Those of us with Hashimoto’s often blame our thyroid for the many signs and symptoms we experience.
Hair loss? Thyroid!
Weight gain? THYROID!
Fatigue? It’s gotta be the THYROID!
While the thyroid plays a crucial role in these symptoms and our well-being, there’s another link that’s often underestimated: the adrenal glands. Treating hypothyroidism without treating the adrenals, is one of the biggest reasons people continue to feel exhausted despite receiving treatment with thyroid hormones.
Patients may initially report feeling more energetic after starting thyroid hormones, but this is usually followed by feeling worse and worse… until they are right back to where they were before they started the thyroid medications. At this point, they will likely go back to their physicians to check blood work, and will be told that everything is normal.
The patient begins to feel crazy… but that’s when another layer of the complex pathology of Hashimoto’s becomes unraveled. Many symptoms of hypothyroidism overlap with symptoms of underactive adrenals. However, physicians don’t routinely check adrenal function in those with Hashimoto’s.
In this article, I’ll discuss:
- What is the connection between thyroid issues and adrenal dysfunction?
- What causes adrenal dysfunction?
- Symptoms of adrenal dysfunction
- How to test your adrenal function
- The Root Cause approach to recovering from adrenal dysfunction
What Are the Adrenals?
The adrenals are two small glands, located on top of each kidney, that release hormones such as cortisol and adrenaline. These “stress hormones” impact many important functions throughout the body. They help establish your stress tolerance, tame inflammation, regulate blood sugar and body fat, control potassium and sodium levels (impacting blood sugar), and influence sex drive and anti-aging… among other things. [1]
You may have heard that the stress hormone cortisol is “bad.” This is misleading — while high levels of cortisol are problematic, what could be equally or more problematic is having low levels of cortisol, especially when it comes to having an autoimmune disease and fatigue.
Cortisol is a hormone that is required for life — we could not live without it, and it is an important anti-inflammatory hormone. In fact, it gets released whenever we have inflammation, to cool things down.
I have found that the majority of people with Hashimoto’s have low levels of cortisol.
What Causes Adrenal Fatigue?
In most cases of adrenal fatigue, the problems generally originate in a communication breakdown that occurs within the hypothalamic-pituitary-adrenal axis, otherwise known as the HPA axis. [2] The HPA axis describes the interactive feedback loop that takes place between these three endocrine glands.
The hypothalamus is like the CEO of our body’s production of hormones. It scans messages from our environment and other endocrine glands, as well as checks the body’s overall hormonal status, before passing on the order for more hormones to the pituitary gland. The pituitary gland then acts as a project manager and will pull together individual workers (like the thyroid gland, the adrenal gland, and the gonads) to do their jobs. The pituitary will also make sure the workers have adequate resources to do their jobs by managing growth and repair, as well as electrolyte/water balance.
The HPA axis works in response to two types of stress: immediate stress and chronic stress. Let’s see how the responses to each type differ.
In cases of immediate stress, the hypothalamus senses stress and sets off a hormone cascade that leads to the activation of our fight-or-flight response. As part of this response, the adrenals pump out extra hormones, and our bodies go from the state of relaxing, digesting and healing, to a survival state.
Our body’s energy is shifted from activities not essential to survival, like growing beautiful hair, metabolizing nutrients into energy, making hormones, and digesting and repairing itself, to instead focusing its resources to meet the great, stress-induced demand for cortisol and adrenaline.
Then, once we’ve escaped from the threatening bear or gotten out of the way of the oncoming car, the demand for emergency levels of hormones settles down, and the focus once again turns to the parasympathetic response, focused on body maintenance and upkeep.
In cases of chronic stress, the never-ending presence of stressful, yet non-life-threatening, situations can lead to the constant activation of the stress response.
To help meet the demand for cortisol, your body will decrease the production of other hormones normally produced by the adrenals such as progesterone, DHEA, and testosterone. [3]
Eventually, with enough chronic stress, the HPA axis becomes overwhelmed and desensitized to the usual feedback loop, and stops sending messages to the adrenals to produce more hormones or less hormones, no matter what’s happening. [4] Additionally, a person may run out of nutrients that are required for proper adrenal function.
One of the most common causes of adrenal fatigue is stress, which creates an intense demand for stress hormones such as cortisol and adrenaline.
If you are struggling with chronic stress, I encourage you to investigate these four common root causes or triggers:
1. Sleep Disorders
One of the fastest ways to induce adrenal dysfunction is through sleep deprivation. In fact, sleep deprivation is used in lab animals to suppress the hypothalamic-pituitary (HPA) axis and adrenal axis. [5] Sleep deprivation can be caused by insomnia, sleep apnea, and shift work.
2. Mental/Emotional Stress
Feelings such as grief, guilt, fear, anxiety, excitement, and embarrassment can be classified as stress. This stress is based on our perception, not on the nature of the individual stress. For example, public speaking may cause plenty of mental stress for someone with social anxiety, but another person who enjoys speaking in front of others may perceive the experience as pleasurable. Situations that are new, unpredictable, and threaten the ego, or that involve feeling a loss of control, are perceived as stressful.
3. Metabolic/Glycemic Dysregulation
Researchers in Poland have found that up to 50 percent of patients with Hashimoto’s have an impaired tolerance to carbohydrates. [6] This means that after consuming carbohydrate-rich foods, their blood sugar levels would spike up very high, causing a great amount of insulin release.
The role of insulin is to clear blood sugar out of our cells, so a large insulin release is followed by a rapid drop of blood sugar (hypoglycemia).
Symptoms of hypoglycemia are very unpleasant and may include irritability, fainting, lightheadedness, or tremors. Hypoglycemia necessitates the release of cortisol to help maintain the glucose supply to the brain and counteracts insulin, causing insulin resistance. [7] (This is also linked to the type 2 diabetes epidemic.)
4. Inflammation
Chronic inflammation may occur from joint pain, obesity, toxic burden, inflammation in the GI tract from irritable bowel disorders, pathogens, or food sensitivities. These conditions will signal cortisol for its anti-inflammatory effect. [8]
Common Symptoms of Adrenal Dysfunction
Symptoms of poor adrenal function may include the following: [9]
- Feeling overwhelmed
- Feeling tired despite adequate sleep
- Trouble falling asleep or staying asleep
- Difficulty getting up in the morning
- Dependency on caffeine
- Cravings for salty foods (a.k.a. the “I just ate a whole bag of chips syndrome”)
- Cravings for sweet foods
- Increased effort required for everyday activities
- Intolerance to exercise
- Low blood pressure
- Feeling faint/dizzy when getting up quickly
- Easily startled
- Mental fog or trouble concentrating
- Alternating diarrhea/constipation
- Low blood sugar
- Decreased sex drive
- Decreased ability to handle stress
- Longer healing time
- Mild depression
- Less enjoyment in life
- Feeling worse after skipping meals
- Increased PMS
- Reduced ability to make decisions
- Reduced productivity
- Poor memory
Do any of these sound familiar?
Testing for Adrenal Issues
In addition to looking at your symptoms, you can determine if you have adrenal dysfunction by utilizing the assessments below.
The Irritability Test
Irritability and overwhelm are two cardinal signs of adrenal dysfunction. My best test for determining adrenal issues is being snappy or short-tempered, feeling overwhelmed, or finding other people annoying. For example, I can always tell that my adrenals are overwhelmed when my mom calls to say hello, and I feel like this is too much of a demand!
Blood Pressure Test
People with adrenal fatigue often have low blood pressure and/or a drop in blood pressure after standing up from a lying down or sitting position (orthostatic hypotension). [10] They may also experience dizziness or lightheadedness when changing positions.
A great way to test for this is by measuring your blood pressure while lying down, then standing up and measuring your blood pressure again. This is a common test functional doctors perform to determine the adrenal function of a patient.
If your blood pressure is below 120/80 mmHg, this may mean that your adrenals are underactive, or that you are dehydrated.
Pupil Contraction
People with low adrenal function may often have difficulty contracting their pupils. Usually our pupils dilate (enlarge) in the dark, and contract (get smaller) in the light. Symptoms of adrenal dysfunction may include light sensitivity, difficulty seeing in bright lights, having to wear sunglasses on most days, or as I like to call it, feeling like a vampire in daylight!
Unstable Temperatures
If you are keeping track of your first morning temperatures, low and unstable morning temperatures may be suggestive of adrenal insufficiency. In contrast, pure hypothyroidism usually results in temperatures that are low, but rather stable, on a daily basis.
The Whole Bag of Chips Test
Have you ever eaten (or wanted to eat) an entire bag of chips in one sitting? You’re not alone! Salt cravings are a cardinal sign of adrenal issues. With adrenal issues, we may find ourselves with intense cravings for salty foods like crackers, chips, pretzels, and olives.
Hormone Testing
Adrenal saliva tests provide a way to test our current adrenal function. These tests are generally only available from functional medicine and integrative health care professionals.
Normally functioning adrenals are supposed to put out the most cortisol in the morning, and the levels of cortisol should decline during the day, until very little cortisol is secreted at bedtime. A cortisol kick in the morning helps us to get out of bed bright-eyed and bushy-tailed, ready to face the day. Low cortisol secretion at bedtime helps us relax and sleep.
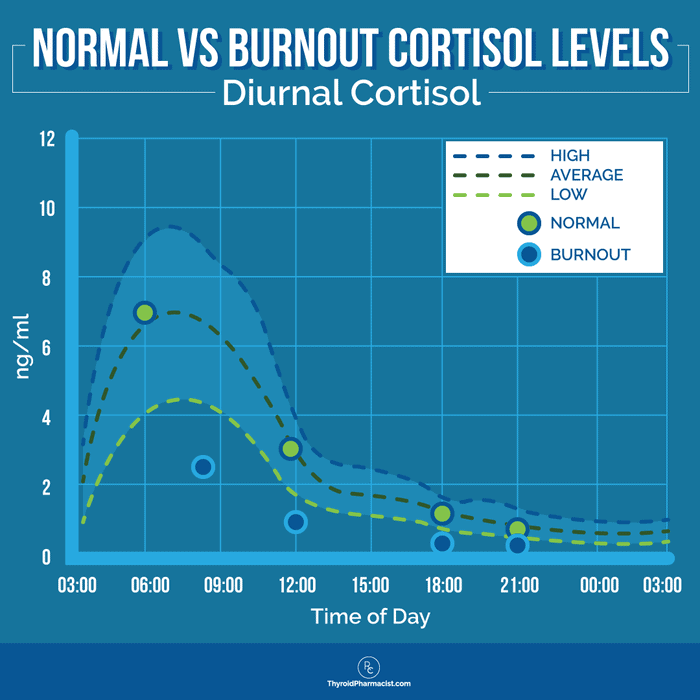
Some people with adrenal dysfunction have the opposite pattern — they can’t get up in the morning and drag their feet until the early afternoon, feel slightly human for a few hours between 2 pm and 8 pm, then get a second wind at bedtime. These people often have a flipped cortisol rhythm, where their adrenals put out very little cortisol in the morning and too much in the evening, causing them to be alert and sleepy at the wrong times.
Other people may have abnormally low cortisol readings all day, every day. In this case, the fatigue lasts all day — I have been there, and it’s not fun. This low cortisol causes inflammation to go unchecked in the body, prevents healing, and causes the person to be sluggish for most of the day.
If you’re going to go down the road of adrenal saliva testing, I recommend the Adrenal Stress Profile test by ZRT, a saliva test that checks for adrenal imbalances by evaluating one’s adrenal hormones DHEA-S and diurnal cortisol (morning, noon, evening, nighttime). You can order this test through my Rupa Health or MyMedLab channels.
I recommend this test to all of my clients with Hashimoto’s, and have found that 90 percent of my clients (who do the test) have some degree of adrenal fatigue.
The Conventional Approach to Adrenal Fatigue
The adrenals are a source of disagreement between conventional medical doctors and natural practitioners. Conventional medical doctors only recognize Addison’s disease as an adrenal insufficiency disorder, but do not recognize “adrenal fatigue” as a medical diagnosis. [11] (Adrenal insufficiency associated with Addison’s disease, which is an autoimmune condition, is more due to autoimmune damage to the adrenals, resulting in their inability to produce hormones, rather than the dysfunctional patterns of cortisol production observed in adrenal fatigue.)
When my integrative doctor first suggested that I get tested for adrenal fatigue, I “Googled” the term and found a “reputable source” that adrenal fatigue was a made-up disorder and did not exist.
Being a skeptical pharmacist, I put off testing my adrenals — I had just ventured into the world of alternative medicine, and was always afraid of people trying to take advantage of me and take my money, not realizing that they were simply trying to help.
But then I got to a point where I was just so exhausted and irritable, despite taking thyroid medications and following a gluten-free diet.
I started talking to Carter Black, RPh, my compounding pharmacist, about the symptoms I was experiencing, and he suggested that I have my adrenals tested. Mr. Black had specialized in hormones for many years and told me that the interventions for adrenal fatigue did indeed work well for many of his patients.
Finally it stuck: maybe it was hearing it from a fellow pharmacist, or maybe because he didn’t have any adrenal test kits to sell to me, that I decided to try it out.
Sure enough, I had an advanced stage of adrenal fatigue, and the recommended treatments helped me feel tremendously better!
Some may refer to adrenal fatigue as HPA axis dysfunction, but regardless, it does exist! Your symptoms and experiences are NOT in your head!
The Root Cause Approach to Recovering From Adrenal Fatigue
There are six main pillars of my Adrenal Recovery Protocol that I’ll explain more in-depth in this section. These are important elements that I outline in even greater detail in my book, Adrenal Transformation Protocol, which is your ultimate guide to healing your adrenals.
However, before I explain these pillars, please note that I don’t recommend any of my go-to adrenal-supportive products for people with Addison’s. Individuals with Addison’s may need steroids and may need to avoid thyroid medications until they are stabilized on steroids. The different supplements and even electrolytes shared in this article can exacerbate Addison’s as well.
1. Rest
Sleep is the reset button for the adrenals. The fastest way to get into adrenal fatigue is through sleep deprivation. The fastest way to get out is to get plenty of sleep. When we sleep, our body releases human growth hormone and repairs itself. Make sure to get at least seven hours of sleep each night, and go to sleep before 10 pm. If you can pull it off, I actually recommend getting 10-12 hours of sleep per night for one month, in my adrenal-focused recovery protocols.
However, in the real world, I know not all of us are able to achieve a good night’s sleep every night, let alone sleep for 10-12 hours. Whether our kids are waking us up every two hours, or we’re working abnormal hours, getting eight hours of restful sleep every night can seem out of reach for many of us. In such cases, I recommend sleeping as much of those 10 to 12 hours as possible, and engaging in relaxation for the remaining hours (such as taking a warm Epsom salt bath).
Be sure to read my article on the sleep apnea and Hashimoto’s connection if you have unrefreshed sleep, snoring, and/or a scalloped tongue.
2. Balance Blood Sugar
Stabilizing your blood sugar through diet is a crucial step in overcoming adrenal fatigue and thyroid conditions. Balancing your blood sugar can create noticeable improvements in how you feel each day.
Aim first and foremost to eat more fats and proteins, and less sugary and starchy carbs. When consuming carbohydrate-rich foods, your blood sugar goes up too high, too quickly, causing symptoms such as nervousness, lightheadedness, anxiety, and fatigue. These swings in blood sugar can weaken your adrenals and cause a spike in your thyroid antibodies.
Two supplements that may help support blood sugar balance are carnitine and myo-inositol. Check out my article on stabilizing your blood sugar with diet for more information.
In the last few years, I started offering my Fatigue and Brain Fog Fix in Six: Thyroid Adrenal Edition program (formerly the Adrenal Transformation Program), which has helped thousands of my readers feel better. In fact, 92 percent of participants reported reduced mental fog, 89 percent had reduced fatigue, and 86 percent had reduced anxiety. This signature program is also outlined in my book, Adrenal Transformation Protocol, which will take readers through my tried and true process to transform their adrenals.

3. Reduce Stress
The most important strategy for combating adrenal fatigue does not involve dieting, supplements, medications, or testing. This strategy, however, is often the hardest to implement.
The strategy is… stress reduction.
Reducing my stress was probably the hardest lifestyle change for me to implement. I only had two settings, “GO” and “SLEEP.” I did not know how to relax, smell the roses, turn off, or unwind.
So, I came up with this list of strategies (described below) to make myself more relaxed and shift my body into a state of relaxing, digesting, and healing. These days, I derive so much joy from life’s simple pleasures, and I hope you will soon be able to do the same! I hope some of my strategies will resonate with you, but many of you will want to come up with your own list.
Many of these items may be really difficult to implement, especially for those of us with responsibilities like jobs, children, or elderly relatives who need our care. However, somehow, you HAVE to schedule time for yourself.
We often expect our doctors to heal us, but the healing comes from within just the same. No one else will do it for you. Put it in your planner if you must.
Do your best to eliminate, simplify, delegate, automate.
Having fewer commitments on our plate, especially in the evenings, can allow for us to go to bed at a deliciously early time… and not feel guilty about it. If you are feeling overwhelmed, reflect on areas in your life that you can work on. For example, are you being bombarded by extra responsibilities around the house? If so, speak up and see if you can delegate some of your tasks to others.
Shift your mindset.
Thinking positive thoughts and practicing meditation can shift your body into “rest, digest, and heal” mode. In essence, positive thoughts and relaxation can send your body messages to promote healing. Even pausing to practice yogic breathing can lead to increased feelings of calm.
One of my favorite yogic-breathing techniques is the 4-7-8 exercise, where you breathe in for a count of 4, hold your breath for a count of 7, and then breathe out for a count of 8.
Positive thoughts can also come in the form of affirmations, which you can repeat throughout the day.
Some of the affirmations I’ve found most helpful are:
- “I love myself.”
- “I am powerful.”
- “I am healing.”
- “I am loved.”
- “The world is a safe and beautiful place.”
- “I am beautiful.”
I also recommend practicing mindfulness as a way of diminishing stress. This means pausing and truly being present in the moment; taking time to notice all of the beauty, kindness, and good things that are present in the world. And if at first you don’t see it, try looking a bit harder — you might just be surprised as you suddenly become aware of the beauty in the trees or the kindness of strangers. 🙂
Be mindful of what you’re listening to.
In the modern world, we are constantly bombarded with toxicity… and I don’t just mean from pesticides and pollution. News channels are meant to set off our fight-or-flight response, releasing adrenaline to keep us glued to the TV, waiting for the latest updates; social media algorithms are set up to keep us scrolling, talk radio features controversy… you get the idea.
We need to stay somewhat connected, so we can be informed. However, I recommend tuning out the negative news, shows, social media feeds, etc. that trigger you, and focusing only on the information you need.
I also suggest incorporating more healing sounds instead. Choose to listen to healing music on a daily basis, whether that’s classical, instrumental, gospel, whatever you prefer.
Here are a few of my favorites. (I like listening to music on YouTube, Pandora, or Spotify!):
- Medicine for the People
- Enya
- Lullabies (they work for babies, as well as for adults! :-))
- “Flow state” music
I also recently rediscovered a form of healing music called Wholetones. This healing music uses specific frequencies to help facilitate restorative sleep and create a sense of peace. My baby boy, Dimitry, used to get very stressed out in the car, often crying in his car seat. While playing lullabies helped a bit, Dimitry immediately stopped fussing and started sleeping with the Wholetones music! I don’t know if this is a coincidence, but I’ve kept that CD in my car player ever since!
Orderliness and predictability are your friends.
Plan your life that way when you can. Get organized, and keep your space neat and clean. Schedule times to clean the house and catch up on life. Make sure you schedule downtime as well.
Laughter Rx. (Laughter is known to boost oxytocin levels.)
Reach out to your partner or call a friend, and do some positive bonding — but only if doing so gives you energy. Are you an extrovert or an introvert? Does socializing give you energy, or take away your energy? In some cases, the answer depends on the person and the situation. If you are energized by socializing, know that bonding with dear friends and sharing laughter, can boost oxytocin and help counter the negative effects of our stress hormone, cortisol!
Even if you’re an introvert, there are other ways to laugh, like watching a funny movie, show or stand-up comedy, or reading or listening to a funny book. Just be sure to do whatever makes you laugh!
Start a journal.
Make a list of what makes you feel better and what makes you feel worse, and be mindful of those things. Focus on doing more of the things that make you feel good, big or small (i.e. having a warm cup of your favorite tea), and less of the things that make you feel worse. You can also use your journal to start a daily gratitude exercise.
Often in times of increased stress, especially when we’re not feeling well, or feel like we do not have control, it can be difficult to remember the good things in our lives. Starting each morning by writing down three things you are grateful for, may help to shift your entire day!
I also created this handy graphic which includes a recap of the strategies above, so you can share, print, or save it, and refer to it whenever you need a reminder!

4. Reduce Inflammation
In addition to reducing stress, reducing inflammation helps support healthy adrenal function and, in turn, healthy thyroid function.
Food sensitivities are a common source of inflammation. [12] Gluten, dairy, and soy are the most common reactive foods in Hashimoto’s, and eliminating them will eliminate inflammation in your body. Elimination diets and food sensitivity testing may help you determine additional foods that may need to be removed from your diet. I have an article on food sensitivities that you can read for more information.
Chronic infections are also a common source of inflammation in the body. [13] Common infections I see in those with Hashimoto’s include H. pylori, Blastocystis hominis, and Candida, but there are numerous potential infections that can be root causes as well.
S. boulardii is one key supplement that I started recommending for people with Hashimoto’s. It tends to be a broad spectrum, gentle, beneficial yeast that can be a tool in lowering gut inflammation from past use of antibiotics, infections, and dysbiosis, by helping with re-establishing a healthy gut flora. I think of it as a one-stop shop for lowering gut inflammation. [14] 🙂
5. Replenish Nutrients and Electrolytes
The salt cravings and feelings of dehydration that occur with adrenal fatigue, are our body’s way of letting us know that we need more salt. Rather than reaching for processed foods or thyroid-toxic iodized salt, including a good-quality sea salt in your diet may help if you feel a bit dizzy getting up in the morning or after a hot bath, or have other symptoms of adrenal fatigue.
I like to recommend buying a pink or gray sea salt and making yourself a salty drink, such as sole — a drink made of filtered water and pink Himalayan salt (recipe is included in the graphic below) — each morning, and sipping it throughout the day. Homemade bone broths with plenty of sea salt are also a great and tasty way to re-hydrate. An electrolyte supplement can also be useful for keeping up proper hydration levels.

In addition to sole, another drink that is great for adrenal fatigue is called the “Adrenal Kickstart.” It consists of fresh orange juice (best if cold-pressed or freshly squeezed and organic), a fat such as coconut cream or coconut milk, and sea salt.

The vitamin C in the orange juice supports the adrenals (the benefits of vitamin C are discussed in depth in the next section). Although orange juice is high in sugar, we are balancing it with oxytocin-releasing fats and clean protein, so this helps to counterbalance the sugar rush one would typically get with drinking just orange juice.
Furthermore, the fats from the coconut and protein powder help with satiety and blood sugar balance, and the sea salt directly supports healthy cortisol production.
6. Build Resilience with Supplements
While supplements often need to be individualized for people depending on their level of adrenal dysfunction (which needs to be determined via testing), I have found that most people with Hashimoto’s feel better when they utilize the ABCs of adrenal supplements.
The ABCs are Adrenal Adaptogens, B Vitamins, and Vitamin C.
Adaptogenic herbs are any natural herb products that support the body’s ability to deal with stressors. [15] In order to be considered an adaptogen, an herb must possess three main qualities. First, the herb must be non-toxic to the patient at normal doses. Secondly, the herb should help the entire body to cope with stress. Finally, the herb should help the body to return to “normal” regardless of how stress is currently affecting the person’s functioning. In other words, an adaptogenic herb needs to be able to both tone down overactive systems and boost underactive systems in the body. Adaptogens are thought to normalize the hypothalamic-pituitary-adrenal (HPA) axis. [16]
Adaptogenic herbs include: ashwagandha, astragalus, reishi mushroom, dang shen, eleuthero, ginseng, jiaogulan, licorice, maca, schisandra (available via Fullscript – if you don’t have an account, you can sign up with my credentials here), spikenard, and suma. These are examples of herbs that may increase the body’s ability to resist stress, and have been helpful in relieving adrenal dysfunction when used in combination with vitamins and minerals.
I personally love using adaptogens. I always joke that adaptogens make other people in my life much easier to tolerate. 🙂 I have taken adrenal adaptogens on and off since 2012. I like to use more of them around holidays and periods of stress, and they really help me stay balanced.
Vitamin C and B vitamins become depleted during high cortisol production.
In particular, deficiencies in pantothenic acid and biotin (vitamins in the “B” family), have been linked to decreased adrenal function in animals and humans. [17]
Vitamin C is an important antioxidant that helps support the adrenals, mitochondria, collagen production, and the suppression of a reactivated Epstein-Barr virus infection, along with many other potential viruses. [18] It’s easy to see how stress can make us vulnerable to catching everything that’s going around, as well as to latent infections reactivating in our bodies.
While some may wish to obtain these nutrients from natural whole food sources, this is not always possible. This is due to gut issues, which can usually result in people with Hashimoto’s having an impaired ability to extract vitamins and minerals from food.
Rootcology’s ABC Blend: Adrenal Support

I created the supplement Rootcology Adrenal Support to use a combination of the ABCs I recommend for balancing the adrenals: Adaptogens, B vitamins and vitamin C. This blend of adaptogenic herbs, vitamins, minerals, and amino acids is designed to support the adrenals and provide a powerful defense from the mental and physical factors associated with occasional stress. The formula synergistically supports mental relaxation while counteracting the metabolic effects of occasional stress as well.
I included ashwagandha in the blend, as ashwagandha has research-supported benefits for thyroid health. A 2018 study examined the effect of ashwagandha on people with elevated TSH levels over a period of eight weeks, and found that compared to the control group, the TSH levels of participants receiving ashwagandha improved significantly, as did T3 and T4 levels, effectively normalizing thyroid function. [19] Please note, ashwagandha is a nightshade, so if you have nightshade sensitivity, you may be sensitive to ashwagandha. (However, some people may only be sensitive to certain nightshades and may tolerate it.)
I also added licorice to this blend. Licorice was one of the herbs that helped me the most in overcoming fatigue. Licorice root extract prevents the breakdown of cortisol into inactive cortisone. [20] Thus, it keeps our cortisol around longer, giving us more energy. It may be helpful for those with low cortisol and low blood pressure. Please note, it should not be used by those with water retention or high blood pressure.
I generally recommend using the ABCs long-term, as life is inevitably full of stress. For added convenience, you can subscribe to get Adrenal Support delivered straight to your door on a monthly or bimonthly basis.
Alternative ABC Blend by Pure Encapsulations
 Daily Stress Formula – For those who have high blood pressure or have a sensitivity to licorice, I like recommending the ABC blend by Pure Encapsulations, which has a similar formulation to the Rootcology ABC blend, but does not contain licorice.
Daily Stress Formula – For those who have high blood pressure or have a sensitivity to licorice, I like recommending the ABC blend by Pure Encapsulations, which has a similar formulation to the Rootcology ABC blend, but does not contain licorice.
Additional Supportive Nutrients
In some cases, you may benefit from additional B vitamins and vitamin C, as well as magnesium, to support your adrenals.
 B Complex Plus – B vitamins play an important role in cell metabolism, thyroid function, and adrenal function. They become depleted in stressful situations that often precede the development of autoimmunity. Four especially important B vitamins are pantothenic acid (B5), thiamine or benfotiamine (B1), biotin (B7), and cobalamin (B12). This exceptional combination of B vitamins, including vitamins B1, B2, B3, B5, B6, B12, biotin, and folate (as Metafolin L-5-MTHF), should be helpful for most people with low energy levels. B vitamins are water-soluble vitamins and do not build up in the body, so the risk for toxicity is almost nonexistent.
B Complex Plus – B vitamins play an important role in cell metabolism, thyroid function, and adrenal function. They become depleted in stressful situations that often precede the development of autoimmunity. Four especially important B vitamins are pantothenic acid (B5), thiamine or benfotiamine (B1), biotin (B7), and cobalamin (B12). This exceptional combination of B vitamins, including vitamins B1, B2, B3, B5, B6, B12, biotin, and folate (as Metafolin L-5-MTHF), should be helpful for most people with low energy levels. B vitamins are water-soluble vitamins and do not build up in the body, so the risk for toxicity is almost nonexistent.
 BenfoMax – Thiamine is one of the B vitamins, known as B1. It supports blood sugar function and the adrenals, and can boost our energy levels. It also has the important roles of converting carbohydrates into energy and aiding with the digestion of proteins and fats. Thiamine is required for proper release of hydrochloric acid in our stomachs, which is needed for proper protein digestion. (Most people with Hashimoto’s have little or no stomach acid.) The latest research suggests that a mild deficiency may exist in people with autoimmune disease and related malabsorption issues. [21] If you’ve been struggling with fatigue, low stomach acid, carbohydrate intolerance, low blood pressure, and your adrenals, you may benefit from up to 600 mg of thiamine a day.
BenfoMax – Thiamine is one of the B vitamins, known as B1. It supports blood sugar function and the adrenals, and can boost our energy levels. It also has the important roles of converting carbohydrates into energy and aiding with the digestion of proteins and fats. Thiamine is required for proper release of hydrochloric acid in our stomachs, which is needed for proper protein digestion. (Most people with Hashimoto’s have little or no stomach acid.) The latest research suggests that a mild deficiency may exist in people with autoimmune disease and related malabsorption issues. [21] If you’ve been struggling with fatigue, low stomach acid, carbohydrate intolerance, low blood pressure, and your adrenals, you may benefit from up to 600 mg of thiamine a day.
 Vitamin C – Vitamin C is essential for supporting adrenal function. I recommend doses of 500 mg to 3,000 mg per day, as tolerated. My favorite way to get vitamin C is through Rootcology’s Electrolyte Blend, as it’s important for adrenal function to stay hydrated and keep our electrolytes in balance. This specifically-formulated blend of electrolytes contains 1734 mg of vitamin C per serving, along with other electrolytes which may help maintain normal hydration levels and support the body during occasional periods of stress. As an added bonus, this blend also contains D-ribose, which supports our energy-producing powerhouses, the mitochondria.*
Vitamin C – Vitamin C is essential for supporting adrenal function. I recommend doses of 500 mg to 3,000 mg per day, as tolerated. My favorite way to get vitamin C is through Rootcology’s Electrolyte Blend, as it’s important for adrenal function to stay hydrated and keep our electrolytes in balance. This specifically-formulated blend of electrolytes contains 1734 mg of vitamin C per serving, along with other electrolytes which may help maintain normal hydration levels and support the body during occasional periods of stress. As an added bonus, this blend also contains D-ribose, which supports our energy-producing powerhouses, the mitochondria.*
 Magnesium Citrate – As magnesium is depleted by stress and is often difficult to obtain from foods, most people will benefit from long-term supplementation. It is also excellent for promoting relaxation and sleep. The citrate version can also help with bowel movements (one of the less glamorous symptoms of hypothyroidism).
Magnesium Citrate – As magnesium is depleted by stress and is often difficult to obtain from foods, most people will benefit from long-term supplementation. It is also excellent for promoting relaxation and sleep. The citrate version can also help with bowel movements (one of the less glamorous symptoms of hypothyroidism).
Advanced Strategies
While many cases of adrenal dysfunction are caused by current stress, and removing or modifying how we respond to those stressors can help with overcoming adrenal dysfunction, in some cases, additional interventions may be needed to address past traumatic stress, as well as the chronically altered release of adrenal hormones.
Traumatic Stress
Traumatic stress may lead to a chronic pattern of adrenal hormone dysfunction. Various types of traumas and abuse have been tied to autoimmune conditions and thyroid hormone abnormalities. [22] Many of my clients have experienced significant traumas such as the loss of a loved one and/or being in an abusive relationship, before the onset of Hashimoto’s. Some of us have also experienced childhood trauma, which can set the tone for altered hormone patterns in adulthood.
Resolving traumatic stress usually requires a targeted therapy (I prefer neurofeedback and EMDR), and is a bit beyond the scope of this article, so until I have a chance to write an article on this topic, you may want to read my book, Hashimoto’s Protocol, as it contains a chapter entirely dedicated to this subject. My Adrenal Transformation Protocol book addresses emotional and psychological stress.
Supplemental Hormones
A variety of hormones and adrenal-supporting substances may be used based on your lab test results and adrenal dysfunction stage.
Although most of these hormones are available over the counter at health food stores, they are certainly not benign and should be used under the supervision of a trained professional with extreme caution. Not everyone will need all of these supplements.
Your practitioner may utilize progesterone, pregnenolone, DHEA, 7-Keto, adrenal glandulars, and in some cases, the medication hydrocortisone, to rebalance your adrenals.
I used to believe that healing the adrenals required hormones, sleeping 12+ hours a day, and quitting caffeine for three to 24 months in order to heal… until I found myself in adrenal dysfunction as a new mom, and realized that the strategies I once used as a young woman would no longer work.
Fortunately, I found a much simpler and effective solution to transforming one’s adrenals into a healing state, in just four weeks! I shifted from surviving to thriving – yes, even as a sleep deprived new mom who was drinking 2 cups of coffee per day – and decided to pilot this program with my clients in 2020. Over 3000 people have now taken my Fatigue and Brain Fog Fix in Six: Thyroid Adrenal Edition program (formerly the Adrenal Transformation Program), and the results have been incredible!
- 92 percent of people reduced their brain fog!
- 89 percent of people had less fatigue
- 86 percent reported less anxiety after the program
- 85 percent had less irritability
- 82 percent had less morning fatigue
- 81 percent improved their sleep
- 81 percent improved their libido
- 80 percent reduced their nervousness
- 78 percent reduced feelings of depression
- 77 percent had fewer mood swings
- 76 percent reduced their joint pain
Based on the results I have seen with my Fatigue and Brain Fog Fix in Six participants, I believe that most people can heal their stress response in just four weeks, even without sleeping for 12 hours a night, without quitting caffeine, and without taking hormones. 🙂
Monitoring Your Thyroid Hormones When Taking Supplements
Whenever you start a lifestyle or complementary intervention to address Hashimoto’s or adrenal issues, I encourage you to work with your doctor to monitor your thyroid symptoms, thyroid hormones, and thyroid antibodies. This is a great idea for any lifestyle intervention, but a must for lifestyle changes that could impact your TSH, especially if you are already taking thyroid medications.
The supplements listed above could impact your TSH and need for thyroid medications. So as you move forward with supplementation, please look out for the following symptoms of being overmedicated: rapid or irregular heartbeat, nervousness, irritability or mood swings, muscle weakness or tremors, diarrhea, heat intolerance, menstrual irregularities, hair loss, weight loss, insomnia, chest pain, and/or excessive sweating.
I recommend testing thyroid hormone levels every six to 12 weeks while using complementary therapies, including root cause medicine, diet, or supplements, to ensure your thyroid medication dosage is optimized — or sooner, if you are showing any of the above symptoms. Thyroid medications are goldilocks hormones — they need to be used in just the right dose — and there are risk factors of being overmedicated.
Testing TSH, T4, T3, and the two most common Hashimoto’s antibodies (TPO and TG antibodies — you can read more about such tests here) is an important part of ensuring that the lifestyle changes you are making are both safe and helpful. 🙂
If your doctor is ordering these thyroid labs for you, be sure to request a copy so that you can see them for yourself and ensure that they are interpreted correctly. If you aren’t able to use your physician for ordering, or have a high deductible insurance plan like I do, you may also wish to self-order your own thyroid monitoring labs. I recommend the Ulta Labs thyroid panel for monitoring your progress, which can be ordered anywhere in the U.S. (some, but not all, insurance companies may reimburse you for self-ordered labs, please be sure to check with your plan).
The Takeaway
The adrenals are two small glands that release very important “stress hormones,” which impact many functions throughout the body, including stress tolerance, inflammation, blood sugar, and body fat. When the body is under constant stress, the adrenal glands eventually become overwhelmed and desensitized, resulting in adrenal dysfunction.
Supporting the adrenals is one of the first things I recommend for all of my clients, as adrenal dysfunction is almost always a factor in Hashimoto’s. It can result in many of the symptoms we often perceive to be a result of our thyroid condition, like fatigue, feeling overwhelmed, trouble concentrating, and a decreased ability to handle stress.
By taking a root cause approach, including getting more rest, balancing blood sugar, reducing stress and inflammation, replenishing nutrients, and building resilience with supplements (like the ABCs in Rootcology’s Adrenal Support), we can help to reduce the impact of stress on the adrenals… and reduce or eliminate many of those symptoms!
I wish you the best of luck on your healing journey!
P.S. You can also download a free Thyroid Diet Guide, 10 thyroid-friendly recipes, and the Nutrient Depletions and Digestion chapter of my first book for free, by signing up for my weekly newsletter. You will also receive occasional updates about new research, resources, giveaways, and helpful information.
I love interacting with my readers on social media, and I encourage you
to join my Facebook, Instagram, TikTok, and Pinterest community pages to stay on top of thyroid health updates and meet others who are following similar health journeys. For recipes, a FREE Thyroid Diet start guide, and notifications about upcoming events, be sure to sign up for my email list!
References
[1] Thau L, Gandhi J, Sharma S. Physiology, Cortisol. In: StatPearls. Treasure Island (FL): StatPearls Publishing; August 29, 2022.
[2] Cook SB. Current Controversy: Does Adrenal Fatigue Exist?. Natural Medicine Journal. 2017;9(10).
[3] Mariotti A. The effects of chronic stress on health: new insights into the molecular mechanisms of brain-body communication. Future Sci OA. 2015;1(3):FSO23. Published 2015 Nov 1. doi:10.4155/fso.15.21; Harvard Health Publishing. Understanding the stress response. Harvard Health Publishing. https://www.health.harvard.edu/staying-healthy/understanding-the-stress-response. Published March 2011. Updated March 18, 2016. Accessed February 25, 2018.
[4] Cook SB. Current Controversy: Does Adrenal Fatigue Exist?. Natural Medicine Journal. 2017;9(10).
[5] Nicolaides NC, Vgontzas AN, Kritikou I, Chrousos G. HPA Axis and Sleep. In: Feingold KR, Anawalt B, Boyce A, et al., eds. Endotext. South Dartmouth (MA): MDText.com, Inc.; November 24, 2020.
[6] Gierach M, Gierach J, Skowrońska A, et al. Hashimoto’s thyroiditis and carbohydrate metabolism disorders in patients hospitalised in the Department of Endocrinology and Diabetology of Ludwik Rydygier Collegium Medicum in Bydgoszcz between 2001 and 2010. Endokrynol Pol. 2012;63(1):14-17.
[7] Sprague JE, Arbeláez AM. Glucose counterregulatory responses to hypoglycemia. Pediatr Endocrinol Rev. 2011;9(1):463-475.
[8] Hannibal KE, Bishop MD. Chronic stress, cortisol dysfunction, and pain: a psychoneuroendocrine rationale for stress management in pain rehabilitation. Phys Ther. 2014;94(12):1816-1825. doi:10.2522/ptj.20130597
[9] Symptoms & causes of adrenal insufficiency & addison’s disease. National Institute of Diabetes and Digestive and Kidney Diseases. https://www.niddk.nih.gov/health-information/endocrine-diseases /adrenal-insufficiency-addisons-disease/symptoms-causes. Published September 2018. Accessed December 14, 2022.; Munver R, Volfson IA. Adrenal insufficiency: diagnosis and management. Curr Urol Rep. 2006;7(1):80-85. doi:10.1007/s11934-006-0046-5
[10] Munver R, Volfson IA. Adrenal insufficiency: diagnosis and management. Curr Urol Rep. 2006;7(1):80-85. doi:10.1007/s11934-006-0046-5
[11] Cadegiani F, Kater C. Adrenal fatigue does not exist: a systematic review. BMC Endocr Disord. 2016;16(1). doi:10.1186/s12902-016-0128-4.
[12] Ohtsuka Y. Food intolerance and mucosal inflammation. Pediatr Int. 2015;57(1):22-29. doi:10.1111/ped.12546
[13] Furman D, Campisi J, Verdin E, et al. Chronic inflammation in the etiology of disease across the life span. Nat Med. 2019;25(12):1822-1832. doi:10.1038/s41591-019-0675-0
[14] Terciolo C, Dapoigny M, Andre F. Beneficial effects of Saccharomyces boulardii CNCM I-745 on clinical disorders associated with intestinal barrier disruption. Clin Exp Gastroenterol. 2019;12:67-82. Published 2019 Feb 11. doi:10.2147/CEG.S181590
[15] Todorova V, Ivanov K, Delattre C, Nalbantova V, Karcheva-Bahchevanska D, Ivanova S. Plant Adaptogens-History and Future Perspectives. Nutrients. 2021;13(8):2861. Published 2021 Aug 20. doi:10.3390/nu13082861
[16] Panossian A, Wikman G. Effects of Adaptogens on the Central Nervous System and the Molecular Mechanisms Associated with Their Stress-Protective Activity. Pharmaceuticals (Basel). 2010;3(1):188-224. Published 2010 Jan 19. doi:10.3390/ph3010188
[17] Pan L, Jaroenporn S, Yamamoto T, et al. Effects of pantothenic acid supplement on secretion of steroids by the adrenal cortex in female rats. Reprod Med Biol. 2011;11(2):101-104. Published 2011 Dec
[18] Valdés F. Vitamina C [Vitamin C]. Actas Dermosifiliogr. 2006;97(9):557-568. doi:10.1016/s0001-7310(06)73466-4
[19] Sharma AK, Basu I, Singh S. Efficacy and Safety of Ashwagandha Root Extract in Subclinical Hypothyroid Patients: A Double-Blind, Randomized Placebo-Controlled Trial. J Altern Complement Med. 2018;24(3):243-248. doi:10.1089/acm.2017.0183
[20] Armanini D, Fiore C, Mattarello MJ, Bielenberg J, Palermo M. History of the endocrine effects of licorice. Exp Clin Endocrinol Diabetes. 2002;110(6):257-261. doi:10.1055/s-2002-34587
[21] Ji Z, Fan Z, Zhang Y, et al. Thiamine deficiency promotes T cell infiltration in experimental autoimmune encephalomyelitis: the involvement of CCL2. J Immunol. 2014;193(5):2157-2167. doi:10.4049/jimmunol.1302702
[22] Dube SR, Fairweather D, Pearson WS, Felitti VJ, Anda RF, Croft JB. Cumulative childhood stress and autoimmune diseases in adults. Psychosom Med. 2009;71(2):243-250. doi:10.1097/PSY.0b013e 3181907888; Jung SJ, Kang JH, Roberts AL, et al. Posttraumatic stress disorder and incidence of thyroid dysfunction in women. Psychol Med. 2019;49(15):2551-2560. doi:10.1017/S0033291718003495
Note: Originally published in October 2016, this article has been revised and updated for accuracy and thoroughness.


 Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Trust me you’re not alone!
Stella – thank you for following this page. I‘ve found that an inability to manage stress is often at the core of the condition. Most people can trace back the development of Hashimoto’s and autoimmune conditions to a particularly stressful time period. Stress is inherent, and it’s how we handle our stress that matters. I recommend self-management stress-reducing habits like mindfulness, yoga, and meditation. Meditation has specifically been found to be helpful in building resilience to stress. If you have a history of childhood trauma like I do, your stress response could be severely impacted, leading you to overreact and get into a ‘fight or flight’ state at the easiest provocations. I recommend therapies like the self-guided tapping, self-help books, neurofeedback or therapist guided EMDR to reset your stress response. https://thyroidpharmacist.com/articles/are-your-adrenals-sabotaging-your-health/
There are several HPA stress profile tests to choose from when you click on the link you provided. Which one do you recommend?
Amy – thank you for reaching out. It is your choice to use the basic HPA Stress Profile 201A or the more complex with all the hormones, the 205-CAR. If you have any other questions about the testing please feel free to email my team at info@thyroidpharmacist.com and they will be happy to help. <3
Thank you for sharing your story, and I hope that you have found a doctor that will listen, and I am glad that you are taking charge of your own health. Keep me posted on your progress
Thank you for writing, and I wholeheartedly agree with you. I am so glad that you have found a compassionate and caring acupuncturist. I had a wonderful experience with mine as well. Hope that this site has been helpful in your journey 🙂
Find a doctor that will listen. Work on balancing your blood sugar, get plenty of rest. Check out my book for a whole chapter on how this works and what you can do about it. It does get better, I promise!
It’s time you Breathe, Believe and know you are Whole.
Yes… We all lived together… I have found out how he has used these last 2 crazy years to turn everyone against me. Would not touch me for over a year because of the weight gain. My normal weight 118 for 30 years.. Lost all but 20 lbs, now he’s interested… Now I want something more in every sence of the word!!! We have been married 24 years, 6 years together before.. I have never been more hurt and have no idea what was ever real?
Thank you for writing. I can appreciate the effect the thyroid can have on the whole body. Many patients are unfortunately under-dosed on thyroid meds, so I would start there…please take a look at the archives on this blog for helpful strategies as well as my book.
Thanks for writing, many of us with autoimmune conditions tend to be that way. This characteristic unfortunately contributes to the vicious cycle. I had to make myself a list and learn how to relax. I still have to remind myself now. Not to get all philosophical on you, but it did help me to do some soul searching and asking myself why I always needed to be so busy and active. I am more scientific then spiritual, but read a book called the “Healing Code” and thought it had some good points about the effect of stress and how to reprogram yourself. Hope that helps and I wish you all the best in your journey. Keep me posted 🙂
Unfortunately we need to take charge of our own health, my hope is that this site and my book will give you the tools and inspiration to do so.
Is there a reason the article doesn’t open, can I have access to it? You mention that some people are sensitive to the night shade’s, how do I find out if I am or not?
Rebecca – thank you for following this page. I am so sorry you are having technical issues. Please email my team at info@thyroidpharmacist.com and they will be happy to help you. 🙂
Stabilizing your blood sugar as well as Selenium would be a great place to start. I have a ton of other strategies in my book that may help. Here’s a post on Selenium- https://thyroidpharmacist.com/1/post/2013/06/nutrient-depletions-in-hashimotos-part-i-selenium.html and anxiety- https://thyroidpharmacist.com/1/post/2013/06/are-you-going-crazy-or-is-it-just-your-thyroid.html
Message to all, if your doc will not listen to you, find another one, and another until you find the right one to recognize your needs.
Would you mind sharing what helped your hair stop falling out? My symptoms are excessive hair falling and fatigue. Fatigue is improving, but what can I do to stop the hair loss? Many thanks.
Meredith – thank you for following this page.
Hair loss is a distressing symptom experienced by women with Hashimoto’s. For women, our hair represents our femininity, and losing our hair is a constant reminder that something is off and that we are not well. Have you read these articles?
HASHIMOTO’S AND GETTING YOUR HAIR BACK
https://thyroidpharmacist.com/articles/hashimotos-and-getting-your-hair-back/
HAIR LOSS AND YOUR THYROID
https://thyroidpharmacist.com/articles/hair-loss-and-thyroid
Selected text
https://thyroidpharmacist.com/articles/hashimotos-and-low-stomach-acid
I just did an adrenal test with ZRT. It shows I have some issues, but I’m having a hard time reading all the results. I wish I would’ve seen your comment about them before I did this. I’ll give BioHealth a try. Thanks for posting.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target 🙁 We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system.
This sounds exactly like me! Except I also have celiac’s disease. I recently went to Mayo Clinic because my adrenals are so enlarged, both of them. Mayo doesn’t believe in adrenal fatigue and put me on an estrogen patch and progesterone, horrible, and I was totally bloated! I quit both after 3 weeks. I then went to a naturopath MD in Chicago, and she gave me cortisol(all natural) that I took for 2 weeks along with nature thyroid. I couldn’t figure out why I felt so awful, turned the cortisol bottle over and it contained 3 different formas of wheat. I am just furious and sick, right now have a horrible sinus infection. I’ve had all blood tests and saliva tests, all came back abnormal. What do I do???
Hi Helen,
I am faced with the same situation. The smallest amount of thyroid medications make me crash. How much Adrenal Cortex did you take? Did you still need to take thyroid medications after you had healed your adrenal glands.
Many thanks
Lucy
Lucy- thank you for following! <3 Did you know thyroid tissue can regenerate? However, the rate at which it does is not always predictable. Thus, some are able to stop the autoimmune attack on their thyroid and regain normal thyroid function. Others can reduce the dose of medications, and others will need to stay on the medications indefinitely. Reversing Hashimoto's means different things to different people. For some, it means a reduction in symptoms, and for others, it means a reduction in your antibodies. I had both. Here a few articles that might be helpful for you:
IS IT POSSIBLE TO RECOVER THYROID FUNCTION IN HASHIMOTO'S
https://thyroidpharmacist.com/articles/is-it-possible-to-recover-thyroid-function-in-hashimotos
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
It’s important to discuss AI thyroid conditions but what about us who have hypothyroidism but no antibodies? Would you still give the same recommendations? I’ve tried T4, combination of T3/T4 and now T3 but my body don’t seem to utilize it. My saliva results are fair but I think it’s some sort of inflammation but it’s so hard to figure it out. My holistic doctor doesn’t have a clue any more what to try next.
Do you have PTSD or unresolved trauma? I’d recommend starting there…
Thanks so for sharing this important info. I don’t know what to say, but I have 3 excellent docs working with me and no one can get me to sleep at night- no one! I get these insane bouts with anxiety (not too sure where they come from), and I get wired and can’t sleep. Actually, most nights I can fall asleep, but I wake up, sometimes a lot, sometimes it’s once, but it’s deadly and I NEVER fall back to sleep. I know my adrenals are KICKED, because I’m like a zombie all day long, but I just can’t find the correct adoptagen. I have tried MANY, with doctor support. I have not tried the one you did, but I am always wiling to. I also wondered if low iodine would have anything to contribute to this issue as well! Please, any suggestions would be greatly appreciated. I am at my wits end!
Could this be causing inflammation? My NP didn’t think so.
I couldn’t find the article referenced in the book. The website stopped linking to articles written in that year. I have had thyroid and adrenal problems for 20 years.
Hey Dr. Wentz, I have Hashimoto’s and high cortisol. A long time ago I tried Thyroid Support from Gaia that contains L-Tyrosene and it made me feel overly anxious. If the Daily Stress Formula from Pure Encapsulations contains L-Tyrosene (250mg), is that a good idea? Are there any other adaptogen recommendations that don’t include it? Thanks so much!
Ilya- Not everyone will need every single supplement! In fact, I believe that most nutrients should come from the diet, this is why I always list food sources for most of the nutrients, vitamins, minerals and probiotics that are depleted in Hashimoto’s in the book and on the blog. However, some may require/prefer supplements and the supplements on the website are a resource for those that do. I recommend getting tested for deficiencies to determine your need for a supplement as instructed in the book and blog. I also don’t recommend starting multiple supplements all at once. I recommend starting one at a time and then adding another a week or so later once it has been confirmed that the first supplement is not causing any harm.
I do have a full supplements chapter in my book. Have you checked it out? Not everyone should be taking every supplement and the book will help uncover your root cause. This will help you figure out your supplementation.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
My ft3 was at 2.51, my free t4 at 0.96, my tsh at 9.42. I have gotten the tsh down three points by just dropping gluten, sugar and caffeine. My question is, would I be a good candidate for your adrenal supplement? My concern is that Ashwagandha can up my t4, and don’t I want it to drop, and my t3 come up??
Thanks
Tiana – thank you for following this page. I wish I could give you more direct advice but, each person will react differently. I would advise you to ask your personal pharmacist or a trusted clinician who’s care you are under. I am not able to respond directly to these types of questions here. Adaptogenic herbs include ashwagandha, astragalus reishi mushroom, dang shen, eleuthero, ginseng, jiaogulan, licorice, maca, schizandra, spikenard, and suma. These are examples of herbs that may increase the body’s ability to resist stress, and have been helpful in relieving adrenal dysfunction when used in combination with vitamins and minerals. Not everyone will need every single supplement! In fact, I believe that most nutrients should come from the diet, this is why I always list food sources for most of the nutrients, vitamins, minerals and probiotics that are depleted in Hashimoto’s in the book and on the blog. However, some may require/prefer supplements, and the supplements on the website are a resource for those that do. I recommend getting tested for deficiencies to determine your need for a supplement as instructed in the book and blog. I also don’t recommend starting multiple supplements all at once. I recommend starting one at a time and then adding another a week or so later once it has been confirmed that the first supplement is not causing any harm.
I do have a full supplements chapter in my book. Have you checked it out? Not everyone should be taking every supplement, and the book will help uncover your root cause. This will help you figure out your supplementation.
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8…
Hashimoto’s Protocol
https://thyroidpharmacist.com/protocol
Dear Dr. Thank you very much for your post. The last year my partner was diagnosed with Hashimoto and two months later a thyroid carcinoma, she was operated, extracted the whole thyroid and received radioactive iodine. Now, she are taking Euthirox 100 mg. She still hypothyroid and always has cold and very tired (but not sleep good!), also have tachycardia and irritable bowel. Recently we start the diet that you recommended and she feeling better. I would like to know if for she applies this information of adrenal fatigue? Although she hasn’t thyroid? I think her brain has not yet learned that her thyroid is not! Thank you very much!
Ismar – thank you for following this page. How wonderful and caring that you are looking out for your partner. <3
Please, understand that due to liability issues, I am unable to answer specific medical questions.
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
I am very touched by all the emails. These interactive issues are complex but Dr Wentz has outlined step by step ideas to begin with.
Personally I believe anyone with an autoimmune condition could just try some of the diet changes, you might get a big surprise. Feeling better is good who knows if a full remission is possible or not. Some people have had them!
Get a notebook. I started with getting dairy and wheat out of my diet, getting more sleep and walking briefly in the morning or when I can.
Try to get a routine and note how you feel. I take multivitamins with lots of B vitamins, fish oil, vitamin D and minerals. If I miss the multivitamin, I get teary and reactive.
Record little pleasures- plant blooming in the garden, seeing a baby, be kind to yourself and model how you want to be treated. Say no and take time for yourself, let others take more responsibility.
People, even our loved ones can’t listen to non stop complaining. If they don’t know what to do they may react by being unsupportive because they feel helpless. Ask for things which would help.
I want to share dinner making- which night could you do?
Lets go to …..something relaxing and fun. Lets watch…..
Find people who understand, read these blogs. Ask for the tests you need at the Drs. I have found a helpful naturopath. She has given be alkylysed minerals to take and they helped to remove excess copper from my system. Filter your water. After 1 month I noticed a big improvement.
I thought I was alright to eat some 100% rye bread but I’m not feeling good again. I get mucous in my throat if I have any dairy.
The pieces to your puzzle come to you gradually. If you’ve observing and noting every day, you’ll work out the mystery with help!!
I got a little off track again and overwhelmed but now I’m going to make a big list of all the things I am doing and new ones I’m trying when I can.
I still need another thyroid test. I had one a year ago so that will make a good comparison.
If you begin to take responsibility for your health and stick to it, family and friends will notice your resolve, you will probably feel better.
Lesli – thank you for following this page and for sharing. <3
I am really hoping to build a database of testimonials to submit to a medical journal. I would very much love if you submitted your story. You would be helping so many. Would you consider doing this?
http://www.thyroidpharmacist.com/testimonial
I have been tested and I do not have Hashimoto’s but I am having problems regulating my thyroid. I Am a flight attendant and travel overseas . My adrenals are blown and managing stress and sleep is a challenge. I have always had a healthy diet but it is difficult while traveling. Do you have any advice for me please .
Lisa – thank you so much for following this page.
Did you know that if you live in the United States, Australia, Europe and most developed countries that add iodine to the salt supply and take thyroid medications, there’s a higher probability that you do have Hashimoto’s?
Depending on the source, estimates are that between 90-95% of those with hypothyroidism have Hashimoto’s.
But most doctors will never tell people that they have Hashimoto’s, or that their own immune system is attacking their thyroid. People are told that their “thyroid is sluggish”, and that these things happen with age and “Just take this pill, you’ll be fine.” I hope you check out these articles that I wrote.
ARE YOU DOING EVERYTHING FOR YOUR THYROID BUT NOT YET WELL?
https://thyroidpharmacist.com/articles/are-you-doing-everything-for-your-thyroid-but-not-yet-well/
DO YOU HAVE HYPOTHYROIDISM OR HASHIMOTO’S OR BOTH?
https://thyroidpharmacist.com/articles/do-you-have-hypothyroidism-or-hashimotos-or-both/
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well.
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
The stress formula you recommend (by pure encapsulations) can be VERY dangerous
to someone with Hashimoto’s. Lemon balm is a big no no especially when it comes to a balanced immune system.
Hello,
I tried various combination adaptogenic herbs this year and they give me insomnia, causing me to wake up between 2-4am and unable to get back to sleep. This starts on day 2 of treatment and persists for months after discontinuation.
I have low cortisol and am thinking of taking Dr James Wilson’s Adrenal Rebuilder (adrenal and other glandular extracts with the hormones removed). In his book, he recommends eating protein before bed to prevent waking up with adrenaline due hypoglycemia caused by low cortisol. I eat a handful of walnuts before bed and that does prevent the adrenaline surge but does not prevent me from waking up and having too many thoughts running through my head. At this point, it may just be anxiety from insomnia that is preventing me from getting back to sleep. I am sleeping later, like 4-5am instead of 2-3am. In the book he also recommended taking an adrenal cell extract with cortisol before bed to prevent waking up due to low cortisol, or even exercising before bed. I don’t have any cell extracts yet but I tried exercising and that did help a bit but I still had restless sleep. I tried licorice root tea and that helped a bit but I still couldn’t fall back asleep.
I am doing your 90-day Hashi’s protocol and just started Adrenal Program but am hesitant to try the adaptogens due to previous ill experience with them. I have borderline low hypothyroid so went on NDT but RT3 went higher so went on T3-only med but it gave me brain fog, low energy and anxiety so I stopped taking it as well (I had just started them and was on really low doses for only a few months). My ferritin went from 90 to 40 while on NDT 1/2 gr daily x 1 mo then Cytomel 5mcg BID x 1 mo. Thyroid antibodies are negative.
My AM serum cortisol has been in range of 6-9 in past year. I had SIBO and Candida for a few years and did a rigorous program to eradicate them, which I believe resulted in my adrenal fatigue (or just worsened it severely). My progesterone is low so I’ve been on oral Progesterone, started with 25mg daily on days 1-28 then increased to 40mg daily on days 1-28 after my last trial of adaptogens. I have also been increasing my melatonin dose from 1mg qhs to 5mg qhs.
Thanks for writing your book. I lost a few pounds of water weight (toxins?) during the liver flush and am hopeful that the adrenal program, in addition to Dr Wilson’s supplements, will help tremendously. I probably won’t do the GI program since I did one last year with the SIBO/Candida program and I get anxiety from glutamine (even Mag Glycinate).
Yours in healing,
Sierra
Sierra – thank you for your support! <3 For questions pertaining to the supplements and protocols please contact my team at info@thyroidpharmacist.com and they will be happy to help you. 🙂
Hi Izabella, I was diagnosed with hypothyroid three years ago, over that time my doctor would call me back in for lab work redo because my liver enzymes were elevated from time to time. Each time labs would show a decrease and wouldnt say anything else. Recently, I was applying for life insurance but wouldnt get coverage becuz liver enzymes were elevated. I went to a specialist, he tested me for eveything possible all test read negative but liver enzymes were still slightly elevated and he had no diagnosis for it. I am on a paleo diet and no gluten or processed sugars, no soy etc… I have your first book and because of it I was able to reverse hypothyroid but still a have this liver issue with no diagnosis. Hope you could shed some light. I do use honey at times for sweetener in my green smoothies and blueberries. Thank You
Kathy – thank you so much for your support! Here is an article you might find helpful. HOW SUPPORTING THE LIVER IS KEY TO RECOVERING FROM THYROID DISEASE
https://thyroidpharmacist.com/articles/support-liver-recover-from-thyroid-disease/
Any suggestions on Generalized Miasthenia with Anti Musk antibodies?
Thank you.
Linas
Linas – thank you for following this page. I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Hi Izabella
I was diagnosed with Hypothyroid about a year ago. Nothing was tested except TSH (16). I was put on levothyroxine and have felt worse ever since. I have taken Levothyroxine, Synthroid, T3, Amour and now Tirosint over the last year. I also have hashimoto’s which I insisted they test for (800). The thyroid medications have only made me feel worse over the last year and I am wishing I would have never started them as my originally complaints were weight gain, tired and swollen. Now I have hot flashes, night sweats, headaches, brain fog, panic attacks, dizziness and an over sense of going crazy! I would like to stop the thyroid medication but have a fear that I will send myself into the ER. I have been gulten, soy, dairy, caffeine free for 50 days and take selenium, vitamin E, B12, Vitamin D3, probiotic. I am wondering if I ever needed this medicine in the first place and can these other supplements help me reverse my condition. I am also waiting on tests for food sensitivity and female hormones. Thanks!
Sarah – thank you for following this page. The most common triggers in Hashimoto’s are: nutrient deficiencies, food sensitivities, intestinal permeability (leaky gut), stress, an impaired ability to get rid of toxins and in some cases, infections. Optimizing your health starts with food. Figuring out which foods nourish you, and which ones cause you harm is the single most important thing you can learn in your health journey.
I’ve found that recognizing and eliminating reactive foods can be a life-changer for most people with Hashimoto’s.
Reactive foods trigger an inflammatory response in the GI tract, leading to malabsorption of nutrients (gluten sensitivity in particular has been implicated in causing a Selenium deficiency, a well known risk factor for Hashimoto’s), and can also produce intestinal permeability whenever they are eaten.
Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods that they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are some articles which I wrote:
BEST DIET FOR HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/best-diet-for-hashimotos-hypothyroidism
TAILORING YOUR THYROID DIET
https://thyroidpharmacist.com/articles/tailoring-your-thyroid-diet-to-your-needs
DAIRY AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/got-hashimotos-you-may-want-to-reconsider-dairy
Dr. Wentz,
I’ve read most of your books, eat according to the SIP diet. My adrenal are low functioning, I have difficulty taking my thyroid meds and I often have stress responses to supplements especially, all B vitamins.
It’s all maddening.
The information regarding accupunture sounds great will certainly look into that as an alternative.
Keep the faith ladies. Remember, you are while perfect and complete.
Wow, that should have said, whole, perfect and complete! ?
Glenna – thank you for following this page. Having Hashimoto’s can feel very stressful. Having out of range thyroid hormones, adrenal fatigue, negative food sensitivities and low nutrient levels can lead to feelings of anxiety, hopelessness and stress. Treating these issues one at a time is the best plan of action. You can recover and regain your health! My new book Hashimoto’s Protocol is a step by step guide to the interventions that helped 80% of the people 80% of the time. I hope you check it out.
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Wow…. I knew it wasn’t all in my head and that something is wrong in my body! I just didn’t know what. My thyroid was so low one year that I started having severe panic attacks. As in I shook so badly I looked like I was having a seizure. I couldn’t sleep for days. Found out my thyroid was so low that I was close to going into a coma.
It took 2 years but the correct synthroid dosage was found. But now I’ve become anemic, b12 deficient, and I’m still low on vitamin d even though I take the highest prescription amount. They can’t give me anymore. I’ve been feeling like my body has been shutting down on me and I’ve been so lost. I also have been obsessively craving salt and chips. Even that part was on this page! And now thanks to you I now have a good idea of what’s going on! My entire adrenal system is haywire right now! Thank you thank you!
Now I just need to find a good specialist and/ or endocrinologist near Omaha, NE. Any recommendations?
Laura – thank you for following this page. I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Thank you so much for all this. I hate being sick soooooooo much!!! I’m terrified about this adrenal stuff. I am a competitive athlete. If I have what seems to be stage 2 adrenal fatigue, do I have to stop training? (I race bicycles.) I haven’t found a whole lot of information online about endurance training and adrenal fatigue. Can I ride easy – keeping my heart rate low? Is this going to put me back? What can I do to stay fit – or at least not lose all of my fitness??? Thank you, Sharon
Sharon – you are very welcome! I would recommend anyone embarking on a program of exercise starts slowly and progresses at their own pace. Exercise can be very healthy, but for people with Hashimoto’s it can create stress. Stress causes our adrenals to pump out extra hormones, and shifts our body from a relaxing, digesting, healing state to a fight or flight state. The body’s energy is shifted from doing “useless” things like growing beautiful hair, metabolizing, making hormones, digesting and repairing itself, and instead, all of the body’s resources are reserved to make cortisol and adrenaline that is pumped through our veins so that we can keep going. Eventually, we run out of nutrients that are required for proper adrenal function and we get to a state of adrenal fatigue. This is when our body is no longer able to heal itself and we feel drained.
Replenishing nutrients and using adaptogens, that balance out the adrenals can be helpful for everyone. The Daily Stress Formula from Pure Encapsulations contains nutrients and adaptogens that can help your body repair itself.
ADRENAL SUPPORT
https://www.rootcology.com/products/adrenal-support
thank you, I purchased 4 of your books and am just now reading them.
I have hashimotos and adrenal fatigue. Finding a competent doctor in the south is most difficult. they cannot read the tests! only TSH. I have asked 3.5 years now to have my adrenals improved only to be told adrenal glands are unnecessary.
My doc cannot read or interpret blood tests. Saw a low TSH and reduced my synthroid and stopped T3. told me to see endocronologist. New patients takes 4 months to get in. My naturopathic has me on vitamins for adrenals now.
I went VEGAN 1.5 months ago and changed blood panel.
Pam – you are very welcome! I appreciate you sharing your journey. <3 Most people feel best with a TSH of around 1 or lower and with a Free T4 and Free T3 in the upper half of the range. It is expected that your TSH will be very suppressed when optimal on NDT medication. How much thyroid replacement therapy is needed is unique and different for each person, so it's important to work with a functional medicine practitioner or a doctor, who can closely monitor your dosage and your progress.Every six weeks is usually a good schedule for testing your thyroid hormones. Here are the tests you need for diagnosis. Most endocrinologists don't run them all so you will have to request them. Make sure to request a copy of your labs as well.
Top 10 Thyroid Tests and how to Interpret them.
https://thyroidpharmacist.com/articles/top-6-thyroid-tests
If you cannot find a Functional Medicine practitioner in your area, it is possible to work with a
practitioner remotely via Skype or some other online video platform. Here are some links that might help:
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
I was diagnosed 8 years ago with Addisons disease (wrongly) as I wasn’t able to produce cortisol. My levels were virtually zero. After being put on Cortisone daily I actually got worse and worse to loosing the use of my arms and legs with zero strength. Thankfully a Dr was clever to test me for CIRS (mold toxicity) and Lymes disease, both of which I had which was the cause of producing no cortisol. Now after getting out of the moldy environment and numerous diet changes, weekly Vit c IV’s, I now have a life back and my body is now producing it’s own cortisol and I have been able to come off cortisone steriods. There is Hope, even though it is hard to see it sometimes. Never give up and always Look For The Root Cause.
Kim – thank you for sharing your journey! My mission is to collect 10,000 success stories with the hope of submitting them to a medical journal in the future. Understandably, you are probably very busy, but if you have some time, please do you mind sharing your full story with me here at this link? https://thyroidpharmacist.com/testimonial/
These stories will go a long way in helping others who are going through a similar journey to yours. Thank you for your consideration!
Sorry for the delay but I have finally submitted my story. I just want to ask whether we are ever notified when and where our stories are published if they are. Thanks
KIM – thank you so much for sharing you journey with me! I am looking forward to reading your story. <3 Please email my team at info@thyroidpharmacist.com and they will be able to give you the publishing information.
hello. I have had thyroid problems for 15 years or more. I am on armour. It wasnt until two years ago that i landed in the hospital with severe health issues, kidney stones, kidney, bladder and uti infections. Was at that time diagnosed with Type II Diabetes. I also was told i had hashimotos. 7 years ago i had surgery to repair a hyatal hernia. it was in the area of the diaphragm, upper stomach and lower throat area. I have been in pain ever since. It affects my pulse rate which can be up to 180. I also know it is affecting my Diabetes. the drs cant see to find what is causing the pain. although they suspect it may be neurological. took gabapentin and helped to reduce the pain considerable….I was wondering can Hashimotos be contributing to the pain? Im am even considering CBD oil or mecial marijuana, due to being unable to take prescription pain meds. Thank you
Brenda – thank you for reaching out and sharing your journey. <3 I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms. I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It's a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/pages/clinician-database
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
http://www.thyroidpharmacistconsulting.com/recommended-compounding-pharmacies.html
wait… don’t you need iodine for thyroid health? Wouldn’t iodized salt be better for thyroid issues?
Jill – thank you for reaching out. I am very hesitant in recommending iodine in Hashimoto’s. Although iodine serves as fuel for our thyroid and is very important in iodine deficiency hypothyroidism, Hashimoto’s is a different mechanism. It’s like pouring gas into an engine that’s on fire… that’s essentially what’s happening in Hashi’s, thyroid inflammation. Adding iodine to the mix before putting out the fire and fixing the engine may result in further damage to the thyroid. In those with a predisposition to autoimmunity, this has been documented time and time again, in animal and human studies.
I have spent 4 years researching about this issue, and have seen too many people suffering the consequences of adding iodine too soon. My approach is, let’s fix the engine first (usually a gut issue), and then add the fuel once we know that the engine is no longer on fire. Hope that you will check out my books. I do have a chapter on the iodine controversy that references numerous studies as well as the work of Abraham and Brownstein. Here are the links to my books :
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
You may also find this article helpful as well:
IODINE AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/iodine-hashimotos/
I jumped the gun a little on my previous post…
I have been on medication for hypothyroidism for over ten years, three years ago I was diagnosed with Hashimoto’s (who knows how long I’ve actually had either of them). I have always struggled with my weight and other little symptoms here and there. Right after my diagnosis, I tried the AIP diet… to no avail – I didn’t feel ANY different. Therefore, I didn’t think much of my diagnosis until I came home from a trip to Thailand and felt like I just couldn’t kick the jet-lag… and here we are four months later – still feeling jet-lagged. I thought maybe it was just macros so I tried that, as well as introducing some pretty major weightlifting and neither my weight or energy budged.
I’m diving in myself now – I read a bit a few years ago and am getting back in since I am desperate. I’ve just eliminated dairy, gluten and soy and am feeling a bit better – it hasn’t even been a week yet but I am so excited to finally figure things out – for myself since there aren’t any doctors who have seemed to help. After much research I decided on what supplements I was going to try – but then I read this and now I’m confused! Does the Adrenal Support have enough of the Benfo-Max? I had one of each in my cart but would taking Benfo-Max in addition to this be too much?
Meg – thank you for reaching out and sharing your journey. I am happy to hear you are diving in and taking charge of your health! <3 The Adrenal Support does not contain thiamine. Here are some articles you might find helpful.
https://thyroidpharmacist.com/articles/thiamine-and-thyroid-fatigue/
https://thyroidpharmacist.com/articles/12-strategies-overcome-hashimotos-fatigue/
could you please remove my last name from the previous comment, if you don’t automatically do so. I looked at other comments and only saw first names, so assumed you did. but it looks like my full name will appear. Thank you.
Sandy – thank you for reaching out. I have removed the message with your last name. <3 For questions about the supplements please email my team at info@thyroidpharmacist.com and they will be happy to help you.
Hi,
Will this supplement work for low cortisol?
Thanks.
Claire – thank you so much for reaching out. Adaptogenic herbs such as ashwaghandha, rhodiola, holy basil, astragalus reishi mushroom, dang shen, eleuthero, ginseng, jiaogulan, licorice, maca, schizandra, spikenard, and suma are examples of herbs that may increase the body’s ability to resist stress, and have been helpful in relieving adrenal dysfunction when used in combination with vitamins and minerals. Not everyone will need every single supplement! In fact, I believe that most nutrients should come from the diet, this is why I always list food sources for most of the nutrients, vitamins, minerals and probiotics that are depleted in Hashimoto’s in the book and on the blog. However, some may require/prefer supplements, and the supplements on the website are a resource for those that do. I recommend getting tested for deficiencies to determine your need for a supplement as instructed in the book and blog. I also don’t recommend starting multiple supplements all at once. I recommend starting one at a time and then adding another a week or so later once it has been confirmed that the first supplement is not causing any harm.
I do have a full supplements chapter in my book. Have you checked it out? Not everyone should be taking every supplement, and the book will help uncover your root cause. This will help you figure out your supplementation.
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
I have a 15 yr old daughter recently diagnosed with Hoshi. Her symptoms are more hyper than hypo with a resting pulse of 115-125. Her T.Peroxidase is 791.8 Thyroglobulin 18. She definitely needs adrenal support but can’t swallow pills, are there liquid, chew-able or dis-solvable options? I have her on a B-12 and D-3 but the mg are low. After reading and more reading I found liquid selenium and Zinc but now I don’t want to start those until we get new blood work. It kills me to see my daughters world turned upside down and I just want to help her function. Everything I find is in a pill form.
Pauline – thank you for reaching out and sharing your daughters journey. My heart goes out to you both. <3 For children, teens, (and adults), I always recommend starting with the diet. Are they gluten, dairy, corn and soy free? Are they eating a nutrient dense diet with fermented foods? Implementing those changes can help many symptoms. For example, some cases of anemia can be helped by eating liver, others may resolve by going gluten free. Acid reflux is often caused by food sensitivities. Most of the interventions recommended in my book can be done with children, with the exception of the dosing of supplements. I do suggest that you work with a functional medicine doctor that is familiar in working with children (I only works with adults). I hope this helps!
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
I an having excessive sweating on one time or otherwise feeling very cold.I have hashimoto’s for about 6 years and have been taking levothyroxine,but I never feeled good, always depressed, severe weight gain, hair loss,i even stopped going to college. I asked my doctor to check my cortisol but he denied saying that that is not needed. Now I started having severe heart palpitations. Can you tell me which supplements should I start with?
Saba – thank you for reaching out. I am so sorry you are struggling with all of this. <3 I am not able to advise on what supplements would be appropriate for you and your specific health needs without a comprehensive health assessment. I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms. I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It's a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
COMPOUNDING PHARMACIES
https://thyroidpharmacist.com/database-recommended-compounding-pharmacies/
Hello, thank you for an informative article. I wanted to inquire about supplements and safety for breastfeeding. From what I have found ginseng is not recommended to take while breastfeeding. Is it safe to take adrenal supplements while breastfeeding (6 month old baby)? Thank you!!
C – thank you so much for following! <3 I do not recommend many of the supplements in my program while pregnant or nursing, as these things have the potential to pass through to the baby. That is not to say that they are necessarily unsafe, but I have not specifically researched each of the supplements' effects on pregnancy and nursing, so I am not be able to confirm their safety. I recommend either waiting to use the supplements or working with your practitioner who is more familiar with these things to discuss the safety of the supplements while pregnant or nursing.
I am bookmarking this article so I can come back to it and remind myself about relaxing. I certainly do have 2 modes, overdrive and off. I recently took my first covid shot. The next day, I experienced this feeling like I wanted to just sit and watch Gomer Pyle reruns. I did not feel sick, but told my friend I did not ever remember experiencing this. I was either remodeling the house or asleep! I was ready to report a side effect called laziness, but my friend said , just enjoy the moment. Hopefully I can come back to this article and try to meditate and just relax more. Thank you!
Jane – thank you so much for sharing. 💕 Most people can trace back the development of Hashimoto’s and autoimmune conditions to a particularly stressful time period. Stress is inherent, and it’s how we handle our stress that matters. I recommend self-management stress-reducing habits like mindfulness, yoga, and meditation. Meditation has specifically been found to be helpful in building resilience to stress. If you have a history of childhood trauma like I do, your stress response could be severely impacted, leading you to overreact and get into a ‘fight or flight’ state at the easiest provocations. I recommend therapies like the self-guided tapping, self-help books, neurofeedback or therapist guided EMDR to reset your stress response. I hope you will keep me posted on your progress.
Hi Izabella Wentz!
Can extreme hunger also be a symptom of adrenal issues?
Lisa – thank you for reaching out. It can be. Our adrenals regulate blood sugar. ❤️ Balancing blood sugar is always one of the top things I recommend to anyone who is hoping to overcome autoimmune thyroiditis (and adrenal fatigue). It was one of the first interventions I tried while working to heal my own thyroid condition, and it made a big difference for me. Here is an article you might find interesting: https://thyroidpharmacist.com/articles/blood-sugar-imbalances-and-hashimotos/
I have been sick for the last 5 years. In Aug 2020, I had my breast implants removed, after being told I had Breast Implant Illness. I am trying to heal my adrenals and address my Hashimoto’s. When I take my Armour thyroid (reduced to 15 mg) It causes symptoms of anxiety. I just can’t handle it. I have read that adrenal dysfunction can have something to do with not being able to tolerate NDT. Can this also be true of the gut? I have dysbiosis and candida. My functional nutritionist put me on MegaSporeBiotic, and I was supposed to get to 2 caps. I made it to one and I am trying to titrate the 2nd cap, but I am struggling with detox symptoms (my Functional Nutritionist just told me to keep trying, it has been 4 months). I make it 10-11 days and it is so bad I have to stop. I have read I have to address adrenals first. Is it common to address the adrenals before repairing the gut and tolerating NDT?
I don’t know how to overcome candida if I can’t tolerate herxheimer reaction? Have tried Charcol and Bind, but did not help symptoms.
Sarah – thank you for reaching out. ❤️ I’m so sorry you are struggling with all of this. Treating hypothyroidism without treating the adrenals is one of the biggest reasons people continue to feel exhausted despite receiving treatment with thyroid hormones. Stress seems to be a precursor to hypothyroidism. Additionally, taking thyroid hormones can actually help us clear out our adrenal hormones faster, which then leads to adrenal fatigue. So, it’s a complicated relationship that has a lot of back and forth. When people have a lot of reactions to different supplements, it’s usually a liver issue. In my book Hashimoto’s Protocol I recommend starting with the liver, then working on the adrenals and then the gut. Here are some articles you might find interesting:
HOW SUPPORTING THE LIVER IS KEY TO RECOVERING FROM THYROID DISEASE
https://thyroidpharmacist.com/articles/support-liver-recover-from-thyroid-disease/
ARE YOUR ADRENALS SABOTAGING YOUR HEALTH?
https://thyroidpharmacist.com/articles/are-your-adrenals-sabotaging-your-health/
IMPORTANCE OF GUT HEALTH
https://thyroidpharmacist.com/articles/importance-gut-health/
This list is overwhelming… It’s so many things to add when you’re already changing diet and lifestyle factors for Hashimoto’s. If you could pick two things to definitely focus on for adrenal fatigue, what would they be? (I think I have the diet aspects down).
April – thank you for reaching out. I understand it can be overwhelming! Just doing one thing at a time, I have found is often the best way to go. ❤️ I recommend self-management stress-reducing habits like mindfulness, yoga, and meditation. Meditation has specifically been found to be helpful in building resilience to stress and you also may want to consider and adrenal adaptogen. I hope that helps!
Thank you for this and all the great info in your Hashimoto’s Protocol book!
I understand the protocol is four weeks long, but do you recommend continuing to take adrenal support supplements following the four weeks?
Jenna – thank you for reaching out. ❤️ For questions about the protocols, please email my team at info@thyroidpharmacist.com and they will be happy help you.
Looking at your test you recommended- I’ve read testing reverse t3 is important and didnt see that on there, what do you think?
Amanda – Thank you for following. Here is an article with my recommendations and more information that I hope is helpful: https://thyroidpharmacist.com/articles/top-10-thyroid-tests/
Hi Izabella,
First of all, I would like to thank you for your work. I’ve had Hashimoto’s disease for 15 years and I’ve had very debilitating symptoms for 2 years now and your approach gives me hope!
I bought your book and started the protocols. I have for sure adrenal dysfunction (tests have shown this to be true). I understand that resting is essential in the protocol but… My problem is that I just can’t sleep properly. I take griffonia, ashwagandha, lemon balm infusion, magnesium, don’t drink coffee, meditate, stop watching screens 2 hours before bed and I still can’t sleep well. I wake up around 3 or 4 a.m. and then toss and turn in bed without being able to get back to sleep properly. In the morning, I am exhausted.
I am afraid that this situation prevents me from healing my adrenals and then my disease. I don’t know what to do… My doctor recommends that I take an antidepressant to help me get back to a good night’s sleep. Is this a good idea?
Thank you so much.
Anaelle (from France!)
Anaelle, my pleasure! I’m so happy to hear you are finding my resources helpful. If you have any questions about the protocols please feel free to email my team at info@thyroidpharmacist.com and they will be happy to help. When it comes to sleep, sleep hygiene is a great place to start but most of my complex clients were already doing it.
I wanted to find a way to help more people sleep better and sleep became a personal struggle for me when I got pregnant and had a baby. I dug into research, lots of lab tests and consulted with some brilliant colleagues. I now have around 80% success rate when we assess and address the six following things
1. Sleep hygiene as mentioned
2. If people are already doing sleep hygiene and especially if they have other signs of magnesium deficiency, I will recommend magnesium citrate.
3. Blood sugar swings can wake people up in the middle of the night. This could be due to excess carbohydrate consumption, inadequate calorie, fat and/or protein intake, and nutrient deficiencies. Supplements including carnitine and myoinositol can help.
4. Dehydration can cause leg cramps, as well as dry mouth and passages, which can lead to sleeping with one’s mouth open and waking up thirsty. The key is hydration and electrolytes earlier in the day, not right before bed as this can raise cortisol and cause us to need to wake up to pee.
5. Hormone imbalance, such as progesterone deficiency , tends to be more common in Hashimoto’s, and this can also lead to sleep deprivation (hello perimenopause and menopause).
6. Gut dysbiosis can lead to a buildup of ammonia, which has been tied to brain fog and frequent night wakings
Here is an article that might be helpful as well:
SLEEP SOLUTIONS
https://thyroidpharmacist.com/articles/sleep-solutions-for-hashimotos/
This article is very informative, thank you! I’m now 35 and probably around 25 years ago my pcp put me on levothyroxine after some blood work. At some point I eventually stopped the meds, only to try getting a new pcp about 10 years ago to diagnose my thyroid. Due to “normal” TSH he didn’t do anything. About 7 or 8 years ago I saw an endocrinologist(I believe he was considered one of the best in his field) who found antibodies attacking my thyroid. Only recently have I discovered that this is called Hashimotos! He treated me with levothyroxine and hydrocortisone(I don’t really understand the reason for this one). Your article has given me hope that I can get better! I’ve gone at least 10 years with symptoms that don’t seem to improve including some form of anxiety. Like you said, I have symptoms of both hypo and hyper thyroid – things like sensitivity to heat and cold, constipation and diarrhea(near as I can tell) even in the same BM, and of course the fatigue. Whether this is hashi’s or HPA dysfunction, the fatigue plus the inability to wake up rested are the most troublesome of my symptoms behind only the digestive issues I’ve experienced. I’ve also been to GI doctors and was just recently diagnosed with SIBO. I’m on a handful of supplements for digestion, and after SIBO treatments I’m still struggling. I may or may not have leaky gut, nutrient defficiencies, and/or food sensitivities. So either it’s still not resolved or it’s been caused by Hashimotos/Adrenal problems this whole time.
I’m confused about whether addressing the adrenal issues I may have would be helpful without first addressing Hashimotos itself? Or is fixing the adrenal dysfunction the path to improving Hashimotos?
I don’t know what I should do first. Do you recommend your latest book, or perhaps one of your books on Hashimotos? I feel like I should seek an ND or functional medicine provider(are these the same thing?) to help guide me as well.
Justin, thank you for following. Adrenal imbalances are very common in Hashimoto’s patients. Treating hypothyroidism without treating the adrenals is one of the biggest reasons people continue to feel exhausted despite receiving treatment with thyroid hormones. Stress seems to be a precursor to hypothyroidism. Additionally, taking thyroid hormones can actually help us clear out our adrenal hormones faster, which then leads to adrenal fatigue. So, it’s a complicated relationship that has a lot of back and forth. Here is an article I hope is helpful: https://thyroidpharmacist.com/articles/addressing-adrenals-must-with-thyroid-problems/
Hi Isabella
I’m currently weaning off hydro cortisone for adrenal exhaustion. I’m on t3 for Hashimoto. Would you recommend your adrenal support supplement. Do you ship to the United Kingdom. Thanks Susan.
Susan – thank you for reaching out. I recommend discussing the addition of adrenal support with your practitioner to help you determine if it would be an option for you. Unfortunately, I am unable to ship internationationally but please email my team at info@thyroidpharmacist.com and they will be happy to share my international alternatives.
Hi, is it not recommended to drink Sole if someone has high Cortisol? I started drinking it, prepared as recommended above, a year ago when my cortisol levels were low (217 nmol/L). Now my levels are high (690 nmol/L) so I’m not sure if drinking sole could make things worse and increase cortisol…. or is it still just supporting the adrenals?
Les, With high cortisol, it’s best to be cautious. Sole can support adrenal function when cortisol is low, but if your cortisol is already high, it may not provide the same benefit and could potentially contribute to fluid or electrolyte imbalance. It’s best to check with your practitioner before continuing, so they can guide you based on your current labs and overall adrenal support plan.