the other numbers are normal. My physician also did an ultra sound on my spleen, everything was normal. I’m seeing an oncologist just to rule out things. I guess my question is could Iodine have caused my platelet count to be high and no matter what I’m doing the inflammation is not going down. I live a very clean chemical free life the kind you talk about in your books. BTW I have all your books. My physician says if oncologist rules out all the possibilities then he wants to start me on a medication to lower my platelet count. I don’t believe in taking pharmaceuticals. I will be flying soon out of the country, I don’t want to end up having a stroke of heart attack. I have stopped taking any iodine for 6 weeks now. I only take 150 mcg that’s in my multivitamin. I don’t know what I can do. Please suggest something.
Thanks
Sarika – thank you for reaching out. I am very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here is an article you might find helpful:
IODINE AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/iodine-hashimotos/
Here are the links to my books as well:
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Jan ’18 N.D. started me on 3mg Prolamine Iodine daily, plus other supplements that have mcg’s in them, I read your article and it really has me questioning her advice!! This was started after testing and finding my TPO >6500, and TgAb 115, in Dec ’17. They have not been retested. I’ve seen endo and int. about numbers and they say, I Just have to live with it! It’s a symptom of my disease (Hashi’s), that they will never go away, but to Diet, Exercise and Lose Weight! They do not get it! When you feel like crap and are fatigued ALL the time, feel physically and emotionally drained and without hope it’s really difficult to push thru daily necessities to live, let alone diet and exercise, besides it’s not a “diet” thing in the way they mean. I went GF Nov ’17, No Soy, No Dairy, I don’t drink soda, or alcohol, and do not eat fast food or anything that comes packaged. I cook “Real Food” and eat clean. If only they new the person I was before the disease they may not think i am just a lazy fat old lady now! Feeling frustrated.
W – thank you for sharing your journey. I am so sorry your are struggling. <3 I understand how frustrating this can be. I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
What do you think about taking a liquid Nascent Iodine supplement?
Karen – thank you for reaching out. I am very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books :
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hi Izabella! Thank you so much for another so informative and well written article. I wonder about detoxified iodine that was developed by Edgar Casey. Do you know anything about this? Would this have another effect on the thyroid than normal iodine? Or would it be the same? Thank you!
Didi – That’s a great question and unfortunately I don’t have any information to share with you at this time but, I will add this to my list of future article possibilities. I would advise you to discuss this with your clinician.
Dear Izabella,
I would like to ask you a question about iodine deficiency and hashimoto’s. What if I really eat a diet low in seafood and I have enlarged thyroid gland with hashimoto’s thyroditis? Should I take multivitamin which contain 150mcg potassium iodide, 200mcg selenium yeast supplement and 2000IU Vitamin D?
Hudson – thank you for reaching out. I am not able to advise as to whether this supplement or any other supplement would be appropriate for you and your specific health needs without a comprehensive health assessment. I recommend that you discuss the use of supplements with your personal doctor.
Thank you for all your hard work and good info you provide for us Hashi’s! My D.O. has me drop one drop of Lugo’s iodine on my skin every day. Apparently, if it disappears fairly quickly then your body needs it and if it stays on your skin for hours then, your body doesn’t need it. I have not seen this method mentioned in any of my Hashimoto’s study? I started taking selenium not for the effects of iodine, but because a micronutrient test showed I was deficient. I wondered what you thought about this iodine protocol? Thank you, Lucy
Lucy – you are very welcome! I am very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books :
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Thank you so much for responding to my question. I’ve read both of your books and wondered why my D.O. was giving me iodine? I thought maybe her method of dosing by what my skin would absorb was acceptable? I’ll print out your thoughts on the iodine debate and take it to my next appointment. In the mean time, I’m stopping the iodine. BTW, congratulations on the birth of your baby girl❣️ Your demeanor seems happier! ?
Lucy – you are very welcome! I hope you will keep me posted on your progress. <3
Hi, I’ve read your article with interest. I’ve had hashimoto’s for decades and it was untreated/neglected by the medical profession for a long time. I also have had coeliac disease and been gluten free for over a decade, so that’s 2 autoimmune diseases that have never really fully been treated properly.
I discovered the AIP diet earlier in the year and I’ve also tested positive for leaky gut antibodies, but it’s been a struggle to get any further forward. I still struggle with energy, fatigue, brain fog etc. It’s a kind of chicken and egg scenario, which do I try to fix first?
My thyroid issue doesn’t seem to be resolving, I’m still fatigued and brain foggy all the time, and my tests don’t seem to get any better.
One very interesting thing I read recently was when moving to a paleo diet we naturally eat more cruciferous vegetables. I am very aware of the impact of these on the thyroid, and while eat in moderation (ie not daily) I still eat more than I used to.
I read that cruciferous veg can prevent iodine uptake, and as a result the thyroid doesn’t get what it needs and the condition can worsen or stagnate, and increasing thyroid meds doesn’t help.
In order to prevent this issue it was recommended to supplement with iodine just a little, alongside selenium, which I already take, alongside a good multivitamin which I thought until recently contained the recommended daily allowance of iodine. It actually doesn’t, so whilst I eat plenty of fish and seafood, perhaps my moderate increase in cruciferous veg is having an impact by preventing iodine uptake and making me sluggish. I’m doing everything else right so this seems to be a reasonable explanation?
What’s your position on this particular school of thought?
I’m interested in trying it but am cautious as I had a bad experience with spirulina in fruit juices years ago that took a long time to resolve, but that was before I knew it was high in iodine and before I knew lots more about Hashimoto’s and the supporting nutrients.
Many thanks for your time, and happy holidays!
Vanessa – thank you for reaching out. Iodine deficiency is not widespread in people with Hashimoto’s, and thus eating cruciferous vegetables (unless a person is otherwise sensitive to them) is perfectly healthy for people with Hashimoto’s and should not impact thyroid function. In the case that a person does have hypothyroidism due to iodine deficiency, he/she can still enjoy crucifers as long as they are cooked or fermented. Cooking/fermenting will break down the iodine blocking content. You can read more about the breakdown of the science behind the thyroid and goitrogens. I am very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Here are a couple articles you might find helpful:
IODINE AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/iodine-hashimotos/
TOP 7 HASHIMOTO’S MYTHS
https://thyroidpharmacist.com/articles/top-7-hashimotos-food-myths/
Hope that you will check out my books as well. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books :
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hi again
I’m not talking about supplementing over and above the daily recommended allowance of iodine, but what with my restricted diet since May this year I possibly haven’t been getting enough for normal function, so was just thinking I just need to get the normal intake again. Why would it not be advisable to have normal amounts of an essential nutrient?
Vanessa – thank you for sharing. <3 I understand. <3 Unfortunately, I am not able to advise on whether this supplement would be appropriate for you and your specific health needs without a comprehensive health assessment. I recommend that you discuss this with your personal doctor who's care you are under.
Hi again
Whilst it would be nice to have a personal doctor to be in the care of, unfortunately the healthcare profession in the UK is light years behind in the endocrine field (and sadly many others), and they just don’t believe in any other kind of treatment. It’s thyroxine monotherapy that is poorly tested and poorly monitored, or nothing. I’ve been to one of the best thyroid consultants in the country and they barely acknowledged the fact I had hashimoto’s, and I had to fight to get them to even test for it. And this was 12 YEARS AFTER I was formally diagnosed and put on thyroxine. For 6 years before that doctors refused to acknowledge my thyroid condition and I suffered hugely. I know this is a familiar story for many people.
So you can see, I’m on my own with this, which is why I come to these forums. And I know I’m definitely not alone on that score.
I have recently bought one of your books, and discovered your website round about the same time without making the connection at first, and have picked up some interesting things I did not know, especially having read many other thyroid related books, but so far nothing has really gone far enough to resolve my issues. Fatigue and brain fog are my biggest day to day problems, in addition to leaky gut which I have also read up on a great deal and am currently treating, but my health status just stays the same, no real change in either direction. Candida and SIBO tests always come back inconclusive (and treating anyway does nothing), parasites and h pylori are always negative. The AIP Protocol has been generally good for me, but nothing more than that, and I still have blood sugar issues. I don’t really know where to go next.
I’ve read your thiamine article with great interest, so am slowly building up my dose of that, and I’ll see what happens. I already take selenium, sublingual B12, magnesium, and vitamin D in the theraputic doses. I’m wary of supplementing with iron as I never test positive for anemia, my iron tests are always pretty good, my multivit contains a little iron and I eat a sensible amount of beef, so I think I’m pretty safe there.
Vanessa – thank you for reaching out and sharing your journey with me. I understand how frustrating this can be. <3 Hashimoto’s often is a combination of food sensitivities, nutrient deficiencies, adrenal issues, gut issues as well as an impaired ability to get rid of toxins. Any of those things would prevent a person from getting better.
Hashimoto's is very much an individual condition. While there are root cause commonalities, each person will have their own or in some cases, more than one root cause. You will have to start with the simplest modifications, by removing triggers, followed by repairing the other broken systems to restore equilibrium, allowing the body to rebuild itself. You will need to dig down to why the immune system is imbalanced in the first place and this will tell you how you begin to finally feel better, reduce your thyroid antibodies and even take your condition into remission.
You will have to create your own health timeline. Look back at your overall history as far back as you can remember. Look for infections, periods of severe stress, the use of medications (especially antibiotics, antacids, and oral contraceptives), accidents, and exposure to toxins. These are events that may have contributed to Hashimoto's. Once you do, you will know what types of changes you need to implement to make yourself feel better.
If you need further support, please check out the list of lab tests inside the “Testing” chapter of my book, Hashimoto’s Root Cause. I also offers a 12-week program, Hashimoto's Self Management Program. Here are some resources you might find helpful as well:
BUILDING YOUR OWN HEALTH TIMELINE
https://thyroidpharmacist.com/sample-health-timeline/
Hashimoto’s Self-Management Program
https://thyroidpharmacist.com/enroll-in-hashimotos-self-management/
PS I have tested and treated Adrenal fatigue successfully, so no more issues there. I also have no RT3 pooling.
I just found your website today. I’m currently being treated by a clinician who has done the things you have recommended.
This past year I have been going through the protocol for healing the gut, the Paleo diet, etc, to try to get my body functioning properly. Currently I’m on bio-identical hormone treatments, including thyroid, but my thyroid is being very stubborn. After reading your article about iodine, it made me curious.
Years ago, I had a CT scan. They were only able to get a small portion of the radioactive iodine in my IV before I went into anaphylactic shock and was rushed into the ER. They told me that normally, a person doesn’t have an allergy to that unless they’ve been exposed before. I had never been exposed to that before. After my reaction, I also discovered that both my sisters are allergic to iodine.
I’m using iodized sea salt for cooking, because I was told it have the same properties as iodine. It’s not the same, they assured me.
Before the test, I could eat whatever I wanted and never gain weight. After the test, it got more and more difficult to keep the weight off, to being a constant battle, along with severe fluid retention. I have constant cravings for salty foods. I just looked at my multivitamin, and it has 75mcg iodine (as potassium iodide).
Have you found anything in your research about iodine allergies causing problems?
TD – thank you for reaching out. I am so sorry you had to experience all of this! <3 My heart goes out to you. I am very hesitant in recommending iodine in Hashimoto's. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto's is a different mechanism. It's like pouring gas into an engine that's on fire... that's essentially what's happening in Hashi's, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let's fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books :
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hello Dr Wentz,
In October my iodine level was 43 but recently my bloodwork showed that it has dropped to 37. My PA has suggested I take 225 mcg of iodine 4x/week but after reading your articles, I am hesitant. Also, my TSH was 1.7 in October but was elevated to 10 in the recent bloodwork. I’m very upset by this and puzzled as to why the big change when I’ve been taking my Natur throid.
Liz – thank you for reaching out. I understand how hard this all is. <3 I am very hesitant in recommending iodine in Hashimoto's. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto's is a different mechanism. It's like pouring gas into an engine that's on fire... that's essentially what's happening in Hashi's, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let's fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books :
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hi Dr. Wentz,
I’m one of those has been a very big advocate of the iodine protocol. For a long time, it was the only thing that got me anywhere near normalcy. In the last week or so though, from going back to the drawing board on my research, i’ve come to feel that I’ve taken I have done it such a high dose for a long enough time (like about a year) that if an iodine deficiency were my continuing issue (I say continuing because I do believe it was absolutely necessary for probably the first 6 to 8 months), Or were my issue at this point, surely I would have reached some sort of level of satiety by now.
I have an upcoming thyroid ultrasound and I had really good results on my last one, results my doctor said it was impossible, because I was taking iodine. So I found myself wavering about whether I was going to walk into this thing and have the same result even more improvement, or if I was going to find out this time, it backfired on me and was now doing damage. I believe that when we keep finding messages and information coming out of the OR saying a certain thing, we’re meant to listen. I’m spiritual from this perspective. So the last couple of days, I suspended my dose and tried taking a little more thyroid medication instead. I found myself with such uncomfortable, unsettling hyper thyroid symptoms, that I weld up taking 50 mg and I RL both days. I noticed a little bit more hair loss in the shower, I had a racing heart beat downs but hose, severe anxiety and that was sufficient to make me doubt myself. My recent tests show that my T4 is suppressed which bothers me for the primary reason that if the only reason I don’t is making me better, or making me feel better, is that it is overtly suppressing my thyroid and causing it to behave as if it were not there, then that’s not really healing and getting better, is it? What I want is to be healed. The thing that made me start trying not to take the iodine is that I wanted to see if I had healed enough not to need it. I was hopeful. I was disappointed.
What I’m going to be trying next is stepping down from it. Based on my symptoms when I tried to go cold turkey like you recommended, I don’t recommend anybody who’s doing high dose iodine do that. I’m also going to add a separate selenium supplement beyond words in my multi and some tyrosine to it. I wanted your advice on how to heal of the thyroid gland from any inflammation the iodine MAY have caused. I would greatly appreciate it. Thank you so much.
Nikki – thank you for reaching out and sharing you journey. I am so proud of your for taking charge of your health. I am very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. You also may want to check out the article above where I discuss a client of my named Jenny. <3 Here are the links to my books as well:
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
I need your help. I have hypothyroid Hashimotos and am on Tirosint 125 mcg. I have to thyroid nodules followed for 20 years but only hypo hashi diagnosed 5 years ago And menopause and on estradiol and progesterone. I had to go the ER for severe side pain and morphine was given, ultrasound of right side and IV contrast for abdominal CAT scan. I did not know thcontrast was iodine until in the test.
During the test I shared and dealt with throat swelling up but worked to stay calm and feel the pressure on both side of airway and chin slowly back off. 18 hours later I feel swelling again. And it ebbs off some. I’m having to take Klonopin to calm down when nothing is upsetting. What do I need to understand to know what my thyroid is or is not doing? Please help me understand.
Veveca – thank you so much for reaching out and sharing your journey. I am so sorry to hear you experienced this. <3 My heart goes out to you. Please understand I am unable to answer specific medical questions. It would not be legal or appropriate for me to give any type of medical advice without a comprehensive health assessment. I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It's a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
COMPOUNDING PHARMACIES
https://thyroidpharmacist.com/database-recommended-compounding-pharmacies/
Recently my endo gave me a whole barrage of blood work. I have Hashimoto’s and have been avoiding iodine, including the salt. My Omega 3 ratio needed some improvement according to bloodwork. I started taking krill oil supplement and increased my fish consumption, especially sardines because they are low in mercury supposedly. I haven’t had antibodies tested since starting the fish oil, but I did develop another nodule. It was biopsied last week, but I am confident it is benign since I have 2 other nodules that were determined benign. My question, how much iodine does krill oil contain and might I be exacerbating my Hashimoto’s by taking in more fish? Kind of darned if you do and darned if you don’t.
Jane – thank you for reaching out and sharing your journey. I am unable to say how much iodine would be in the brand of krill oil you are taking. Here is an article you might find helpful:
FISH OIL FOR HASHIMOTO’S
https://thyroidpharmacist.com/articles/fish-oil-for-hashimotos/
Thank you, very informative article!
Jane – you are very welcome! <3 I hope you keep me posted on your progress.
Hi! First, I want to say THANK YOU so much for all your hard work and research to create so much educational material for Hashi sufferers! I’m reading your HP book for the third time! Second, I was wondering what your opinion was of the Seeking Health Optimal Prenatal tablets? I normally am a fan of Dr. Lynch’s products but saw that the iodine amount included is 250mcg? Thank you so much!
Kelly – thank you for reaching out. Unfortunately, I have not been able to evaluate this supplement. Taking a quality prenatal supplement is important to the health and development of your baby. I recommend the Designs for Health Prenatal Pro Essential Packets. I also recommend that you discuss the use of any supplement before using with your practitioner. Here is a link: https://www.purerxo.com/thyroidpharmacist/rxo/products/product_details.asp?ProductsID=2397
Hi Dr. Izabella,
I never had thyroid issues, but a practitioner suggested I take high dose of nascent iodine. I did not take selenium with it. I took 3200 mcg of (8 drops of 400 mcg over an 8 hour period). I ended up in the hospital with renal and liver failure, delirium, elevated heart rate, elevated blood pressure for 9 days. That was over a month ago, and just this week have the anxiety attacks subsided and I am able to physically fall asleep without any meds. I’m 38 years old and was in perfect health, on no medications. Now, I have a constant metallic taste in my mouth and my renal and liver numbers are still off. No physicians I have been too understand about iodine. Do you have any suggestions or know if my thyroid and other organs should recover? Was that dosage exceptionally high? The bottle said a person could take up to 3 drops, 3 times daily. So what I took was still under the amount on the bottle. Thank you for your help, as I am at a loss in finding any help.
Melissa – thank you so much for reaching out and sharing your journey. I am so sorry you had to experience this. <3 My heart goes out to you. I am very hesitant in recommending iodine in Hashimoto's. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto's is a different mechanism. It's like pouring gas into an engine that's on fire... that's essentially what's happening in Hashi's, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let's fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books :
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hi Dr. Wentz,
I have 2 questions (I apologize for the length of the second one though).
1) What are you thoughts on treating sero-negative Hashimoto’s with Restorative Formulations Thyroid Px?
2) What are a patient’s options when neither her PCP, Endocrinologist or Naturopath are willing to properly address a thyroid condition? In 2017, I was diagnosed with Premature Ovarian Failure (POF), and have been struggling to conceive a baby. I’ll be 40 this year (diagnosed at 37 years old) and have hormone levels consistent with a 60-70 year old woman. The cause of my POF is idiopathic, but I do have a long-term history of an autoimmune condition.
Since 2017, I’ve done thyroid panel blood work, and my results are never consistent. I always have an elevated thyroglobulin and my labs swing toward hypothyroidism. An ultrasound last year showed I had a small thyroid nodule, and bumpy texture to my thyroid. The nodule was biopsied and found to be benign. From my research, I believe I have sero-negative Hashimoto’s. However, each provider I’ve consulted with will not prescribe any medication. They all say sero-negative Hashimoto’s isn’t well documented and I don’t show any evidence of having this condition. I’ve been taking thyroid supplementation with zinc, selenium and iodine, but I really feel I need medication. I’m located in Northern CA (Sacramento to be exact), and don’t have any options left to get help.
So, what would you recommend for someone in my situation? I believe that if I could address my underlying thyroid issues, maybe it would help resolve my severe infertility issues.
Shalar – thank you for reaching out and sharing your journey. I am so sorry you are struggling with at this. I understand how frustrating it can be to find a practitioner that will listen. About 95% of people with Hashimoto’s have elevated Thyroid Peroxidase Antibodies, while 80% will have elevated Thyroglobulin Antibodies. They can both be important in monitoring the autoimmune attack on the thyroid, and can both be used to monitor the effect of interventions. Some interventions will lower TPO antibodies more, while others will have a greater effect on TG antibodies. This can depend on the individual and their body’s response.
Some people with Hashimoto’s test negative for thyroid antibodies because their overall immune health is so weak, they do not produce enough antibodies. I tested negative for antibodies several times. Now, I insist on a thyroid ultrasound. A thyroid ultrasound can be used to detect changes in the thyroid, associated with Hashimoto’s. Given that Hashimoto’s is one of the leading causes of hypothyroidism worldwide, it’s best to be certain, one way or another. I have written several articles about how to best decrease thyroid antibodies.
Here are some articles I think you might find helpful:
HASHIMOTO’S AND THYROID ANTIBODIES: PART 1
https://thyroidpharmacist.com/articles/hashimotos-and-thyroid-antibodies/
HASHIMOTO’S AND THYROID ANTIBODIES: PART 2
https://thyroidpharmacist.com/articles/part-2-mechanisms-reduce-thyroid-antibodies/
I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It’s a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
COMPOUNDING PHARMACIES
https://thyroidpharmacist.com/database-recommended-compounding-pharmacies/
Hello Dr. Wentz,
Thank you for your expertise in this field. It’s sometimes difficult to find credible information and it takes hours and hours to sort through it all. I read your book. I found out that Geotrichum candidum is likely what contributed to my Hashimoto’s. It’s an overgrowth of a specific type of yeast. I did not see this specific strain of yeast mentioned in your book. Do you have experience treating others with this? Warmly, Bonnie
Bonnie – thank you for following my research! <3 I appreciate you sharing this. I don't have any specific information to share at this time on geotrichum candidum. I will add this to my research list. Please keep me posted on your progress.
Thank you, Dr. Wentz,
Any information you can provide would be so appreciated. I have tried western medicine and natural medicine including diflucan, oregano oil, cadicid forte, caprylic oil, grapefruit seed extract, olive leaf extract, undecenoic acid, Chinese skullcap, you name it. I get ovarian cysts rupturing if I eat anything that feeds it. It’s obvious that my thyroid, hormones, and adrenals are suffering. It’s difficult when you go from being healthy to then not having a normal human experience. I made some progress with a nutrient dense paleo diet but I still feel like I’m waiting. Waiting to get better all the way. If your research leads you to geotrichum candidum please please let me know.
Warmly,
Bonnie
I was wondering. I’ve read a lot of your work and was working on my health timeline. I got a CT scan with contrast at one point to check out a cyst. I felt awful after. Could that have been the iodine in the contrast? I have Hashimotos.
Gina – thank you for reaching out. <3 I'm so sorry you are not feeling well after this testing. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto's is a different mechanism. It's like pouring gas into an engine that's on fire... that's essentially what's happening in Hashi's, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let's fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books :
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hi Dr. Wentz,
Thank you for your work and contribution to all dealing with chronic diseases and especially thyroid issues.
I am 30 years old and my situation is very complex. I have severe CFS/ME, EDS, MCAS for 8 years now which has caused many problems: nutritonal deficiencies, neurological inflammation, and long standing gut issues/severe food intolerances, fatty liver from rice consumption and gallbladder sludge, heat intolerance, dry skin, eyes and mouth . I can only tolerate white rice and goitrogenic vegetables (bok choy and mustard greens asian variety). This is all I eat and have eaten for the past 5 years.
Now I have developed a mutinodular goiter and I have hypoechoic nodules. I believe I am severely Iodine deficient eating this way for so long and also selenium deficient, but everytime I try and take either I feel much worse, esp the iodine causing thyroid pain and enlargement. you said intolerance to selenium is usally a sign of iodine deficiency?
Iodine studies Random and 24 hr are severely low:
24 hr urine: 18 ug/24 hr(75-500)
Random urine: 15 ug/L (34-523)
But my Thyroid panel is within range, but have fluctuating TPO Ab:
Feb 2017–30 H (<9 IU/mL)
May 2018–24 (<35 IU/mL)
May 2019–17
Jly 2019–37 H (tried supplementing with Lugols 2% with very small drops on skin) I get severe diarrhea with any oral iodine.
Sep 2019–27
TG ab Negative all times tested concurently with tpo ab.
TSH:
2014: 0.85 uIU/mL (0.34-4.82 uIU/mL)
2016: 1.26
2017: 1.80
5/19: 1.54
7/19: 2.04
9/19: 2.80
FT4:
2014: 1.67 ng/dL (0.76-1.80 ng/dL)
2016: 1.25
5/19: 1.15
7/19 1.03
9/19: 1.02
FT3
5/19: 3.64 pg/mL (2.3-4.2 pg/mL)
7/19: 3.81
9/19: 3.71
DO MY LAB VALUES INDICATE POSSIBLE HASHIMOTOS TO YOU? PLEASE– MY PCP, ENDO, AND FUNCTIONAL MEDICINE DOC SAY ITS LOOKING WORSE, BUT DONT GIVE ME ANYTHING TO DO ABOUT IT EXCEPT WATCH AND WAIT TILL BIOPSY.
I am bedbound am miserable, please any input that could help steer me in the right direction. Should I be on thyroid hormone? My docs say no way with these labs.
Thank you.
Puddin – thank you so much for reaching out and sharing your journey with me. I am so sorry you are bedbound and struggling with all of this. My heart goes out to you. <3 Nodules and goiters are often the result of toxicity and/or the autoimmune process. So, doing interventions to reduce the autoimmune attack on the thyroid, and toxicity, can be helpful to reduce them.Conditions that I have found to respond really well to the Hashimoto’s protocols have been rheumatoid arthritis, lupus, Celiac disease, irritable bowel syndrome, eczema, asthma, Graves’, premature ovarian failure, psoriasis, Alopecia Areata, and Sjogrens. I have also seen the protocols help with Fibromyalgia, chronic fatigue syndrome, PCOS, as well as Type 2 diabetes, Crohn’s, and Ulcerative colitis.
A great place to start is with diet/nutrition: The diet I recommend for people with autoimmune conditions is the traditional Paleo diet which eliminates grains, dairy, soy, and processed foods and focuses on nutrient-dense foods like meats, vegetables, nuts, seeds, and eggs. It has helped a lot of people feel much better, and some have even been able to eliminate thyroid antibodies by following this diet.
Unfortunately, not everyone gets better on the Paleo diet. In some cases, we need to dig deeper. People may have additional sensitivities that contribute to the immune system dysfunction. People with Hashimoto’s are especially sensitive to a multitude of foods, especially gluten, dairy, soy, and eggs.
That’s where the Autoimmune Paleo (AIP) diet comes into play. This diet goes beyond Paleo and removes an additional couple of foods such as nuts, seeds, and eggs. AIP is the starting point - if you don’t remove the inflammatory foods, you can’t know if your other interventions are working or not. An elimination diet is the gold standard for determining the foods one is sensitive to.
Here are a few articles that hopefully help you get started:
THYROID NODULES
https://thyroidpharmacist.com/articles/hashimotos-and-thyroid-nodules/
TOP 10 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
IMPORTANCE OF GUT HEALTH
https://thyroidpharmacist.com/articles/importance-gut-health/
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
Unfortunately I made the bad decision to try a thyroid healing smoothie that had kelp and spirulina in it. Been having tremors and symptoms of hyperthyroidism. I’m guessing I launched an iodine attack on my thyroid:/
Gina – thank you so much for reaching out and sharing your journey. I am so sorry you are going through this! My heart goes out to you! <3 If you have been exposed to high doses of iodine, it may be helpful to take a selenium supplement, to negate the negative effects of the iodine excess. Here are some resources you might find helpful:
NUTRIENT DEFICIENCIES PART 1: SELENIUM
https://thyroidpharmacist.com/articles/nutrient-depletions-in-hashimotos-part-i-selenium
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Your comments are interesting and I appreciate them! I have tried numerous times to supplement with iodine in various forms and I never have success! I take zinc and selenium, the max dose recommended and have for years. I take L Setria glutathione and NAC. I have taken as low as 200mcg of iodine in the form of kale and still found myself feeling hypo thyroid. I know that iodine is important, but I have not found a way to get it without messing up my thyroid. Frustrating!
Anna – thank you so much for sharing your journey! I understand how frustrating this can all be. <3 I am very hesitant in recommending iodine in Hashimoto's. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto's is a different mechanism. It's like pouring gas into an engine that's on fire... that's essentially what's happening in Hashi's, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let's fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books :
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Food Pharmacology
https://www.amazon.com/Hashimotos-Food-Pharmacology-Nutrition-Protocols/dp/0062571591?tag=thyroipharma-20
Hello Dr Wentz, Thank you for all of your great research, You have helped me tremendously in my Hashimoto’s journey. Do you have any recommendations concerning having a CT scan where they will inject 80cc of iodine in me to be used as contrast? From my online research it looks like I should drink alot of water after the procedure but I am quite concerned about this massive amount of iodine. Thank you.
Pam – thank you so much for reaching out. <3 I understand how hard this is. Iodine excess has been recognized as a trigger to Hashimoto’s. This is true particularly in people who are genetically predisposed to Hashimoto’s and who may perhaps have certain vulnerabilities like a selenium deficiency. If you have been exposed to high doses of iodine, it may be helpful to take a selenium supplement. As always I recommend that you discuss this with your practitioner who's care you are under and see what protocols they suggest.
Here are come resources you may find helpful as well:
Selenium
https://thyroidpharmacist.com/articles/selenium-deficiency-and-hashimotos/
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hello Dr. Wentz, I’ve been taking a supplement marketed to improve hair health and energy levels which contains iodine derived from kelp (equivalent 275 mcg) and 10 mg Zinc on a daily basis. I have diagnosed hypothyroid but not hashi (although it runs in the family). Do you think a supplement like this is safe to take?
Alison – thank you for reaching out. I am very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books :
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hi Izabella,
My antibodies just came back as 50.9 and my iodine test showed I am deficient 48ng/ml. I am confused, do I avoid iodine or should I be taking it to raise my levels? Thank you
Justine – thank you for reaching out. <3 Most people with thyroid conditions are not deficient in iodine, and it’s important to note that excessive iodine intake can exacerbate Hashimoto’s. However, if your iodine levels are indeed low, I would recommend taking a multivitamin such as Nutrient 950 by Pure Encapsulations. A dose of up to 250 mcg of iodine per day (these levels are found in most multivitamins and prenatal vitamins) has been found to be helpful and beneficial in people with Hashimoto’s; however, doses above 300 mcg can be potentially inflammatory. I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine. My approach is, let's fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books :
Hashimoto’s Root Cause
https://amzn.to/2XXCqcQ
Hashimoto’s Protocol
https://amzn.to/3cJ89T4
I was diagnosed with Hashimoto’s thyroiditis two months ago, and since then, I have followed the guide in your book on a gluten-free diet and limited my iodine intake. In the last week test result, my TgAb and the TPOAb levels were almost no change about 220 U/ml, but my TSH level rose from 0.01 uIU/ml to 4.06 uIU/ml. In my case, should I increase iodine intake? Thanks.
Jinny – thank you for reaching out and sharing your journey. Please understand, I am not able to advise on whether adding iodine would be appropriate for you and your specific health needs without a comprehensive health assessment. I recommend that you discuss this with your personal doctor. I am very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books :
Hashimoto’s Root Cause
https://amzn.to/2XXCqcQ
Hashimoto’s Protocol
https://amzn.to/3cJ89T4
In 1986 I was 4yo kid living in Poland while the Chernobyl explosion happened. For 4 days there was no information about toxing cloud. After that everyone had to receive big doses of liquid called “Lugola” which was liquid iodine. I’m dealing with hypothyroidism for 7 years now. My sister has Hashimoto. Do you think those big doses of “Lugola” had any influence on our thyroid condition?
Thank you in advance, Isabella
Agata – thank you for reaching out and sharing your journey. <3 I grew up in Poland, in a small farming village on the southeast side of Poland, and was exposed to radiation from Chernobyl at age four. A 1997 study of children who were between age 0 and 7 at the time of the Chernobyl nuclear fallout and lived close to the Chernobyl nuclear reactor showed that 80% of them had thyroid antibodies, compared to 17% of genetically similar children who were farther away from the Chernobyl site. Here are a couple articles you might find intersting:
WHY WOMEN HAVE MORE THYROID DISORDERS
https://thyroidpharmacist.com/articles/women-thyroid-diso
THYROID NODULES
https://thyroidpharmacist.com/articles/hashimotos-and-thyroid-nodules/
Can you tell me more about taking coenzyme Q10 and HASHIMOTO?
I started taking it and things got worse, is it by that or maybe something else has caused the new situation?
Ellen – thank you for reaching out. I don’t currently have information to share on coenzyme Q10 an Hashimoto’s specifically but, I will add it to my list of possible future articles to research. Please understand, I am not able to advise on why you would have this experience using this supplement without a comprehensive health assessment. I recommend that you discuss this with your personal doctor.❤️
What salt has the least iodine?
Hi Kathy, I personally like Himalayan or celtic sea salt. ❤️
Hi Izabella, thanks so much for all you do. I’ve found your book and blog invaluable.
I have >1000 TPO antibodies and a TSH of 3.8. I have recently found out that I have an Iodine: Creatinine deficiency at 56 ug/g.
I have a creatinine urine of 0.41 g/l and iodine urine of 22.9 ug/l (which seem to be within range).
With that, would you recommend a low does iodine supplement of < 200mg? An adrenal saliva test has also come back normal in case that helps!
Thank you!
Harriet – you are very welcome! ❤️ A dose of up to 250 mcg of iodine per day has been found to be helpful and beneficial in people with Hashimoto’s. I do recommend discussing this further with your practitioner.
I am torn reading this. I was diagnosed with Hashimoto’s 3 years ago and have never been able to get my TPO into a range to know how high it is. All the testing here in Washington tops out at 1000, so all I know is it is over 1000 and has been for as long as I have known about it. All my other numbers have improved with meds, I take both T3 andT4 along with a handful of other supplements. When I started this, I was sure my body could heal itself if given the right tools. I may be wrong in that. I recently finished 4 months of peptide therapy with no changes so I build a near infrared sauna and am going to try that now. The protocol I was reading says to take Iodine, so I got some but decided to look into it first. Now I am torn. My goal is to not have to take thyroid meds for the rest of my life, but the cycle continues. For now, I will not take the Iodine.
Sebrina – thank you for sharing your journey! ❤️ I understand the struggle! I’m so proud of you for taking charge of your health and continuing to work on finding your root cause! I do suggest that you join one of the Hashimoto’s groups that are out there. Being able to share ideas of what has worked with one another and offer support for each other can be very helpful and please keep me posted on your progress.
We know that HT is a several risk factors disease. I would like to know if exposure to pollutants surrounding petrochemical complexes can trigger HT?
Carlos – thank you for reaching out. ❤️ Toxins and chemicals are established environmental triggers for developing Hashimoto’s in people who are genetically predisposed. These include iodine intake, bacterial and viral infections, hormonal imbalances, toxins, as well as therapy with certain types of medications and mercury! In people with Hashimoto’s, only 50% of their
identical twins presented with thyroid antibodies, meaning that genes alone are not everything and that environmental triggers are extremely important. Here are some articles which you may find interesting:
THYROID AND SKIN
https://thyroidpharmacist.com/articles/the-thyroid-and-skin/
MERCURY EXPOSURE AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/mercury-exposure-hashimotos/
FLUORIDE
https://thyroidpharmacist.com/articles/fluoride-and-your-thyroid/
Dear Mrs Wenz, I follow you for few years and have your book and trust your advice. Recently I have been to a functional doctor who has a good reputation and seems very knowledgeable. She advised, among other supplements to take Lugol 5% to address the Hashimoto hypothyroiditis and the high cholesterol levels (linked to the hypothyroid). Do you have any positive experince with this remedy? Many thanks.
Cristina – thank you for following. I’m so glad you are finding my research helpful and that you have found a practitioner.❤️ I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in both animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have an entire chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. For more info check out the article above!
This article helped me to realise why i was feeling bad taking high levels of kelp (and got high TSH readings). Happily, it also helped me to quickly and markedly improve my condition.
Rico – thank you so much for sharing! ❤️ I’m so glad to hear my researched helped! Please keep me posted on your progress.
Thank you for this detailed recap. However, I don’t see the WHO studies listed among the sources. Could you provide a link to them? Thanks a lot!
Angela – thank you for reaching out. ❤️ Please email my team at info@thyroidpharmacist.com and they will be happy to help you!
Dear Izabella, thank you so much for providing this valuable information! Years ago I tested slightly positive for thyroid antibodies, didn’t think much of it at that time, but I was still having ongoing candida symptoms. A while back I started taking Lugol’s iodine according to the megadose protocol. I did feel sceptical about it, since it is a man-made product. We would never be able to get this amount of iodine from food. But as you mentioned, in the beginning I felt amazing. My body temperature rised and the candida symptoms cleared up. Unfortunately I needed more and more iodine to get the same results and all the while my thyroid started to not feel right. I felt irritable and restless. My thyroid became swollen and felt kind of stiff. I found out this could mean it was under attack by antibodies. Also, the candida symptoms worsened. I found your article and that was really a gamechanger! I stopped taking iodine and I am now only taking selenium, vitamin C and probiotics. Fortunately this helped a lot, I feel calm and happy. My body temperature is still higher than before and the candida symptoms are vanishing. I cannot thank you enough for educating about Hashimoto’s. So grateful for having a sustainable solution and looking forward to a healthy future!
Nadine – thank you so much for sharing your journey! ❤️ I’m so glad you were able to figure out what was causing the issue and that you are feeling so much better! I do hope you will continue to keep me posted on your progress.
Hi Dr. Wentz! I had been consuming dulse for around 2 months. I gradually went from 1/2 tsp. to 2 tablespoons a day, and was feeling pretty well. (Approximately 850 mcg iodine) Around the 2 month mark I started having terrible hormonal symptoms, heavier period, a lot more clotting, nausea, anxiety, blood sugar issues. I am praying I have not destroyed my thyroid! Do you think there is a chance this will clear itself up by removing the iodine sources in my diet? I stopped the dulse immediately once the symptoms started. I am limited on the supplements I can take due to sensitivities, but I do eat a whole food plant based diet. Thank you for this article! Wish I would have read it before consuming so much dulse.
Brooke – thank you for reaching out and sharing. ❤️ I recommend discussing this with you practitioner who is familiar with you health history. I am very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies. I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. You can find more information in my book and in the article above!
Any input on how to treat Hashimoto’s brought on by COVID?
Holly – thank you for reaching out.❤️ Everyone is different, we do know that viruses in general, can definitely trigger Hashimoto’s. Here are a couple articles you might find helpful:
VIRUSES
https://thyroidpharmacist.com/articles/viruses-may-trigger-hashimotos/
WHERE DO I START WITH HASHIMOTO’S?
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
I have Hashimoto and I’m on a Paleo diet for over a year, I had my selenium levels tested, my iodine tested, my Vit. D tested, Vit B tested & I had my Mercury levels tested. My iodine levels (Urine creatinine test) are extremely low, my Selenium levels are at high toxic levels & my Vit. D, also at high toxic levels. Vit B very high too. Mercury is normal. I’ve since stopped taking selenium and Vit. D, and only take Vit B once a week. I just don’t know what to do concerning my iodine as my levels are 34 mcg and apparently the range should be 75-500mcg.
Rachel – thank you for following. Most people with thyroid conditions are not deficient in iodine, and it’s important to note that excessive iodine intake can exacerbate Hashimoto’s. However, if your iodine levels are indeed low, I would recommend taking a multivitamin such as Nutrient 950 by Pure Encapsulations. A dose of up to 250 mcg of iodine per day (these levels are found in most multivitamins and prenatal vitamins) has been found to be helpful and beneficial in people with Hashimoto’s; however, doses above 300 mcg can be potentially inflammatory. I also recommend discussing your test results with your practitioner who is familiar with your health history to help you decide the best options for you. ❤️
Hello! I’m really in need of some advice. Male, 32. I’ve been noticing that I react very badly to high-iodine foods, such as seaweed, sea products and fish on a daily basis. Even if I get around 150 mcg a day from food, it seems too much, and I get hypothyroid symptoms – fatigue, cold, slow digestion, dry skin, numb extremities, mood swings, bad reactions to goitrogens. Eating 1-2 Brazil nuts for selenium helps a bit but not much. As I recall, I didn’t get too much iodine while growing up as I didn’t like fish, very rarely ate seaweed and we didn’t use iodized salt. I would get some fish maybe once or twice a week, eggs and dairy here and there. However, I was pretty healthy, smart and active, so no development issues at all. My thyroid was pretty small on ultrasounds, around 12 cm3.
Can it be assumed that a person’s iodine needs will be dependent on their intake as adolescents? So if the thyroid is used to get little iodine, it doesn’t require that much for an adult to function correctly? Thanks!
Vitticus – thank you for following. I am very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies. I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here is an article you might find interesting:
IODINE AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/iodine-hashimotos/
Dear Dr ª Izabella,
I have hashimoto and i feel better on a vegetarian diet.
I eat eggs and cheese, except milk, yogurt, ice cream etc.
Which is the best source of iodine except sea salt fortified with it?
I normally use pink himalayan salt, but that has no iodine correct?
I have read sea salt has nano particles.
I also read that you say, that white bread has iodine, does gluten free bread contain any iodine?
I would like to keep a lower intake of iodine of at least 150 mcg.
What is your opinion on cranberries?
I don’t want to use any supplements for iodine
Please recommend me a healthy way to achieve my iodine needs without supplements on a vegetarian diet like i described above.
Kind Regards,
Rui – thank you for reaching out. I am very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies. I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. If your iodine levels are indeed low, I would generally recommend taking a multivitamin such as Nutrient 950 by Pure Encapsulations. A dose of up to 250 mcg of iodine per day (these levels are found in most multivitamins and prenatal vitamins) has been found to be helpful and beneficial in people with Hashimoto’s; however, doses above 300 mcg can be potentially inflammatory. Hope that helps
I have caused my thyroid to swell up after taking Lugol’s for several weeks. I was taking on average two drops a day. Plus, I was getting a little extra iodine from a mineral supplement. My thyroid has swollen to the point of being uncomfortable. It seems to ebb and flow throughout the days. I have stopped all iodine supplements and have started taking selenium and myo-inositol in hopes that this swelling will go down. Have you seen this happen before from iodine supplementation ? Have you seen the swelling go down in time?
Thanks
Mike – thank you for reaching out. I’m so sorry you had this experience. I do recommend checking in with your practitioner. When it comes to Iodine supplementation, I am very hesitant in recommending it in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire.
Dear dr. Wentz,
Your work on thyroid disease has been tremendous, thank you.
Regarding iodine, I am a male, 40.
I have been diagnosed with subclinical hypothyroidism and positive TPOab 10 years ago, with a TSH bouncing around between 3 and 7 throughout the decade.
But like many other people I have not been taken quite seriously by doctors who do not seem to know much about what causes this.
I have read studies showing how Iodine intake has declined in the European population (where I am from) and according to a study in the Lancet 60% of people in Europe live in countries that harbour Iodine deficiency.
https://www.thelancet.com/journals/lancet/article/PIIS0140-67360312935-2/fulltext#:~:text=Overall%2C%20more%20than%2060%25%20of,countries%20that%20harbour%20iodine%20deficiency.&text=West%20and%20Central%20Europe%20assesses%20its%20iodine%20nutrition.
Since I eat gluten free for my celiac disease, I do not eat Iodised bread or Iodised pasta.
I ran my average diet through a food tracking app, and despite eating yoghurt and eggs my dietary intake came out to be low intake of Iodine.
I have been taking a kelp supplement of 400mcg for about 6 weeks and selenium, and I do notice a few bodily symptoms have improved.
Still I feel a bit between a rock and a hard place, Iodine can aggravate Hashimoto and elevate TSH, but having an Iodine deficiency is also detrimental for the thyroid, and all other body systems that need Iodine.
I just wished doctors would be more helpful and educated on the issue.
Rob – thank you so much for sharing your experience. I’m so glad you are seeing some improvements. Doses of up to 250 mcg of iodine per day such as those found in most multivitamins and prenatals have been found to be helpful and beneficial in people with Hashimoto’s; however, doses above 300 mcg can be potentially inflammatory.
Hi, thanks for the article! I don’t have any problems with my thyroid, the doctor checked years ago. But my body has difficulty regulating temperatures and I have a lot of fatigue. I also have/had lyme disease, psychosomatic symptoms and lactose and histamine intolerances. So my doctor suggested I take spirulina to support my thyroid. Only I started to get a really sore throat. It lasted a few weeks and then disappeared. But now I stopped taking it for a week and the sore throat is back already for a couple of days. I can’t find on the internet why I have this and what it means. My doctor also didn’t know what was going on. She thought because of my sensitivities I could feel it working for my thyroid. But now it’s back when I stop taking it I’m confused if I should take it or not. Because both options give me pain. Do you have any idea what’s happening? The pain started at a dosage of 500mg and I was taking 1500mg before I stopped. Kind regards, Terry
Terry – thank you for reaching out and sharing your journey. I’m so sorry you are struggling with this pain. For some, spirulina can increase the autoimmune response as it has some immune modulating properties. Additionally, the iodine is problematic and can cause further thyroid damage.
Wow! This article was extremely informative! I have had Hashimotos (known diagnosis) for 10 years, although I have been on Synthroid (75mcg) for 20. Recently I have been diagnosed with osteoporosis at 66. I went to a functional doctor and he gave me this supplement that has 153mcg of iodine. I saw red flags, (unfortunately it was an expensive supplement and now I am stuck with it). After reading this article, I see that I am already getting plenty of iodine through my diet. I do eat a few brazil nuts a day, but also yogurt daily and I love shell fish. I will proceed with caution with bone supplements. Thank you for the article!
Jane – thank you so much for sharing! So glad to hear you are taking charge of your health and finding my resources helpful.
Hi Izabella
I have been diagnosed with subclinical hypothyroidism with elevated Hashimotos Antibodies present. This article confuses me a little as I think I am in the minority. I have slightly elevated selenium levels and severely deficient levels of Urine Iodine being 15 ug/L. Should I take a supplement or just add iodised salt? I eat seafood/fish pretty much daily so am surprised by my results…
Rebecca – thank you for reaching out. This is something I recommend you discuss with your practitioner to help you determine what is the best option for you and your health condition.
Hi Dr. Wentz,
What are your thoughts on iodine for Hashimoto’s patients who are trying to conceive? It seems that most prenatal vitamins contain iodine and since most OB/GYNs aren’t well versed in thyroid conditions, it’s difficult to know whether the iodine in prenatals is beneficial, neutral, or harmful for Hashimoto’s patients when trying to conceive. I know you can’t provide specific medical advice, but would appreciate your thoughts generally on iodine supplementation when trying to conceive or whether Hashimoto’s patients should try to find prenatals without iodine. Thanks!
Stacy, Thank you for reaching out. Small doses are generally safe (amounts in prenatal vitamins and multivitamins), but above 400 mcg can be inflammatory.
Can you share how much iodine is recommended post half thyroid surgery removal? Thanks!
Joan – thank you for following. Generally no more than what’s in a multivitamin.
Dear Dr. Izabella,
I am a 55-year-old man with Hashimoto’s, but my thyroid is still functioning. I am currently trying to reduce my antibodies and have lowered my intake of dairy and gluten. I’ve also started taking supplements including Vitamin D3, Magnesium, Zinc, Selenium, and Omega-3.
I noticed that the Wellman Multivitamin contains most of these, but it also includes 150 micrograms of iodine. Is it safe to take, considering that my only consistent source of iodine is from two eggs daily, with no other major iodine-rich foods in my diet?
Thank you for your advice.
Thank you so much for reaching out and sharing your journey. It’s wonderful to hear that you’re being proactive about supporting your thyroid health by reducing gluten and dairy and incorporating key nutrients. When it comes to iodine, people with Hashimoto’s often have varying responses. Some may benefit from small amounts, while others may find that even low doses can increase thyroid antibodies or trigger symptoms. The iodine content in your multivitamin 150 micrograms, is considered within the RDA for adults (150 mcg/day), and your current dietary intake from eggs sounds modest.
That said, iodine needs can be highly individualized, especially in the context of Hashimoto’s. Some people do best avoiding supplemental iodine altogether unless they have a documented deficiency. Others may tolerate small amounts when selenium levels are optimized, so it’s great that you’re already including selenium in your supplement routine, as adequate selenium may help support thyroid health and modulate the body’s response to iodine.
Ultimately, I recommend working with your practitioner to monitor your thyroid function and antibody levels regularly while introducing any new supplements. This way, you can ensure that your regimen continues to support your health goals in a personalized and safe way.
Dear izabella.
Here you say that:
Bread (2 pieces) = 90 mcg of iodine
Is this bread made with iodized salt or no?
How much iodine contains bread with normal sea salt (without iodine).
Thank you!
Hi Manuel, Great question! The estimate of 90 mcg of iodine for two slices of bread is based on bread made with iodized salt, which is commonly used in commercial baking in some countries. If the bread is made with non-iodized salt, such as natural sea salt or Himalayan pink salt, the iodine content would likely be much lower. It’s always a good idea to check with the manufacturer when possible, especially if you’re aiming to follow a low-iodine diet for thyroid health.
Dr Wentz, your work is very informative. Thank you for your insights. As a hashimoto’s sufferer myself, I’ve had confusion over iodine as well. I was wondering if you are familiar with Dr David Brownstein and his research. He is an iodine advocate. His research citing the benefits of high dose iodine seems to be in contradiction with your research. How do we navigate through these conflicting sets of information?
Thank you
Ahmet, Thank you so much for your kind words and for sharing your experience. I completely understand the confusion surrounding iodine, it’s one of the most debated topics in thyroid health! While iodine is indeed essential for thyroid hormone production and can be very beneficial in cases of iodine deficiency related hypothyroidism, Hashimoto’s operates through a different mechanism. In those of us with autoimmune thyroid conditions, adding iodine too soon can sometimes make things worse rather than better.
I often compare it to pouring gasoline on an engine that’s already on fire, the thyroid is inflamed, and adding more fuel (iodine) before addressing the inflammation can potentially accelerate damage. This pattern has been observed repeatedly in both human and animal studies, especially in individuals predisposed to autoimmunity. I’ve spent several years researching this issue and have seen many people experience setbacks after introducing high-dose iodine without first addressing underlying triggers, often related to gut health, nutrient deficiencies, or immune system imbalances. My approach is to focus on calming the immune system and supporting the body’s natural healing processes before reintroducing iodine, if appropriate. I do have a full chapter dedicated to the iodine controversy in my books, where I discuss this topic in more depth and reference the work of Dr. Brownstein alongside other research studies. Here are links so that you can check out my books:
Hashimoto’s Root Cause
https://amzn.to/2XXCqcQ
Hashimoto’s Protocol
https://amzn.to/3cJ89T4
I’ve had Hashimoto’s for decades, and been stable on my dosage of synthroid for many years. Pretty sure at this point my thyroid is dead. Ultrasound shows it as “small.” I’ve also developed Parkinsons and have mild symptoms. I’ve read that sea moss may be helpful protecting the brain from Parkinsons, but it’s also hihgh in iodine. Is it likely to inflame the thyroid now?
Hello, Thank you for sharing your story. I generally don’t recommend it for people with Hashimoto’s but if this is something you’re interested in please work with your practitioner to ensure your iodine levels remain stable. There are also other, more thyroid-friendly ways to support brain health and reduce inflammation (like optimizing omega-3s, vitamin D, antioxidants, and gut health), which are part of my root-cause approach. Please always be sure to discuss any new supplement with your doctor, especially with Parkinson’s and thyroid meds on board.