Did you know that most cases of thyroid disease are autoimmune in nature? (1)
Hashimoto’s thyroiditis is an autoimmune condition that happens to affect the thyroid gland. This means that our immune system recognizes the thyroid gland as a foreign invader and begins to attack it, eventually leading to the destruction of our thyroid tissue. When this destruction goes on long enough, the person will lose their ability to produce thyroid hormone.
Hashimoto’s is a progressive autoimmune condition that results in the destruction of the thyroid gland and leads to hypothyroidism — and in some cases, to other types of autoimmune conditions as well. (2)
The condition may take many years to develop and is thought to be triggered by damage to the thyroid gland. This results in immune cells congregating in the thyroid gland, and eventually losing their ability to differentiate the thyroid gland from a foreign invader (like a virus or bacteria).
Hashimoto’s is not usually discovered until it has progressed to the advanced stages, where there is significant damage to the thyroid gland.
In this article, I’d like to start at the beginning and walk through the stages of Hashimoto’s. I’ll cover:
- How Hashimoto’s is diagnosed
- The 5 stages of Hashimoto’s
- Reversing the condition
How is Hashimoto’s Diagnosed?
It takes an average of 10 years to be diagnosed with Hashimoto’s between the start of the autoimmune attack on the thyroid gland, and when the person is diagnosed. I had symptoms of thyroid disease for over a decade before I was diagnosed with Hashimoto’s, and many of my clients and readers share a similar timeline between first having symptoms and getting an official diagnosis.
Getting a diagnosis can take so long because most conventional doctors only test one’s TSH levels, but they won’t be elevated until stage 4. There are better tests — that are covered by insurance — that can reveal thyroid disease up to a decade before a change in TSH is detected. But in my experience, most doctors won’t run these tests until a change in TSH is seen. It is really quite backward!
The longer this immune response is in place, the more thyroid damage occurs — and the greater the likelihood of the person progressing to hypothyroidism, where the thyroid gland becomes so damaged that it is no longer able to make enough thyroid hormone.
If we detect the condition earlier, we can prevent the damage…not to mention a decade of symptoms!
The most helpful tests for diagnosing Hashimoto’s include thyroid antibody tests (TPO and TG antibodies) and thyroid ultrasounds. If your doctor won’t order these tests for you, you can self-order them through Ulta Lab Tests, for a relatively low cost. Additionally, some insurance plans will reimburse patients for the labs they order online.
Left unbalanced, the immune system may go on to attack different parts of the body, leading to the development of other autoimmune conditions.
There are no current treatment recommendations or guidelines in the world of conventional medicine to address the immune system attack on the thyroid gland. Rather, the focus is on restoring normal thyroid hormone levels.
In the case when a person is found to have Hashimoto’s with thyroid function that still falls within the normal limits by standard reference ranges, most conventional doctors will say: “I can’t do anything for you now, but follow up with me when your thyroid burns out. We can start you on medications at that point.”
Giving thyroid medications to a thyroid-deficient person is extremely important and can save lives, but this type of “rescue care” does nothing for preventing the progression of the autoimmune condition or for helping a person heal from the condition.
It’s akin to pouring more water into a bucket with a hole in it, without plugging up the leak!
Medications are very important, of course, if someone has a low level of thyroid hormones.
However, they will only address the symptoms — and not the root causes — of the autoimmune disorder.
Hashimoto’s Stages
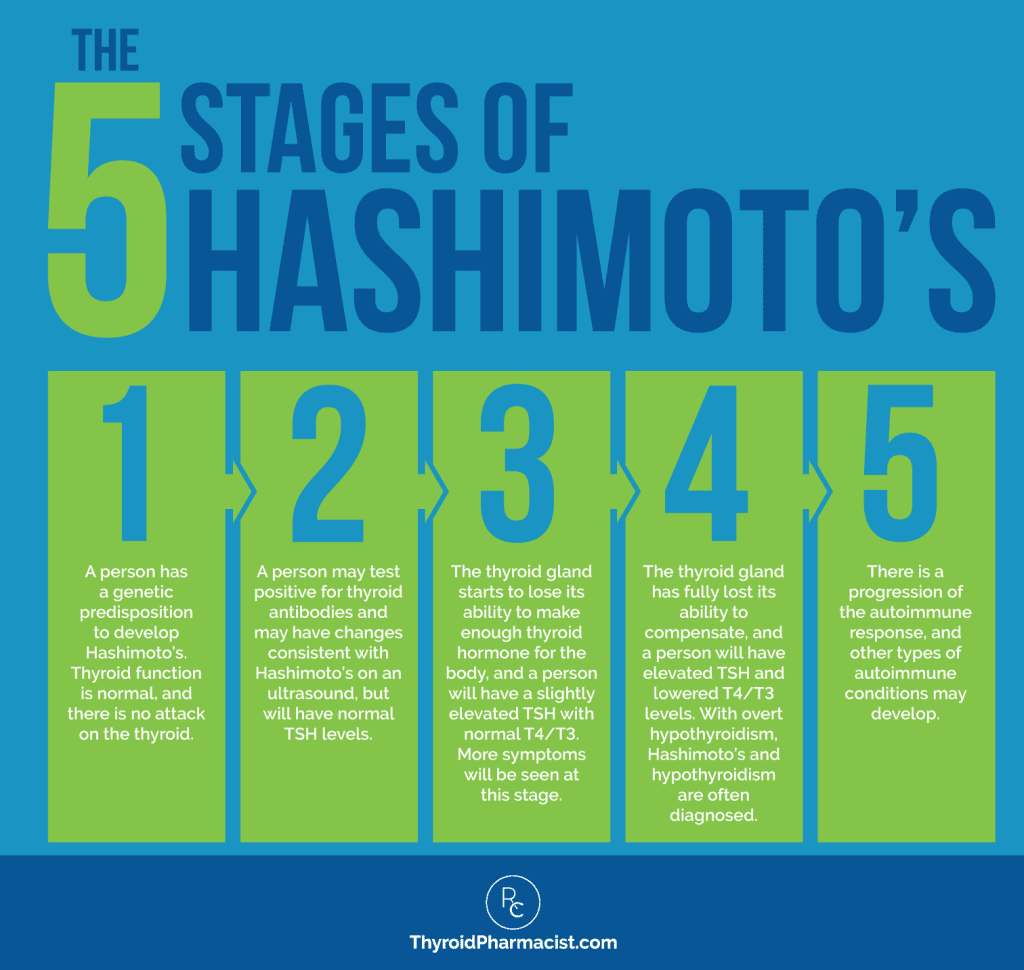
In a 2014 article, Wiersinga and colleagues identified 5 stages of Hashimoto’s. (3)
Stage 1: Genetic Predisposition
In the initial stage, a person will have the genetic predisposition for Hashimoto’s, but they will not have been exposed to the necessary triggers, and thus will have normal TSH and T4/T3 hormones.
They will not have any thyroid antibodies, nor any changes in their thyroid gland. Alternatively, this could be called stage 0, as there are no manifestations of disease at this point.
If you have thyroid disease, then this may be the stage your relatives and children are currently in. Or, if you have a family member with thyroid disease and you’re reading this, you could be in this stage. This stage is the best time to think about prevention. (4, 5)
For more information on this, I encourage you to check out this article I wrote on preventing Hashimoto’s.
Stage 2: Immune Cell Infiltration of the Thyroid Gland
Hashimoto’s is characterized by an overabundance of lymphocytes (white blood cells) in the thyroid gland. In small amounts, these immune cells play an important cleanup role, but when there are too many of them in an organ, this means trouble. It is thought that, initially, the immune cells may be there with good intentions — to clean up dead and diseased thyroid cells — but at some point, they begin to attack healthy thyroid tissues as well.
In this early stage of Hashimoto’s, a person will usually have elevated thyroid antibodies. Up to 80-90 percent may show an elevation of thyroid antibodies in blood, when tested for thyroglobulin and thyroid peroxidase antibodies, respectively. (6)
However, some people may never have thyroid antibodies present in blood — but sure enough, upon a thyroid ultrasound or biopsy, changes in the gland that are consistent with Hashimoto’s, will be apparent. (7)
This stage may go on for decades before enough damage is done, and before one can detect a change in thyroid hormone levels on a blood test — at this stage, the TSH, Free T3, and Free T4 levels will be normal.
Even in this stage, people may experience symptoms such as anxiety, fatigue, miscarriage/infertility, mood swings, excess weight, or weight loss, because their body is fighting hard to keep their thyroid levels normal, and this can be exhausting and draining on the usual body functions and nutrients.
Additionally, in this stage, there is almost always impaired gut wall function. (8)
Sadly, at this stage, most patients are not diagnosed with Hashimoto’s by conventional medicine. When they are, they’re usually told to wait and watch, and may even be referred to psychiatrists or offered antidepressants for their “mood symptoms.” 🙁
This is the ideal stage to instill lifestyle interventions and the root cause approach to prevent the progression of the condition and damage to the thyroid gland, as the inflammation in your body has just begun at this point.
In a broad overview, you’ll need to identify your triggers and strengthen your body by addressing:
- Food sensitivities
- Nutrient depletions
- Intestinal permeability
- Toxins
- Adrenal dysfunction
- Chronic infections
I’ve had many people reverse their antibodies and symptoms at this stage by just going gluten-free — according to my survey results, 70 percent of participants said their digestive symptoms improved on a gluten-free diet — but some may need a deeper exploration.
I outline my tried and tested protocols for doing all of the above in my book Hashimoto’s Protocol, and you can read more about the importance of finding your root cause in my article.
Can you have no thyroid antibodies but still have Hashimoto’s?
Yes, this is known as seronegative autoimmune thyroiditis, or serum-negative Hashimoto’s.
80-90 percent of people with Hashimoto’s will have TPO antibodies, TG antibodies, or both. (6) However, some people will never test positive for thyroid antibodies, yet may have full-blown Hashimoto’s, with all the symptoms associated with it.
In seronegative Hashimoto’s, the person will still have the hypoechoic pattern on their thyroid gland that is seen with Hashimoto’s upon ultrasound examination. They will also have thyroid autoimmunity, but may not have measurable circulating thyroid antibodies. (9)
Rotondi and colleagues have determined that seronegative autoimmune thyroiditis is a less aggressive form of Hashimoto’s, but nonetheless, the person may still develop hypothyroidism and even progress to other autoimmune conditions, which may or may not have respective positive antibody blood markers (such as seronegative rheumatoid arthritis). (10)
People who do not have thyroid antibodies will likely have smaller thyroid glands and be less likely to have goiters compared to people with Hashimoto’s antibodies.
Serum-negative Hashimoto’s should be treated the same way as serum-positive Hashimoto’s, of course, with the exception of tracking thyroid antibodies. In serum-positive Hashimoto’s, thyroid antibodies can be used as a marker to determine if one has reduced the autoimmune process.
Stage 3: Subclinical Hypothyroidism
The third stage of Hashimoto’s is known as subclinical hypothyroidism.
In this stage, TSH levels may be slightly elevated on blood tests (3-10 mU/L), and the levels of free T3 and free T4 are going to be normal. The person’s thyroid antibodies may be even higher than in stage 2, as increases in TSH can increase the inflammation of the thyroid gland. Some individuals, however, will continue to be antibody negative.
In the world of conventional medicine, this stage is controversial in terms of treatment. Doctors may take a “wait and watch approach,” but if nothing is done, this is the stage where one would begin to experience more symptoms that will eventually progress to overt hypothyroidism.
Some individuals have been able to reverse their condition at this stage without using medications, but I would not linger in this stage for too long, as an elevated TSH contributes to thyroid gland inflammation. Studies have shown that adding a small dose of thyroid medication to lower the TSH at this stage, results in a reduction of thyroid antibodies and can also make a big difference in your symptoms. (11)
While I understand that some people may have a dogma against medications and would prefer to do things the natural way, as a pharmacist, Hashimoto’s patient, and advocate, I am not a proponent of telling my readers to martyr themselves for a cause. In contrast to other medications that act as artificial chemical messengers to block or activate pathways in our bodies, thyroid medications have the same chemical structure as our internally produced thyroid hormones, and most of the symptoms associated with thyroid medications are usually due to improper dosing.
Thus, I, along with most progressive, integrative, and functional medicine physicians, will often recommend thyroid hormone treatment at this stage (some even advocate for treatment with thyroid medications during stage 2).
To learn more about optimizing thyroid medications, download my free eBook below!
In some cases, once the autoimmune attack is balanced, the person may be able to wean off thyroid medications naturally, under their doctor’s supervision.
Lifestyle interventions and the root cause approach are also critical at this stage to feel better, prevent further damage, and reverse the condition!
Stage 4: Overt Hypothyroidism
At this stage, the person has started to have thyroid gland failure. Their thyroid gland will be destroyed to the point where they will no longer be able to make their own thyroid hormone.
The person will have an elevated TSH, with low levels of free T3 and free T4. Thyroid antibodies may be even higher than in previous stages. This is the most common stage when a person is diagnosed, as the person usually has a significant amount of thyroid symptoms at this point.
This is also the stage where a person will require thyroid medications to prevent serious health consequences. Even the staunchest conventional physicians almost always recommend thyroid medication at this point.
Lifestyle changes and the root cause approach are critical at this stage, as you will likely be very symptomatic. Since you will have likely had an inflammatory process in your body for almost a decade at this point, you will need to take on the most aggressive treatment.
I often recommend Low Dose Naltrexone (LDN) at this point to prevent the progression of autoimmunity.
At stage 4, natural tissue regeneration is going to be much more challenging, but luckily, there are new options that exist that can accelerate thyroid tissue repair (see my article about lasers for tissue regeneration to learn about experimental strategies that may help).
Stage 5: Progression to Other Autoimmune Disorders
Having Hashimoto’s puts a person at greater risk for developing other autoimmune conditions like celiac disease, psoriasis, Sjogren’s, rheumatoid arthritis, lupus, multiple sclerosis, and many others… (12-14)
This is a progression of the autoimmune response — as the immune system continues to be imbalanced, it may find additional glands and body tissues to attack, such as the small intestine in celiac disease, the saliva and tear glands in Sjogren’s, and the joints in rheumatoid arthritis. (15)
At this stage, the person will have been likely treated with thyroid medications, so if they are receiving ideal treatment, their TSH, Free T3, and Free T4 numbers should be in a good range.
But, unfortunately, thyroid medications and removing the thyroid gland do nothing to stop the disease progression.
If a person’s hormones are not well-controlled with medications, if they have an enlarged thyroid gland, out-of-control antibodies, Graves’ disease, thyroid nodules, or thyroid cancer, or are not able to have balanced thyroid hormones as they swing from hyper/hypothyroidism, some doctors may recommend surgical removal of the thyroid gland.
Removing the thyroid gland will eliminate thyroid antibodies, but unfortunately, will not stop the autoimmune progression.
Additionally, people who have had their thyroid glands removed (or who have gone through radioactive iodine treatment) may suffer adverse reactions from these procedures and will need to take thyroid medications for the rest of their lives.
That said, it is still possible to reverse autoimmunity and significantly reduce and eliminate the symptoms of other autoimmune conditions.
I recommend the fundamental Hashimoto’s Protocol approach, as well as many advanced protocols at this stage, including LDN, an elimination diet, and treating infections, to help you reverse the autoimmunity.
As long as the thyroid gland has not been completely destroyed, surgically removed, or treated with iodine, there is still some hope for restoring function through advanced protocols like low-level laser therapy. (16)
Depending on how advanced the other autoimmune conditions may have become, the person may need additional organ-specific therapies that are beyond the scope of this article (such as specialized exercises, medications, and whole-body light therapy for multiple sclerosis).
It’s important to note here that autoimmune conditions do not always start with Hashimoto’s. It is thought that the first organ that becomes susceptible to autoimmune damage is the “weakest link,” where the person has a genetic predisposition or the organ has become damaged. (17)
Hashimoto’s is the most common autoimmune condition, but the thyroid gland is not always the “weakest link” for everyone. A person may start off with a different autoimmune condition, like celiac disease, and then progress to Hashimoto’s.
Reversing the Condition
When I was diagnosed with Hashimoto’s, a part of me was relieved. I felt like I had the answer to my many years of symptoms and that, perhaps, thyroid medications would help me feel normal again. But another part of me was confused: if my immune system was out of balance and causing my thyroid problem, why was I not trying to balance my immune system? It seemed foolish.
It reminded me of when I was a kid and my older brother would pick on me. I would complain to my mom, but, tired of her kids’ constant bickering, she told me to “ignore him and he will just go away.”
Of course, ignoring my brother never worked, and eventually, I had to take things into my own hands. Now, while ignoring him didn’t work, fighting certainly didn’t work either — he’s four years older than me, and has the tall genes!
It took some creative, outside-of-the-box thinking, but eventually, I found a way to outsmart him, and he stopped picking on me. I was always a little nerdy, so I offered to do his homework and write his papers for him, in exchange for some peace and respect. The same works for thyroid disease; rather than ignoring the condition or becoming a “thyroid warrior” where we are essentially battling ourselves, we need to think about how to outsmart the condition!
I felt like a little kid in the doctor’s office again, and I wanted to know if there was anything I could do to outsmart my immune system.
Additionally, while my weight, energy levels, and anxiety all improved once I started on thyroid medications, I also had many other symptoms that were not “thyroid related,” per se, and not responsive to thyroid treatment, like my acid reflux, irritable bowel syndrome, joint pain, and fatigue.
I knew that I could not change my genes, but perhaps if I were to find and identify my triggers, I would be able to prevent the progression of the condition.
So I searched for ways to reverse autoimmunity and came across a word that became my goal: remission.
Remission is defined as “the state of absence of disease activity in patients with a chronic illness, with the possibility of the return of disease activity.” While going into remission was not the same as finding a “cure,” I thought it would be a more realistic goal to shoot for.
The remission stage is the point where a person has addressed their underlying triggers and has eliminated them. The person will have a healthy gut and adrenals, be cleared of toxins, have appropriate levels of macro and micronutrients, and will likely have seen a significant drop in their thyroid antibodies.
The goal is to get them <35 IU/mL. (Some people have been able to reduce theirs down to 0 IU/mL!)
While there is no cure for Hashimoto’s, we can put it into remission by eliminating the underlying triggers and thyroid antibodies — and in many cases, we can regenerate and heal thyroid tissues using innovative, experimental therapies.

The Takeaway
Some endocrinologists may say that it’s inappropriate to diagnose a person with Hashimoto’s solely based on the presence of thyroid antibodies (which may be present in 10-20 percent of the general population) if they have a “normal” TSH and do not present with any thyroid symptoms. (18)
However, a 2013 study found that people with thyroid antibodies have similar structural features and blood flow patterns on ultrasound tests, as those with Hashimoto’s who have progressed to overt hypothyroidism. (19) Thus, changes in the thyroid gland may start long before the symptoms of hormonal imbalances finally manifest.
In my opinion, I believe that people should be screened for Hashimoto’s through antibody and/or ultrasound testing. This early detection of the autoimmune process will help a person prevent a myriad of unpleasant symptoms, as well as the progression of the destruction of the thyroid gland, if the root cause of the condition can be identified.
While it’s possible to regenerate thyroid tissue and return to normal thyroid function (even with the normalization of thyroid tissue appearance on ultrasound), it’s obviously much easier to prevent damage than it is to repair it!
By digging for your own personal triggers — which are often food sensitivities, nutrient depletions, toxins, stress, or infections — and addressing gut health, you can often nip the disease in the bud before it reaches a more advanced stage. I’ve seen many people reverse their antibodies in the early stages with simple changes like going gluten free!
It’s my hope that by spreading awareness of Hashimoto’s symptoms, optimal lab ranges (instead of “normal” lab ranges), and empowering people with the knowledge they need to advocate for themselves in the doctor’s office, we can dramatically shorten the average time it takes for Hashimoto’s to be diagnosed.
My book Hashimoto’s Protocol can help you address your Hashimoto’s, regardless of the stage you find yourself in — even if you’ve had your thyroid gland removed! In it, I outline a proven treatment that has helped thousands heal and many others feel better, while reversing the autoimmune damage at the root of the disease.
I’d love to hear your story! At what stage were you diagnosed with Hashimoto’s?
P.S. You can download a free Thyroid Diet Guide, 10 thyroid-friendly recipes, and the Nutrient Depletions and Digestion chapter for free by signing up for my newsletter. You will also receive occasional updates about new research, resources, giveaways, and helpful information.
For future updates, make sure to follow us on Facebook, Instagram, TikTok, and Pinterest!
References
- Ragusa F, Fallahi P, Elia G, et al. Hashimotos’ thyroiditis: Epidemiology, pathogenesis, clinic and therapy. Best Pract Res Clin Endocrinol Metab. 2019;33(6):101367. doi:10.1016/j.beem.2019.101367
- Mincer DL, Jialal I. Hashimoto Thyroiditis. In: StatPearls. Treasure Island (FL): StatPearls Publishing; September 28, 2021.
- Wiersinga WM. Thyroid autoimmunity. Endocr Dev. 2014;26:139-157. doi:10.1159/000363161
- Balázs C. Örökletes és környezeti tényezők szerepe autoimmun pajzsmirigybetegségekben [The role of hereditary and environmental factors in autoimmune thyroid diseases]. Orv Hetil. 2012;153(26):1013-1022. doi:10.1556/OH.2012.29370
- Lee HJ, Li CW, Hammerstad SS, Stefan M, Tomer Y. Immunogenetics of autoimmune thyroid diseases: A comprehensive review. J Autoimmun. 2015;64:82-90. doi:10.1016/j.jaut.2015.07.009
- Fröhlich E, Wahl R. Thyroid Autoimmunity: Role of Anti-thyroid Antibodies in Thyroid and Extra-Thyroidal Diseases. Front Immunol. 2017;8:521. Published 2017 May 9. doi:10.3389/fimmu.2017.00521
- Rotondi M, de Martinis L, Coperchini F, et al. Serum negative autoimmune thyroiditis displays a milder clinical picture compared with classic Hashimoto’s thyroiditis. Eur J Endocrinol. 2014;171(1):31-36. doi:10.1530/EJE-14-0147
- Fasano A. All disease begins in the (leaky) gut: role of zonulin-mediated gut permeability in the pathogenesis of some chronic inflammatory diseases. F1000Res. 2020;9:F1000 Faculty Rev-69. Published 2020 Jan 31. doi:10.12688/f1000research.20510.1
- Croce L, De Martinis L, Pinto S, et al. Compared with classic Hashimoto’s thyroiditis, chronic autoimmune serum-negative thyroiditis requires a lower substitution dose of L-thyroxine to correct hypothyroidism – journal of endocrinological investigation. SpringerLink. https://link.springer.com/article/10.1007/s40618-020-01249-x. Published April 21, 2020. Accessed July 19, 2022.
- Rotondi M, de Martinis L, Coperchini F, et al. Serum negative autoimmune thyroiditis displays a milder clinical picture compared with classic Hashimoto’s thyroiditis. Eur J Endocrinol. 2014;171(1):31-36. doi:10.1530/EJE-14-0147
- Adlin V. Subclinical hypothyroidism: deciding when to treat. Am Fam Physician. 1998;57(4):776-780.
- Boccuti V, Perrone A, D’Introno A, Campobasso A, Sangineto M, Sabbà C. An unusual association of three autoimmune disorders: celiac disease, systemic lupus erythematosus and Hashimoto’s thyroiditis. Auto Immun Highlights. 2016;7(1):7. doi:10.1007/s13317-016-0079-9
- Cojocaru M, Cojocaru IM, Silosi I. Multiple autoimmune syndrome. Maedica (Bucur). 2010;5(2):132-134.
- Ruggeri RM, Trimarchi F, Giuffrida G, et al. Autoimmune comorbidities in Hashimoto’s thyroiditis: different patterns of association in adulthood and childhood/adolescence. Eur J Endocrinol. 2017;176(2):133-141. doi:10.1530/EJE-16-0737
- Harpreet S, Deepak J, Kiran B. Multiple autoimmune syndrome with celiac disease. Reumatologia. 2016;54(6):326-329. doi:10.5114/reum.2016.64911
- Höfling DB, Chavantes MC, Juliano AG, et al. Assessment of the effects of low-level laser therapy on the thyroid vascularization of patients with autoimmune hypothyroidism by color Doppler ultrasound. ISRN Endocrinol. 2012;2012:126720. doi:10.5402/2012/126720
- Ludwig RJ, Vanhoorelbeke K, Leypoldt F, et al. Mechanisms of Autoantibody-Induced Pathology. Front Immunol. 2017;8:603. Published 2017 May 31. doi:10.3389/fimmu.2017.00603
- Sinclair D. Thyroid antibodies: which, why, when and who?. Expert Rev Clin Immunol. 2006;2(5):665-669. doi:10.1586/1744666X.2.5.665
- Chaudhary V, Bano S. Thyroid ultrasound. Indian J Endocrinol Metab. 2013;17(2):219-227. doi:10.4103/2230-8210.109667
Note: Originally published in April 2017, this article has been revised and updated for accuracy and thoroughness.

 Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Very good information. For years my doctor could not find anything that even made him suspect I had a thyroid problem. When our daughter was diagnosed with Hashimotos , her endocrinologist wanted to check me. The doctor herself did the ultrasound and immediately found one side of my thyroid smaller than the other. I started with a small dosage of thyroid medicine which has been increased since then, but now I feel much better. I have regular appointments with my endocrinologist now so she can watch my progress. Nothing ever showed up in just regular blood work. Thanks for this info.
Charlotte – thank you for following this page. It is good to hear that you have a caring doctor. 🙂
Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year
My 16 year old daughter was recently diagnosed with Hashimotos disease.
I live in NJ outside the Philadelphia Area. Is there a doctor or doctors that you can refer. The endocrinologist we saw today did exactly what you wrote. How can I find a doctor who would be willing to prescribe LDN and even work on her diet. She is gluten free already because of all the digestive issues you mentioned are related to this disease. She has had problems since she was 6 years old with gluten.
Rosa – thank you for following this page. I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Rosa
I also had this problem, where a doctor wrote me off and told me anything I might want regarding “remission” was basically a pipe dream. Needless to say that was disheartening. However, it fed the fire to prove it wasn’t just a dream. I am going to start with a doctor here in Ohio that is titled a “functional medicine” doctor. He goes in depth and looks for the root causes, and things that could be affecting my body that I don’t know about. I am hoping this approach, and this functional medicine will do things my “drug” doctor wouldn’t even consider. The only down side I see right now to trying this new approach is it probably will not be covered my insurance because it isn’t “necessary”. But, at this point my dream, inspired by Dr. Izabella, is priceless.
Christina – thank you for sharing your journey. <3 I am so happy you have found a Functional M.D. and I am looking forward to seeing your progress on this here. Here are a couple articles you might find interesting as well.
IS IT POSSIBLE TO RECOVER THYROID FUNCTION IN HASHIMOTO'S
https://thyroidpharmacist.com/articles/is-it-possible-to-recover-thyroid-function-in-hashimotos
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
Hi this is kinda a random comment. But I was diagnosed when I was 7 with Hasimotos and I’m now 16. I take medication to act as my thyroid hormone. I think I was able to be diagnosed so early because my mom also has Hasimotos. I never realized until now that I was kinda young to be diagnosed. I go 2-3 times a year to the endocrinologist and get labs taken to motor my levels. It just became normal. So I was curious as to what Hasimotos actually is now that I’m older, and your article really helped. Thanks!
monitor * lol
Kennedy – you are very welcome! Three things MUST be present in order for autoimmunity to occur …
1. Genetic predisposition
2. Environmental triggers
3. Intestinal permeability (leaky gut)
Developing autoimmunity is like a three-legged stool, all of these factors must be present for autoimmunity to occur! When you remove one of these, you can prevent or stop autoimmune disease. While we can’t change genes, if we know the trigger, we can remove it and we can heal the gut. Here are some links which might help:
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
IS HASHIMOTO’S HYPOTHYROIDISM GENETIC?
https://thyroidpharmacist.com/articles/is-hashimotos-genetic
Hi Dr. Izabella,
After reading your article I have had some hope of trying some different things to if not cure my thyroid, atleast return some of its function so thank you for giving me that hope. I was put on the birth control pill over 10 years ago for poly cystic ovaries and severe pain during my periods. Once I finally got off the pill and resumed my monthly periods, I was told I had developed Hashimotos autoimmune thyroiditis, as a side effect of this particular medication. I am currently on a dosage of 100mcg daily, and have been told that its irreversible and I have to be on this medication for the rest of my life.
My question is – my parents dont have any thyroid problem. So if you’re saying it has to be genetic in order for it to be autoimmune, how do I get it checked and/or confirmed? And what are my next steps?
I would really appreciate your help and response. I’m a mom of 2 boys under 6 and saying that it’s been tough to do it all while having Hashimotos is an understatement. I’ve never been told of any alternative treatments, and I would really be open to trying anything.
Thank you so much!
Ananya – thank you for following. Here is some information which you may find interesting.
Three things MUST be present in order for autoimmunity to occur…
1. Genetic predisposition
2. Environmental triggers
3. Intestinal permeability (leaky gut)
Developing autoimmunity is like a three-legged stool, all of these factors must be present for autoimmunity to occur! When you remove one of these, you can prevent or stop autoimmune disease. While we can’t change genes, if we know the trigger, we can remove it and we can heal the gut.
Here are some articles that I hope you find helpful:
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
http://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year
IS HASHIMOTO’S HYPOTHYROIDISM GENETIC?
http://thyroidpharmacist.com/articles/is-hashimotos-genetic
I’m so grateful to have fond your website.
I was diagnosed with Hashimoto’s disease 8 years ago after having my first child. And the Dr put me on levothyroxin 50, which is low dose and things were ok but not so good.
She didn’t say anything about changing my diet witch made things go downhill with my second pregnancy. My thyroid gotg bigger and my symptoms got a lot worse, then they discovered that I have white spots on my brain and they said it’s MS but I had no symptoms other than severe headaches. I decided to see a natural path, and that changed my life. The natural Dr told me it’s not MS and helped me change my diet and with time my thyroid got as better as it can be, and my levothyroxin was lowered to where I had to take half a of 25mg pill then I stopped taking medication. I was so happy with low energy but no medicine for 2 years. But now my thyroid went back to the way it started and it’s getting bigger and my levothyroxin is back to 50:( even though I’m still going gluten and dairy free, I’m trying to avoid soy but it’s hard because its in almost everything.
I don’t know what else to do!
My goiter is making me cough at night and I have severe headaches, and all the other lovely symptoms:(
Please help if you can think of anything!
P.S. what did you mean when you said treat infections? Like any infection, or only sever one’s trigger antibodies?
Nagham – thank you for reaching out. Nodules and goiters are often the result of toxicity and/or the autoimmune process. So, doing interventions to reduce the autoimmune attack on the thyroid, and toxicity, can be helpful to reduce them. Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. Here are the links to my books:
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hi there! I enjoyed the tips and info you provided above thank you. Really interesting to hear about the benefits of cutting gluten out for tx. I was diagnosed earlier this year. In fact last year when I went into the doctors it didn’t come back autoimmune until spring with the antibodies almost at 200 now. I knew something was off last year when I was waking up drenched in night sweats and swelling in my thyroid. The levothyroxine is doing its job but they currently are ordering ultrasounds of my thyroid and lymph nodes to make sure all is well as they said my throat felt lumpy and bumpy. Still extremely tired and dealing with recurring oral candida every 4-6 weeks. Have you heard of that with hashimotos? Thanks so much
Ashlynn
Ashlynn – thank you for following. I’m so glad to year you are enjoying my research and finding it helpful. Yeast is an opportunistic organism that acts up when your overall health is impaired or when your immune system is compromised. Most people with Hashimoto’s will have a high degree of yeast overgrowth, especially of the Candida genus. Treating this overgrowth can be very helpful in restoring health. A note about Candida: Candida can be a primary or a secondary root cause. While conventional medicine underdiagnoses issues related to yeast overgrowth, natural medicine practitioners seem to overdiagnose yeast and may say Candida is a root cause for all ailments. I recommend a Candida protocol for most people with Hashimoto’s.
Candida and Hashimoto’s
https://thyroidpharmacist.com/articles/candida-and-hashimotos-connection/
Hi
Im on 300mg thyroxine a day & i seem to be getting more & more tired & i have no energy, i also have a b12 deficiency which i have monthly shots for.
I am also having trouble staying asleep awake roughly 4-5 times a night. Can you give me any advice on this or is it best to see my own doctor.
Many thanks
Sue – thank you for following this page. I’m sorry to hear that you are not doing well. 🙁
Please, understand that due to liability issues, I am unable to answer specific medical questions. I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Hi I ordered your book. I was recently diagnosed and went on medication. My hair was falling in clumps and stopped for some time but it’s falling again. My blood work looks fine except for the antibodies that’s high. I am still on medication what do you think I can do to help this.
Valerie – thank you for following this page. Hair loss is a distressing symptom experienced by women with Hashimoto’s. For women, our hair represents our femininity, and losing our hair is a constant reminder that something is off and that we are not well. Have you read these articles?
HASHIMOTO’S AND GETTING YOUR HAIR BACK
https://thyroidpharmacist.com/articles/hashimotos-and-getting-your-hair-back/
HAIR LOSS AND YOUR THYROID
https://thyroidpharmacist.com/articles/hair-loss-and-thyroid
Do you have a list of functional/holistic doctors in the Chicagoland area? I have your book but feel I need a doctor to work with me. Thanks for all your good work and Congratulations on the #1 Bestseller!!!
Joyce – thank you for following this page and for your support. <3
I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
So Far in the researh and disovery stage……significant issues of Thyroid, Diabetes, and other immune issues very prevalant I have more autoimunite issues that nedd to be addressed.
Kathy – thank you for following this page. Good for you, taking charge of your health! <3
When I was first diagnosed with Hashimoto’s, I felt so alone. My doctor didn’t think it was a big deal, and none of my friends or co-workers had it. It wasn’t until I started to research online that I found others who were going through the same thing.
A couple of years after my diagnosis, I found Hashimoto’s 411, a closed Facebook group run by Alice Berry McDonnell. This group is amazing! It is comprised of an army of highly motivated, smart, supportive women and men (now 45,000+ strong), and each of them sharing ideas of what worked for them, things they were planning to try, and offering support to one another. The comfort I received from knowing that there were others going through the same challenges as I, was enormous.
https://www.facebook.com/groups/hashimotos411/
Ask questions. Post your thoughts. Scan the files. It is an absolutely amazing resource. Best of all it’s kept private from spammers.
How would one gi about Adrenal Detox please ??, I have Cronic IBS and have addressed this problem, and have eliminated gluten, and nuts as they were a huge problem. I have also suffered with quiet severe spondylitis for the last 15 years. Any suggestion.
Kind Regards.
Michelle – thank you for following this page.
Please, understand that due to liability issues, I am unable to answer specific medical questions.
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Can you please give me advice on how I can improve my 13year old daughter’ energy? She has Hashimito’s and is currently taking Euthyrox after a month of Eltroxin. Her symotoms just seem to be getting worse and we are only seeing her endo in a months time. ANY advice would be greatly appreciated! Thank you.
Nicolene – thank you for following this page. My heart goes out to you and your daughter. <3
Please, understand that due to liability issues, I am unable to answer specific medical questions.
Fatigue was the most debilitating symptom I experienced with Hashimoto’s. It actually started 8 years before I was finally diagnosed in 2009, after I got Mono (Epstein-Barr Virus) in college. I needed to sleep for 12 hours each night to be able to function, and by “function” I mean after hitting the snooze button on my alarm clock for two hours (ask my poor husband), I would drag myself out of bed and then had to drink 4-6 cups of caffeine everyday to keep myself awake. I often had Red Bull and Pepsi for breakfast, and was the epitome of “wired but tired”. I hope my articles help you get started 🙂
OVERCOMING THYROID FATIGUE
https://thyroidpharmacist.com/articles/top-10-tips-for-overcoming-hashimotos-fatigue
THIAMINE AND THYROID FATIGUE
https://thyroidpharmacist.com/articles/thiamine-and-thyroid-fatigue
I have both your books and am in the process of healing my thyroid after being on Thyroxin for 20 years. I’ve been dairy, gluten and soy free for 5 weeks and have more energy than I had 10 years ago. I’ve also lost 4.5kg. I went to my GP to get all the tests you recommend. He wouldn’t do Tg Antibodies…because my thyroid is underactive. When I told him that I had cut out gluten he was concerned. .he said you need gluten in the diet! So I asked if I can have a gluten sensitivity test. He said I have to eat gluten for 2 weeks and then get tested for coeliac serology. Will eating gluten for 2 weeks affect my antibodies? Will they be elevated if gluten is a reason for my Hashimoto’s?
Nicole – thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions.
It depends on the person and their individualized food sensitivities. Some people go into remission just gluten free, others may have to go as far as autoimmune Paleo. The most common triggers in Hashimoto’s are nutrient deficiencies, food sensitivities, intestinal permeability (leaky gut), stress, an impaired ability to get rid of toxins and in some cases, infections. Optimizing your health starts with food. Figuring out which foods nourish you, and which ones cause you harm is the single most important thing you can learn in your health journey.
I’ve found that recognizing and eliminating reactive foods can be a life-changer for most people with Hashimoto’s.
Reactive foods trigger an inflammatory response in the GI tract, leading to malabsorption of nutrients (gluten sensitivity, in particular, has been implicated in causing a Selenium deficiency, a well-known risk factor for Hashimoto’s), and can also produce intestinal permeability whenever they are eaten.
Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts, and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function!
BEST DIET FOR HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/best-diet-for-hashimotos-hypothyroidism
TAILORING YOUR THYROID DIET
https://thyroidpharmacist.com/articles/tailoring-your-thyroid-diet-to-your-needs
DAIRY AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/got-hashimotos-you-may-want-to-reconsider-dairy
Hi!
I’ve been following you forever! You are the only one who really understands the thyroid. I have your other book and I will be purchasing your new book. This article helped me because I am feeling overmedicated and starting going lower on my meds. Just had my bloods drawn waiting on results. I have Hashimoto’s, celiac, sjogrens. I’m taking NDT and LDN and my vitamins. So it is possible to reverse this? How do I get guidance? My doctor asks me what amount of NDT I want next? He’s a decent doctor because he prescribes LDN which is hard to get. I’m going on how dizzy I feel versus am I getting sleepy? Not very scientific.
Please advise.
Thank you ,
Andrea
Andrea – thank you for following this page and for your support. <3
Thyroid tissue can regenerate, but the rate at which it does is not always predictable. Thus, some are able to stop the autoimmune attack on their thyroid and regain normal thyroid function. Others can reduce the dose of medications, and others will need to stay on the medications indefinitely. I'm currently working on some protocols to help with tissue regeneration.
Reversing Hashimoto's means different things to different people. For some, it means a reduction in symptoms, and for others, it means a reduction in your antibodies. I had both. Here a few articles that might be helpful for you :)
IS IT POSSIBLE TO RECOVER THYROID FUNCTION IN HASHIMOTO'S
https://thyroidpharmacist.com/articles/is-it-possible-to-recover-thyroid-function-in-hashimotos
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
HASHIMOTO’S SELF CARE, GETTING AND STAYING IN REMISSION
https://thyroidpharmacist.com/articles/hashimotos-self-care
Is it possible to get a consultation for my condition. Though I have symptoms ever since year 2000, I have never been treated properly except being prescribed Thyroxine. Thanks in advance.
Bea – thank you very much for your inquiry.
I do provide a limited number of consultations, however, my consultative schedule is all full at the moment. I have a 12-week online program called Hacking Hashimoto’s that covers all of the strategies that I go through with my one-on-one clients, in a self-paced format, so that participants have access to all of the things I’ve learned about Hashimoto’s without having to schedule costly consults with me or another practitioner. There are a few requirements that you should pay attention to, such as my book is a required read.
HACKING HASHIMOTOS
http://hackinghashimotos.com/
In addition, any person that goes through the program will have the opportunity for a follow-up consultation with one of my thyroid pharmacist consulting members.
Lastly, here’s the link to the book in case you have not read it already.
AMAZON
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Im 49 years old and in 2013 I became sick lost 40 pds in 3 weeks and was anxious , tired, depressed just horrible! Couldn’t go to work. I wnt from Hypo to Hyper and it took 6 months for me to feel better. Was on Antidepressant and anti Anxiety meds. Until the high dose which I was on 150 synthroid left my body and then i was on 112 synthroid. Again in 2016 same thing happened i was on 175 synthroid. horrible feeling! Was feeling better by August another 6 months. Now its April 2017 Feb I started feeling strange again. All Im told is Antibodies will always be high and can’t be reversed I’m so upset and tired of feeling this way and Drs. just thinking its physiological? Of course it is ? Im not making this up!!! Please help. Thank you in advance :0) Just want to feel myself again.
Donna- Thyroid tissue can regenerate, but the rate at which it does is not always predictable. Thus, some are able to stop the autoimmune attack on their thyroid and regain normal thyroid function. Others can reduce the dose of medications, and others will need to stay on the medications indefinitely. I’m currently working on some protocols to help with tissue regeneration.
Reversing Hashimoto’s means different things to different people. For some, it means a reduction in symptoms, and for others, it means a reduction in your antibodies. I had both. Here a few articles that might be helpful for you 🙂
IS IT POSSIBLE TO RECOVER THYROID FUNCTION IN HASHIMOTO’S
https://thyroidpharmacist.com/articles/is-it-possible-to-recover-thyroid-function-in-hashimotos
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
How likely is it that someone with Hashimoto’s will develop other auto immune diseases? My daughter, age 20, was recently diagnosed and we are working on getting her dosing right. Once that’s done, is it definitely/probably/possibly/not likely that she’ll come down with something else if she does nothing else to treat the disease (i.e. gluten-free eating)?
Glenda- Hashimoto’s may be associated with other autoimmune diseases like Type 1 diabetes mellitus, multiple sclerosis, rheumatoid arthritis, celiac disease, lupus, Addison’s disease, pernicious anemia and hypoparathyroidism. Polyglandular autoimmunity is a medical term used to describe when one person has two or more autoimmune diseases. Here is some information you may find interesting.
Three things MUST be present in order for autoimmunity to occur…
1. Genetic predisposition
2. Environmental triggers
3. Intestinal permeability (leaky gut)
Developing autoimmunity is like a three-legged stool, all of these factors must be present for autoimmunity to occur! When you remove one of these, you can prevent or stop autoimmune disease. While we can’t change genes, if we know the trigger, we can remove it and we can heal the gut.
REVERSING AUTOIMMUNITY AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
IS HASHIMOTO’S HYPOTHYROIDISM GENETIC
https://thyroidpharmacist.com/articles/is-hashimotos-genetic
So if she doesn’t do anything to change one of these “legs of the stool”, is she mostly to develop other diseases? She currently has no other symptoms except for the fatigue and menstrual irregularities which seem to be getting better with the medicine.
Hi Dr,
I’ve been ill for over ten years around 5 yrs ago I had to travel west to Nevada for a funeral I currently live in IL. I was only there 3 days but by the 2nd day I was feeling amazing. Went home feeling horrible again well last yr I decided to go for an extended stay I was there for 3 weeks while there again by third day my thyroid shrunk I wasn’t short of breath my heart stopped racing no more joint pains and everyday there felt more and more amazing. It seems that my problem may be environmental I see a lot about gut health and thyroid disease but not what in the environment that can cause it. And is my only choice to move.
Donna- Here is some information you may find interesting.
Three things MUST be present in order for autoimmunity to occur…
1. Genetic predisposition
2. Environmental triggers
3. Intestinal permeability (leaky gut)
Developing autoimmunity is like a three-legged stool, all of these factors must be present for autoimmunity to occur! When you remove one of these, you can prevent or stop autoimmune disease. While we can’t change genes, if we know the trigger, we can remove it and we can heal the gut.
REVERSING AUTOIMMUNITY AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
IS HASHIMOTO’S HYPOTHYROIDISM GENETIC
https://thyroidpharmacist.com/articles/is-hashimotos-genetic
Did you move Donna? Did you feel better and did you figure it out if it was the weather, or the water or something else?
Hi Izabella, I have ordered your new book and can’t wait for it to arrive. I know you can’t give specific medical advice but I was wondering if you had any general weight loss tips for people with Hashimotos. I am gluten and soy free and working up to going dairy free but I just can’t seem to lose the extra weight. I am also working with a Functional Medicine guy and have a good doctor but no-one seems to be able to help with the weight loss. Thanks!
Charlotte- Thank you so much for your support. I’m looking forward to hearing your progress on this page. Make sure to take the book slow, take notes, highlight, and establish a baseline when making changes. When it comes to weight gain these are a couple of things to think about.
1) What was your recent TSH, Free T3 and Free T4? Sometimes when those numbers are on the outskirts of normal, your metabolic rate may still be impaired making it more difficult for you to burn calories. Most people report feeling well with a TSH between 0.5-2.
2) What type of medication are you on? Some report more weight loss with T4/T3 combinations (Armour, Nature-Throid, compounded medications) versus T4 medications (Synthroid, Levoxyl, Tirosint) alone. T4 is a precursor to T3, but some individuals do not convert T4 to T3 properly, and the T3 component is the metabolically active one.
3) What type of diet are you eating? Some report more weight loss with T4/T3 combination vs T4 alone. Some do not convert T4 properly.The Standard American Diet (S.A.D.) full of sugar and simple carbohydrates is perfectly designed to cause us to gain weight year after year. Even yogurts that are marketed as “healthy” contain the equivalent of 16 teaspoons of sugar. Divorcing the S.A.D. is often a step that many of us must take to not just lose weight, but to also feel better. Some diets that have been helpful include the Body Ecology Diet, the Paleo Diet, the Virgin Diet, Autoimmune Paleo Diet, GAPS diet, SCD diet, Weston A. Price Diet, or the Mediterranean Diet. You may need to modify these diets to your own individuality.
BEST DIET FOR HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/best-diet-for-hashimotos-hypothyroidism
HOW TO LOSE WEIGHT WITH HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/how-to-lose-weight-with-hashimotos
Hi There, I was just wondering is hypothyroidism called Hasmito’s? I have had hypothyroidism for 23 years. I have no thyroid funtion which has led me to some difficult changes. I have depression and anxiety, and have recently discovered pain in my foot which radiates up to my hip. Can this be a sign of MS?
Laura – thank you so much for following this page.
Did you know that if you live in the United States, Australia, Europe and most developed countries that add iodine to the salt supply and take thyroid medications, there’s a higher probability that you do have Hashimoto’s?
Depending on the source, estimates are that between 90-95% of those with hypothyroidism have Hashimoto’s.
But most doctors will never tell people that they have Hashimoto’s, or that their own immune system is attacking their thyroid. People are told that their “thyroid is sluggish”, and that these things happen with age and “Just take this pill, you’ll be fine.” I hope you check out these articles that I wrote.
ARE YOU DOING EVERYTHING FOR YOUR THYROID BUT NOT YET WELL?
https://thyroidpharmacist.com/articles/are-you-doing-everything-for-your-thyroid-but-not-yet-well/
DO YOU HAVE HYPOTHYROIDISM OR HASHIMOTO’S OR BOTH?
https://thyroidpharmacist.com/articles/do-you-have-hypothyroidism-or-hashimotos-or-both/
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well.
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
I have been in a weight loss program for a little over a month and even though I’m working really hard changing up my diet and exercising I feel like I’ve been gaining more weight because of stress and I’ve been struggling so bad. I am trying to educate myself more about my condition and I feel like I don’t even have a doctor just going to give me the right medication I’ve been taking the same medication for 6 months and I feel like it’s not even helping. But because of my insurance I feel like I always get really crappy doctors that just don’t care about me all I want is just money. I am almost to a point where I want to give up I don’t know where to go or who to talk to and I really could use some advice.
Meagan – Thank you for following this page. I’m sorry to hear that you are having a difficult time. 🙁
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Hello! Since 15 I have found Hashimoto. Until now I have had no problems, but I suffer from depression for about 5 years and doctors suggest it is from Hashimoto. Now my treating physician prescribed L-tiroxsin and the endocrinologist Eutyrox. Do you think there is any possibility of an alternative treatment method for Hashimoto. These is my indicators that’s are not in the norm others are okay.
TSH 8,65 mIU/ml 0,27 – 4,2
Free T4 8,86 ng/l 9.30 -17.00
A-TPO (MAT) 212,7 IU/ml 0-34
25-OH-Vitamin D 13,7 ng/ml
Reverse T3 89,0 pg / ml 90-215
Thank you in advance! Georgieva
Elenka – thank you for following this page.
Please, understand that due to liability issues, I am unable to answer specific medical questions.
Depression is a common symptom of Hashimoto’s and a consequence of chronic illness. I recommend you read this article as well:
ROOT CAUSES OF DEPRESSION AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/root-causes-of-depression-and-hashimotos/
A couple of years after my diagnosis, I found Hashimoto’s 411, a closed Facebook group run by Alice Berry McDonnell. This group is amazing! It is comprised of an army of highly motivated, smart, supportive women and men (now 50,000+ strong), and each of them sharing ideas of what worked for them, things they were planning to try, and offering support to one another.
https://www.facebook.com/groups/hashimotos411/
Hi Dr. Izabella,
I watched your nine week series in completion. I read the Root Cause. I also got your book the day it came out Hashimoto Protocol.
I am under the care of a naturopath who follows you as well.
I have had all the blood, stool, urine tests etc.
I have followed the AIP paleo for six weeks now religiously. I do everything your book says to do. I am on nature throid. I work out regularly, cardio regularly too. I have eaten well for many many years. I have been on synthroid for many years prior to a year ago. I am on progesterone and estrogen. I am on all the supplements you recommended. I am 58 and very healthy and in shape except for a minor struggle with weight. Until a year ago. I gained 20 pounds in six months. This is horrendous to me. So my question for you is..In the last six weeks of very strict gluten free, dairy, soy, sugar, egg free diet ( I even gave up nuts and caffeine for two weeks..no change so I brought them back in) I have lost three pounds. My only symptom of Hashmmotos are my labs, the extreme weight gain and inability to lose weight. I always feel great and have energy. I just am gaining weight and can’t lose it!!
I have h. pylori. Currently I am on your triple antibiotic regimen. When this ends in three days, I will start LDN. I am hoping this will then allow me to start repairing the leaky gut.
Agh! Can you give me any helpful advice?
Can you give me any other thoughts as to what to do?
Thank you so much for all you do for us. I have already given your info and books out to many people.
Cathy – thank you for following this page. Good job helping yourself heal! <3
Please, understand that due to liability issues, I am unable to answer specific medical questions.
When it comes to weight gain these are a couple of things to think about.
1) What was your recent TSH, Free T3 and Free T4? Sometimes when those numbers are on the outskirts of normal, your metabolic rate may still be impaired making it more difficult for you to burn calories. Most people report feeling well with a TSH between 0.5-2.
2) What type of medication are you on? Some report more weight loss with T4/T3 combinations (Armour, Nature-Throid, compounded medications) versus T4 medications (Synthroid, Levoxyl, Tirosint) alone. T4 is a precursor to T3, but some individuals do not convert T4 to T3 properly, and the T3 component is the metabolically active one.
3) What type of diet are you eating? Some report more weight loss with T4/T3 combination vs T4 alone. Some do not convert T4 properly.The Standard American Diet (S.A.D.) full of sugar and simple carbohydrates is perfectly designed to cause us to gain weight year after year. Even yogurts that are marketed as "healthy" contain the equivalent of 16 teaspoons of sugar. Divorcing the S.A.D. is often a step that many of us must take to not just lose weight, but to also feel better. Some diets that have been helpful include the Body Ecology Diet, the Paleo Diet, the Virgin Diet, Autoimmune Paleo Diet, GAPS diet, SCD diet, Weston A. Price Diet, or the Mediterranean Diet. You may need to modify these diets to your own individuality.
BEST DIET FOR HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/best-diet-for-hashimotos-hypothyroidism
HOW TO LOSE WEIGHT WITH HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/how-to-lose-weight-with-hashimotos
Dear Mrs. Wentz
Very informational page, thank you. However, I disagree with a few of your statements or at least I don’t think they are universally valid. I have quite a severe form of Hashimoto’s. I haven’t had devastating symptoms until 2 years ago, when Iiterally crashed. Before that, I experienced episodes of fatigue when doing sports (mainly endurance), had dry skin, hives (uticaria), episodes of sweating, racing heartbeats and nightsweats. But it alway subsided after a couple of weeks and I did no longer think about it. Until 2 years ago. From that point on, it took me another year to get diagnosed. At this point, I was already unable to work, severly exercise intolerant and mostly housebound.
However, I NEVER had elevated thyroid antibodies. And my case is really severe. That’s why I think the statement of no antibodies means a milder course of the disease is simply not true. I know other patients who have also become bedridden and developed other autoimmune conditions without ever having elevated antibodies. The same goes for the TSH: I was already incapable of working and forced to stay home, but my TSH wan’t clinically elevated – it always stayed around 2.8 to 3.2 with a normal range up to 4. It wasn’t until much later when I was already being treated with levothyroxine that labwork showed a TSH of 5.
Also my ft4 and ft3 habe never shown below the normal range. They were low for sure, but never abnormal.
In case you’re wondering, I’ve been diagnosed due to my obviously hypo symptoms and a thyroid-ultrasound. It showed a total thyroid size of only 5.5 ml (for males over here in europe the normal range is between 18 – 25 ml) and excessive perfusion of my thyroid (all red and yellow on the ultrasound), which is a clear sign of inflammation. However, the remaining structure of my seems echonormal. So here again, there isn’t anything that cannot be found when it comes to Hashimoto’s.
I hope this helps other sufferers and maybe even doctors to think again when diagnosing this disease.
Best regards from Switzerland,
Stefan
Stefan – thank you for following this page and for your feedback.
Absolutely, some people with Hashimoto’s test negative for thyroid antibodies because their overall immune health is so weak they do not produce enough antibodies. I’ve tested negative for antibodies several times. Now I’ve insisted on a thyroid ultrasound. Given that Hashimoto’s is one of the leading causes of hypothyroidism worldwide, I wouldn’t stop until I know one way or another.
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well. Have you done all these tests?
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
Hi Dr. Wentz —
I was recently diagnosed with Hashimoto’s and I believe I fall somewhere between stage 2 and 3. I have the antibodies but my TSH, FT4 and FT3 are in the normal range (although my FT3 are at the low end of the normal range.) My doctor said that we need to wait until those level are out of range to be treated and we should test my blood again in a year, however I am symptomatic. So after reading some of your articles and your latest book, I decided to try some supplements. I was wondering if in your opinion the pure encapsulations women’s nutrient would be helpful as I don’t currently take any other multivitamin and it seems to cover the zinc and selenium your advise or should I skip the multivitamin and just try the separate zinc and selenium.
thanks
Meridith – thank you for following this page.
Please, understand that due to liability issues, I am unable to answer specific medical questions.
Most conventional physicians use the TSH test to determine if one has a thyroid disorder and to dose thyroid medications.
However, this test can often time be misleading, as levels of circulating hormones may fluctuate at different times, such as in Hashimoto’s, the person affected may fluctuate between highs and lows.
Additionally, when scientists first set the “normal” ranges of TSH for healthy individuals, they inadvertently included elderly patients and others with compromised thyroid function in the calculations leading to an overly lax reference range.
This resulted in people with underactive thyroid hormones being told that their thyroid tests were “normal,” based on this skewed reference range.
WHAT TO DO IF YOUR TSH IS NORMAL AND YOU ARE ANYTHING BUT
https://thyroidpharmacist.com/articles/what-to-do-if-your-tsh-is-normal-and-you-are-anything-but
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well.
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
Hi Dr IZABELLA
I always read you articles which i love, so helpful
I have just a question if you can help .
what can i do to get rid of thyroid nodules ? I fixed a lot of things by reading what you post, but nodules i don’t knows i tried few things but there are not going away
Doctors are pushing me for surgery and i don’t want to go with it .
Thanks
Sue
Sue – thank you for following this page and for your kind words! <3
Please, understand that due to liability issues, I am unable to answer specific medical questions. I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Hi I just found out I have Hashimoto and I am wondering when I read your stages where I am at. They seem to base it off of the TPO being high in addition to the TSH elevated. The T4 free was normal range (barely) and T3 they didn’t test for (although I changed docs and am now awaiting results for T3 free).
What are the ranges for TPO? and does that help determine the stage your in?
They ruled Diabetes out and not sure they tested for others.
Does Hashimoto make it so you can’t exercise or may cause you to injure yourself easier until you get your levels in a good range?
Annemarie – thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions.
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Dr. Wenzt,
In 2009 I found out I had (have) Hashimotos. I also learned I had thyroid cancer. My thyroid was removed. Since then I learned how to eat to help control the symptoms that accompany flares. My question is, what do I do now? How do I proceed to a full life. I slid slightly off my diet and suffered the consequences with an array of symptoms. I just want to know how to proceed without damaging more of my body.
Thank you in advance.
Kami
Kami – Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research in journey for overcoming my autoimmune thyroid condition. I’ve also attached some articles I think will help you find your way.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
IS HASHIMOTO’S A SURGICAL DISEASE
https://thyroidpharmacist.com/articles/is-hashimotos-a-surgical-disease
HASHIMOTOS AND THYROID CANCER
https://thyroidpharmacist.com/articles/hashimotos-and-thyroid-cancer
THE CONVENTIONAL, COMPLEMENTARY AND ALTERNATIVE APPROACH TO HASHIMOTO’S AND THYROID CANCER
https://thyroidpharmacist.com/articles/the-conventional-complementary-and-alternative-approach-to-hashimotos-and-thyroid-cancer
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
TOP 10 TAKEAWAYS FROM 2232 PEOPLE WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/top-10-takeaways-from-2232-people-with-hashimotos
This article is so enlightening. I’ve been struggling with all of these symptoms for years – 10 years to be exact – since my last child was born. I’ve seen four different doctors, all of whom immediately think Thyroid when I describe my symptoms, only for them to order bloodwork and it come back “normal. They then tell me it can’t be my thyroid and I get told to change my diet, take this antidepressant, etc. I’ve tried everything. Finally, my most recent doctor noticed my thyroid has grown significantly and ordered the bloodwork as well as an ultrasound. The bloodwork was “elevated but within normal ranges” as usual, and the ultrasound revealed a goiter. He told me there was no need for medication. My see rate is high, as well. I’ve been tested for Lupus, RA, Diabetes, etc. All clear. In the meantime, my symptoms get worse and more join in. Finally, he told me to get my hormones checked with my gynecologist. She did a “complete hormone panel with a full Thyroid panel” all of which came back normal, except for TSH which was on the high end of normal. She put me on the lowest dose of Armour and it did seem to let me rest a little better and I had a little more energy, but that is all. Next test showed the same, so she took me off of it, said it wasn’t needed. I’ve begged and pleaded with several doctors to refer me to am endocrinologist, but they all say it’s not needed. I’ve tried getting my own appointments but insurance will not cover it without referral and here they will not accept you without insurance.
Years ago when this all started and the first doctor gave me these normal results, I sent off for a saliva thyroid panel and those results came back off the charts with me being hypothyroidism. Every doctor told me those tests are not accurate, only the blood tests are.
I’m exhausted, I’m in pain, and everyone I know asks me if I have thyroid issues because of my symptoms. You name it, I have it. I even have eye issues now, but the eye doctor says I’ve got 20/20 vision.
Please tell me what I can do. How can I get further testing? For years we’ve tried to find answers for my issues and every time we end up at Hashimoto’s. I just can’t find a doctor willing to listen to me enough. Normal for “most people” isn’t normal for everyone. If my tests shoe elevated or low even in normal ranges, does that not mean they could be “not normal for me?
Thank you for your time.
Shanna – thank you for following this page. I’m so sorry to hear that you are struggling! 🙁
I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
You may also be interested in my 12-week online program, called Hashimoto’s Self-Management, that covers all of the strategies that I go through with my one-on-one clients, in a self-paced format, so that participants have access to all of the things I’ve learned about Hashimoto’s without having to schedule costly consults with me or another practitioner. In addition, any person that goes through the program will get access to a Quick search Q&A Database of 1000+ questions asked by past program participants, Root Cause Assessment based on 100’s of my clients’ root causes and triggers, 2-week Meal Plans, recipes, and shopping lists to get you started on the following diets: Paleo, Autoimmune Paleo, SIBO, Candida. Also, Discounts on lab tests, high-quality supplements, and consultations and much more to support you in your journey! There are a few requirements that you should pay attention to, such as my book is a required read.
I had hypothyroid symptoms for years
And I had to struggle so much to lose weight
But when you gain weight
Most people think you eat too much
The fact is allergies to food
Might be the biggest cause
Of hashimoto’s
At least , that is what I think
Courtnay – thank you for following this page and the feedback.
Did you know that reactive foods trigger an inflammatory response in the GI tract, leading to malabsorption of nutrients (gluten sensitivity, in particular, has been implicated in causing a Selenium deficiency, a well-known risk factor for Hashimoto’s), and can also produce intestinal permeability whenever they are eaten?
Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts, and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
What I find confusing is how to understand testing for children. I was recently
Diagnosed as having hashimotos. I have had an elevated ANA for over 15 years. My mother had a thyroid issue but I do not know if it was hashimoto (she has passed away). My grandmother had lupus. My son has had some issues ongoing for years and when I read through the hashimoto information it seems like it could correlate. I had his thyroid tests and he has the thyroid peroxidase antibodies but they aren’t out of the normal range. Should a child have this antibody or is anything above a zero indicative of hashimoto? It’s very confusing.
Susan – thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions.
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Susan -Thank you so much for following this page. I understand your frustration and my heart goes out to you and your son. <3 Here is some information which you may find interesting.
Three things MUST be present in order for autoimmunity to occur...
1. Genetic predisposition
2. Environmental triggers
3. Intestinal permeability (leaky gut)
Developing autoimmunity is like a three-legged stool, all of these factors must be present for autoimmunity to occur! When you remove one of these, you can prevent or stop autoimmune disease. While we can't change genes, if we know the trigger, we can remove it and we can heal the gut.
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm
IS HASHIMOTO’S HYPOTHYROIDISM GENETIC?
https://thyroidpharmacist.com/articles/is-hashimotos-genetic
Thank you for an insightful article. My 17-year-old son was recently diagnosed with Hashimoto’s. He would tell you he had no symptoms, but I felt he was abnormally tired and wanted to sleep too much. The pediatrician took my concern seriously and ordered blood tests. His TSH was 5.9, so they did antibody testing and found 218 TP and 37 TGO. He will soon start a low dose of hormone replacement. I’m concerned that he’s so young and will likely have to deal with this the rest of his life. Are there any studies showing how patients diagnosed with Hashimoto’s as teens do long-term? Is he more at risk for other diseases because of his thyroid condition?
Susan -Thank you so much for following this page. Here is some information which you may find interesting.
Three things MUST be present in order for autoimmunity to occur…
1. Genetic predisposition
2. Environmental triggers
3. Intestinal permeability (leaky gut)
Developing autoimmunity is like a three-legged stool, all of these factors must be present for autoimmunity to occur! When you remove one of these, you can prevent or stop autoimmune disease. While we can’t change genes, if we know the trigger, we can remove it and we can heal the gut.
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm
IS HASHIMOTO’S HYPOTHYROIDISM GENETIC?
https://thyroidpharmacist.com/articles/is-hashimotos-genetic
I’m confused. Will my thyroid kick out more hormone (at some point) before burning out? I have had Hashi’s for ten years. My traditional doc just recently reduced my meds by about 10mcgs. I thought maybe my 98% gluten free and about 90% grain free roller coaster (for 4yrs or so…good, then having grain or gluten here and there, not every meal and not even daily) was maybe having benefit. I don’t have physical symptoms (like gut or bowel) to remind me. Then, I had the fear, that my thyroid might be ready to burn out: send out a burst of hormone and slowly die.
My roller coaster has been fueled by lack of support (family), the expense of everyone’s supplements (not affordable for me, so I buy what I can over the counter) and, honestly doubt. I can’t afford to see an doc not covered by my insurance (especially when I have no family support).
So, even if my thyroid is starting to fizzle, can I restore it by being good on my grain-free, gluten-free, healthy diet?
Vicoria – thank you for following this page. Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Are elevated liver enzymes related to Hashimoto’s?
Thanks for educating me in so many ways about Hashi.
Vicki – Thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Hi have hashimoto apparently. No one in UK seems to care, I am worried about it. Had scans and asparations done and told yes you have this now go away until it gets worse. I am having trouble swalling and throw up alot and cant stand anyone touching my neck or even a breeze on it makes me gag…I am struggling and dont know what else to say to my doctor. It feels like I have hands round my throat. Do I need medication at this stage?
thanks Pam
Pamela – thank you for following this page. I understand our frustrations! I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
The UK does not have a big FM community but it is possible to work with an overseas FM practitioner remotely via Skype. You may have to go to London to see someone. Have you joined any UK groups and asked for help? There are 70 UK practitioners on the Functionalmedicine.org link
http://www.thyroidpharmacistconsulting.com/europe1.html.
https://ifm.org/find-a-practitioner/
Hi, I tested positive for antibodies and was diagnosed with Hashimotos 22 years ago after my Dr. felt a lump on my thyroid gland. Through ultrasound it was determined that I had an enlarged thyroid…not a goiter. My TSH levels were elevated and I was prescribed Synthroid. About 5 years ago my endocrinologist also prescribed Cytomel after my labs showed I was low in T3 hormone. I also had half of my thyroid removed about 14 years ago. None of my Dr’s have talked about the antibodies or have ever re-tested me for them. I was diagnosed, put on the meds and check my TSH yearly. I usually just follow up with my GP each year for the labs and its like pulling teeth to get them to do more than just the TSH. What tests should my Dr’s be doing…T3, T4, free T3 & T4, reverse, uptake, etc???Does it matter if I take my meds the morning of my blood draw? will that effect my levels? Could I still be having antibody issues and should I be tested for them on a regular basis? Thanks so much for your articles, they are very helpful. When I was diagnosed 22 years there wasn’t much info out there yet.
Stephanie – Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
I was wondering if there are other lab tests we should be doing due to the side effects of Hashimotos such as testing for vitamin deficiencies??? Thanks!
Stephanie – thank you for following this page. Here are some articles you might find helpful.
COMMON QUESTIONS ABOUT LAB TESTS, YOUR DOCTOR, AND YOUR THYROID
https://thyroidpharmacist.com/articles/common-questions-about-lab-tests-your-doctor-and-your-thyroid
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
6 MOST IMPORTANT NUTRIENT DEFICIENCIES IN HASHIMOTO’S
https://thyroidpharmacist.com/articles/6-important-nutrient-deficiencies-hashimotos/
Hi Izabella,
After suddenly developing Tachycardia at age 37 years, which didn’t go away for 4 weeks, I was diagnosed with Graves disease and put on propylthiouracil. No other symptoms. I hate taking pills and so after four months I slowly weaned myself off, thinking that the worst that could happen is that I develop tachycardia again. But nothing happened. So I’m wondering if you can explain why I have had no sign of thyroid problems 20 years later (now 57 years). Should I be worried/see a doctor?
Thanks Susan
Susan – thank you for following this page. It’s good to hear that you are feeling better. Graves and Hashimoto’s are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto’s, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people) – Hashimoto’s results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually people with Graves have hyperthyroidism and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine, the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The information I present is based on my own research, in my journey for overcoming my autoimmune thyroid condition.
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hi there, I have been having “attacks” for years and its always been ruled as anxiety or panic attacks etc. The last attack that i had (which was almost a week ago) was the worst ever where i literally felt as though I’m going to die. I was admitted to hospital and my symptoms were so vague because its difficult to describe how i am feeling when this happens and a doctor decided to run all sorts of tests from an EEG to lab tests in order to find out what the problem was and he did. I was diagnosed with HT and I’m seeing a specialist in the next coming weeks. I’m relieved because finally i know whats wrong but on the other hand I’m scared to get “the attack” again. your article has made me feel so much better especially the remission and reversing part but i have no idea what triggers the attacks and i have no idea where to start with this. are there certain foods that can be avoided or such?
Natalia – thank you for following this page. Anxiety symptoms are very common in people with thyroid disorders. Here are some articles which might help:
HASHIMOTO’S AND ANXIETY
https://thyroidpharmacist.com/articles/hashimotos-and-anxiety/
AUTOIMMUNE THYROID DISEASE AND ANXIETY
https://thyroidpharmacist.com/articles/autoimmune-thyroid-disease-and-anxiety
ARE YOU GOING CRAZY OR IS IT JUST YOUR THYROID
https://thyroidpharmacist.com/articles/are-you-going-crazy-or-is-it-just-your-thyroid
Hello. Thank you so much for writing this article.
I’m 28 and was diagnosed with Hashimoto’s about 4 months ago and I can’t seem to get it under control.
My TSH level started at around 6 when I was first diagnosed. My thylarod glad was also enlarged (i had a rather big bump on my neck) but ultrasound showed no lumps. I got Euthyrox 25, and later went up to 50. After about a month and a half my TSH level was 51. I was completely shocked. Both of my T3 and T4 were always in the normal/ok range. After a little over 2 months of Euthyrox 75, my TSH is down to 8 (T3 and T4 are still ok).
Is it normal to have these spikes in TSH levels after receiving medication?
I would love to hear your opinion as I’m not getting much info from my doctors.
Thank you.
Sonja – thank you so much for following this page. There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication which you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
HOW THE DOSE OF YOUR THYROID MEDICATION CAN UNCOVER YOUR ROOT CAUSE
https://thyroidpharmacist.com/articles/the-dose-of-your-thyroid-medication-can-uncover-your-root-cause/
HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications/
Hi Dr Izabella,
My son has been diagnosed with Hypothyroidism and Hashimoto. He is six , on the autism spectrum , diagnosed with PANDAS. What treatment options can you recommend for him?
You mentioned about working with a functional medicine clinician. What do you mean by that?
Thanks,
Gauri
Gauri – thank you for reaching out. My heart goes out to you and your son. <3 - I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
I was just diagnosed with Hashimoto’s Disease. My endocrinologist wants to biopsy 4 nodules one of which is calcified and do a bone density test. I also have Von Willebrand’s Disease, MTHFR being homozygous of C677T (two copies), I am vitamin D deficient, I have to be on hormone replacement due to a total hysterectomy in 2011 (I was 27 when all of my reporductive organs including ovaries were removed), I have spina bifida occulta and pericarditis. I am sure I forgot to name some things as I suffer with a poor memory. I am scared to do the biopsies as I had to have my right breast biopsied since they found a spot they were concerned about and my mom had just been diagnosed with breast cancer so I was high risk. The MR guided biopsy was just terrible! I have pain in my right breast all of the time now. I bleed a lot and have had bad experiences. I am on the fence, I want to know what these areas on my thyroid are but I don’t want to anger them and make them spread or have them become worse. Also, since I have had surgery to remove organs due to cervical cancer and endometriosis, I am not to privy to wanting to hear that I will need to have my thyroid removed as well. Do you recommend I get a biopsy? I really am scared!!! I just want to feel better! I am tired of feeling fatigued and exhausted all of the time, my throat is always sore, I can not speak for very long without my voice becoming hoarse, hurts to swallow, pain in front of the neck that travels up to my ears, I have brain fog, and I have developed food sensitivities and feel sick basically whenever I eat! I am still trying to figure out all of my other diagnosis since the blood issues are all pretty recent! I would like any advise you could give if you wouldn’t mind. Thanks
Wiseriver – thank you for reaching out. Please understand I am not able to respond directly to these types of questions here. I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Hi Izabella,
I recently purchased your Hashimotos Protocol book and have started implementing the changes in my daily lifestyle. I have been Gluten and Dairy free for 2 months no with no changes. I am also on NDT ( have been for the last 6 months) however I am losing more hair than ever. I started experiencing hair shedding 4 years ago and I have not been able to find a cure to stop it. I know hair loss was one of your symptoms, what did you implement that made you stop your hair loss and how long did it take? Did all of your hair grow back? I’m only in my early twenties and hair loss is affecting my life as I’m losing hope that my hair will not get back to how it used to be before I was diagnosed.
Hashimotos – thank you for following this page. Hair loss is a distressing symptom experienced by women with Hashimoto’s. For women,
our hair represents our femininity, and losing our hair is a constant reminder that something is off and that we are not well.
Sometimes, when your TSH is on the outskirts of the normal range, you can continue to lose hair, and your hair may lack luster and shine. If your hair tangles easily, this is a sign that you may not be getting enough thyroid hormone. Talk to your doctor. You should see a change within 4-6 weeks.
Consider the type of thyroid medication you are taking. T3, the more active thyroid hormone, is your “beautiful hair” hormone that helps you grow your hair and prevents it from falling out. Synthroid, Levoxyl, and Tirosint only contain T4, the less active hormone. T4 should be converted to T3 in the body…except this doesn’t always happen. Sometimes an addition of Cytomel**may be cross-contaminated with gluten*** (a T3 medication) or a switch to a medication that contains a combination of T3/T4 such as Armour, Nature-Throid or compounded T4/T3 may result in a return of your hair’s luster and shine.
HASHIMOTO’S AND GETTING YOUR HAIR BACK
https://thyroidpharmacist.com/articles/hashimotos-and-getting-your-hair-back/
HAIR LOSS AND YOUR THYROID
https://thyroidpharmacist.com/articles/hair-loss-and-thyroid
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
Hi Dr. Izabella,
I am 23 and have been recently diagnosed with Hashimoto’s. After my initial appointments and getting my TSH levels back in range, I then waited 6 months for my next appointment and my tests came back with my TSH having risen again. What can cause my levels to change quickly like this? Could it be stress? Are there things I should do or avoid to try to prevent these changes from occurring?..To help manage my antibodies and slow down the progression. I do not have a gluten sensitivity and eat fairly well. So what can be my trigger?
Many thanks
Sarah – thank you for reaching out. – Most conventional physicians use the TSH test to determine if one has a thyroid disorder and to dose thyroid medications. However, this test can often times be misleading, as levels of circulating hormones may fluctuate at different times, such as in Hashimoto’s, where the person affected may fluctuate between highs and lows.
Additionally, when scientists first set the “normal” ranges of TSH for healthy individuals, they inadvertently included elderly patients and others with compromised thyroid function in the calculations, leading to an overly lax reference range. This resulted in people with underactive thyroid hormones being told that their thyroid tests were “normal,” based on this skewed reference range.
WHAT TO DO IF YOUR TSH IS NORMAL AND YOU ARE ANYTHING BUT
https://thyroidpharmacist.com/articles/what-to-do-if-your-tsh-is-normal-and-you-are-anything-but/
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well.
TOP 6 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
I was just diagnosed with Hashimoto and was doing a little research on my on to find out more about it. I literally tripped overy this page. I can’t wait to read more of this wealth of information you have provided. I just wanted to take a moment and say thank you so much for all of your time, energy and efforts. Thanks so much, Connie
Connie – you are so very welcome! Here are some articles you may find helpful.
THE MANY FACES OF HASHIMOTO’S
https://thyroidpharmacist.com/articles/the-many-faces-of-hashimotos/
10 MOST HELPFUL DIY INTERVENTIONS FOR HASHIMOTO’S
https://thyroidpharmacist.com/articles/10-most-helpful-diy-interventions-for-hashimotosaccording-to-my-clients
I am 26 and am struggling with thyroid issues. I have been diagnosed with Hashimotos in the last 6 months. My husband and I are wanting to have a baby but we have had one chemical miscarriage this past month. What steps should I take and do you think it is possible to conceive and carry a healthy baby if you have Hashimotos? Thanks for your advice.
Sandy – thank you for reaching out. I am so sorry for your loss. Pregnancy can often be a trigger – iron deficiency and immune shift, as well as potentially the baby’s thyroid cells that circulate in the body, may be a trigger. You can bring it back to balance with lifestyle interventions. You might find these articles helpful.
Hashimoto’s and Pregnancy
https://thyroidpharmacist.com/articles/hashimotos-and-pregnancy/
KAREN’S HASHIMOTO’S SUCCESS STORY
https://thyroidpharmacist.com/articles/karens-hashimotos-success-story/
WHY WOMEN HAVE MORE THYROID DISORDERS
https://thyroidpharmacist.com/articles/women-thyroid-disorders/
ESTROGEN DOMINANCE AS A HASHIMOTOS TRIGGER
https://thyroidpharmacist.com/articles/estrogen-dominance-as-a-hashimotos-trigger
Is the LDN life long? Or does that make the correction per se and eventually it will no longer be needed?
Stephanie – thank you for following this page. The time to start feeling better will of course vary per person. Once you start to feel better, maintain the dose for 2-3 months and follow-up with your physician to see if your laboratory markers have improved. LDN should be used as part of an arsenal to help you overcome your autoimmune condition. Appropriate levels of Vitamin D, full spectrum light exposure, food sensitivities all play a role in autoimmunity and need to be considered as well. It’s also best to work with a compounding pharmacy that can help you titrate your dose correctly. LDN is not a commonly prescribed medication, and it may not always be possible to convince your doctor to prescribe it. On my quest to try LDN, I talked to my local compounding pharmacist to figure out which doctors in my area were knowledgeable about prescribing LDN. I also want to stress that LDN is not a cure, but rather an immune modulator that can be used to prevent further damage to the thyroid while one is looking for their root cause or to rebalance the immune system when the root cause cannot be found. Root causes are different for different people but may include infections or food sensitivities that result in an immune imbalance. Here are some articles you might find interesting.
LOW DOSE NALTREXONE – LDN
https://thyroidpharmacist.com/articles/low-dose-naltrexone-and-hashimotos
6 DIFFERENT ROOT CAUSES
https://thyroidpharmacist.com/articles/6-different-hashimotos-root-causes
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
SUNSHINE FOR YOUR THYROID
https://thyroidpharmacist.com/articles/get-some-sunshine-for-your-thyroid
Thank you for the resource and in-depth information. I was wondering if you could refer me to a reference for what a high antibody result would be / what results would indicate Hashimoto’s?
Daisy – thank you for reaching out. Here is an article you might find helpful.
Top 10 Thyroid tests and how to Interpret
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
I am on levythyroxine and my levels tend to stay in the ok window. I have the lupus anticoagulant antibody and I have Chiari to deal with. Lately every time I wake up my hand arm leg and foot on my right side are completely asleep. To the point I cannot feel where my arm is! No one can tell me what is going on. Could it be my thyroid causing this? I am at wits end.
Pam – thank you for reaching out. Please understand, I am not able to respond directly to these types of questions here. I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Great information. Guess I’m 1 in 1000, though. My TSH went low, followed by my thyroid hormones.
My mom has thyroid disease, I don’t yet know what type but I have asked her. Her sister also, her great grandmother, her niece honestly most of the females in my family. Anyways I am 37 now and have many of the symptoms fatigue, pale/dry skin, difficulty managing weight (a recent gain of 5 kg despite consistent exercise and a good diet), Depression, mood swings, serious digestive problems (it used to be constipation but now I have violent and explosive stools the consistency of diarrhea which I have had for months with only the occasional reprieve of constipation, I haven’t had a normal stool in years) and menorrhagia for which I have to receive treatment. In college I developed Hypothyroidism but then it was discovered I was pregnant and pregnancy seemed to level me back out. After giving birth (I have only ever been pregnant one time) I was unable to lose weight, I stayed exactly the same weight down to the ounce for a solid year. Nothing I did could shift that weight. Since my thyroid has been up and down and now it is at a plateau of slight elevated. My mom also remained slightly elevated before suddenly entering a critical phase, she nearly died before she received treatment because of the wait and see approach. That same approach is being used with me and I feel fairly certain I will have to reach critical levels before treatment is even possible. I have never been tested for thyroid antibodies but I feel if she does have this type I might be able to site genetics and force my doctor into administering the test. I can’t say they will treat me even if I have it =( Why? I just don’t understand when the medicine for it is safer than the meds for most things. Should I just go gluten free and try and treat myself? I did try gluten free for a year when I was about 33 because of my digestive problems and desperation and actually I lost weight and had normal stools which is why I thought of this type during my research and also the very strong genetic link in my family.
Candice -Thank you so much for following this page. Three things MUST be present in order for autoimmunity to occur …
1. Genetic predisposition
2. Environmental triggers
3. Intestinal permeability (leaky gut)
Developing autoimmunity is like a three-legged stool, all of these factors must be present for autoimmunity to occur! When you remove one of these, you can prevent or stop autoimmune disease. While we can’t change genes, if we know the trigger, we can remove it and we can heal the gut. Here are some links which might help:
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
IS HASHIMOTO’S HYPOTHYROIDISM GENETIC?
https://thyroidpharmacist.com/articles/is-hashimotos-genetic
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead,’ or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
You might also be interested in my books:
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
The Hashimoto’s Protocol is my latest book, which is a more step by step, in-depth plan that streamlines the most effective interventions. https://www.amazon.com/Hashimotos-Protocol-Reversing-Thyroid-Symptoms-ebook/dp/B01HXK6GVQ/ref=sr_1_1?ie=UTF8&qid=1505933035&sr=8-1&keywords=hashimotos+protocol+izabella+wentz
Hi Doctor Wentz,
I am from India aged 55 years[male]. I recently discovered this page and find the information to be most comprehensive and detailed. I would like a general opinion on the following situation.
i have been recently disgnosed with a condition called”chronic auto-immune urticaria” by an allergist who put me through a series of blood tests which revealed the following.
-immunoglobulin-e—246.6 iu/ml.
-rh factor–less than 11.50 iu/ml.
-c reactive protein–0.34 mg/dl.
-anti thyroid antibodies…1265.70u/ml.
-anti body to thyroglobulin 15.60 u/ml.
I was put through a ASST test[atalogous skin serum test which turned positive for CAU].
i have been prescribed glemont-f which i understand is a anti histamine/anti asthama medicine but no thyroxine. Upon asking, my allergist, says that since my TSH level is around 4.01 i need not have any medicine for thyroid abnormality.I read many articles[including yours] which says that patients with elevated antibodies must be treated for hypo thyroidism. I am not satisfied with my allergist. My symptoms are generalised itching and weals almost everyday. I have had this condition for over three years now. Should i go to a physician who will give me a trial dose of thyroxine to check if my urticaria resolves.
Will be grateful for a general opinion on this situation.
with best wishes,
RAM. b v.
india..
b v ramesh – thank you for following this page. I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms. If you cannot find a Functional Medicine practitioner in your area, it is possible to work with an
overseas practitioner remotely via Skype or some other online video platform. Here’s a link which might help:
http://www.thyroidpharmacistconsulting.com/europe1.html
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
Here is an article which you may find helpful as well.
THE COMMON ROOT CAUSE OF HASHIMOTOS HIVES AND IBS
https://thyroidpharmacist.com/articles/the-common-root-cause-of-hashimotos-hives-and-ibs/
That’s all great if you have the right insurance or referral- Big Pharma puppet doctors could care less! I do not have the right insurance. I am stage 4 and slowly dying. Now they blame all on mental illness. Can’t wait to die- these doctors are crooks.
jjk – thank you for sharing. I understand how frustrating this can be. When I was first diagnosed with Hashimoto’s, I felt so alone. My doctor didn’t think it was a big deal, and none of my friends or co-workers had it. It wasn’t until I started to research online that I found others who were going through the same thing.
A couple of years after my diagnosis, I found Hashimoto’s 411, a closed Facebook group run by Alice Berry McDonnell. This group is amazing! It is comprised of an army of highly motivated, smart, supportive women and men (now 45,000+ strong), and each of them sharing ideas of what worked for them, things they were planning to try, and offering support to one another. The comfort I received from knowing that there were others going through the same challenges as I, was enormous. Here is the link to this group:
https://www.facebook.com/groups/hashimotos411/
After reading this article, I now believe that getting 2/3 of the HPV vaccine, Gardasil, may be my big trigger. Do you have any more information on how I can address this root cause?
Emily – thank you for following this page. Here are some articles you may find interesting.
LIVER SUPPORT
https://thyroidpharmacist.com/articles/support-liver-recover-from-thyroid-disease/
SAUNA
https://thyroidpharmacist.com/articles/8-benefits-infrared-sauna-can-reduce-symptoms-hashimotos-hypothyroidism/
6 DIFFERENT ROOT CAUSES
https://thyroidpharmacist.com/articles/6-different-hashimotos-root-causes/
That is no comfort when you are dying. Now I am having tremors. Not even my family believes me now.
Jkk – I am so sorry you are struggling. I understand how difficult and frustrating this can be. When I was first diagnosed with Hashimoto’s, I felt so alone. My doctor didn’t think it was a big deal, and none of my friends or co-workers had it. It wasn’t until I started to research online that I found others who were going through the same thing.
A couple of years after my diagnosis, I found Hashimoto’s 411, a closed Facebook group run by Alice Berry McDonnell. This group is amazing! It is comprised of an army of highly motivated, smart, supportive women and men (now 45,000+ strong), and each of them sharing ideas of what worked for them, things they were planning to try, and offering support to one another. The comfort I received from knowing that there were others going through the same challenges as I, was enormous. Here is the link to this group:
https://www.facebook.com/groups/hashimotos411/
Tha k you so much for the article it is very beneficial. I am diagnosed with hashimoto’s and subclinical hypothyrodism with some food intolerances towards gluten, lactose and sorbitol. However, checking my blood pictures for the last couple of years i can see i always have absolute neutropenia and lymphocytosis and sometimes monocytosis. Is this related to hashimotos since the high lymphocytes are the antibodies that attack the thyroid?
Bassem – Thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms. Here are some links which might help:
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
MY RECENT CHALLENGES AND FINDING DR. RIGHT
https://thyroidpharmacist.com/articles/my-challenges-and-finding-dr-right/
Thank you Dr. Wentz for this informative article. I have a question regarding the following statement: “Removing the thyroid gland will eliminate thyroid antibodies, but unfortunately, will not stop the autoimmune progression.” I have always wondered if a patient is still considered to have Hashimoto’s after removal of the gland. I have hashi’s and thyroid cancer and have chosen to try to save my thyroid if possible because I assume that I will probably feel worse without it. I didn’t realize that there would still be an autoimmune attack after removal. Can you please expand on this?
Kelly – thank you for reaching out. Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this. Sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. Here are the links to my books:
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Your explanation of the progression of this disease and my experience sound like you are describing my life. I was not diagnosed for almost ten years and I ran the full gamut of anti depression medications, severe acid reflux, mood swings, anxiety, extreme weight gain, general lethargy and brain fog. They did not treat me until my thyroid was too far gone. I noticed you talk about high a high white blood count. I remember them mentioning that in the beginning, so it struck me that I had that too. The original Dr. only did the TSH test and said it was a “little” off, but did not seem like enough to be causing all of my symptoms and put me on an antidepressant.
Luckily I found a Rock Star integrative medicine Dr 4 years ago. She did all of the tests you mention and also developed a nutrition and supplement plan (ongoing).
Great information! I hope it helps some people before they have to suffer for so many years.
Lisa – thank you so much for sharing your journey! <3
Hi Dr – I has a question about infertility and Hashimotos.. I’ve recently been diagnosed with Hashimotos and subclinical hypothyroidism… my blood work has been the same for over 4 years – many many antibodies and TSH in the range of of 5.43. It was borderline so not one of my 3 fertility specialists picked it up or saw a problem. In 4 years I have had 8 fresh cycles of IVF and have had repeated implantation failure. Dr’s kept saying my age is the issue (also I also have a low egg reserve) as everything else was fine. I have never been able to believe this as we started the IVF journey when I was 34 due to my husband having critically low sperm.. I also have endometriosis but even with these two diseases, Each IVF yielded at least 2 perfect embryos that were given top grades by the labs with all the hopes of success… So it did not make sense to me that at least 16 perfect embryos (actually more as we have had frozen cycles and IUI’s inbtw this whole drama) have failed to implant in me, with no other explanation from doctors other than my age is a contributing factor 🙁
At 38 I have gone to see a 4th Fertility specialist to have a final IVF through egg donation… we are at the end of our road financially and emotionally.. This 4th Dr has finally found my potential issue that could have been a huge factor in all our previous failures.. He would not treat me with IVF until my TSH is below 2.5 as it would lead to implantation problems, miscarriage or problems with the future child.. so off to an endocrinologist where I was diagnosed with Hashis and hypothyroidism and I am now on thyroid meds and my TSH is coming down slowly. Unfortunately as I am now 38 my eggs probably are too old now… and we cant afford to give my eggs another chance which I am devastated and angry about as this could have been picked up 4 years ago before our first IVF … our only last option forward is to try an egg donor. We are due to start this process in just a few days…
So after reading my saga (thank you if you managed to read all ?) – My question is – if we lower my TSH to the correct level 2,5, will my antibodies also come down? At last check before medication my thyroglobulin was 23 and my thyroid peroxidase Ab was 213 … noone has really explained this properly to me or said how far off my levels are, so I’m a little in the dark as to what these antibody results mean.. How do these antibodies affect implantation / carrying a child… and should I try to get these antibodies as well as my TSH down before having a donor embryo transferred to me?
Thank you – Vikki
Vikki – Thank you for following this page. Most people feel best with a TSH of around 1 or lower and with a Free T4 and Free T3 in the upper half of the range. It is expected that your TSH will be very suppressed when optimal on NDT medication. How much thyroid replacement therapy is needed is unique and different for each person, so it’s important to work with a functional medicine practitioner or a doctor, who can closely monitor your dosage and your progress.Every six weeks is usually a good schedule for testing your thyroid hormones.
Here is a research article which might help further:
TOP 10 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
Can having had Guillian-Barre syndrome cause or contribute to Hypothyroidism?
Julie – thank you for following this page. Epstein-Barr is a virus that causes mononucleosis (commonly called “Mono”), a debilitating viral infection that is common among college students, and is also known as the “kissing disease,” because individuals are exposed to the virus through saliva of those who are infected.
Specific immune cells known as CD8+ T cells are needed to fight off the Epstein-Barr virus, however, some individuals may have a low baseline level of these types of immune cells. (CD8+ T cells decrease with age, are lower in women, and in the presence of low vitamin D intake). When these fighter cells are low, the Epstein-Barr virus may take up residence in our organs (such as the thyroid) and essentially hijack the organ to help the virus hide and multiply.
The timing of infection may also matter as well, for example, children in developing countries usually contract the Epstein-Barr Virus when they are under the age of 10. This usually results in an asymptomatic infection—one that does not cause them symptoms. In contrast, in developed countries, where individuals are not usually exposed to the virus until they are in high school or college, the infection is symptomatic in 50% of the older kids affected. This is because by the time we reach college age, CD8+ T cells, the ones that fight EBV, have declined by threefold compared with the number of cells we had in childhood.
Animal fats, broths, soups and stews support the body’s ability to suppress the viruses. Monolaurin or lauric acid, one of the components of coconut oil, has been found to be active against the Epstein-Barr virus. Replication of many viruses including Epstein Barr is inhibited by glycyrrhizic acid, an active component of licorice root. Quercetin, Co-Enzyme Q10, N-Acetylcysteine, and glutathione were also reported to be helpful in chronic fatigue syndrome because of their anti-viral properties.
You also need to be sure to ask for the Epstein Barr Virus Early Antigen test, as this is a test that will let us know if the virus is actively replicating. Here is a link which might help:
EPSTEIN-BARR VIRUS AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/epstein-barr-virus-and-hashimotos
Hi Dr Wentz,
I’ve been following your advice for years and finally in the last 6 months have put my Hashimoto’s in remission. I went from taking 125ug of Levothyroxin down to zero, and after I stopped taking Levothyroxin completely for 6 weeks my lab test showed TSH < 0.01 still with no meds. How could this be? is my thyroid all of a sudden overproducing? what is going on? should I wait a bit more and test again? Any insight would be awesome 🙂
Justin – Thank you for following this page. Most people feel best with a TSH of around 1 or lower and with a Free T4 and Free T3 in the upper half of the range. It is expected that your TSH will be very suppressed when optimal on NDT medication. How much thyroid replacement therapy is needed is unique and different for each person, so it’s important to work with a functional medicine practitioner or a doctor, who can closely monitor your dosage and your progress.Every six weeks is usually a good schedule for testing your thyroid hormones. Here is a research article which might help further:
TOP 10 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
Hi Dr. Izabella,
I was wondering if you might be able to give me some advice please?
I am a 32 year old male. I was diagnosed with Hashimoto’s 1 week ago. The TSH reading was 6.03. My T3 and T4 levels are in normal range. I also have anti TPO levels of >1300. I had an ultrasound check which revealed that I had diffused spongiform nodules in my left and right thyroids, which collectively measured 2.5cm x 1.5 cm in space, in each thyroid.
I have since started a gluten free diet, and I am taking selenium and probiotics tablets. Apart from this diagnosis, my only symptoms is moderate anxiety. I am also taking 25mg of levothyroxine daily.
Is this diagnosis something to be worried about long term, in your medical opinion?
Kind regards,
Matt
Matt – thank you for sharing your journey. 🙂 Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year
Good morning, I came a crossed this website searching for answers, it’s so often that you are let down by doctor’s that you go searching for answers… So here is my story.. I am a 49 year old female who as RA. I take Orencia once a week for this. I have been feeling terrible for over a year now. Can’t sleep, tired all the time, not just tired actual fatigue.. gaining weight, by this I mean I can gain ten pounds in a week.. In fact from the date I had bloodwork taken on the 18th, to the date I went back in for results on the 28th, I gained 10 pounds… Just all around craziness.
So, I got test results back and they said Hashimotos. my numbers were TSH 1.52 Free T3 3.37 Free T4 1.09 Reverse T3 15.9 and Thyroid Peroxidase Antibodies 443.
They tall me this, yet don’t want to put me on any medication? I don’t understand.. I feel like crap, am gaining more weight day by day, which contributes to the lack of energy, I am so tired I can’t functions some days.. What am I supposed to do?? Why would they not put you on medication for something to prevent losing it entirely?? Can you please help with this ? I just need to know if I should be seeking out other professionals for this or not?
Diana – thank you so much for sharing your journey here. I understand how hard this is. It took me three years to get into remission, but every change can bring huge benefits. There are 5 stages to thyroid disease. A conventional doctor won’t look at stopping the autoimmune attack progressing. What we usually see is that a person with only thyroid antibodies and normal TSH is considered to be in Stage 2 of thyroid disease, a person who has an elevated TSH with normal T4/T3 with or without thyroid antibodies, is in Stage 3 of thyroid disease, a person with elevated TSH, lowered T3/T4 +/- thyroid antibodies is in Stage 4 of thyroid disease, regardless if she/he has thyroid antibodies or not. Stage 5, is when the person progresses to other types of autoimmune disease. Functional medicine doctors really aim to find and treat underlying causes and prevent serious chronic disease rather merely treat disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid/
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
I have Hashimotos and hypothyroidism. I am being treated with Armour Thyroid and my doctor recently tested my TPO antibodies and they were at 1926. She did not seen concerned, but I am. Should I go see a specialist and if so, what kind? Thank you.
Lacey – thank you for reaching out! I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms. I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It’s a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/pages/clinician-database
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
http://www.thyroidpharmacistconsulting.com/recommended-compounding-pharmacies.html
Here is a research article which might help as well:
TOP 10 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
Hello!
Will the protocol work also if I have a serum negative Hashimoto?
Thank you
Giuliana – thank you for reaching out. Some people with Hashimoto’s test negative for thyroid antibodies because their overall immune health is so weak they do not produce enough antibodies. I’ve tested negative for antibodies several times. Now I’ve insisted on a thyroid ultrasound. Given that Hashimoto’s is one of the leading causes of hypothyroidism worldwide, I wouldn’t stop until I know one way or another.
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well. Have you done all these tests?
Top 10 Thyroid Tests and how to Interpret them.
https://thyroidpharmacist.com/articles/top-6-thyroid-tests
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this. Sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. Here are the links to my books:
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Thank you for the above, but for me it’s a bit too late. I didn’t find out I had Hashimoto’s until my goiter was pushing out of my neck. Right now it’s cutting off half my windpipe and has even pushed it to one side a bit. I can barely swallow and talking has become forced. I need to have my thyroid removed before I lose the ability to swallow and breathe. Do you have any suggestions for those of us who have reached such an advanced stage before even being diagnosed?
Rachel – thank you for sharing your journey. I am so sorry you are going through this. My heart goes out to you. <3 Nodules and goiters are often the result of toxicity and/or the autoimmune process. So, doing interventions to reduce the autoimmune attack on the thyroid, and toxicity, can be helpful to reduce them. I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms. I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It's a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you. Here are some resources you might find helpful.
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/pages/clinician-database
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
http://www.thyroidpharmacistconsulting.com/recommended-compounding-pharmacies.html
I’ve been following your work for a few years, thank you for your resources.
I was diagnosed with hypothyroidism at the age of 16 (I am now 35) after a doctor told me my thyroid was enlarged and after ultrasounds and blood work I was put on thyroid medication and have been on it ever since. Last year I asked my doctor to do antibody testing to see if I had Hashimotos and there were no antibodies present. I have eaten a gluten free mostly paleo diet for 4 years to control endometriosis but have also had normal blood work for thyroid
During this time except for T3/reverse T3.
Would my diet make the antibodies not be present? If I don’t have hashimotos then I can’t seem to find what caused my thyroid issues in the first place. I was so young at diagnosis, but my mom who also has hypothyroidism said no one ever mentioned hashimotos. I can’t seem to find much information about hypothyroidism not related to hashimotos.
Lydia – thank you for reaching out and sharing your journey. Some people with Hashimoto’s test negative for thyroid antibodies because their overall immune health is so weak they do not produce enough antibodies. I’ve tested negative for antibodies several times. Now I’ve insisted on a thyroidultrasound. Given that Hashimoto’s is one of the leading causes of hypothyroidism worldwide, I wouldn’t stop until I know one way or another.
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well. Have you done all these tests?
Top 10 Thyroid Tests and how to Interpret them.
https://thyroidpharmacist.com/articles/top-6-thyroid-tests
I am a 28 year old Man from India, now working in Germany. In the month of February this year, there was some pain in my neck near the thyroid gland. I thought, maybe it was due to one of my wrong exercise moves, as I was working out that time. But then, 2 weeks later, the pain was too much. It used to hurt while swallowing something. Also, my left eye lashes were bulged and I felt feverish. So, I immediately went to a doctor. They did the blood test and told me that my thyroid was overactive(TSH: 0.03, T3: 5.9 ng/l, T4: 2.6 ng/dl at this stage). They prescribed Carbimazol 10mg, 2 tablets a day. They told that this is a permanent condition and I’ll have to be on meds for life. I started taking them for a week and the condition wasn’t getting better. I started feeling shaky, feeling like I would collapse when I was walking. So, I called my family doctor in India asking for help. He told me to stop Carbimazol, eat plenty of fruits and just relax, relax for a few weeks and see. This helped me and I felt a little better.
3 weeks later, I found a different doctor here in Germany and told her my problems. She advised for Thyroid Scintigraphy. The reports said that there is a suspicion of an accompanying autoimmune thyroiditis type Hashimoto and asked me to start L-thyroxine 75 mcg(By this time, TSH: 14.65, T3: 2.5 ng/l, T4: 8.4 pg/ml, anti-TPO: 13.2 IU/ml). I started these tablets and started feeling completely well after a month. But now again, sometimes I feel very tired and not so well. Some other times I am totally alright. Every 3 months I’m going to the doctor now to check the levels and they are asking me to continue the same medicine(75 mcg). My latest report looks like all parameters are normal(TSH: 3.47 mU/l, T4: 1.6 ng/dl, T3: 2.7 ng/l from a report dated 31.07.2018)
Yesterday, I saw one of your videos on youtube and got to know that you had been through this. I’m just waiting right now to get my book delivered soon, so that I can learn more from it. I do not trust the doctors anymore. They also told that they will give an iodine shot after few months if you are still hyper.
I just need some help from you on finding the root cause of my problem. When this pain started for me first time in February, I was a very busy person. It was like, I used to get up and do a fast pace workout for 45 minutes; then rush to work and work for 9 hrs; then come back and give some tuitions for my friends; and also parallely learn German. Slept for max 6 to 7 hours. Could this amount of work, have stressed the body and made the body give up? Also, at this time, I was eating animal foods almost everyday, thinking on just protein and protein. I hardly used to eat fruits and vegetables. Could this be the cause? You had mentioned in one of the posts above that there is a possibility that this disease can be reversed. Is there a certain time frame after the onset of this disease, that it cannot be reversed. This last question came up because I only got to know about you yesterday, and feeling that I should’ve found you way earlier this year when my disease had started.
Pardon me for asking too many questions. Looking forward to hear from you.
Tharun – thank you for reaching out and sharing your journey. Hashimoto’s often is a combination of food sensitivities, nutrient deficiencies, adrenal issues, gut issues as well as an impaired ability to get rid of toxins. Any of those things would prevent a person from getting better. Hashimoto’s is very much an individual condition. While there are root cause commonalities, each person will have their own or in some cases, more than one root cause. You will have to start with the simplest modifications, by removing triggers, followed by repairing the other broken systems to restore equilibrium, allowing the body to rebuild itself. You will need to dig down to why the immune system is imbalanced in the first place and this will tell you how you begin to finally feel better, reduce your thyroid antibodies and even take your condition into remission.
You will have to create your own health timeline. Look back at your overall history as far back as you can remember. Look for infections, periods of severe stress, the use of medications (especially antibiotics, antacids, and oral contraceptives), accidents, and exposure to toxins. These are events that may have contributed to Hashimoto’s. Once you do, you will know what types of changes you need to implement to make yourself feel better. Here are some resources you might find helpful. <3
BUILDING YOUR OWN HEALTH TIMELINE
https://thyroidpharmacist.com/sample-health-timeline/
6 DIFFERENT ROOT CAUSES
https://thyroidpharmacist.com/articles/6-different-hashimotos-root-causes/
INFECTIONS AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/infections-and-hashimotos/
PERIODONTITIS
https://thyroidpharmacist.com/articles/periodontitis-a-trigger-for-hashimotos
When it comes to remission, did you know thyroid tissue can regenerate? The rate at which it does is not always predictable. Thus, some are able to stop the autoimmune attack on their thyroid and regain normal thyroid function. Others can reduce the dose of medications, and others will need to stay on the medications indefinitely. I’m
currently working on some protocols to help with tissue regeneration. Reversing Hashimoto’s means different things to different people. For some, it means a reduction in symptoms, and for others, it means a reduction in your antibodies. I had both. Here a few articles that might be helpful for you:
IS IT POSSIBLE TO RECOVER THYROID FUNCTION IN HASHIMOTO’S
https://thyroidpharmacist.com/articles/is-it-possible-to-recover-thyroid-function-in-hashimotos
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
Good day. I have been battling symptoms for years. I was actually told that at 45 I was just old and that being tired was just part of the process. I was put on an ever increasing dosage of antidepressants. Finally someone listened to me and I was diagnosed with Hashimoto’s – my antibody level was 434.4. I have been on Levothyroxine for several years and though I no longer fall asleep for 3 hours after I take my dog for a walk in the morning, I still suffer fatigue, weight gain, gastrointestinal trouble etc. Recently my TSH level was shockingly low (.167) which has never been the case. My prescription hasn’t changed and my last TSH test was 1.29 just 3 months ago. My Free T4 was 1.5 – which is pretty much where it usually is. I am so confused as to what is going on. I was just scoped to determine if I have Celiac disease. I was told I am lactose intolerant. I am struggling to make sense of everything. I have constant fatigue, bloating, gas – mostly burping, my periods – even though I was put on birth control to counteract hot flashes – have become completely abnormal – some months I don’t even have one, I have significant break outs like I haven’t had since I was a teenager – I am now 48. I feel like I am on a constant rollercoaster. I tried talking to my endocrinologist and she suggested I needed spiritual healing! I asked if I should change my diet – go gluten free (I have been vegetarian for 25 years) or cut out sugar. She said there was no need. Everything I read about Hashimoto’s suggested gluten could be troublesome so I tried going gluten free and think I did feel a bit better. I went back on gluten so that I could be officially tested and have felt horrible. I feel increasingly crazy! It seems as though doctors want to dismiss my complaints. The more they dismiss the crazier I feel! I just want to get back to the world of the living. After this long prelude my questions are 1. What does the low TSH in my last bloodwork indicate? and 2. Should I continue to push for answers or should I just resign myself to reading internet posts and messing with my diet to find what works?
Jennifer – thank you so much for reaching out and sharing your journey. I am so sorry you have had to go through this. <3 Most people feel best with a TSH of around 1 or lower and with a Free T4 and Free T3 in the upper half of the range. It is expected that your TSH will be very suppressed when optimal on NDT medication. How much thyroid replacement therapy is needed is unique and different for each person, so it's important to work with a functional medicine practitioner or a doctor, who can closely monitor your dosage and your progress. Every six weeks is usually a good schedule for testing your thyroid hormones. Please do not give up! I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It's a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/pages/clinician-database
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
http://www.thyroidpharmacistconsulting.com/recommended-compounding-pharmacies.html
Here is a research article which might help further as well:
TOP 10 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
Hi!
My anti-TPO have always been between 400 and 800 for the last ten years. In 2015, they were at almost 5,000 and my endocrinologist wasn’t worried about it. Now, I went through a major depression at the same time. They went down around 1,000 after that. I had my levels checked last week again and now they are at 3,900. Should I consider a thyroid removal? I feel like crap even though I take .88 of Levo and my TSH is within normal range. Thank you for your advise.
Maite – thank you for reaching out. I am so sorry to hear you are struggling with this. My heart goes out to you. <3 Most people feel best with a TSH of around 1 or lower and with a Free T4 and Free T3 in the upper half of the range. It is expected that your TSH will be very suppressed when optimal on NDT medication. How much thyroid replacement therapy is needed is unique and different for each person, so it's important to work with a functional medicine practitioner or a doctor, who can closely monitor your dosage and your progress. Every six weeks is usually a good schedule for testing your thyroid hormones. I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It's a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/pages/clinician-database
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
COMPOUNDING PHARMACIES
http://www.thyroidpharmacistconsulting.com/recommended-compounding-pharmacies.html
Here is a research article which might help as well:
TOP 10 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
Can a person be really agressive due to the disease?
Ana – thank you for reaching out! Anxiety symptoms are very common in people with thyroid disorders. Here are some articles which might help:
ARE YOU GOING CRAZY OR IS IT JUST YOUR THYROID
httpa://thyroidpharmacist.com/articles/are-you-going-crazy-or-is-it-just-your-thyroid
HASHIMOTO’S AND ANXIETY
https://thyroidpharmacist.com/articles/hashimotos-and-anxiety/
AUTOIMMUNE THYROID DISEASE AND ANXIETY
httpa://thyroidpharmacist.com/articles/autoimmune-thyroid-disease-and-anxiety
Hi DR. Thankyou for this amazing website. Just diagnosed with hash as a 45 year old male. TSH is at 11, thyroid antibodies 201. T3 + T4 normal. Pain in neck area. Very tired, almost impossible to stop drinking coffee in the morning. Starting meds tomorrow, and after seeing your website will seriously look at my diet + keep exercising. Plus will get back into Tai Chi. It’s very good for the immune system. When i used to do it daily i never got sick. Ever. All the best =]
Jeremy – thank you for following! <3 Fatigue was the most debilitating symptom I experienced with Hashimoto’s. It actually started 8 years before I was finally diagnosed in 2009 after I got Mono (Epstein-Barr Virus) in college. I needed to sleep for 12 hours each night to be able to function, and by “function” I mean after hitting the snooze button on my alarm clock for two hours (ask my poor husband), I would drag myself out of bed and then had to drink 46 cups of caffeine everyday to keep myself awake. I often had Red Bull and Pepsi for breakfast, and was the epitome of “wired but tired”. I hope my articles help you get started :)
OVERCOMING THYROID FATIGUE
https://thyroidpharmacist.com/articles/top-10-tips-for-overcoming-hashimotos-fatigue
THIAMINE AND THYROID FATIGUE
https://thyroidpharmacist.com/articles/thiamine-and-thyroid-fatigue
Hi Dr. Wentz, I was diagnosed with hypothyroidism this summer (TSH 4.3). My doctor ran both Hashimoto’s antibody tests which came back negative. I also believe my doctor told me that my ultrasound did not show signs of Hashimoto’s. I have had symptoms for YEARS like you mention but “normal” tests. After reading many books on hypothyroidism, I had myself tested for Epstein Barr Virus. My VCA IgG and Nuclear Angiten IgG were off the charts in the triple digits with a negative early antigen IgG.
My question is, is it possible to have non-Hashimoto’s hypothyroid with Epstein Barr virus? Or is it likely that I actually have Hashimoto’s but it hasn’t been detected? I am mostly concerned due to dietary reasons. I know if I have Hashimoto’s, I need to look at my diet and make some big changes.
Koda – thank you for reaching out and sharing your journey with me. <3 My heart goes out to you! <3 Without going into too much detail, the first of the crucial defining moments in my disease development may have started during my undergraduate studies at the University of Illinois. Due to the communal living setting of dormitories (and less than stellar hygiene habits of most college students), I had recurrent strep throat infections and even contracted mononucleosis, a viral infection caused by the Epstein-Barr Virus (EBV), which is implicated in triggering many autoimmune conditions. I received multiple courses of antibiotics as well as flu shots (which may be associated with EBV infections) and started birth control for menstrual cramps.Animal fats, broths, soups, and stews support the body’s ability to suppress the viruses. Monolaurin or lauric acid, one of the components of coconut oil, has been found to be active against the Epstein-Barr virus. Replication of any viruses including Epstein Barr is inhibited by glycyrrhizic acid, an active component of licorice root. Quercetin, Co-Enzyme Q10, N-Acetylcysteine, and glutathione were also reported to be helpful in chronic fatigue syndrome because of their anti-viral properties. It is my belief that this combination had a profound impact on my gut flora, and thus my immune system. Here is an article which you might find interesting:
EPSTEIN-BARR VIRUS AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/epstein-barr-virus-and-hashimotos
My doctors have known I had hypothyroid issues for many years, but I was unable to tolerate synthroid or levothyroxine so I went untreated for a number of years until Tirosint became an option with the medical community finally understanding sometimes it is the fillers in medications people can’t tolerate.
I did wonderfully on Tirosint. My numbers headed towards normal, I dropped a lot of weight in quick order and then maintained a level weight for about 3 years. Unfortunately, my dosage kept having to be raised every time I had blood work, but it still was working. Until recently.
About 5 months ago, it was like my thyroid just shut down completely. I’ve gained about 60 pounds despite more exercise and no changes to my diet.
My most recent blood work showed my free t4 slightly low (0.77), but my TSH is frighteningly high at 55.48!! I’m beside myself and don’t know what to do next.
Jennifer – thank you for reaching out. I am so sorry you are struggling with this. Here are a couple of things to think about.
1) What was your recent TSH, Free T3 and Free T4? Sometimes when those numbers are on the outskirts of normal, your metabolic rate may still be impaired making it more difficult for you to burn calories. Most people report feeling well with a TSH between 0.5-2.
2) What type of medication are you on? Some report more weight loss with T4/T3 combinations (Armour, Nature-Throid, compounded medications) versus T4 medications (Synthroid, Levoxyl, Tirosint) alone. T4 is a precursor to T3, but some individuals do not convert T4 to T3 properly, and the T3 component is the metabolically active one.
3) What type of diet are you eating? Some report more weight loss with T4/T3 combination vs T4 alone. Some do not convert T4 properly.The Standard American Diet (S.A.D.) full of sugar and simple carbohydrates is perfectly designed to cause us to gain weight year after year. Even yogurts that are marketed as “healthy” contain the equivalent of 16 teaspoons of sugar. Divorcing the S.A.D. is often a step that many of us must take to not just lose weight, but to also feel better. Some diets that have been helpful include the Body Ecology Diet, the Paleo Diet, the Virgin Diet, Autoimmune Paleo Diet, GAPS diet, SCD diet, Weston A. Price Diet, or the Mediterranean Diet. You may need to modify these diets to your own individuality.
Here are some resources you may find helpful as well:
BEST DIET FOR HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/best-diet-for-hashimotos-hypothyroidism
HOW TO LOSE WEIGHT WITH HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/how-to-lose-weight-with-hashimotos
HOW THE DOSE OF YOUR THYROID MEDICATION CAN UNCOVER YOUR ROOT CAUSE
https://thyroidpharmacist.com/articles/the-dose-of-your-thyroid-medication-can-uncover-your-root-cause/
Hello,
I am diagnosed with hypothyroidism and my mother has Hashimoto (as well as other family members). So, the chances are big that I probably have it to. Before it this was diagnosed though, I was diagnosed with B12 deficiency. I took shots once a week for almost a year, but we saw very little progress. Therefore, my mom thought I might have hypothyroidism, but the blood results showed just a slight difference from the norm. Therefore, it was said it was the stress. I was (/am still) experiencing stress, fatigue, difficulties with my gut/intestines, concentration issues, weight gain, feeling low etc… Therefore, we were wondering if there was a connection between B12 deficiency and hypothyroidism/Hashimoto. That when you get B12 shots, but not the levothyroxine, the effect of the B12 shots don’t work and that therefore the symptoms don’t go away. I am currently writing an essay about the connection between the two (since it is said that patients with Hashimoto have a higher prevalence of B12 deficiency). Do you maybe have any more information about this matter? And do you, maybe have scientific articles that prove the claims made in this article that I can use for my essay?
Kind regards
Kady – thank you for reaching out and sharing your journey. The most common triggers in Hashimoto’s are; nutrient deficiencies, food sensitivities, intestinal permeability (leaky gut), stress, an impaired ability to get rid of toxins and in some cases, infections. Optimizing your health starts with food. Figuring out which foods nourish you, and which ones cause you harm is the single most important thing you can learn in your health journey. I wanted to pass along these articles that I wrote. I hope they help.
6 MOST IMPORTANT NUTRIENT DEFICIENCIES IN HASHIMOTO’S
https://thyroidpharmacist.com/articles/6-important-nutrient-deficiencies-hashimotos/
How B12 Deficiency Affects Hashimoto’s
https://thyroidpharmacist.com/articles/b12-thyroid/
WHAT’S CAUSING YOUR LEAKY GUT
https://thyroidpharmacist.com/articles/whats-causing-your-leaky-gut/
Hello,
I am currently on my health journey of being diagnosed with Hashimoto’s officially 3 years ago. I had extensive blood work, which I will do again end of January. I have had my WBC count drop from 3.2 to 2.9 all within about a year and also tested for the MTHFR gene, which I have a mutation with. In your experience, are these related to the Hashimoto’s or a totally separate issue? Thanks for your input.
Tish – thank you for reaching out. These genes are not implicated in Hashimoto’s, but indirectly, having the MTHFR gene variation can help to create a perfect storm for Hashimoto’s. If you have the MTHFR gene variation, you’re more likely to accumulate heavy metals and toxins and have a more difficult time clearing them out, which, overtime, can trigger Hashimoto’s as well as cause symptoms related to liver congestion. For this reason, treating this gene variation may actually improve the symptoms you’re experiencing. Here is an article you might find helpful:
MTHFR
https://thyroidpharmacist.com/articles/mthfr-hashimotos-and-nutrients/
Thank you so much for this article, I have the genetic deposition on my mothers side both her and her sister had it. However, I am having a hard time being diagnosed and unfortunately am one of those people they as being a hypochondriac more than someone who has a predisposition. I found out I had Thyroid nodules in 2017, but my TSH was 2.7 and my Free T4 was .7 so they didn’t care about the symptoms. At that point my anti TPOs were elevated. I had hair loss, wieght gain that was fluctuating, dry skin, edema in my legs, and I’m only 36. The endocrinologist just passed me back to my primary care. I was retested last month (at my request) and my TSH was 5.01 and Free T4 was .8. They didn’t like the results so I was retested this Monday and the results came back as TSH 2.8 and Free T4 1.2. I am at a loss for words and don’t even know if I can walk into the office without them saying “we told you so, it hasn’t changed, those numbers are a fluke.” Did I mention I’m a Veteran.
Thank you,
Feeling Like a lost caused
Hope – thank you for your service and for sharing your journey with me. I am so sorry you are dealing with all of this. You are not a lost cause! <3 Most conventional physicians use the TSH test to determine if one has a thyroid disorder and to dose thyroid medications. However, this test can often times be misleading, as levels of circulating hormones may fluctuate at different times, such as in Hashimoto’s, where the person affected may fluctuate between highs and lows.
Additionally, when scientists first set the “normal” ranges of TSH for healthy individuals, they inadvertently included elderly patients and others with compromised thyroid function in the calculations, leading to an overly lax reference range. This resulted in people with underactive thyroid hormones being told that their thyroid tests were “normal,” based on this skewed reference range.
WHAT TO DO IF YOUR TSH IS NORMAL AND YOU ARE ANYTHING BUT
https://thyroidpharmacist.com/articles/what-to-do-if-your-tsh-is-normal-and-you-are-anything-but/
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all so you will have to request them. Make sure to request a copy of your labs as well.
TOP 10 THYROID TESTS AND HOW TO INTERPRET THEM
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
Hello,
I would like to thank you for all the work you’ve done here.
I have hashimoto’s for about 10 years, few years before that i was diagnosed with autoimmune hepatitis and through a change of lifestyle and adding some helpful supplements got free of it. Later i shifted my lifestyle back to being unhealthy as i thought it was alright. About a year ago my body let me know how wrong i was. My antibodies however went down on itself by half since three years ago. I know i am feeling much worse now and am trying to make my lifestyle more healthy again. But i would like to ask if it’s normal, that the antibodies come down on itself if i did nothing to help it.
PS: i havent checked TSH levels the last time, so i dont have this information, but from how i feel i guess it went worse. Also i wont write here about the levels of antibodies as the lab has some other method of testing it
Lots of love and thank you <3
Barbora – thank you for reaching out. IgG subclass antibodies have a half-life of 21 days and stick around on immune cells for about two to three months. They need constant “reminders” in the form of an antigen so that their production continues. If the antigen is removed, the antibodies will go away as well. The time period required for them to completely forget about the antigen and disappear is nine to twelve months.
The following things need to be in place for the antibodies to forget about the thyroid:
1) The thyroid stops expressing TPO.
2) The thyroid cells are not damaged and able to regenerate.
3) There are no substances that look like TPO (glandulars, gluten, infections, other triggers).
4) The immune system is balanced.
5) The autoimmune cells are confused by a decoy.
Some of these requirements are quick and easy, and others will take some time …
The thyroid will stop expressing TPO for two reasons. One of them is thyroid destruction, which we do not want; the other is thyroid suppression. Thyroid suppression is induced by limiting iodine and taking a thyroid supplement to bring TSH to 1 mIU/L or so. This can take up to three months
In the case of autoimmune conditions, traditional and alternative medicine practitioners may focus on rebalancing the immune system (i.e. steroids and immune-modulating drugs used in traditional medicine, or else herbs, supplements, or acupuncture used in alternative medicine).
While this approach may be helpful for taming the immune system in the short term or overcoming autoimmune flares, it is often a temporary solution and the immune system may become imbalanced again once the medications,acupuncture, and herbs and supplements are stopped if the underlying issue that lead to the immune system imbalance is not addressed. Thus we can say that immune modulation treats only the symptoms, and not the root cause.
As we can’t change genes, our approach to addressing the root cause of Hashimoto’s is threefold:
1) Reducing triggers
2) Eliminating intestinal permeability
3) Providing the body with nutrients to regenerate
Identifying and eliminating triggers and toxins will likely take a few weeks to a few months. Providing the thyroid with the nutrition needed to help rebuild and detoxify will likely take three to six months.
Rebalancing the immune system by addressing the root cause of autoimmunity (intestinal permeability, gut dysbiosis, infections) may take one to three years, but in the meantime, we can modulate the immune system and throw our thyroid antibodies a decoy. Hope this helps!
https://thyroidpharmacist.com/articles/hashimotos-and-tpo-antibodies/
my mom was diagnosed about 11 years ago after years of feeling tired and having other doctors write off her symptoms. then all of a sudden her muscles ate away at each other and she is now on oxygen. she doesnt tell me what all happened but do u have an idea. she is in heart failure now and I want to know what happened all I know if doctors wrote off her symptoms then finally she was diagnosed with hashimotos but it was like too late?? please I just want to know
Charlotte – thank you so much for reaching out. I am so sorry to hear about your mom. My heart goes out to you both. <3 Most conventional physicians use the TSH test to determine if one has a thyroid disorder and to dose thyroid medications. However, this test can often times be misleading, as levels of circulating hormones may fluctuate at different times, such as in Hashimoto’s, where the person affected may fluctuate between highs and lows. Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. <3 Take care of yourself
I was recently diagnosed with underactive thyroid and Hashimoto’s.
My levels are way out of whack: TSH 14.45 (.45-5.33) – TPO/AB 9864.20 (0-9) – Free T4 .54 (.58-1.64) However, I’m not super symptomatic. In fact, didn’t know I had an issue with my thyroid. I had gone to the doctor regarding pain under my left rib that I’ve had for years. I had gone gluten-free 6 years ago and recently fell off the diet. I started feeling awful, so went in for the left-side-pain. They did an allergy test and said I was not allergic to gluten, so I started eating it again. Bad idea. I felt like I was dying. So, I went back to the doctor and they ran bloodwork. The above levels are what we found. My doctor says they don’t treat Hashi’s and just wants me to start Synthroid. I’m reluctant to start a lifelong relationship with pharmaceuticals, without treating the actual issue. So I went home and started your protocol immediately. In days my symptoms left. I have an appoint in 1 month with an endo. I would like them to retest my levels then to see what diet alone does.
If I can seem to bring my levels down, do I have to go on pharmaceuticals? I rarely ever even take ibuprofen and am terrible at taking pills on time, let along every day.
I’m 54 years old, 5’4″ and weigh 139 lbs.
I’d love any advice you can offer <3
Beth – thank you so much for sharing your journey with me! I am so happy to hear you are feeling better. <3 I cannot say whether you will ever need medication as everyone is different. I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms. I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It's a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
http://www.thyroidpharmacistconsulting.com/recommended-compounding-pharmacies.html
Hello,
I am a male and my tsh has risen from the 1s to slightly over 4.5 in the last 5 years. I have 2 very small nodules diagnosed 2 years ago. T3 & T4 normal and no antobodies. Most recently my WBC count has been coming slight high (ref range 4.5-9.9) and I am 11.3, platelets very slightly above high end of ref range. I have also been on cholesterol and BP meds for years. I feel physically fine though. My 2 questions, (1) can Hashimoto raise WBC count due to chronic mild inflammation? (2) is not having the thyroid antibodies good or bad – I read that 10% don’t test positive for antobodies.
Thank you!
Ps – I am not looking for medical advice!
NG – thank you for reaching out. <3 Some people with Hashimoto’s test negative for thyroid antibodies because their overall immune health is so weak they do not produce enough antibodies. I’ve tested negative for antibodies several times. Now I’ve insisted on a thyroidultrasound. Given that Hashimoto’s is one of the leading causes of hypothyroidism worldwide, I wouldn't stop until I know one way or another. Here are the tests you need for diagnosis. Most endocrinologists don't run them all so you will have to request them. Make sure to request a copy of your labs as well. Have you done all these tests?
Top 10 Thyroid Tests and how to Interpret them.
https://thyroidpharmacist.com/articles/top-6-thyroid-tests
Here is an article where I discuss WBC counts as well:
Selenium Deficiency
https://thyroidpharmacist.com/articles/selenium-deficiency-and-hashimotos/
Hi. I was just at my Endo on Friday. She looked at my ultrasound pics and said I have Hashimotos. She said the ultrasound was indicative of it. Yet my TSH was normal and I have no antibodies. I’ve had odd symptoms for a long time, which nobody has been able to figure out. Now I’m not sure. Is it really Hashimoto’s or not? She was quite sure that it is. Now I’m confused after getting my TPO antibody test back.
Jerilyn – thank you for reaching out. <3 Some people with Hashimoto’s test negative for thyroid antibodies because their overall immune health is so weak they do not produce enough antibodies. I’ve tested negative for antibodies several times. Now I’ve insisted on a thyroid ultrasound. Given that Hashimoto’s is one of the leading causes of hypothyroidism worldwide, I wouldn't stop until I know one way or another. Here are some articles you might find helpful:
HASHIMOTO'S AND THYROID ANTIBODIES: PART 1
https://thyroidpharmacist.com/articles/hashimotos-and-thyroid-antibodies/
HASHIMOTO’S AND THYROID ANTIBODIES: PART 2
https://thyroidpharmacist.com/articles/part-2-mechanisms-reduce-thyroid-antibodies/
What is the role of lithium in Hashimoto’s? I have been taking lithium for 10 years and I’m starting to have fluctuations in TSH along with symptoms of hypothyroidism.
Ashley – thank you for reaching out. <3 Nutritional lithium is an essential micronutrient. Lithium has a long history of clinical use for supporting healthy mood and behavior. Mechanisms for this involve promoting the neurotransmitter activity of dopamine (our “happy hormone”) and serotonin (a “stress reducing” hormone). Here are some articles you might find helpful:
9 MEDICATIONS TOXIC TO YOUR THYROID
https://thyroidpharmacist.com/articles/9-medications-toxic-thyroid/
MYO-INOSITOL FOR OCD, ANXIETY, PCOS & HASHIMOTO’S
https://thyroidpharmacist.com/articles/myo-inositol-and-hashimotos/
I was diagnosed 2 weeks ago with Hashimoto’s after years of symptoms. I had an ultrasound and my thyroid is already 4cm on the left and 3cm on the right. The MD is recommending surgery. I have already gone gluten free and will also add dairy free and am on 50,000 of vitamin D once a week, as my level was 16. My question is, in your opinion, I understand you cant give “medical advice”, is surgery usually the only option with a thyroid that large. Can I still reduce the size of my thyroid? I still plan on maintaining the gluten free lifestyle I am assuming a thyroidectomy is not the over-all solution for the resolution. Your website is wonderful, as it is hard to find information on this disease. thanks.
Heather – thank you for reaching out and sharing your journey. I am so sorry you are struggling with all of this. <3 Nodules and goiters are often the result of toxicity and/or the autoimmune process. So, doing interventions to reduce the autoimmune attack on the thyroid, and toxicity, can be helpful to reduce them. Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism, it's an autoimmune disease that needs to be managed. Whether you have all, part or no thyroid, the autoimmunity still persists in most cases. We need to re-balance the immune system which begins in the gut. With the exception of discussing proper thyroid medication dosing, the majority of my website and book's focuses on balancing the immune system. The info I present is based on my own research and journey overcoming my autoimmune thyroid condition.
Here are some articles you may find helpful.
THYROID NODULES
https://thyroidpharmacist.com/articles/hashimotos-and-thyroid-nodules/
IS HASHIMOTO’S A SURGICAL DISEASE
https://thyroidpharmacist.com/articles/is-hashimotos-a-surgical-disease/
I am so thankful to have found this page. I have been suffering from extreme fatigue, heavy menstrual cycles, constipation, gaining 10 lbs for no reason, and few other issues for several months. As an athlete I have seen my abilities start to wane no matter how hard I train. Coupled with fighting this fatigue, it has been literal misery. I finally went to the Dr. and had labs drawn for thyroid. I had low TSH levels, everything else “was in range” but my protein was low. I am nearly a carnivore eating mostly high protein meats, so this was a curious find. The Dr. told me I am fine. I again expressed that something is wrong and I feel like I am dying- this is not an exaggeration of how I am feeling. I had labs drawn at an urgent care, the Dr. there is familiar with thyroid issues as his wife has low thyroid. He diagnosed me as sub clinical hypothyroidism and helped me get into a different PCP. I saw them this week and they feel it is Hashimoto’s, but are not testing for that for a few weeks when they do the blood draw to recheck the thyroid levels. I have been devouring info. Learning of triggers and thinking about days that I felt more horrible than others and the things I did the day before has been insightful. After 3 weeks of a low dosage of thyroid rx, I do feel noticeably better some days, but other days I have felt like I did before starting the rx. I just want to get back to competing at the level I was a year ago, and do it without feeling so awful. Any thoughts on being a competitive athlete with Hashomoto’s? Thank You for this page and all of the insight. It has been more helpful than you’ll ever know.
Christina – thank you so much for reaching out and sharing your journey with me. <3 I'm so sorry you are struggling with all of this. I would recommend anyone embarking on a program of exercise starts slowly and progresses at their own pace. Exercise can be very healthy, but for people with Hashimoto’s it can create stress. Stress causes our adrenals to pump out extra hormones, and shifts our body from a relaxing, digesting, healing state to a fight or flight state. The body’s energy is shifted from doing “useless” things like growing beautiful hair, metabolizing, making hormones, digesting and repairing itself, and instead, all of the body’s resources are reserved to make cortisol and adrenaline that is pumped through our veins so that we can keep going. Eventually, we run out of nutrients that are required for proper adrenal function and we get to a state of adrenal fatigue. This is when our body is no longer able to heal itself and we feel drained. Replenishing nutrients and using adaptogens, that balance out the adrenals can be helpful for everyone. You may find this article helpful as well:
ARE YOUR ADRENALS SABOTAGING YOUR HEALTH?
https://thyroidpharmacist.com/articles/are-your-adrenals-sabotaging-your-health
Thank you for all you do, Dr. Wentz! I recently received not-so-great lab work related my TSH, T3, T4, and Antibodies and started reading all 3 of your books (which have been SO HELPFUL so far – thank you!!). I have been chewing Orbit Peppermint gum for years – probably upwards of one pack a day – and am wondering if this is contributing negatively to my Hashimoto’s. I realize this is an odd question, but was wondering if chewing gum is inherently bad. Orbit’s first ingredient contains Sorbitol (I know you’ve written about Stevia and Xylitol in the past stating that it would be okay but I haven’t seen anything written about Sorbitol). I do suffer from bloating – at time I look like I am 4 months pregnant – but I don’t have issues with bowl movements. Thank you in advance for your help! Really appreciate it.
Lindsey – thank you so much for reaching out and sharing. Everyone is different, the best way to see if you are reacting to a food would be to eliminate it for a period of time. The gold standard or the most accurate test for uncovering reactive foods and individual food sensitivities is actually the elimination diet. In contrast to other diets that simply exclude common problematic foods, an elimination diet is done to determine what particular food intolerances the individual may have. An elimination period of at least 2-3 months is a good starting place, but you may want to continue if you feel that you still have more healing to do. Then you can try a new food every 4 days and monitor yourself for reactions. Going through an elimination diet will help you figure out your own individual food triggers and your specific response to each trigger food. Here is an article I hope you find interesting!
https://thyroidpharmacist.com/articles/elimination-diet-for-hashimotos
Is it weird that they didn’t do an ultrasound after I was diagnosed with Hashimoto’s? I’m not hypothyroid but after two years of INSANE hive and angiodema breakouts and tons of doctors’ visits with no answers, a PA at a dermatologist ordered extensive blood testing because he suspected I have Hashimoto’s and he was right. My TSH is actually on the low side (1.04), and even though I’m experiencing symptoms (AIP has helped immensely in managing) the only options presented to me by the endocrinologist were to put me on a low dose of levothyroxine, even though that would potentially make me hyperthyroid with my low TSH, or, of course “wait and see”. I just think it’s weird that I’m experiencing symptoms but no other imaging or testing was done after the initial bloodwork.
Megan – thank you for reaching out. <3 I understand how frustrating this is. I recommend getting an ultrasound done at least once every 1 to 5 years, if everything looks normal. If you have nodules, you may want to do that more often—once every two years. Most people feel best with a TSH of around 1 or lower and with a Free T4 and Free T3 in the upper half of the range. It is expected that your TSH will be very suppressed when optimal on NDT medication. How much thyroid replacement therapy is needed is unique and different for each person, so it's important to work with a functional medicine practitioner or a doctor, who can closely monitor your dosage and your progress. Here is a research article which might help further:
TOP 10 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
A chronic sore throat and hoarseness led to the discovery of nodules on my thyroid (by ultrasound). My TSH was .95 so the doctors did no further blood work. Biopsies of 2 of the nodules were benign (that’s all the information the endo gave me). The nutritionist I have been working with for gut health (multiple food allergies) ordered a full thyroid panel for me, but aside from low total T3, thyroid function seemed OK and antibodies were normal. But then I got the actual biopsy report, which states that one of the nodules is “consistent with lymphocytic (Hashimotos) thyroiditis in the correct clinical setting.” I don’t know if I need to be concerned about this. Obviously I need to be proactive and get my gut health and adrenal health under control (significant life stressors have been a MAJOR factor this past year and I do not feel well), but do I have serum negative Hashimotos or not, since my blood work is normal? I need a new doctor, that’s for sure, because communication has been terrible. The only reason I even know what my antibodies, free T3 and free T4 are is because I took it upon myself to get further testing–the endo just said, see you in a year for another ultrasound and TSH. She completely ignored my symptoms.
Danielle – thank you so much for reaching out and sharing your journey. <3 I understand how hard it is to find a doctor who will listen! Nodules and goiters are often the result of toxicity and/or the autoimmune process. So, doing interventions to reduce the autoimmune attack on the thyroid, and toxicity, can be helpful to reduce them. Here is an article I wrote that might be helpful:
THYROID NODULES
https://thyroidpharmacist.com/articles/hashimotos-and-thyroid-nodules/
I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms. I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It’s a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Thank you for this clear article which I am passing on to my GP. I closely follow your work. My question is related to during the tests that led to my original diagnosis in 2013, following several years of what I now know to be hypo symptoms, the thyroid scan did not take up any dye whatsoever. With standard hormone replacement dosages and numerous vitamin and mineral supplements, my results for T3/T4 and antibodies are now within normal ranges but I still have issues especially with depression and fatigue and low libido. Is there any value in the case of a dead thyroid gland in pursuing LDN? If so, I will also give the doctor your LDN article too. We do have a local compounding pharmacist. Thank you.
Kerrie – thank you for reaching out and sharing my research! I do recommend that you discuss the use of LDN with your practititoner. <3 Low Dose Naltrexone (LDN) is an immune modulator that can be used to prevent further damage to the thyroid while one is looking for their root cause or to rebalance the immune system when the root cause cannot be found. Root causes are different for different people but may include infections or food sensitivities that result in an immune imbalance. Appropriate levels of Vitamin D, full spectrum light exposure, food sensitivities all play a role in autoimmunity and need to be considered as well. It’s also best to work with a compounding pharmacy that can help you titrate your dose correctly. This article gives the full details:
LOW DOSE NALTREXONE AND HASHIMOTOS
https://thyroidpharmacist.com/articles/low-dose-naltrexone-and-hashimotos
What stage would Hashitoxicosis be considered?
Lila – thank you for reaching out. <3 When thyroid cells are broken down, they release thyroid hormones into the bloodstream. This causes thyroid hormone surges (or a transient hyperthyroidism known as thyrotoxicosis or Hashitoxicosis). Here is an article you might find helpful: https://thyroidpharmacist.com/articles/the-many-faces-of-hashimotos/
Thank you for the great article. I wish this was around when I was younger. I was first diagnosed with anemia around 11 and then thyroid issues around 17 but I had the symptoms for 3 years prior to being diagnosed. I was diagnosed with RA and Sjogrens at 40 and now Lupus, and Sub-cutaneous Lupus at 50. I have seen 2 functional medicine doctors and I firmly believe that the detox program he had me on caused my Lupus. I have been gluten free for 10 years and soy, dairy, egg, corn, mushroom and pineapple free for 5 years. On a recent trip to Italy I discovered that goat and sheep’s milk cheese does not bother me like regular dairy. The most recently Functional Medicine doctor said I had SIBO as well. Should I look to “cure” that first as all issues start in the gut?
Lynda – thank you for sharing your journey. <3 We know that intestinal permeability (aka leaky gut) is present in every case of autoimmunity and often precedes the development of Hashimoto’s. According to the Institute of Functional Medicine, many people develop IBS 5-10 years before an autoimmune diagnosis. I was one of them and didn’t take my gut health as seriously as I should have. Gut problems are often caused by infections like H. pylori, parasites like Blasto, SIBO, an imbalance of bacteria, and enzyme deficiencies or food sensitivities (especially to gluten, dairy, and/or soy). Even stress can be a factor in gut permeability. Conditions that I have found to respond really well to the Hashimoto’s protocols have been rheumatoid arthritis, lupus, Celiac disease, irritable bowel syndrome, eczema, asthma, Graves’, premature ovarian failure, psoriasis, Alopecia Areata, and Sjogrens. I have also seen the protocols help with Fibromyalgia, chronic fatigue syndrome, PCOS, as well as Type 2 diabetes, Crohn’s, and Ulcerative colitis. Here are some articles you might find interesting.
6 DIFFERENT ROOT CAUSES
https://thyroidpharmacist.com/articles/6-different-hashimotos-root-causes/
IMPORTANCE OF GUT HEALTH
https://thyroidpharmacist.com/articles/importance-gut-health/
Hi, Dr izabella🙂
I’m very glad that I found your website. It is very informative!
I was recently diagnosed with hashimoto’s disease and by reading this article I am on stage 2.
Since my tsh, t4 and t3 levels are normal, my doctor told me that I don’t need to be on medication and I’ll just have to have a blood test once or twice a year.
I also do get stomach pain occasionally but my doctor told me that it’s not related to hashimoto’s however now that I have read your article, I’m thinking that it may be related.
I would like to know if hashimoto’s disease worsen over time. Since I have high levels of tg and tpo antibody, will I have stage 3 hashimoto’s as I get older?
Noreen – thank you for reaching out. There are 5 stages to thyroid disease. A conventional doctor won’t look at stopping the autoimmune attack progressing. What we usually see is that a person with only thyroid antibodies and normal TSH is considered to be in Stage 2 of thyroid disease, a person who has an elevated TSH with normal T4/T3 with or without thyroid antibodies, is in Stage 3 of thyroid disease, a person with elevated TSH, lowered T3/T4 +/- thyroid antibodies is in Stage 4 of thyroid disease, regardless if she/he has thyroid antibodies or not. Stage 5, is when the person progresses to other types of autoimmune disease. Functional medicine doctors really aim to find and treat underlying causes and prevent serious chronic disease rather merely treat disease symptoms. Here are some resources you might find helpful:
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid/
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
You may also like to check out the doctors that other patients recommend on this list:
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
Hi Dr. Wentz,
I have been experiencing a number of symptoms for 15 years, with that number increasing in size and severity over the last few. Recently, I was doing research for something I thought was unrelated, but lead me to the thyroid. I have every single symptom plus the ones that have shown connections/links. I made my doctor check my levels, and and while my tsh, t3, and t4 are within normal range at the time of testing, both my TPO AB and Thyroglobulin AB are high, TPO nearly 2000. My grandmother was diagnosed very late in life with Grave’s and my mother in her 40s with Hypothyroidism. The doctor is saying I’m fine and that the antibodies might be passed down from my mom/grandma, but I am very symptomatic. I understand you can’t answer in specifics due to legal reasons, but can you at the very least tell me if this is something you’ve seen? Can I be symptomatic and have a large amount of antibodies and not have Hashimoto’s? I have also been grain-free and dairy free for years as a personal choice, over-exercise and eat extremely healthy because I gain weight easily if I don’t. So he kept calling me “healthy,” despite not feeling that way at all.
Molly – thank you for reaching out. Antibodies are a sign of an autoimmune attack on the thyroid, which indicates an autoimmune thyroid disease like Hashimoto’s or Graves’. If the attack on the thyroid gland persists, the damage done to the thyroid will progress, and symptoms may appear as you progress from the early to later stages of Hashimoto’s. But the good news is we can reverse this progression and put autoimmune disease into remission by addressing the underlying root causes of it, such as food sensitivities and infections. Here is an article you might find helpful:
5 STAGES OF HASHIMOTO’S THYROIDITIS
https://thyroidpharmacist.com/articles/5-stages-hashimotos-thyroiditis
I believe that’s this article. The doctor is saying that my anti-bodies could be inherited despite there being nearly 2000 of them. Can that actually happen? So I definitely have an autoimmune disease if I have that amount? And thank you!
Molly – thank you for reaching out! ❤️ Antibodies are a sign of an autoimmune attack on the thyroid. Addressing the root causes of the autoimmunity can help reduce them as well as symptoms. As for genetics, three things MUST be present in order for autoimmunity to occur…
1. Genetic predisposition
2. Environmental triggers
3. Intestinal permeability (leaky gut)
Developing autoimmunity is like a three-legged stool, all of these factors must be present for autoimmunity to occur! When you remove one of these, you can prevent or stop autoimmune disease. While we can’t change genes, if we know the trigger, we can remove it and we can heal the gut. Here are some articles I hope you find helpful:
HASHIMOTO’S AND THYROID ANTIBODIES: PART 1
https://thyroidpharmacist.com/articles/hashimotos-and-thyroid-antibodies/
HASHIMOTO’S AND THYROID ANTIBODIES: PART 2
https://thyroidpharmacist.com/articles/part-2-mechanisms-reduce-thyroid-antibodies/
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
http://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm
IS HASHIMOTO’S HYPOTHYROIDISM GENETIC?
http://thyroidpharmacist.com/articles/is-hashimotos-genetic
Hi,
I have had Hashimoto for appr. 10 years and I am on medication. I have less than 0.1 ng/mL thyroglobulin in my last lab tests. Does that mean I am at stage 4 and that I have no more thyroid? Is there still anything I can do?
Florian – thank you for reaching out. Thyroid tissue can regenerate, but the rate at which it does is not always predictable. Thus, some are able to stop the autoimmune attack on their thyroid and regain normal thyroid function. Others can reduce the dose of medications, and others will need to stay on the medications indefinitely. Reversing Hashimoto’s means different things to different people. For some, it means a reduction in symptoms, and for others, it means a reduction in your antibodies. ❤️ I had both. Here’s an article that might be helpful for you:
https://thyroidpharmacist.com/articles/is-it-possible-to-recover-thyroid-function-in-hashimotos
Hi,
How does taking Levothyroxine affect my lab results?
How can I know in which stage I am if I am taking Levothyroxine?
Thank you in advance for your response 😊
Elias – thank you for following. If you are taking a T4 only medication such as levothyroxine, you can go ahead and take your medication in the morning before the test. T4 medication has a long half-life, and your levels will be stable regardless of when you take it. If you take a T3 medication on the other hand, or a combination of T3/T4, T3 has a shorter half-life so your blood work may not be reflected accurately. It will appear that you have more thyroid hormone on board than you do. Thus it may be helpful to delay your morning dose of a T3/T4 medication until after you do the test to see (try to schedule the test in the morning). Here is an article that I hope is helpful.
HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications/
My DIL was diagnosed with a very high TSH of over 10 after delivery of her 3rd child. pregancy was normal, and she felt good. She was put on synthroid. This has een 2 yrs ago and it continues to worsen. Can pregnancy and?or delivery trigger hashimotos?
Tammy – thank you for sharing. I’m so sorry your DIL is still not feeling well. Yes, pregnancy can often be a trigger for developing Hashimoto’s or for an autoimmune flare – iron deficiency and immune shift, as well as potentially the baby’s thyroid cells that circulate in the body, may be a trigger. You might find these articles interesting.
ESTROGEN DOMINANCE AS A HASHIMOTOS TRIGGER
https://thyroidpharmacist.com/articles/estrogen-dominance-as-a-hashimotos-trigger/
WHY WOMEN HAVE MORE THYROID DISORDERS
https://thyroidpharmacist.com/articles/women-thyroid-disorders/
Over 20 years ago I was diagnosed with Hypothyroidism, Hashimoto’s disease and Autoimmune Neutropenia ( we have no idea what caused the neutropenia). For the past 20 years my health has been a battle of ups and downs, many doctor’s, many tests more diagnoses. To date I currently have approx. 10 different autoimmune diseases (plus additional diagnoses) and they just keep coming. I am currently dealing with an out of control thyroid, my recent TSH was low,0.135 free T3 – 3.36 and T4 – 1.46 were normal, my TPO was 206.30, and Thyroglobulin was 12, both well above where they are supposed to be. My doctor has been struggling manage my numbers and symptoms at the same time. My hair has been falling out, I have about half as much hair as I had six months ago. I have been taking Collagen to try to preserve what I have left. My pain level has increased despite being on LDN (and increasing the dose), my fatigue has gone up. I am currently receiving Octagam Infusions once a month in hopes of getting my immune system to calm down. My current white blood cell count is 2.7, ANC. 490, absolute Neutrophil Count 0.5. Four the past 4 months I have been having gut issues and don’t seem to be resolving. I just had a thyroid ultrasound of which I was told there are nodules and the left side of my thyroid has shrunk and is considerably smaller than the right (this came from the ultrasound tech, I don’t have the official results) she showed me the right and left lobes I could clearly see the difference. I have to manage my care very closely because when doctor’s see my immune numbers they start to panic and wonder why I am not currently in the hospital, they are not good numbers. It is so frustrating that I am still fighting this health issue, I am need to be healthier and feel like I can function and not walk around like a zombie. I want to live not just exist. My husband stumbled across your information so I am reading it now, but I would be open to any advice, thoughts, ideas, help, anything you can offer!!
Kathy – thank you so much for sharing your journey. I’m so sorry you are struggling with all of this. I do understand how hard it all is. Hashimoto’s is often a combination of food sensitivities, nutrient deficiencies, adrenal issues, gut issues as well as an impaired ability to get rid of toxins. Any of those things would prevent a person from getting better. Hashimoto’s is very much an individual condition. While there are root cause commonalities, each person will have their own or in some cases, more than one root cause. Oftentimes patients will have additional autoimmune conditions as well. Most autoimmune conditions have common root causes, and a lot of times the things that are recommended for one autoimmune condition will help with others. Conditions that I have found to respond really well to the Hashimoto’s protocols have been rheumatoid arthritis, lupus, Celiac disease, irritable bowel syndrome, eczema, asthma, Graves’, premature ovarian failure, psoriasis, Alopecia Areata, and Sjogrens. I have also seen the protocols help with Fibromyalgia, chronic fatigue syndrome, PCOS, as well as Type 2 diabetes, Crohn’s, and Ulcerative colitis.
You will have to start with the simplest modifications, by removing triggers, followed by repairing the other broken systems to restore equilibrium, allowing the body to rebuild itself. You will need to dig down to why the immune system is imbalanced in the first place and this will tell you how you begin to finally feel better, reduce your thyroid antibodies and even take your condition into remission. You will have to create your own health timeline. Look back at your overall history as far back as you can remember. Look for infections, periods of severe stress, the use of medications (especially antibiotics, antacids, and oral contraceptives), accidents, and exposure to toxins. These are events that may have contributed to Hashimoto’s. Once you do, you will know what types of changes you need to implement to make yourself feel better.
If you need further support, please check out the list of lab tests inside the “Testing” chapter of my book, Hashimoto’s Root Cause. I also offer a 12-week program, Hashimoto’s Self Management Program. Here are some resources I hope you find helpful as well. ❤️
BUILDING YOUR OWN HEALTH TIMELINE
https://thyroidpharmacist.com/sample-health-timeline/
Hashimoto’s Self-Management Program
https://thyroidpharmacist.com/enroll-in-hashimotos-self-management/
ROOT CAUSE RESET
https://thyroidpharmacist.com/enroll-in-root-cause-reset/
This has been really helpful. I am really struggling to understand why a biopsy of my thyroid nodule indicates “cytologic findings are suggestive of hyperplastic nodule in the setting of lymphocytic (Hashimoto) thyroiditis”, yet my labs and antibodies are fine. Does this simply mean I have the autoimmune disorder, but it hasn’t yet damaged my thyroid? The nodule is on my isthmus and I talked with a surgeon who suggesting removing it (isthmus because nodule is contained within it). It has been growing over the last 2 years. I am not sure if this is the right thing to do. Will it help to remove this? Is my hashimoto contained in this nodule or will removing it cause more problems down the road?
Amy – thank you for sharing. I’m so sorry you are struggling. Nodules and goiters are often the result of toxicity and/or the autoimmune process. Addressing nutrient deficiencies in iodine, selenium, and vitamin D, clear out any toxins by opting for natural products to lessen the burden on your liver, changing your diet and removing foods that you are sensitive to, balancing your blood sugar, and addressing estrogen dominance, are interventions that can help. Here is an article you might find helpful as well:
THYROID NODULES
https://thyroidpharmacist.com/articles/hashimotos-and-thyroid-nodules/
hi dr wentz, thanks for this helpful article. i’m very stuck regarding what to do for my thyroid, as i’ve had hashimoto’s since 2004 (on euthyrox w/o concern), but i have a 3.7 cm nodule and i now have to decide between radiofrequency ablation and partial thyroidectomy. i’m on nearly a full thyroid replacement dose so i don’t think removing half of my thyroid would be tragic but i’m also hopeful that RFA would be successful, but i also know it introduces inflammation to the gland as well. do you have any thoughts? thanks!
Kate – thank you for reaching out. Nodules and goiters are often the result of toxicity and/or the autoimmune process. Addressing nutrient deficiencies in iodine, selenium, and vitamin D, clearing out any toxins by opting for natural products to lessen the burden on your liver, changing your diet and removing foods that you are sensitive to, balancing your blood sugar, and addressing estrogen dominance, are all interventions that can help. Here is an article you might find helpful as well:
THYROID NODULES
https://thyroidpharmacist.com/articles/hashimotos-and-thyroid-nodules/
This article helped me make a break through. For the last 10 years, my health has changed. I have seen neurologist, rheumatologist, gastroenterologist, allergist, one internal medicine doctor, and a multitude of primary care doctors. Not a single one tested my TSH levels, nor did they test for Hashimoto’s. If it were not for this article, I would continue to suffer, undiagnosed, and untreated. From the bottom of my heart to the top of my future health, thank you!
Tricia – Thank you so much for sharing!❤️❤️❤️ It makes me so happy to hear that you have found my research helpful. Please keep me posted on your progress.
I was diagnosed with thyroid problems when I was 18. I’ve lived a life of up and downs. I’ve been so tired, I could not take one more step. I’m 53 now and I can’t be more tired of it. Over 30 yrs of meds that do not work. No one believes how you feel. I’m ready to either do something about it, or else. Now I have a little hope. Reading your articles and hopefully books. But I still want to talk to someone about it. I am really greatful I was referred to look you up!
Chris – thank you for reaching out and sharing your journey. I’m so glad you are taking charge of your health and finding my resources helpful. Don’t give up! I believe that everyone needs to find a practitioner that will let them be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It’s a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
COMPOUNDING PHARMACIES
https://thyroidpharmacist.com/database-recommended-compounding-pharmacies/
Hi Dr. Wentz, what’s your experience or knowledge on LDN increasing hormones like ACTH/cortisol? I’ve seen this in studies in higher doses and personally experienced it at 4.5 mg. Do you believe this mechanism of action is inevitable irrespective of dose? I want to try it again for my Hashimoto’s but am turned off by this finding. Thanks!
Kate – thank you for reaching out. I recommend discussing your concerns with your practitioner to help you determine if its an option for you and your health needs as everyone reacts differently. This is something I have not yet researched but will add it to my list to look into further and share my findings when I do. ❤️ If you would like to share the studies you have found please feel free to email them to my team at info@thyroidpharmacist.com and they will pass them on to me.
As I look back to the first signs of Hashimotos and Celiac, that would have started in the mid 60’s, a couple of years after I suffered horrific reactions to the OPV and Tetanus vaccine. I went undiagnosed for almost 50 years. In that time I not only developed Hashis and Celiac, but the Celiac skin disorder, Dermatitis Herpetiformis or DH, environmental allergies, IBS, and Fibromyalgia. AFter blood work was done proving Hashis and Celiac, I went gluten free, which helped to a certain degree. It was only 6 years later that I discovered the relationship of DH to Celiac that I went completely grain free, soy free, nothing with yeast or molds, and no foods high in iodine or sugar. That is when my health took a major turn for the better. I have tried taking T3, T4, Synthroid, and Armours with no success, just terrible reactions. I have to allow my food to be my medicine as pharmaceuticals are my worst enemy. My only question here is, is there a correlation between Hashimotos and high cholesterol?
Catryna – thank you for sharing your journey. Cholesterol can be elevated for a variety of reasons. One of the reasons why cholesterol may be elevated is actually due to hypothyroidism. Sometimes you will get a person on a thyroid medication and their cholesterol will actually normalize. Another reason may be due to adrenal issues. A person with adrenal dysfunction might see higher levels of cholesterol occurring, because adrenal hormones are made from cholesterol. Basically, it’s the body’s way of trying to get more of a supply of cholesterol, to make more adrenal hormones. So, supporting your adrenal function may be something to look into. You could do that with the B vitamin, vitamin C, and then doing an adrenal saliva test. Here is an article with more info:
ARE YOUR ADRENALS SABOTAGING YOUR HEALTH?
http://thyroidpharmacist.com/articles/are-your-adrenals-sabotaging-your-health
DID YOUR THYROID CONDITION START OR WORSEN DURING PERIMENOPAUSE
https://thyroidpharmacist.com/articles/thyroid-condition-start-worsen-during-perimenopause/
Thank you so much for this article! I’ve been struggling with symptoms for years. My TSH levels have been in the 1-2 range until the last 5 years when they went to the 2-3 range. One July 1, my level doubled from a year and a half ago to 4. My PCP keeps saying I’m in normal range, but I’ve been trying to get help for these symptoms for a couple of years. Fatigue, anxiety, hair loss – especially my eyebrows, and now significant (30lbs) weight gain. As I read up on hypothyroidism, I see that I have almost all of the possible symptoms and have had a few of them for over a decade.
Can you recommend someone to see near me (Grand Rapids, MI) who will actually look at my history and my number s and my symptoms and allow me to try medicine? I’m willing to do whatever it takes to get this under control. The side effects have been near devastating in my personal and professional life. I feel like my PCP and team aren’t trying to help. In fact, I get pushback in asking for testing. They even wrote to me yesterday and used the wrong name in the email.
I’m feeling so discouraged and just want help. I’m willing to travel to have someone help me. Any recommendations you could give would be so appreciated!
Thanks,
Amy
Hi Amy, thank you for following. I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and preventing serious chronic disease rather than treating individual disease symptoms. Check out these resources:
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Recommended Compounding Pharmacist list
https://thyroidpharmacist.com/database-recommended-compounding-pharmacies/
Please help us. My grandson is eight years old. I adopted them five years ago. I am their only parent they have left. He got sick in November with severe jaundice and his liver and kidneys hurt really bad. He has crystallized urine and also we have found something with his thymus gland. It is too small I believe and his lymph nodes have calcified now he is not growing and he is not retaining nutrition, even with medicine to be hungry. He is still not hungry. He is the size of a four year-old and he is very pale and weak and very tired and getting sick every day we are treating with Specialist but they still do not have answers. It has gone on so long and his fading away. He has diagnosed with Hashimoto. He’s on 75 mg His bones ache and he has severe headaches in the left side of his brain all the time he has trouble breathing sometimes and food seems to make him feel better when his liver starts hurting he gets jaundice and then turns pale and back-and-forth very quickly changes coloring. He falls asleep regular now Quite often because he’s so tired. He doesn’t have energy at all, and he cries all the time because he’s so sick we’ve had low red blood cells, high blood platelets and a fluctuation with the white blood cells going up and down. He also has enlarged red blood cells on every test. Can you help us please?
Jacqueline, Thank you so much for reaching out, and I’m truly sorry to hear about what your grandson is going through. My work primarily focuses on adults, but I recommend working closely with a functional medicine practitioner experienced in pediatrics if you’re not already. In general, many children with autoimmune conditions benefit from a nutrient-dense diet that’s free of gluten, dairy, and soy, with a focus on vegetables, clean proteins, and fermented foods to support gut health. Please email my team at info@thyroidpharmacist.com and they will be happy to share some resources I’ve collected as well. I know how overwhelming this must be, and I’m sending you and your grandson so much love and strength as you continue seeking answers and healing. ❤️