Depression is a topic near and dear to my heart.
Many moons ago, I lost a loved one to suicide… and while I’ll never understand the immense pain of a person in the moment before they choose to end their life, I can tell you that the loss leaves families and survivors (like me), in utter devastation and despair. Some even spiral into a deep depression from the trauma.
I was one of them.
Losing my loved one created the type of hole in my heart that I hope others never have to experience, and was likely a factor in the development or exacerbation of my autoimmune condition.
I personally battled with depression before my Hashimoto’s diagnosis. I had worked and interned in various mental health settings as a pharmacy student for about 10 years, with the goal of specializing in psychopharmacology, before realizing that I had Hashimoto’s — and that perhaps there was more to treating mood disorders than a prescription pad.
In my experience with my thyroid clients with depression, we’ve had about an 80 percent success rate using the very strategies I share below.
For the last decade, depression has become a distant memory for me. On most days, I feel calm, happy, and empowered, and sometimes forget how it feels to not be in a great mood every day.
The past few years have been so hard on many of us, including me, and I wanted to share this article with you, with the hope that it will offer you some new information to help you cope if you are struggling with depression. I’ve noticed that since 2020, many of us need to do EXTRA to support our mental health.
I share this information with you, and I hope that you will benefit from it and also share it with someone you care about who may need it. How I wish I knew then what I know now. It breaks my heart that some of the kindest and most amazing people I used to know are no longer around to enjoy the beauty of this world, and that others are not living their lives due to the dark cloud of depression hovering over their heads.
If you’re reading this, please know this: often depression can be resolved when an underlying thyroid issue is addressed.
While there are reasons for depression beyond thyroid health, because it’s Thyroid Awareness Month, and because I am the Thyroid Pharmacist, I would love to share the connection between thyroid issues and depression in my little corner of the internet.
Some people struggle for years without a proper diagnosis of thyroid disease — and even worse, many of those with a proper thyroid diagnosis don’t receive the right treatment and continue to have depression. It breaks my heart to think about the many thyroid patients who get labeled as clinically depressed instead of being tested for thyroid antibodies, and to think of the patients who start on thyroid hormones without consideration of dosage and form, resulting in ongoing symptoms, including depression.
The good news is that, once a diagnosis of Hashimoto’s (or thyroid disease) has been made, we can start looking for and addressing the root causes that might be leading to feelings of depression, including optimizing thyroid hormones. This article focuses on some of the low-hanging fruits that can help many people with depression feel better.
In this article, you’ll learn about:
- The connection between Hashimoto’s and depression
- Root causes of depression
- Strategies and solutions for depression that can help some 80 percent of people feel better
Depression and Hashimoto’s: What’s the Link?
Clinical depression, or major depression, is a mental health disorder characterized by persistently depressed mood or loss of interest in activities, causing significant impairment in daily life. Symptoms and severity can vary from person to person. It is estimated that some 21 million adults (8.4 percent) in the U.S. have experienced major depression at least once, and the prevalence is greatest in women and young adults. (1)
It might surprise you to discover that Hashimoto’s (and other thyroid disorders) and depression often co-occur — most people are unaware of how frequently this happens. A 2018 review paper found that “the chance of developing symptoms of depression that were of clinical relevance is 3.3 times higher among patients with hypothyroidism compared with healthy controls.” (2)
In Hashimoto’s, there is a breakdown of the thyroid gland, which can rush thyroid hormones into the bloodstream, resulting in transient hyperthyroidism. This can result in symptoms such as agitation, anxiety, and even psychosis. Anyone who has experienced symptoms of hyperthyroidism (due to the fluctuations in thyroid hormone often seen in Hashimoto’s) can describe how terrible this feels. (3)
Once the thyroid hormone is cleared out, the person may be functionally hypothyroid, which is linked with symptoms of depression, such as apathy, low mood, fatigue, and brain fog.
Thus, it’s possible that some cases of depression are related to the thyroid. (4) In fact, one reader with thyroid disease told me, “I feel like I’m sitting on the sidelines of life, watching everyone else enjoy their journey, wondering if I’ll ever have my zest for life back.”
If you are feeling alone and like no one believes you, please know that you are not alone, and it’s not in your head! I suggest reading this article about what it feels like to have Hashimoto’s to understand that many people struggle with feelings of depression and more, and it can take a while to get a proper diagnosis.
A study in 2004 found an association between the presence of a mood disorder, and the presence of thyroid peroxidase (TPO) antibodies. (5) Other research has connected depression, distress, obsessive-compulsive symptoms, and anxiety, with high levels of TPO antibodies. (2,6) TPO antibodies are early signs of an autoimmune attack on the thyroid, even when one’s TSH (thyroid stimulating hormone) number is still in a range that is considered normal.
In my experience, appropriate identification and treatment of a thyroid condition can resolve symptoms of depression. I’ve also seen plenty of instances where people have enjoyed well-deserved levels of health and happiness after addressing the underlying root causes and consequences of thyroid disease.
Conventional Treatments for Depression
Research supports the link between mood disorders and Hashimoto’s. For example, people with bipolar disorder (as well as depressive and anxiety disorders) were found to have a higher prevalence of antithyroid antibodies. (To further complicate the issue, prescription lithium, a medication often used for bipolar disorder, can actually trigger Hashimoto’s. However, nutritional lithium, which is an extremely low dose compared to prescription medication, may offer some mood benefits with lower risks. I encourage you to read more about that in the linked article.)
Doctors who are aware of the link between thyroid issues and mood disorders will take a deeper look at the role of thyroid disease and may consider thyroid medications in those presenting with symptoms. Likewise, progressive psychiatrists will test all of their patients who present with new-onset depression, anxiety, and mental health symptoms for thyroid disorders, and will often be open-minded about prescribing thyroid medication.
Unfortunately, despite all of the research that’s out there, these types of psychiatrists are a minority, and sometimes people are misdiagnosed (and even hospitalized) with conditions like bipolar disorder or schizophrenia when, in fact, they had thyroid imbalances.
In the majority of cases, conventional doctors favor the use of antidepressants (or a referral to a psychiatrist)! “Antidepressant” is a common name for the type of medication used to treat depression. (For a lot of people, Prozac comes to mind, though not all of the medications work on the same pathways as Prozac.)
That said, the most common antidepressants are SSRIs (selective serotonin reuptake inhibitors). These include brand names such as Zoloft, Prozac, Celexa, and Paxil. These drugs work by decreasing serotonin (our “happy hormone”) reuptake (reabsorption) in the brain, which leaves more serotonin available in the brain to positively affect mood. Common side effects of SSRIs include nausea, sexual dysfunction, insomnia, nervousness, and tremors.
Another commonly prescribed group of antidepressants is called SNRIs (serotonin and norepinephrine reuptake inhibitors). Cymbalta, Effexor XR, and Pristq all fall into this category of drugs that work by improving serotonin and norepinephrine (a neurotransmitter and hormone in the nervous system) levels in the brain. Common side effects include nausea, drowsiness, fatigue, constipation, and dry mouth.
Wellbutrin (bupropion) is another medication that has a few different indications. Most commonly, it’s used as an antidepressant that works on the norepinephrine and dopamine pathway and may be given as a stand-alone medication, or in combination with SSRIs to counteract the sexual side effects and fatigue caused by SSRIs. This medication is also FDA-approved for smoking cessation. (I’ve written about the connection between smoking and Hashimoto’s before, and I personally took bupropion in college for the purposes of smoking cessation.) This medication may also help with weight loss, focus, and energy. However, it can also lead to a suppression of TSH, the communication hormone that tells our body to make more thyroid hormone — potentially resulting in what is known as “central hypothyroidism,” where the TSH is normal but the actual thyroid hormones (T3 and T4) are low because the communication pathway isn’t working properly. (7,8)
I took this medication in college around the time I started having thyroid symptoms, and I remember that I felt more focused and energetic when I took it. I often wonder if this medication either masked some of my symptoms, contributed to my thyroid hormones being low, or potentially led to a suppression of TSH, masking the fact that I was hypothyroid whenever I was checked. This is why I often recommend doing a full thyroid panel to screen for thyroid conditions, and why depression is a big red flag for me when it comes to thyroid conditions.
Additionally, medications that were once traditionally used for treating schizophrenia are now used as “add-on” therapies for treatment-resistant depression. In the real world, as a consulting pharmacist, I saw a lot of heavy-duty use of these medications, and in some cases, this led to debilitating side effects (fainting, lethargy, loss of balance, sexual side effects, and metabolic syndrome, with some individuals earning over 100 pounds in the course of a year or two after initiating these medications).
Do Antidepressants Help with Depression?
When I hear people in natural medicine speaking about the evils of antidepressants, I think of my deceased loved one… oh, how I wish he had considered antidepressants, instead of taking his life. While it’s true that most mood-altering medications do have some unfavorable side effects, they can help some people feel better, and can save lives.
At the end of the day, as someone who wants to alleviate the world of suffering, I am supportive of most methods people use to heal.
As someone who has dispensed antidepressants, taken antidepressants, and monitored patients who were initiated on antidepressants, I can tell you firsthand that they do work really well for some people. I have had patients come to my pharmacy in deep despair, clutching onto their first prescription for an antidepressant — I sometimes would just listen to my patients for hours, on the phone in the late evenings when the pharmacy was quiet, and would see them feeling better and better every month they would come in to get their refills, often with a spark of hope in place of the dark shadow they carried at our first meeting.
That said, antidepressants don’t work for everyone. A major study completed in 2006, the STAR*D trial, showed that around 30 percent of people were “responders” to most antidepressants. Additionally, the STAR*D trial found that less than five percent of people were found to be in remission from depression with SSRI drugs, even after using them for a year. (9)
(Please note that if you are currently taking prescription antidepressants, it is important not to stop taking your medications without the oversight of your physician or therapist.)
Side Effects
Additionally, as I alluded to earlier, side effects are common with mood-altering drugs.
While I believe most medications have their time and place, the truth is, most mood-altering drugs are “dirty drugs” (this is official pharmacist lingo, lol). They interact with many receptors, leading to a long list of symptoms.
As a pharmacist, I often got reports from my patients and clients of feeling like zombies, gaining weight, having “dulled” feelings, living in a fog, having sexual dysfunction, becoming manic, and feeling worse on antidepressants and other mood-altering medications.
Suicidality
One of the scariest side effects of antidepressants that I learned about in pharmacy school is increased suicidality. We were taught that some people who were prescribed medications for depression could be more likely to die by suicide within weeks of starting them. The theory proposed to us students was that “people got more energy before their mood improved… and thus, this burst of energy gave them the opportunity to take their lives.”
Increased suicidality is a possible effect of antidepressants for a few reasons. For instance, it can happen if the drug is just not the right fit for the person, if a person is prescribed the wrong type or dose of medications, or if there are cofactors such as alcohol abuse present. It can’t always be predicted because different drugs work differently for each individual. That’s why, when these drugs are prescribed for the first time, a practitioner should carefully monitor the patient, and will often start with a lower dose, then increase it once no negative symptoms are reported.
In any case, this possibility of suicide was so scary to me as a young practicing pharmacist.
Suicide is a permanent solution for a temporary problem, and is devastating for loved ones of the deceased, who often go on to have post-traumatic stress disorder, survivor’s guilt, and even new onset autoimmune disease. (One day I’ll write more about my personal connection to loss… but for now, if you’re reading this and struggling with depression, I want you to know that you can feel better — and there are so many people and things that can help you. Don’t give up.)
Drug Dependence
Antidepressants can also cause a downregulation of our internal production of neurotransmitters. This means that people can become dependent on taking them and have withdrawal symptoms when they try to come off of them.
When I was a consulting pharmacist, I saw this firsthand, and have worked with monitoring numerous people to help them slowly wean off antidepressants.
This dependence occurs because antidepressants prevent us from properly clearing serotonin from our brains, causing it to stick around longer. Unfortunately, the body takes notice of all of this serotonin hanging around. Soon, we begin to produce less serotonin, and we become less sensitive to the serotonin we do have. When not addressed, this result may become permanent.
Beyond antidepressants, I’ve seen other mood-altering drugs being used for refractory depression (depression that doesn’t respond to medication treatment), some “off-label,” others with FDA approval.
For example, some of the “dirtiest” drugs out there include antipsychotic medications like Seroquel, Risperdal, and in particular Zyprexa. They have been traditionally used for schizophrenia, but are now being used for depression as well. I’ve seen people gain hundreds of pounds in the course of a year, become diabetic, lethargic, and withdrawn, and develop irreversible, involuntary movements and painful muscle contractions, from using antipsychotic medications.
From 2008 to 2011, the majority of my recommendations as a consultant pharmacist were to reduce or taper antipsychotic medications for clients due to the horrible side effects and lack of perceived benefit. From 2012 onwards, one of the key deliverables of my job was to help reduce the use of antipsychotic medications in the elderly.
Furthermore, I think it’s important to understand the root cause of the problem. For example, giving a person mood-stabilizing medications because of fluctuations in mood (due to Hashimoto’s), is like putting masking tape over the “check engine” light in a car, instead of checking the engine.
Antidepressants alone should never be the sole solution, even for a person with severe depression and anxiety. If you are someone who is taking antidepressants, root cause solutions can help you get the most benefit from them, and can even help you wean off of them (under your doctor’s supervision).
As a pharmacist, I really got a kick out of this article from the satirical news publication The Onion:

Let’s dive in and discuss some of the root causes of depression (including, but not limited to thyroid issues), as well as some solutions beyond medications.
The Root Cause Approach
I remember speaking to one of my young clients who was living in a mental health group home, about his goals, in my past job as a consultant pharmacist. He mentioned that he had hoped to be free of psychiatric medications, yet because of his diagnosis, I was so sad that our team of healthcare professionals would have to tell him that he would not meet his goal, and that he needed to choose a more “realistic” goal. In conventional medicine, medications are often life-long. Thankfully, I now know that psychiatric medications are not a life sentence.
The amazing thing that I’ve learned with functional medicine is that many people with lifelong psychiatric diagnoses can recover after receiving proper thyroid care. This is because many of the same root causes, triggers, and strategies that help Hashimoto’s, can also help depression (when the root cause of depression or a mood disorder is due to the thyroid). In fact, 81 percent of the participants in my Hashimoto’s Self-Management Program reported an improvement or resolution of depression!
One reader shared how liberating and transformational it was to realize the depression was related to their Hashimoto’s:
“One year ago, I was feeling anxious, depressed, and like I was going crazy! I was sent to a psychiatrist and prescribed Seroquel [an antipsychotic medication] and clonazepam [an anxiety medication]. 5 months later, I read your blog and went to my primary care doctor and demanded testing for Hashimoto’s. I wasn’t going crazy, I had TPO Antibodies well into the 600 range. I am being weaned off of the psychiatric meds and I immediately changed doctors. Thank you, Dr. Wentz, or I would still be spending thousands on a psychiatrist. And my TPO is slowly coming down.”
While there are many different root causes, strategies, and solutions for depression, I want to focus on a few low-hanging fruits that can help a person with depression, whether used in conjunction with antidepressants, or on their own. Many of these can be DIY options, as well as approached with the help of your primary care doctor.
These include:
- Optimizing thyroid hormones
- Making dietary changes
- Addressing nutrient deficiencies
- Utilizing supplements that have been shown to improve mood and stress
- Implementing mood-boosting lifestyle changes
Thyroid Hormone Optimization
First and foremost, if your TSH is elevated, you may need to consider thyroid hormone medications.
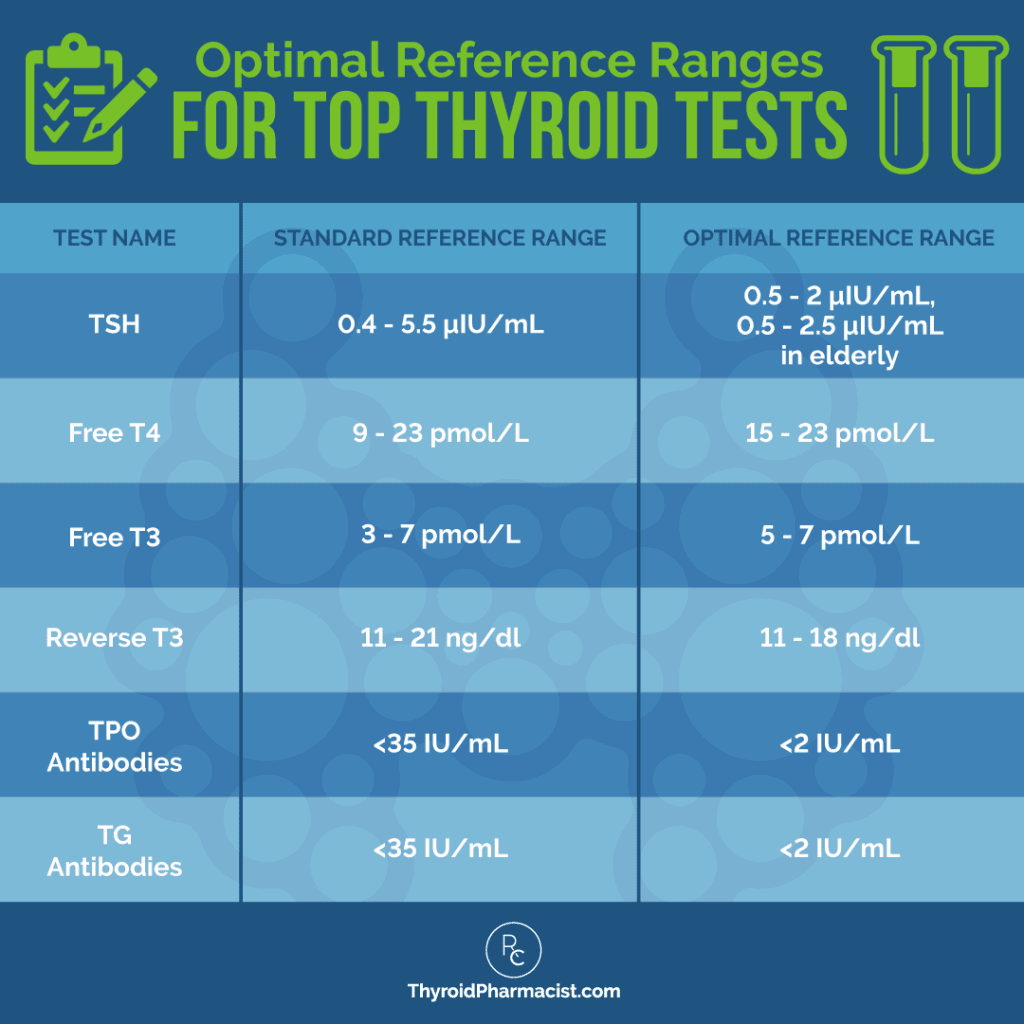
If you’re already on thyroid medications, you may need to adjust your current dosage to optimize your TSH levels. A survey of over 2000 Root Cause readers found that as far as medications and mood, getting TSH levels between 1 and 2 μIU/mL, and in some cases, under 1 μIU/mL, helped a person improve their mood symptoms. (Levels that are too high or too low indicate an imbalance of thyroid hormone levels and have been associated with various symptoms, including depression and anxiety.)
However, it’s important to note that some people continue to have these symptoms despite taking medications like Synthroid, levothyroxine, or Levoxyl. Not everyone can be optimized on a T4 medication alone.
One of the biggest signs that a person with thyroid disease is not converting T4 to the active T3 properly, is depression.
Additionally, medical studies have shown that 25 percent of people who do not see improvements with antidepressants, report feeling better once they were started on Cytomel® (a T3-containing thyroid hormone). (9)
If you are still having symptoms of depression while on your thyroid medications, consider talking to your doctor about switching your medications.
Taking a T3-containing medication, in particular, has been shown to reduce symptoms of depression. Around 60 percent of readers whom I surveyed, reported an improved mood after switching to a T3/T4 combo medication like Nature-Throid, WP Thyroid, Armour, or a compounded T4/T3 version.
You may want to read my articles on understanding your thyroid labs and taking thyroid medications for more information on how adjusting thyroid medication dosages or switching medications can help optimize your thyroid hormone levels and elevate your mood.
Dietary Changes
I have found that for some people with Hashimoto’s, their depression may in fact be a sensitivity reaction to food(s).
Some of the most common food sensitivities that can lead to symptoms of depression are gluten, dairy, grains, soy, nuts, and seeds. Eliminating these foods from one’s diet can bring enormous relief to a person’s mood and mental state. In fact, in my survey of readers with Hashimoto’s, 60 percent of people reported symptoms of improved mood by eliminating gluten, 59 percent saw improvements by going grain-free, and 45 percent by giving up dairy. I recommend starting with an elimination diet to begin to uncover the foods that are problematic for you.
Additionally, balancing blood sugar levels is one of the most important components in reducing anxiety for people with Hashimoto’s, and can have an impact on symptoms of depression as well. When insulin levels swing from high to low, it’s like being on an emotional rollercoaster that can cause some of the extreme emotions that are characteristic of mood disorders. Of the people with Hashimoto’s that I surveyed, 61 percent reported improved mood with a low glycemic index diet, while 65 percent experienced improvement on a sugar-free diet.
Nutrients for Depression
Addressing nutrient depletions can be a game changer when it comes to relieving depression. Oftentimes, a deficiency in a key nutrient results in many of the symptoms associated with depression, and supplementing with a quality supplement can make all the difference in improving mood.
Nutrient depletions that are often seen in people experiencing symptoms of depression include:
- Vitamin B6: Depression can be caused by something so simple as a deficiency in B6, and a recent study showed that high-dose vitamin B6 supplementation reduced anxiety and depression. (10) B6 is required for the production of neurotransmitters, and unlike antidepressants that artificially raise the levels of neurotransmitters, B6 has very few side effects. One clue that you may be deficient in B6 is poor dream recall. I generally recommend a dose of 50 to 100 mg. The pyridoxine form can also be used; however, doses above 300 mg should be avoided due to the potential of induced peripheral neuropathy. I’m excited to share that I’ve added P5P to the Rootcology portfolio, and that Pure Encapsulations also offers P5P. The P5P version of B6 can help to promote serotonin production, leading to a more positive mental outlook, better gut health, and an improved response to stress. (As a bonus, it can also help with gut health, blood sugar balance, and menstrual symptoms like water retention.)
- Vitamin B12: A deficiency in B vitamins, particularly B12, can have a huge impact on mental health. One study found that one quarter of women who were diagnosed with severe depression were deficient in this crucial nutrient. Of the readers with Hashimoto’s that I surveyed, 56 percent experienced an improved mood when they began supplementing with B12. (11,12)
- Methylfolate: Studies have shown that people with low levels of folate have a 7 percent response rate to treatment with antidepressants, while those with high levels of folate have a 44 percent response rate; therefore, it is often used in the treatment of depression. You can take methylfolate as a standalone supplement, or as part of a combination product like MTHFR Pathways. (13)
- Iron (ferritin): Several symptoms of iron deficiency are similar to that of depression: fatigue, irritability, and brain fog. I personally became iron deficient while pregnant, and felt like I became tearful and emotional overnight… These symptoms are usually considered “normal” for pregnant women, yet iron deficiency is the most common deficiency in pregnancy. I was already taking an oral iron supplement, but ended up needing to supplement with two burgers a day, and iron IVs, to stay happy. One day I told my husband that I didn’t feel loved because he hadn’t gotten burgers for me that day. 🙂 Testing iron and ferritin levels is incredibly important, and proper management may bring relief to symptoms of depression for many people. (As a side note, iron deficiency is more common in pregnant and menstruating women, while iron overload is more common in men and postmenopausal women. An overload of iron can also lead to mood alterations, so be sure to get tested and not just supplement.) (14,15)
- Omega-3: A number of studies show that omega-3 fatty acids can be effective against the treatment of major depressive disorder and other psychiatric disorders, with no associated side effects. I generally advise 1 to 4 grams per day for most people. (16)
- Vitamin D: Most people, especially those of us living further away from the equator, are deficient in vitamin D, and a deficiency in this important nutrient has been linked to elevated thyroid antibodies and depression. Sixty-four percent of my readers have reported improvements in mood when they’ve taken a D3 supplement. 5000 to 10000 IU per day is what it usually takes to get your vitamin D levels in range. I do recommend testing for vitamin D, and supplementing accordingly. (17)
- Magnesium: Multiple studies have linked magnesium deficiency with depression and anxiety, as this vital nutrient plays a key role in hormone balance and brain chemistry. Magnesium is required for the production of the sex hormones progesterone, estrogen, and testosterone, and also helps regulate cortisol — all of which impact mood and cognitive function. Magnesium is also an important component in thyroid hormone production, and helps balance blood sugar — key factors in mood stabilization. (18,19)
- Selenium: Selenium is essential for thyroid hormone synthesis. Research shows that it is also closely tied to mood disorders and cognitive function. Selenium deficiency is not only common in those with Hashimoto’s, but also with depression. (19,20) I often recommend Selenium from Pure Encapsulations, as it is generally well-tolerated.
- Myo-Inositol: Small studies have found that myo-inositol can help with depression as well as with obsessive-compulsive symptoms. It has also been shown to be a promising nutrient in reversing Hashimoto’s and normalizing TSH levels. (21, 22) I’ve seen success with Rootcology Myo-Inositol Powder in helping clients get a better sleep, balance hormones, and improve their mood.*
- Rootcology Selenium + Myo-inositol delivers a therapeutic range of both selenium and myo-inositol, and synergistic effects of the two combined has been shown to lower TSH.* For more information on the benefits of selenium and how to supplement properly, please take a look at my article on selenium deficiency and Hashimoto’s.
Stress Response Support
In my experience, treating hypothyroidism without treating the adrenals, is one of the biggest reasons people continue to feel exhausted despite receiving treatment with thyroid hormones — and it can also lead to symptoms of depression.
The adrenal glands release hormones, such as cortisol and adrenaline, that impact many important functions throughout the body, including stress tolerance and mood. In cases of chronic stress, the never-ending presence of stressful, yet non-life-threatening situations, can lead to the constant activation of the stress response. To help meet the demand for cortisol, your body will decrease the production of other hormones normally produced by the adrenals, such as progesterone, DHEA, and testosterone. (23,24)
Eventually, with enough chronic stress, your body becomes overwhelmed and desensitized to the usual feedback loop, and stops sending messages to the adrenals to produce more hormones or less hormones, no matter what’s happening.
In the functional medicine community, we call this adrenal fatigue.
If you think stress could be at the root of your depression, you may want to look into supporting your adrenals. As a starting point, I recommend the “ABCs” — Adaptogens, B vitamins, and vitamin C.
Adaptogenic herbs support the body’s ability to deal with stressors and are thought to work by normalizing the hypothalamic-pituitary-adrenal (HPA) axis. Some herbs, such as ashwagandha, can help normalize thyroid hormone levels, as well as support the body’s stress response. (25,26)
Of the readers I surveyed, 77 percent said their mood improved when they took adaptogenic herbs.
The B vitamins and vitamin C become depleted during high cortisol production. In particular, deficiencies in pantothenic acid (B5) and biotin (another B vitamin) have been linked to decreased adrenal function in animals and humans. Meanwhile, vitamin C helps to regulate cortisol and prevent blood pressure from spiking in response to stressful situations. (27,28)
My Rootcology Adrenal Support supplement contains all three ABCs, but since it contains licorice root extract, I do not recommend it for those with high blood pressure. Pure Encapsulation’s Daily Stress Formula is a great option for supporting the adrenals of those who have high blood pressure.
Lifestyle Interventions
There are many types of therapies, exercises, and activities aimed at reducing depression — the important thing is finding one that will work for you. This may take some experimentation, but a few of my favorite forms of mental health therapy include:
- Bright light therapy: Bright light therapy (BLT) is considered among the first-line treatments for seasonal affective disorder (SAD), yet a growing body of literature supports its use in other mental health conditions, including non-seasonal depression. BLT uses a lamp to mimic sunlight to adjust the person’s circadian rhythm and elevate their mood. I’m a big proponent of being out in nature and enjoying the sunshine (especially on a beach vacation); however, those of us living in colder climates may not always have the ability to escape. In such cases, you can purchase a therapy light online to sit under for 15 minutes a day, in the comfort of your home.
- Meditation: Stress and anxiety are major triggers of depression, and meditation can alter your reaction to those feelings by training the brain to sustain focus, and return to that focus when negative thinking arises. Meditation has even been found to change certain regions of the brain that are linked with depression. There are many apps that can help you begin a meditation practice (Headspace is a popular one), but even just closing your eyes, sitting still, and focusing on your breath for five minutes is a wonderful place to start.
- Exercise: Research has shown that exercise works as well as antidepressants for some people with depression. (29) While high-intensity exercise releases the body’s feel-good chemicals called endorphins, low-intensity energy over a sustained period of time causes the release of proteins called neurotrophic (or growth) factors. These proteins cause nerve cells to grow and make new connections, which improves brain function and makes you feel better. My favorite forms of exercise to give me a mental boost are hiking, yoga, and walking with my little family. 🙂
- Art therapy: The healing power of art is emerging as an evidence-based therapeutic modality for depression.
One meta-review published in 2015 examined the impact of art therapy on depression, anxiety, trauma, distress, inability to cope, and low self-esteem. It concluded that patients receiving art therapy (using the process of creating artwork as a form of mental therapy) had significant improvements in 14 out of 15 randomized control trials. (30)
By immersing themselves in the art of creation, people with depression are often able to push back against the darkness inside their minds and find ways to express themselves when words fail. You don’t have to consider yourself an “artist” to explore this form of therapy — it’s all about the process of creation, not the final product. Many years ago, at the suggestion of a grief and trauma therapist, I painted this mandala to express my grief. I still remember what I tried to convey through it. The red colors symbolize the intense pain I felt, the faint yellow, my exhaustion from crying, and the orange colors are signs of confusion. The flower outlines my struggle to keep it together at the time. Yet, you can also see hope, transformation, and healing on the horizon (as depicted through the little sunbursts).

- Yoga: Gentle forms of yoga, such as Yin Yoga and Hatha Yoga, have been shown to calm the nervous system and relax the mind. Many controlled studies have found benefits from yoga for depression and its symptoms, such as difficulty concentrating and lack of energy. The combination of meditation and physical movement involved in yoga provide two important elements for relieving depression: meditation helps allow a person to clear their mind, while controlled, focused movements help strengthen the body-mind connection. (31)
- Sauna therapy: Saunas provide many benefits for Hashimoto’s, including stress relief and mood elevation (I like to recommend infrared saunas specifically, but any type of heat therapy can be helpful). The sympathetic nervous system and HPA-axis try to respond to compensate when the body is stressed by the rising body temperature. When a person is in the infrared sauna, their norepinephrine levels rise, but the body’s stress hormones epinephrine and cortisol do not. Growth hormone, beta-endorphins, and prolactin also increase. Beta-endorphins account for the reason a sauna session feels so pleasurable. The muscles also relax, allowing the body to release any tension and be free of stress. During this time, the body’s parasympathetic nervous system takes over, putting the body in a state of complete relaxation. (32,33)
In my 2015 survey of 2332 readers with Hashimoto’s, 74 percent of people reported that using a sauna boosted their overall mood. (Please note that sauna use may not be recommended in specific circumstances, or for those with certain medical conditions. You can learn more about infrared sauna contraindications in my article on saunas and Hashimoto’s.)
- Neurofeedback: This is a form of biofeedback therapy that uses real-time displays of brain activity to help self-regulate brain function. Research has shown its effectiveness for a variety of brain-related conditions, including depression. I like the Neuroptimal system and recommend finding a local neurofeedback practitioner in your area who has one.
- Eye Movement Desensitization and Reprocessing (EMDR) Therapy: In this form of therapy, the individual thinks about the painful memory, then follows a series of finger movements performed by the therapist, to help desensitize the negative feelings associated with the traumatic experience. If your depression results from events that occurred in your past, utilizing therapy may be the path to healing. EMDR, or Eye Movement Desensitization and Reprocessing, is a method used by psychotherapists to help people eliminate the lasting effects of traumatic events. This type of therapy was initially developed by Francine Shapiro, PhD, who noticed that certain eye movements reduced the intensity of her disturbing thoughts and made her less anxious during a walk in nature. She tested the method with trauma victims suffering from PTSD, and published her findings in 1989, establishing it as an evidence-based level treatment for trauma and post-traumatic stress disorder. (34)
I highly recommend working with a therapist who specializes in EMDR if you have encountered traumatic events in your past. I assure you, you can get past them.
In terms of helping me cope with the traumatic loss of my loved one, I worked with Dr. Allan Botkin, the creator of IADC, a version of EMDR targeted to the loss of loved ones. The therapy was life-changing, and I recommend it to anyone who has lost someone.
Other Strategies to Address Depression
Some 80 percent of the people with Hashimoto’s that I surveyed reported that alternative therapies such as acupuncture and massage therapy improved their mood.
- Speaking with a counselor or therapist is another important step toward mental health for many people. Sometimes, talking through the problem can be the best way to find the root cause — especially if past trauma is a factor.
- I encourage you to seek an integrative-minded practitioner who is trained in functional medicine.
- Low-dose (nutritional) lithium may be helpful, and unlike prescription lithium, is not harmful to the thyroid. (Read my article on nutritional lithium for more information.)
- You may also try using amino acids, orthomolecular medicine, and the Organic Acids Test to help you find additional targets for healing. The Organic Acids Test can identify hidden causes of depression and autoimmune issues, such as yeast and/or mold, elevations in Clostridia bacteria, and altered neurotransmitters. (35,36)
Though this is not a comprehensive list of all of the therapies available to treat depression, they are easy places to start if you are looking for alternatives or complements to prescription antidepressants.
Takeaway
About 80 percent of my clients with depression who have followed the above-mentioned recommendations, report that their symptoms improved.
As always, I encourage you to take control of your own health and advocate for your needs. If your symptoms, including depression and other mood-related symptoms, are possibly related to your thyroid, be sure to advocate for comprehensive lab testing and the right medications (being under- or overmedicated can contribute to inaccurate lab tests and thyroid symptoms).
Additionally, I encourage you to look into the Root Cause Approach to healing Hashimoto’s and utilize the interventions listed above, as well as in my Hashimoto’s Protocol book, to begin improving your health today!
I love interacting with my readers on social media, and I encourage you to join my Facebook, Instagram, TikTok, and Pinterest community pages to stay on top of thyroid health updates and meet others who are following similar health journeys. For recipes, a FREE Thyroid Diet start guide, and notifications about upcoming events, be sure to sign up for my email list!
References
- Major Depression. National Institute of Mental Health. Updated January 2022. Accessed September 25, 2022. https://www.nimh.nih.gov/health/statistics/major-depression
- Siegmann EM, Müller HHO, Luecke C, Philipsen A, Kornhuber J, Grömer TW. Association of Depression and Anxiety Disorders With Autoimmune Thyroiditis: A Systematic Review and Meta-analysis [published correction appears in JAMA Psychiatry. 2019 Jun 19;:]. JAMA Psychiatry. 2018;75(6):577-584. doi:10.1001/jamapsychiatry.2018.0190
- Symptoms: Overactive Thyroid (hyperthyroidism). National Health Service. Updated September 2019. Accessed October 2022. https://www.nhs.uk/conditions/overactive-thyroid-hyperthyroidism/symptoms/
- Hage MP, Azar ST. The Link between Thyroid Function and Depression. J Thyroid Res. 2012;2012:590648. doi:10.1155/2012/590648
- Carta MG, Loviselli A, Hardoy MC, et al. The link between thyroid autoimmunity (antithyroid peroxidase autoantibodies) with anxiety and mood disorders in the community: a field of interest for public health in the future. BMC Psychiatry. 2004;4:25. Published 2004 Aug 18. doi:10.1186/1471-244X-4-25
- Müssig K, Künle A, Säuberlich AL, et al. Thyroid peroxidase antibody positivity is associated with symptomatic distress in patients with Hashimoto’s thyroiditis. Brain Behav Immun. 2012;26(4):559-563. doi:10.1016/j.bbi.2012.01.006
- Haugen BR. Drugs that suppress TSH or cause central hypothyroidism. Best Pract Res Clin Endocrinol Metab. 2009;23(6):793-800. doi:10.1016/j.beem.2009.08.003
- Honkanen, Emma A. MD et al. Bupropion Causes Misdiagnosis in Brain Dopamine Transporter Imaging for Parkinsonism. Clinical Neuropharmacology. 2019; 42(5):181-183. doi: 10.1097/WNF.0000000000000359
- Gaynes BN, Warden D, Trivedi MH, Wisniewski SR, Fava M, Rush AJ. What did STAR*D teach us? Results from a large-scale, practical, clinical trial for patients with depression. Psychiatr Serv. 2009;60(11):1439-1445. doi:10.1176/ps.2009.60.11.1439
- Field DT, Cracknell RO, Eastwood JR, et al. High-dose Vitamin B6 supplementation reduces anxiety and strengthens visual surround suppression. Hum Psychopharmacol. 2022;37(6):e2852. doi:10.1002/hup.2852
- Syed EU, Wasay M, Awan S. Vitamin B12 supplementation in treating major depressive disorder: a randomized controlled trial. Open Neurol J. 2013;7:44-48. Published 2013 Nov 15. doi:10.2174/1874205X01307010044
- Laird E, O’Halloran AM, Molloy AM, et al. Low vitamin B12 but not folate is associated with incident depressive symptoms in community-dwelling older adults: a 4 year longitudinal study [published online ahead of print, 2021 Dec 13]. Br J Nutr. 2021;1-22. doi:10.1017/S0007114521004748
- Shelton RC, Sloan Manning J, Barrentine LW, Tipa EV. Assessing Effects of l-Methylfolate in Depression Management: Results of a Real-World Patient Experience Trial. Prim Care Companion CNS Disord. 2013;15(4):PCC.13m01520. doi:10.4088/PCC.13m01520
- Lee HS, Chao HH, Huang WT, Chen SC, Yang HY. Psychiatric disorders risk in patients with iron deficiency anemia and association with iron supplementation medications: a nationwide database analysis. BMC Psychiatry. 2020;20(1):216. Published 2020 May 11. doi:10.1186/s12888-020-02621-0
- Richardson AC, Heath AL, Haszard JJ, Polak MA, Houghton LA, Conner TS. Higher Body Iron Is Associated with Greater Depression Symptoms among Young Adult Men but not Women: Observational Data from the Daily Life Study. Nutrients. 2015;7(8):6055-6072. Published 2015 Jul 23. doi:10.3390/nu7085270
- Wani AL, Bhat SA, Ara A. Omega-3 fatty acids and the treatment of depression: a review of scientific evidence. Integr Med Res. 2015;4(3):132-141. doi:10.1016/j.imr.2015.07.003
- Penckofer S, Kouba J, Byrn M, Estwing Ferrans C. Vitamin D and depression: where is all the sunshine?. Issues Ment Health Nurs. 2010;31(6):385-393. doi:10.3109/01612840903437657
- Serefko A, Szopa A, Poleszak E. Magnesium and depression. Magnes Res. 2016;29(3):112-119. doi:10.1684/mrh.2016.0407
- Wang J, Um P, Dickerman BA, Liu J. Zinc, Magnesium, Selenium and Depression: A Review of the Evidence, Potential Mechanisms and Implications. Nutrients. 2018;10(5):584. Published 2018 May 9. doi:10.3390/nu10050584
- Benton D, Cook R. The impact of selenium supplementation on mood. Biological Psychiatry. 1991;29(11):1092-1098.
- Mukai T, Kishi T, Matsuda Y, Iwata N. A meta-analysis of inositol for depression and anxiety disorders. Hum Psychopharmacol. 2014;29(1):55-63. doi:10.1002/hup.2369
- Benvenga S, Nordio M, Laganà AS, Unfer V. The Role of Inositol in Thyroid Physiology and in Subclinical Hypothyroidism Management. Front Endocrinol (Lausanne). 2021;12:662582. Published 2021 May 10. doi:10.3389/fendo.2021.662582
- Ranabir S, Reetu K. Stress and hormones. Indian J Endocrinol Metab. 2011;15(1):18-22. doi:10.4103/2230-8210.77573
- Kozlowska K, Walker P, McLean L, Carrive P. Fear and the Defense Cascade: Clinical Implications and Management. Harv Rev Psychiatry. 2015;23(4):263-287. doi:10.1097/HRP.0000000000000065
- Esmaealzadeh N, Iranpanah A, Sarris J, Rahimi R. A literature review of the studies concerning selected plant-derived adaptogens and their general function in body with a focus on animal studies. Phytomedicine. 2022;105:154354. doi:10.1016/j.phymed.2022.154354
- Sharma AK, Basu I, Singh S. Efficacy and Safety of Ashwagandha Root Extract in Subclinical Hypothyroid Patients: A Double-Blind, Randomized Placebo-Controlled Trial. J Altern Complement Med. 2018;24(3):243-248. doi:10.1089/acm.2017.0183
- Camfield DA, Wetherell MA, Scholey AB, et al. The effects of multivitamin supplementation on diurnal cortisol secretion and perceived stress. Nutrients. 2013;5(11):4429-4450. Published 2013 Nov 11. doi:10.3390/nu5114429
- Brody S, Preut R, Schommer K, Schürmeyer TH. A randomized controlled trial of high dose ascorbic acid for reduction of blood pressure, cortisol, and subjective responses to psychological stress. Psychopharmacology (Berl). 2002;159(3):319-324. doi:10.1007/s00213-001-0929-6
- Recchia F, Leung CK, Chin EC, et al. Comparative effectiveness of exercise, antidepressants and their combination in treating non-severe depression: a systematic review and network meta-analysis of randomised controlled trials. Br J Sports Med. 2022;56(23):1375-1380. doi:10.1136/bjsports-2022-105964
- Uttley L, Scope A, Stevenson M, et al. Systematic review and economic modelling of the clinical effectiveness and cost-effectiveness of art therapy among people with non-psychotic mental health disorders. Health Technol Assess. 2015;19(18):1-vi. doi:10.3310/hta19180
- Jean M, Umair M, Muddaloor P, et al. The Effects of Yoga on Bipolar Disorder: A Systematic Review. Cureus. 2022;14(8):e27688. Published 2022 Aug 4. doi:10.7759/cureus.27688
- Smith SM, Vale WW. The role of the hypothalamic-pituitary-adrenal axis in neuroendocrine responses to stress. Dialogues Clin Neurosci. 2006;8(4):383-395. doi:10.31887/DCNS.2006.8.4/ssmith
- Hussain J, Cohen M. Clinical Effects of Regular Dry Sauna Bathing: A Systematic Review. Evid Based Complement Alternat Med. 2018;2018:1857413. Published 2018 Apr 24. doi:10.1155/2018/1857413
- Shapiro, F. Efficacy of the eye movement desensitization procedure in the treatment of traumatic memories. 1989. https://onlinelibrary.wiley.com/doi/abs/10.1002/jts.2490020207
- Potera C. Molding a link to depression. Environ Health Perspect. 2007;115(11):A536. doi:10.1289/ehp.115-a536a
- The Clinical Significance Of Organic Acids Testing To Mental Health – How Fungal, Bacterial, Mitochondrial, And Other Test Markers Influence The Brain. Great Plains Laboratory, LLC. April 19, 2018. Accessed November 6, 2022. https://www.greatplainslaboratory.com/articles-1/2018/4/19/the-clinical-significance-of-organic-acids-testing-to-mental-health-how-fungal-bacterial-mitochondrial-and-other-test-markers-influence-the-brain
- Hadtstein F, Vrolijk M. Vitamin B-6-Induced Neuropathy: Exploring the Mechanisms of Pyridoxine Toxicity. Adv Nutr. 2021;12(5):1911-1929. doi:10.1093/advances/nmab033
Note: Originally published in November 2020, this article has been updated and expanded for thoroughness and accuracy.


 Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Gerri- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTOS AND THYROID CANCER
https://thyroidpharmacist.com/articles/hashimotos-and-thyroid-cancer
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Jill- I am so glad you are feeling better!! Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
Katy- That is great!! Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
GUT, BRAIN, AND AUTOIMMUNE DISORDERS: THE ROLE OF FOOD
https://thyroidpharmacist.com/articles/gut%C2%A0%C2%A0brain%C2%A0and-autoimmune-disorders
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
Liz- There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications
Candace- I personally struggled with pain in the form of body aches and stiffness as well as carpal tunnel in both arms in 2010, when I was first diagnosed with Hashimoto’s. It was awful, I had to wear braces on both arms all day and even at night for about 6 months.
I took NSAIDs every day to deal with the pain so I could get through my workday.
I hope these articles help you get started.
PAIN AND HASHIMOTOS
https://thyroidpharmacist.com/articles/pain-and-hashimotos
PAIN HASHIMOTOS AND FIBROMYALGIA…
https://thyroidpharmacist.com/articles/pain-hashimotos-and-fibromyalgia%E2%80%A6
TURMERIC FOR YOUR THYROID AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/turmeric-for-your-thyroid-and-hashimotos
Theresa- Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
Nancy- Did you know that if you live in the United States, the UK, Australia, Europe and most developed countries that add iodine to the salt supply and take thyroid medications, there’s a higher probability that you do have Hashimoto’s?
Depending on the source, estimates are that between 90-95% of those with hypothyroidism have Hashimoto’s.
But most doctors will never tell people that they have Hashimoto’s, or that their own immune system is attacking their thyroid. People are told that their “thyroid is sluggish”, and that these things happen with age and “Just take this pill, you’ll be fine.” I hope you check out these articles that I wrote.
ARE YOU DOING EVERYTHING FOR YOUR THYROID BUT NOT YET WELL?
https://thyroidpharmacist.com/articles/are-you-doing-everything-for-your-thyroid-but-not-yet-well
DO YOU HAVE HYPOTHYROIDISM OR HASHIMOTO’S OR BOTH?
https://thyroidpharmacist.com/articles/do-you-have-hypothyroidism-or-hashimotos-or-both
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well.
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests
Teresa- There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications
Ashley- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Marygrace- I’m very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation, and adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, animal and human studies. I have spent 4 years researching this and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my book. I have a whole chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein.
AMAZON
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Michelle- Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
Dr. Wentz,
I’ve noticed that even with just 1mg Lithium Orotate, I start to gain weight (with no change in diet or exercise). I’m suspecting the LO is a having an impact on my thyroid (I’m typically hypersensitive to all forms of supplements). Would taking kelp and selenium help me from becoming hypothyroid?
Kevin – thank you for reaching out. I’m so sorry you had that experience with LO. As for Kelp, I do not recommend for those with active Hashimoto’s due to it’s high content of Iodine. Additionally, excess iodine can perpetuate/worsen the autoimmune attack in Hashimoto’s and lead to additional thyroid cell destruction. Selenium on the other hand is often a nutrient those of us with thyroid disease are deficient in and something I do often recommend. Here are a couple articles with more info that I hope are helpful:
IODINE AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/iodine-hashimotos/
NUTRIENT DEFICIENCIEs: SELENIUM
https://thyroidpharmacist.com/articles/selenium-deficiency-and-hashimotos/
Agnes- You may be interested in checking out the Root Cause Recipe Portal. It is full of autoimmune paleo and paleo recipes. You’re able to organize weekly shopping lists, meal planning, etc. Hope you check it out. 🙂
http://rootcauserecipes.com/
Lenore- Thank you so much for your support. I’m looking forward to hearing your progress on this page. Make sure to take the book slow, take notes, highlight, and establish a baseline when making changes. 🙂
My symptoms are: depression, apathy, fatigue, heart palpitations, slightly dry skin
Do you think I should get a blood test to see if I have a thyroid problem? I’ve been struggling for years with the depression and the other problems with nothing seeming to help but I haven’t experienced any weight gain, sensitivity to the cold, constipation or muscle pain like most other people seem to.
Stella – please, understand that due to liability issues, I am unable to answer specific medical questions.
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Is there more information out there regarding the use of Levothyroxine as a prophylactic treatment for Hashimotos patients that are euthyroid? I have only been able to find one study that yielded some positive results, albeit only a study run for a year. I am hoping to avoid if at all possible, going into overt hypothyroidism and maintaining my thyroid levels balanced early on in the process.
Chris – thank you so much for following this page.
There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
HOW THE DOSE OF YOUR THYROID MEDICATION CAN UNCOVER YOUR ROOT CAUSE
https://thyroidpharmacist.com/articles/the-dose-of-your-thyroid-medication-can-uncover-your-root-cause/
HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications/
My teenage daughter is hypothyroid and takes medication. Her TSH levels have improved. Now she is suffering from depression and fatigue, she is not herself, says she cannot control her head, cant take it anymore, cries a lot and doesnt want to go to school. I feel for her that she is suffering and I want to help. Is it common that with improving TSH levels depression is triggered? She used to be a happy girl.
Thank you for this information. My boyfriend has Hashimoto’s and depression. I was struck by this sentence: “One of the biggest signs that a person with thyroid disease is not converting T4 to the active T3 properly is depression.” Do you happen to have any sources on that? It might help to convince his doctor. Thanks a lot!
Angela – thank you for following this page. I highly recommend that you work with a functional medicine clinician. It’s an entire medical speciality dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
I was diagnosed with hashimotos in 10/2014, 8 months after my first child was born. I went and still am gluten free and for the most part dairy and nightshade free. My Tpo was 220 when diagnosed and am at 72 now. I am on 65mg nature throid and my TSH is in the 3’s and T3 is at the higher level. I am primarily paleo and do AIP off and on. I’m feeling lack of energy and lack of interest and started getting anxiety attacks 8 months ago. Should I order the 94 allergy test? Wondering if I am eating something that is a trigger? I just want to feel normal again. Thank you.
Robin – thank you for following this page. Did you know that reactive foods trigger an inflammatory response in the GI tract, leading to malabsorption of nutrients (gluten sensitivity, in particular, has been implicated in causing a Selenium deficiency, a well-known risk factor for Hashimoto’s), and can also produce intestinal permeability whenever they are eaten?
Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts, and pain by eliminating the foods they are sensitive to. Some will also see a significant in thyroid antibodies! An additional subset of people will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
TAILORING YOUR THYROID DIET
https://thyroidpharmacist.com/articles/tailoring-your-thyroid-diet-to-your-needs
Hello Isabella. I’m 23 and was diagnosed with euthyroid Hashimoto’s 6 years ago. Do you really think my depression, which break out a year ago could be linked to euthyroid Hashimoto’s? All the doctors I have seen told me that being euthyroid, my depression is not linked to my thyroid. Could you suggest me supplements please? Thanks, Julie
Julie – thank you for following this page. I’m sorry to hear that you are struggling! 🙁
Depression is a common symptom of Hashimoto’s and a consequence of chronic illness.
I recommend you read this article as well:
ROOT CAUSES OF DEPRESSION AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/root-causes-of-depression-and-hashimotos/
In all of your articles and comment responses regarding unyielding depression in spite of good TSH, FT3 and FT4 levels, I have yet to see you (or Dr. Kelly Brogan) write anything about the implications of RT3 and whether that is a contributing factor for ongoing depression. I have been suffering with this as well as weight issues since the year prior to my Hypothyroid diagnosis in 2003, with worsening depression despite “good” TSH, FT3 and FT4 which my endocrinologist deems “the best she has ever seen them, so my depression is due to something else, and has no further suggestions.” She does not test for RT3 nor has she tested my 24 hour cortisol or other adrenal hormones. There is only one functional medical practitioner where I live in Saskatoon, Saskatchewan, and besides putting me on an elimination diet (which has also not helped), he does not seem to know much more than I do. The last 7 years have seen me lose my job, my income, my sanity, and relationships. My life has been taken from me and I have no quality of life. I am at the end of my rope. If you could provide any insight, it would be very much appreciated. Thank-you in advance.
Tanis – Thank you for following this page and I’m sorry to hear that you are struggling.
When I was first diagnosed with Hashimoto’s, I felt so alone. My doctor didn’t think it was a big deal, and none of my friends or co-workers had it. It wasn’t until I started to research online that I found others who were going through the same thing.
A couple of years after my diagnosis, I found Hashimoto’s 411, a closed Facebook group run by Alice Berry McDonnell. This group is amazing! It is comprised of an army of highly motivated, smart, supportive women and men (now 45,000+ strong), and each of them sharing ideas of what worked for them, things they were planning to try, and offering support to one another. The comfort I received from knowing that there were others going through the same challenges as I, was enormous.
https://www.facebook.com/groups/hashimotos411/
Ask questions. Post your thoughts. Scan the files. It is an absolutely amazing resource. Best of all it’s kept private from spammers.
I dealt with depression, alopecia areata and back pain since I was a teenager.In 2006 I was diagnosed with celiac disease and hashimotos and put on a gf diet and natural thyroid hormones (armour,compounded, nature’s throid and wp).Now,after my third child and 8 years of non stop nursing ,especially at night,my doctor put me on compounded synthetic t4/t3 slow release because new research says that people with hashimotos don’t do well on natural thyroid. I can’t find this info anywhere, and all I know is that I am getting worse.Been on a paleo diet and things got worse,like me developing carpal tunnel syndrome, mctd,shortness of breath in a daily basis for 1 year and a half,excruciating back pain that stops me from moving, alopecia areata coming back,depression and so on
I have been taking stress response by gaia,selenium and other things with little help.Really don’t know what else to do.I’m still 20 lb overweight even though my tsh went down.While my tsh went down,my antibodies went up from over 500 to over 700 now being on a grain and dairy free diet.While on natural thyroid my mind and body were so much better, but now supposedly are not good for me.My doc told me he could loose his license if he would prescribe that to me,which I know is lie. Question is why?
Ann – thank you so much for following this page. My heart goes out to you! There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication which you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
HOW THE DOSE OF YOUR THYROID MEDICATION CAN UNCOVER YOUR ROOT CAUSE
https://thyroidpharmacist.com/articles/the-dose-of-your-thyroid-medication-can-uncover-your-root-cause/
HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications/
20 yrs ago my mom was diagnosed with depression, and was prescribed prozak. And over the next 6 months she went on and off. She felt horrible off and horrible on, but the doctor kept saying she needed it. And after she admitted that she felt suicidal on it, he said you need more……my mom committed suicide :'( and 20 yrs later I am her age and found an amazing natural path doctor, so that I don’t go down the same road. And actually avoided doctors for so many years living miserable, but afraid of the same diagnosis. I am currently being tested for hashimoto’s and celiac (going off gluten changed my life) Anyh
Anyhow, I really believe that my mom struggled with this. Losing someone to suicide, isn’t easy. Both my brother’s have turned to drugs to cope. My younger one died 2 yrs ago from drugs, and my older is in the struggle losing everything.
Thank you for your dedication to educate ♡
Michelle – you are very welcome! <3
Michelle – thank you for following this page and for sharing. I am so happy you are taking charge of your heal and I’m looking forward to seeing your progress on this page. <3
How does one know which diet to try?
Would I just check my Antibody levels once a month for improvement and then move onto the next diet if it doesn’t?
I understand some people get better from diet alone, but do most need Thyroid medication for Hashimoto’s?
How do you know if your medication dose is too low or if it just isn’t the right one for you?
How do I know if I need selenium vs a diet vs other things?
This seems very complicated with so many possible treatments that it’s overwhelming where to even start.
Max – thank you for following this page. The most common triggers in Hashimoto’s are: nutrient deficiencies, food sensitivities, intestinal permeability (leaky gut), stress, an impaired ability to get rid of toxins and in some cases, infections. Optimizing your health starts with food. Figuring out which foods nourish you, and which ones cause you harm is the single most important thing you can learn in your health journey.
I’ve found that recognizing and eliminating reactive foods can be a life-changer for most people with Hashimoto’s.
Reactive foods trigger an inflammatory response in the GI tract, leading to malabsorption of nutrients (gluten sensitivity in particular has been implicated in causing a Selenium deficiency, a well known risk factor for Hashimoto’s), and can also produce intestinal permeability whenever they are eaten.
Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods that they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are some articles which I wrote:
BEST DIET FOR HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/best-diet-for-hashimotos-hypothyroidism
TAILORING YOUR THYROID DIET
https://thyroidpharmacist.com/articles/tailoring-your-thyroid-diet-to-your-needs
DAIRY AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/got-hashimotos-you-may-want-to-reconsider-dairy
One more thing:
Why do symptoms start?
As in, if we had Hashimoto’s for a while, why would symptoms start when they do?
I’ve always eaten the same, so it wasn’t from a sudden shift of diet.
Did my body just reach a tipping point?
Max – Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this. Sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. Here are the links to my books:
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
In 2016 I was diagnosed with both Hashimotos and FSH muscular dystrophy..it’s been a hard road both trying to find someone to help with my thyroid and also accepting the fact I now have a different future with my MD..I struggle with a lot of pain especially at night and also insomnia among other symptoms but those being the main ones..I am at a loss cause when I talk to drs the one question I always get is are you seeing anyone and somehow it always ends up with you have all the signs of depression and I think we should put you on antidepressant..I get frustrated cause I do have a lot on my mind and I’ve always worked in healthcare so that may make it worse but I know I need to start taking the right steps as far as diet to start the healing for my thyroid but just frustrating that every dr just wants to throw antidepressants at you and not just understand that I’m 35 and have health issues that will create a lot of havoc and a muscle disease that I will have forever..what do I say or do to make doctors understand and willing to help me in the right way?
Christina – thank you for sharing your journey here. <3 I understand how frustrating this can all be. I have personally struggled with pain in the form of body aches and stiffness as well as carpal tunnel in both my arms in 2010 when I was first diagnosed with Hashimoto’s. It was awful, I had to wear braces on both arms all day and even at night for about 6 months. I took NSAIDs every day to deal with the pain so that I could get through my workday. I hope that these articles help you get started:
PAIN AND HASHIMOTOS
https://thyroidpharmacist.com/articles/pain-and-hashimotos
PAIN HASHIMOTOS AND FIBROMYALGIA…
https://thyroidpharmacist.com/articles/pain-hashimotos-and-fibromyalgia/
TURMERIC FOR YOUR THYROID AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/turmeric-for-your-thyroid-and-hashimotos
I was diagnosed with Hashimoto’s disease in 1982 at the age of 12 and by then my thyroid had already been completely destroyed. My personality is that of an introvert. I have been plagued with waxing and waning anxiety and depression through out my teens and adult live but basically told to “suck it up” in most cases or just called too sensitive. I was diagnosed with psoriasis in 1982 as well.
My family doctor diagnosed me with General Anxiety Disorder last year and put me on Paxil because of overwhelming conditions at work. I found most helpful (it cleared up my psoriasis!) but it does come with some nasty side effects. Literally last month I learn there is a link between Hashimoto’s disease and anxiety and depression.
Could I have had General Anxiety Disorder undiagnosed for the better part of 35 years cause by Hashimoto’s?
Richard – thank you for reaching out and sharing your journey. <3 Anxiety symptoms are very common in people with thyroid disorders. Here are some articles which might help:
HASHIMOTO'S AND ANXIETY
https://thyroidpharmacist.com/articles/hashimotos-and-anxiety/
AUTOIMMUNE THYROID DISEASE AND ANXIETY
httpa://thyroidpharmacist.com/articles/autoimmune-thyroid-disease-and-anxiety
ARE YOU GOING CRAZY OR IS IT JUST YOUR THYROID
httpa://thyroidpharmacist.com/articles/are-you-going-crazy-or-is-it-just-your-thyroid
Thank you for all of your information! I read all the way to the end! I’m sure this information will be very helpful to me considering I see myself in everything you’ve written.
Jodi, you are very welcome! <3 Please keep me posted on your progress.
One of the supplements u listed has lemon balm in it. I thought lemon balm wasn’t good for hashimoto’s but it’s good for graves.