Wouldn’t it be amazing if we could find the one doctor who could give us a magic pill to make all of our problems go away? We would lose weight, grow our hair back, have energy again…
While there may not be one magic pill out there, finding the doctor who is right for you, can change the course of your health journey and put you on the path toward healing.
I recommend that everyone with Hashimoto’s consult with a healthcare professional. Even if you are extremely knowledgeable about Hashimoto’s, it helps to have an objective individual to bounce ideas off of, help you identify potential triggers of your condition, and resolve them.
That said, one of the questions I hear the most from my readers is: “What type of doctor should I see for Hashimoto’s?”
The sad reality is that many patients are often disappointed after meeting with conventional doctors, who tell them that there is nothing that can be done about the autoimmune attack on the thyroid. Such doctors only prescribe one type of thyroid hormone, don’t dose the thyroid hormones correctly, and leave their patients feeling miserable!
In this article, I’d like to offer some information about the conventional approach to thyroid care, versus a Root Cause approach, and how to find a doctor who can help you meet your wellness goals.
Read on to learn:
- The conventional approach to thyroid treatment
- The Root Cause approach to treating Hashimoto’s
- Different approaches to medication management
- Questions to ask your practitioner
- Insurance concerns
The Conventional Approach
The conventional approach to treating Hashimoto’s focuses on looking at one particular organ or function (the thyroid), versus looking at the body as an integrated whole.
Here are the typical recommendations made for those with Hashimoto’s:
1. The standard of care approach to Hashimoto’s, practiced by most conventional doctors and endocrinologists, is focused on testing for low levels of TSH (thyroid-stimulating hormone) if a patient presents with a series of known thyroid symptoms.
The issue with this for someone with Hashimoto’s is that it is not a “preventative” test, and a person with Hashimoto’s may appear to have normal TSH levels and be told they are fine… for years.
TSH often tests as abnormal only after a lot of damage to the thyroid has already been done. There are five stages of disease progression in developing Hashimoto’s, and TSH doesn’t usually test as abnormal until stage 4!
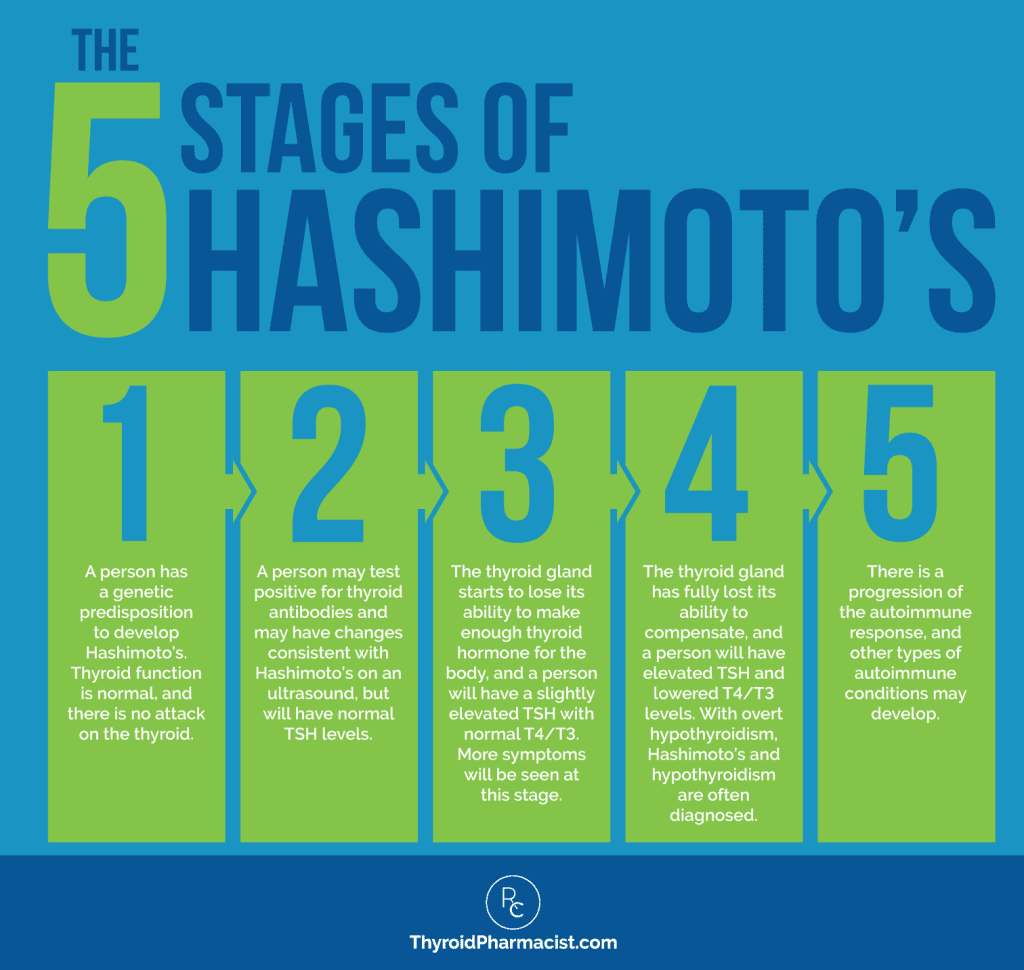
If your thyroid labs appear “normal,” you’re likely going to be told that there is nothing you can do, other than wait until the thyroid is destroyed to the point that you will need thyroid medications.
2. If thyroid levels are deemed “abnormal,” levothyroxine (T4) is the thyroid hormone of choice prescribed to most people with Hashimoto’s.
However, patients are frequently not dosed on medication appropriately because outdated and cookie-cutter lab reference ranges are used. These measure the levels of thyroid hormone in the pituitary gland, but not in the rest of the body. (Furthermore, I’ve found that many clients respond better to non-T4-centric hormone medications. This is because some people’s bodies don’t adequately convert T4 to T3, so they may need a combination T4/T3 medication for optimal support. (As a pharmacist, I take appropriate medication use seriously. Please check out my article on thyroid medication options to learn more.)
3. Thyroid medications are expected to address a patient’s symptoms, and patients are often told that they should begin feeling better in a few weeks. Once on this prescription-only path, a patient will likely have limited follow-ups that are focused primarily on the medication’s effectiveness at improving their TSH levels. TSH levels may improve, but the patient’s condition can worsen, as Hashimoto’s is progressive and their immune system will likely continue to attack the thyroid (if the underlying root cause of the condition is left unaddressed).
Many have gone to conventional doctors to seek help for specific symptoms like brain fog and weight gain, only to be given limited recommendations such as “Perhaps you’re just getting older”, or the often hurtful “Exercise more and eat less” (which of course can make things worse if you have impaired thyroid and adrenal function).
Patients who continue to be symptomatic are often referred to other specialists for additional medications to target symptoms, such as dermatologists for hair loss, or psychiatrists for depression. These symptoms are not recognized as being related to the autoimmune thyroid condition or its root causes.
4. The conventional approach is about managing the “disease” rather than offering the support and tools needed to help patients fully recover. There are usually no lifestyle recommendations or attempts to find triggers for the autoimmune response against the thyroid, and one’s thyroid antibodies are rarely even tracked. (However, the progression, or regression, of Hashimoto’s can often be tracked by monitoring fluctuations in one’s thyroid antibody levels, as higher antibody counts are usually correlated to a greater autoimmune attack on the thyroid. Read more about that here.)
5. The conventional approach limits its focus to the particular follow up appointment and labs, monitoring the medication’s effects at each visit, instead of having a practitioner truly partnering with the patient to figure out why their bucket is leaking in the first place (and what they can do about it).
There is never a focus on making the autoimmune issue better! Instead, the condition is seen as “irreversible”, but patients are told that medication will at least supply the body with the hormone (which the thyroid is no longer able to produce on its own) that it needs.
So, Should I See an Endocrinologist?
One of the common questions I receive from readers is whether they should see an endocrinologist once they have been diagnosed with Hashimoto’s.
Oftentimes, patients think that endocrinologists will have access to the latest and greatest advances in medicine, but this is not necessarily the case with Hashimoto’s.
While I have the utmost respect for the profession of endocrinology and believe that every person who has been diagnosed with Hashimoto’s should see an endocrinologist at least once for a full evaluation and a thyroid ultrasound, many patients with Hashimoto’s end up disappointed with the care they receive from their endocrinologists and conventional doctors.
This is because the conventional medical approach to treating thyroid disease focuses on replenishing thyroid hormone levels with the use of synthetic thyroid medications once the “thyroid has burned itself out” and can no longer produce its own thyroid hormones.
While there is a time and place to see an endocrinologist, I recommend that most people with Hashimoto’s find a functional medicine-minded practitioner who can help dig for root causes and take an individualized approach to treating the condition.
The Root Cause Approach
Most conventional doctors have not been trained in the root cause approach. When asked what to do about the immune imbalance that triggered the autoimmune disease in the first place, they, unfortunately, don’t have any answers.
Oftentimes, conventional doctors will kindly offer to test you for other autoimmune conditions, as the underlying immune imbalance can translate into the development of new autoimmune conditions if not addressed, but they will NOT test you for underlying root causes of the autoimmune condition.
Why?
Simply, because this is not something they have been trained in — much of their training is focused on identifying a condition, and using medications and/or surgery to treat the condition.
My training in pharmacy school was very much the same. “If someone has ‘X’ disease, you recommend ‘Y’ drug!” I learned about helpful lifestyle changes for a few of the conditions as well, but to be perfectly honest, the lifestyle recommendations were severely lacking in my training.
Furthermore, most conventionally trained doctors, pharmacists, and nurses are not trained in root cause resolution. I was never told that adrenals, food sensitivities, toxins, nutrient deficiencies, digestive issues, and infections could create chronic autoimmune illness within the body, and that addressing these issues can help a person feel better and even result in remission.
In contrast, the Root Cause approach focuses on why your immune system may be out of balance in the first place.
The Root Cause approach focuses on figuring out what triggered your condition, what can exacerbate your condition, as well as the interventions that can make you feel better, reduce the attack on the thyroid gland, prevent you from getting another autoimmune condition, and get your condition into remission.
This approach to Hashimoto’s is patient-centered and looks at the underlying issues and the person’s individuality.
The Root Cause Approach to Hashimoto’s involves:
- Utilizing comprehensive thyroid tests to determine diagnosis and the need for thyroid hormone therapy.
- Using optimal and functional ranges of thyroid hormones instead of outdated reference ranges.
- Optimizing thyroid hormones, utilizing the T1,T2, T3, and T4 hormones when necessary (all are produced by the thyroid gland, but only T4 is present in levothyroxine, the most commonly prescribed thyroid drug).
- Optimizing nutrition through eliminating reactive foods as well as addressing deficiencies and digestion.
- Addressing the stress response.
- Addressing the health of the detoxification system.
- Addressing the state of the gut.
- Identifying the person’s unique triggers such as chronic infections, toxins, or traumas.
- Tracking thyroid antibodies every three months to see if the interventions are making the condition less aggressive.
- Appreciation of the person’s experience and always utilizing the person’s symptoms as a guide for adjusting treatment.
There is a whole, growing field of medicine dedicated to this approach, known as functional medicine.
Functional medicine practitioners can have a variety of backgrounds. Some may be medical doctors, doctors of osteopathy, physician assistants, nurse practitioners, chiropractors, (compounding) pharmacists, naturopathic doctors, doctors of integrative medicine, acupuncturists, and nutritionists. This list may also extend to other professions as well.
While all of the above-listed practitioners can help you with addressing the root cause of the condition, in most states, only medical doctors, osteopathic doctors, physician assistants and nurse practitioners will be able to prescribe thyroid hormones (look for ones that are trained in functional or integrative medicine). Some may also be limited in the ability to prescribe other helpful medications like LDN, which has been found to be helpful for improving thyroid symptoms and antibodies.
The biggest challenge with seeing these types of practitioners is that they are often not going to be covered by insurance. This is because the recommendations, interventions, and tests recommended by these types of practitioners are often considered “experimental,” and insurance companies are going to be very resistant in reimbursing them for their services.
However, these are the professionals working with the latest research and coming back with unmatched outcomes and numerous success stories! (Sometimes, amazing success stories result after a few simple lifestyle changes that they recommend!)
Approaches to Medication
When the TSH is elevated to the point of needing medications, most conventional doctors will prescribe Synthroid (generic name: levothyroxine), a synthetic T4-containing thyroid medication, which was the number one prescribed medication in the U.S. in 2019, accounting for 114 million prescriptions!
While levothyroxine may work well for some people with Hashimoto’s and hypothyroidism, there are many people who continue to have symptoms of hypothyroidism on this medication. One reason is because levothyroxine (chemical name tetraiodothyronine or T4) is a prohormone that needs to be converted to the more physiologically active liothyronine (chemical name triiodothyronine or T3) in the body, to fully activate thyroid receptors.
“On paper”, this simple conversion should happen just fine, but it doesn’t always happen that way in the body. This is because the conversion requires a lot of different pieces to be in place, including having enough nutrients (that act as co-factors in the chemical process), having proper gut and liver function, and being on a low-stress setting (as chemical messengers related to stress may block or alter the conversion, resulting in the person not having enough T3 on board).
Some people who do not have enough T3 on board may benefit from T3-containing thyroid medications or natural desiccated thyroid medications (NDT), which are derived from the thyroid glands of animals and don’t require a person to convert T4 to T3 (a process that is impaired in many people with Hashimoto’s).
However, most conventional practitioners are not going to be comfortable with medications other than synthetic T4 medications… In fact, most clinical guidelines and pharmacology textbooks recommend only using synthetic T4 medications.
This is because, in prior years, the NDT medications were not manufactured precisely, and this resulted in inconsistent dosing between batches.
Additionally, T3 medications were misused and given to people without thyroid disease in high doses, to induce hyperthyroidism and try to achieve weight loss — a very dangerous scenario!
Today, the manufacturing process of NDT medications has been revamped, and now the medications are safe and effective when used correctly for people who are supposed to receive them (i.e. people with hypothyroidism) — unless, of course, there’s a recall! More on that in a minute.
If you’re seeing a conventional doctor and taking a synthetic thyroid medication, you can cry, plead and beg for NDT or a T3-containing medication, but most of them are not going to give you a medication they are not experienced in prescribing. And this is actually a good thing — you don’t want to be someone’s very first patient on a medication they don’t know how to use. Instead, you want to work with a practitioner that is well versed in using the various thyroid medications.
Another reason why a person may not feel well while taking levothyroxine could be due to issues related to absorption. For those needing to take multiple medications or those that have issues with malabsorption such as low stomach acid, H. pylori, acid reflux or SIBO, taking a medication like Tirosint may aid with proper absorption.
If you are struggling with thyroid symptoms despite being on thyroid medications, it may be helpful to see a doctor that is trained and familiar with the use of a variety of thyroid medication options, including T4-only medications (Synthroid, Levoxyl, Tirosint, levothyroxine, Euthyrox), T3 medications (Cytomel, liothyronine), Natural Desiccated Thyroid (NDT) medications (Armour*, Nature-Throid, WP Thyroid), and compounded thyroid medications (hypoallergenic blends of T4 and T3 in compounded, physiological ratios). This type of a practitioner will be able to help you find the type of thyroid medication that will work most effectively for you.
As such, I urge you to seek an expert that is knowledgeable in thyroid pharmacology. 🙂 (You’ll find resources to help you find such a practitioner in your area, further on in this article!)
Note: I wanted to give you a heads up that there has been a recent recall on all current lots of Nature-Throid and WP Thyroid (manufactured by RLC Labs, Inc), due to certain lots being found to be sub-potent. This means that the affected medications may have too little thyroid hormone in them. A person who is stable on their current dose of thyroid hormone, who then receives these affected lots, may become hypothyroid!
As such, there may be a current backorder of Nature-Throid and WP Thyroid medications in your area. Please contact RLC Labs and your local pharmacist directly if you have any questions or concerns.
*Note: While Armour Thyroid does not have any gluten-containing ingredients, it is not tested for gluten content, and cannot be certified as gluten-free. Armour does contain sodium starch glycolate, which can be derived from wheat or corn.
Questions to Ask Your Practitioner
So, how do you find the right doctor?
If you’re looking for a practitioner who can help you address Hashimoto’s, it’s important to know what you are looking for in a healthcare partner.
For example, if you are getting started on your thyroid journey and want to get some baseline labs and a thyroid ultrasound, you might want to start with an endocrinologist. If you’re looking for a more comprehensive approach that involves addressing your root causes, a functional or integrative practitioner is going to be your best bet. If you are looking for someone to help personalize your thyroid medications, compounding pharmacists are an excellent resource.
Here are some questions to ask your practitioner to see if they are a good fit for you:
- Do they prescribe hypoallergenic thyroid hormones like Tirosint, compounded thyroid medications, or natural desiccated thyroid medications (NDTs like Armour Thyroid, Nature-Throid, WP Thyroid, NP Thyroid and others)?
- Do they have experience with prescribing low-dose naltrexone (LDN)?
- Do they order a full thyroid panel that includes TSH, Free T4, Free T3, TPO/Tg antibodies, or just the TSH test?
- Do they have accounts with functional medicine lab companies like Ulta Labs, Direct Labs (GI-MAP test for gut infections), My Med Labs (food sensitivity testing), or ZRT Laboratory (Adrenal Stress Profile) so they can help you dig for hidden root causes?
- Can they order food sensitivity tests?
- Optional: Do they offer telemedicine (virtual appointment via video conferencing) options?
I encourage you to write out a list of these and other questions you have for your healthcare provider, and look for a like-minded practitioner who can offer you the level of care that you need on your individual journey.
Finding Dr. Right in Your Area
To help you locate a practitioner in your area, I have compiled a database of patient-recommended clinicians and practitioners. However, you will still need to be your own advocate in asking the right questions to find someone who will be a good fit for you. Customers looking for a new practitioner on our list should contact the practitioner to verify their knowledge and background before their appointment. Unfortunately, I’m unable to evaluate each of them individually at this point, but I hope this list provides a starting place for you.
You can also check my list of compounding pharmacies to find a pharmacist who will compound your thyroid medications for you.
I also recommend searching the Institute of Functional Medicine’s practitioner database, where you can search world-wide for healthcare advocates who are experienced in functional medicine. ZRT Laboratory offers a practitioner database as well.
Booking Virtual Appointments
While 2020 has been a crazy year, these days, there is something that may help even if you live in a place with very few experienced practitioners. Something to consider is telemedicine, which allows you to work with a functional doctor remotely, via Skype, Zoom, Google Meet, or other video conferencing applications. With telemedicine, you can work with a practitioner who is a good fit for you, but may not be located in your area.
More and more, medicine is using these remote options, and many doctors are embracing technology to expand their services. In the current climate that we are living in, this might be particularly beneficial! When looking for Dr. Right, be sure to ask if they offer virtual appointments.
Remember, you are your best health advocate!
Will Insurance Cover My Practitioner?
If you are working with a practitioner who accepts insurance, keep in mind that they may not be able to spend as much time with you as necessary due to reimbursement guidelines, and they may not be able to order functional medicine labs.
While these labs can be extremely important in getting to the root cause, they are outside the standard of care and considered experimental, so most endocrinologists, primary care doctors, and internal medicine doctors will not run those tests.
Many insurance companies refuse to reimburse doctors who use “non-approved labs” or order what they deem as too many tests for a patient. Unfortunately, the insurance companies have too much control over the practice of medicine.
Oftentimes, you will need to find a practitioner outside of insurance to get the care, attention, and testing you deserve. In some cases, you may be able to submit the claims to your insurance company for reimbursement. However, some insurance companies may not reimburse for these labs, so be prepared to pay out of pocket if needed.
I think of these tests as a health investment. Many of us will go out and spend money on a purse or a pair of shoes that makes us feel better in the short term, but spending money out of pocket for a lab test could dramatically improve our health in the long term.
In the event that you cannot find a doctor who will be able to prescribe medications and order the functional medicine labs, you may want to work with your medical doctor on monitoring your medications while you work with a functional medicine practitioner (who may not have prescriptive authority) to order the tests for you.
If you cannot find a practitioner to order the tests for you or if you have a high deductible, you can also order the same tests on your own through direct-to-consumer lab companies. (I’ve set up a few tests that you can order through them at a discounted price! Find them here, in the “Labs” section.)
The Takeaway
I believe that everyone needs to find a practitioner who will let them be a part of their healthcare team. You want someone who can guide you and also listen to you and your concerns. You want someone who is open to thinking outside the box and who understands that you may not fit in with the standard of care.
It’s also important that you don’t expect your doctor to change for you. Instead, find a doctor that fits your situation and understands your needs. There is a time and a place for an endocrinologist, a functional medicine practitioner, and a compounding pharmacist. It is up to you to ask the right questions and find the healthcare partner who will help you achieve your healthcare goals.
For more information on being your own healthcare advocate and finding your root cause, I encourage you to pick up a copy of my books Hashimoto’s: The Root Cause and Hashimoto’s Protocol. I wrote these books after struggling to find the help I needed from my doctors, learning to dig for my own root causes, and discovering the world of functional medicine. My goal is to empower you with the knowledge you need to get better and give you the tools and strategies you need to take back your health, as well as reduce your dependency on the medical system!
There are many strategies (that you’ll find in my books) that you can implement on your own, such as eliminating inflammatory foods (and inflammatory people, too, as stress is a huge trigger!), addressing your nutrient deficiencies, and taking helpful supplements.
But for other interventions, like getting on the right medication, testing for infections, or doing an advanced detoxification protocol, it is helpful to have a specially trained practitioner on your side.
One day, I hope that every single practitioner will be well versed in diagnosing and reversing Hashimoto’s! In the meantime, over the past few years, I’ve been collecting names and contact information for practitioners that can help from other thyroid patients.
If you’re looking for practitioners who believe in the root cause approach to treating thyroid issues, check out my list of patient-recommended practitioners!
I hope that this information helps you take charge of your own health!
P.S. You can download a free Thyroid Diet Guide, 10 thyroid-friendly recipes, and the Nutrient Depletions and Digestion chapter for free by signing up for my newsletter. You will also receive occasional updates about new research, resources, giveaways and helpful information.
For future updates, make sure to follow us on Facebook and Instagram too!
References
- Lewis S. The Top 50 Drugs Prescribed in the United States. Healthgrades website. https://www.healthgrades.com/right-care/patient-advocate/the-top-50-drugs-prescribed-in-the-united-states. Published September 5, 2019. Accessed August 13, 2020.
Note: Originally published in September 2015, this article has been revised and updated for accuracy and thoroughness.


 Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Anne- Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
Sheila- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Sheila, Did you ever find an amazing doctor? I live in the same area and am on the hunt! Thanks so much!
Christine- When it comes to weight gain these are a couple of things to think about.
1) What was your recent TSH, Free T3 and Free T4? Sometimes when those numbers are on the outskirts of normal, your metabolic rate may still be impaired making it more difficult for you to burn calories. Most people report feeling well with a TSH between 0.5-2.
2) What type of medication are you on? Some report more weight loss with T4/T3 combinations (Armour, Nature-Throid, compounded medications) versus T4 medications (Synthroid, Levoxyl, Tirosint) alone. T4 is a precursor to T3, but some individuals do not convert T4 to T3 properly, and the T3 component is the metabolically active one.
3) What type of diet are you eating? Some report more weight loss with T4/T3 combination vs T4 alone. Some do not convert T4 properly.The Standard American Diet (S.A.D.) full of sugar and simple carbohydrates is perfectly designed to cause us to gain weight year after year. Even yogurts that are marketed as “healthy” contain the equivalent of 16 teaspoons of sugar. Divorcing the S.A.D. is often a step that many of us must take to not just lose weight, but to also feel better. Some diets that have been helpful include the Body Ecology Diet, the Paleo Diet, the Virgin Diet, Autoimmune Paleo Diet, GAPS diet, SCD diet, Weston A. Price Diet, or the Mediterranean Diet. You may need to modify these diets to your own individuality.
BEST DIET FOR HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/best-diet-for-hashimotos-hypothyroidism
HOW TO LOSE WEIGHT WITH HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/how-to-lose-weight-with-hashimotos
I have hyperthyroidism and the Dr. Has put me on synthroid 20mg to 50mg . I have gained a lot of wait since my accident . I have also been on a lot of medicines to for pain , because I have RSD,CPS, depression,arthritis in my back , now having problems with my knees bursa, sprained mcl, I was hospitalised both legs swelled up and were very red. I can’t exercise or barely walk for that matter , the DR.s tried cortisone shots did not work. I take neurontin, Zoloft, Wellbutrin XL,BUSPAR,SEROQUEL,LEVOTHROXINE,METHDONE,TRAMADOL,EYEDROPS,NASALSPRAY. I’ve been on meds. Since 2004 of June 22nd. Day of accident at work to right foot 2,000 lbs dropped on foot by fork lift and rsd is in right foot, there was fracture, swelling, discolouration,very pain ful , could walk on it, sensitive to touch but a delayed reaction to touch like 1/2 hour to even hour I’d be in pain where I was touched! So I’ve been on all of this for13 years . Some of meds. We’re a lot stronger in beginning hydrocodone,methdone,lidocaine patches,fentanal patches,symbalta,nuerontin,altrum,etc. So many! I want to go off all this try canibis oil? Not sure ? I have not asked about it yet? I quit smoking so I don’t want to smoke it just oil drops for body not mind ? What do you think?
Jennifer – Thank you for following this page. My heart goes out to you! <3 Please, understand that due to liability issues, I am unable to answer specific medical questions, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Sue- You are so very welcome! I look forward to hearing your progress on this page!! I hope you also check out my book! Here’s the link in case you’re interested. 🙂
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Arie- Thank you so much for your support! I know it’s a lot to ask, but if you haven’t already, would you mind leaving a review on Amazon? 🙂
http://www.amazon.com/Hashimotos-Thyroiditis-Lifestyle-Interventions-Treating/dp/0615825796/ref=cm_cr_pr_product_top?ie=UTF8
Kathy- I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Hi my is Mrs.christie Jensen
I have thyroid issues
I can’t get help with this
I want to be able get pregnant
But can’t can you please help me with this please
Christie- Here is an article you may find interesting! 🙂
PREGNANCY
https://thyroidpharmacist.com/articles/hashimotos-and-pregnancy
Thanks so much for all the information you’ve given over the years. Do you have any doctor recommendations in the Toronto region of Ontario, Canada?
Vinnie – You are very welcome. I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Hi
Im a health care professional and was just dx with Hashimotos. Please email me top notch specialist in orange county, 92782 area. Thank you
Nazila – thank you for following this page.
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
I always have high TSA number during annual wellness blood draw….6, 4, 8 this year. However I have no symptoms as I’m in good physical shape, lots of energy, etc. Primary Dr says go on levothyroxine. I’ve read articles that say over 50% of population has a thyroid condition and wasn’t thrilled what I read about taking synthetic drug for life. I don’t want to ignore high readings but have no symptoms. What to do?
Mike – thank you for following this page. Please, understand that due to liability issues, I am unable to answer specific medical questions.
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Thank you Dr. Wentz for all your good information that you share! I have bought both your books and am learning a great deal. I have been diagnosed with Hashimoto’s over a year ago. I’m on thyroid meds and don’t like it. I’m trying to learn all I can to beat this and hopefully will with all your helpful information. Thank you so much!
Amy – Thank you so much for your kind words and the support. <3 I’m looking forward to hearing your progress on this page. Make sure to take the book slow, take notes, highlight, and establish a baseline when making changes.
Hi,
My 6 year old daughter is diagnosed with hashimoto desease. Please give me advise on what to do?
Abraham – thank you for following this page.
Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year
I was diagnosed with hashimotos last month. By my pcd.
He also said i had leaky gut syndrome.
He put me on a plant based compound thyroid pill .my TSH level was 900
I started research myself and found the AIP DIET.
My gut feels 100% better. But im still struggling with chronic fatigue. Any suggestions?
Angela – thank you for following this page.
Fatigue was the most debilitating symptom I experienced with Hashimoto’s. It actually started 8 years before I was finally diagnosed in 2009 after I got Mono (Epstein-Barr Virus) in college. I needed to sleep for 12 hours each night to be able to function, and by “function” I mean after hitting the snooze button on my alarm clock for two hours (ask my poor husband), I would drag myself out of bed and then had to drink 4-6 cups of caffeine everyday to keep myself awake. I often had Red Bull and Pepsi for breakfast, and was the epitome of “wired but tired”. I hope my articles help you get started 🙂
OVERCOMING THYROID FATIGUE
https://thyroidpharmacist.com/articles/top-10-tips-for-overcoming-hashimotos-fatigue
THIAMINE AND THYROID FATIGUE
https://thyroidpharmacist.com/articles/thiamine-and-thyroid-fatigue
Hi Dr. Wentz. I am wondering if you know of any functional doctors in the Athens, Greece area? I am finding it supremely hard to find anyone other than regular endocrinologists. Thank you.
Stea7 – thank you for following this page. Here are a couple links that you might find helpful.
http://www.thyroidpharmacistconsulting.com/europe1.html
https://www.functionalmedicine.org/practitioner_search.aspx?id=117#results
Thank you Dr. Wentz for those links. In my area, there is only a nutritionist. So, in your opinion, would it be best for me to see a regular endocrinologist for the medicine and then the nutritionist for further testing. Can they order the types of tests that need to be done i.e. for h.pylori, adrenals, etc? Thank you again for all of your efforts.
Chris – I have a 12 week online program called Hashimoto’s Self-Management Program that covers all of the strategies that I go through with my one-on-one clients, in a self-paced format, so that participants have access to all of the things I’ve learned about Hashimoto’s without having to schedule costly consults with me or another practitioner. In addition, any person that goes through the program will get access to a Quick search Q&A Database of 1000+ questions asked by past program participants, Root Cause Assessment based on 100’s of my clients’ root causes and triggers, 2-week Meal Plans, recipes, and shopping lists to get you started on the following diets: Paleo, Autoimmune Paleo, SIBO, Candida. Also, Discounts on lab tests, high-quality supplements, and consultations and much more to support you in your journey! There are a few requirements that you should pay attention to, such as my book is a required read. Hashimoto’s Self-Management Program http://hackinghashimotos.com/ I also have a team of consultants who I’ve personally trained on the protocols outlined in my books and program. Generally, the team will give priority for consultations to those who have read the book and completed the program. You can find out more about my team and consulting services here. https://www.thyroidpharmacistconsulting.com/pages/meet-the-thyroid-pharmacist-team
Thank you so much for recommending functional medicine to me a few months ago for my daughters Hashimotos! She is now seeing Dr. Curtis in Georgia. Dr. Curtis has conducted tests to help identify deficiencies and sensitivities in my daughters system that she believes are contributing to her ongoing health issues. She has already helped my daughte improve her stomach issues (traditional GI doctor said she had an ulcer and placed her on 3 medicines but her stomach issues just kept getting worse). Now Dr. Curtis has placed my daughter on WP Thyroid (a T4/T3 blend), as well as LDN and some other supplements. We are Praying that these changes help to improve her overall health and prevent her thyroid from being completely destroyed.
Dr. Curtis says the goal is to get my daughters Hashimotos into remission (something traditional doctors say is impossible!)
I cannot thank you enough for your books, (which started me on this journey to help my daughter), and your advice regarding functional medicine!!
Carol – Thank you so much for your support. I’m looking forward to hearing your daughter’s progress on this page. Make sure to take the book slow, take notes, highlight, and establish a baseline when making changes. I know it’s a lot to ask, but if you haven’t already, would you mind leaving a review on Amazon? 🙂
https://www.amazon.com/Hashimotos-Protocol-Reversing-Thyroid-Symptoms/dp/006257129X/ref=sr_1_1?ie=UTF8&qid=1491842521&sr=8-1&keywords=hashimotos+protocol
Hi Carol! I realize that this post is over a year old, but I live in GA and have been searching for a doctor that will perscribe LDN. Unfortunately I can not find the doctor you are talking about. Apparently there many Dr. Curtis’ in GA. Well if you see this post, or if anyone has any Information that’ll help me please let me know! Thanks so much!
Stephanie – thank you for reaching out. Here is a link to my patient recommended database. I hope you find it helpful.
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Hello.
All this helpful information is such a relief – Thank you!
I was recently diagnosed with Hoshimoto but I have all the symptoms of Graves Disease. My thyroid is in a hyper state and I’m miserable. Yet, the only treatment my primary physician has prescribed is a beta blocker for my heart palpitations. She says that I just have to wait for my thyroid to burn out and then I can begin treatment for hypothyroidism.
Is my condition playing out this way very common?
Thanks for any advice you can lend.
Denise – thank you for following this page. Graves and Hashimoto’s are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto’s, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people)-Hashimoto’s results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually, people with Graves have hyperthyroidism, and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own, and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
HASHIMOTO’S AND GRAVES’ REMISSION AFTER HELICOBACTER PYLORI ERADICATION
https://thyroidpharmacist.com/articles/hashimotos-and-graves-remission-after-helicobacter-pylori-eradication/
Exactly how did you get well? With or without drugs for life? I found a functional medicine practitioner but after the testing, there was no help. I guess some are not so great with treatment. I did get to spend much out of pocket cash & the list of supplements increased but all it showed me is what they say about those kinds of Doctors. They do nothing but charge for supplements after diagnosis of Hashimoto’s or hypothyroidism but nothing improves. Maybe it is time to go to a “real” Doctors.
Paula – thank you for following this page. I cannot make that decision for you but, I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. That is why I highly recommend a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms. Here are a couple links to some resources that you might find helpful.
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
How do I find out what Doctors in my area are knowledgable about Thyroid Pharmacology as you suggested? Is there a website or a list I can refer to? This is the problem I am having with getting help for my disease. I don’t know who I am supposed to see who can help me with my specific problems. I have been diagnosed with Hashimotos, Hypothyroidism, PCOS, GAD and Asthma. I have been put on Levothyroxine, given the labs and that has basically been all the help I have received. No suggestions from any of my Doctors (and I have been through MANY in the last 10 yrs or so) on what I can do to stop the pain I endure daily, the brain fog, the fatigue, etc. I believe it’s my gut health that needs to be addressed first, but no Doctor has touched the subject. I don’t feel I absorb nutrients as I should. Maybe high levels of mucus in my body, preventing absorption. I have tons of theories of what is wrong, but no professional in my area to help navigate me. I am beyond frustrated.
Kat – thank you for following this page. I understand your frustration! <3 I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
Here are some resources you might find helpful.
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
i’ve been diagnosed with hashi since early 20’s, i’m now 46. my first dr. (endocrin) told me always take synthroid, never generic. years later life got complicated and i stopped focusing on my issue and let life it slip by not getting blood work, and taking synthroid here and there,etc not consistent. i’m an RN so i should know better but we are sometimes worse at taking care of ourselves. anyhow, the past year has been awful and suffering from basically what i describe as bipolar. sleep for days, brain fog, depression cant get out of bed and days of not sleeping, and almost in manic state. i’v gone recently down the natural route to a nurse practitioner office and she started me on nature throid. my thyroid peroxidase is >900 ( worse than she’s ever seen ) tsh was 90 and is now 38, free t3 is 2.6. the past year has been tough but i still have not been able to take the med like i should…daily with no food etc. the past 2 months i’ve made an extra effort to take the med faithful and still my labs out of wack but slight improvement. she wants to add cytomel and LDN (im on suboxone so i need to talk to the doc who gives me that in order to go on LDN). my question is..at what point do i say, nature throid not working for me, let me go back to synthroid and perhaps see an MD and not a nurse practitioner. i’v also received testosterone pellets and taking iron bis and D3 10000 with K 2supps from her but never faithfult with the supps.
Nicole – thank you so much for sharing your journey. I understand how difficult this can be. <3 There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication which you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
HOW THE DOSE OF YOUR THYROID MEDICATION CAN UNCOVER YOUR ROOT CAUSE
https://thyroidpharmacist.com/articles/the-dose-of-your-thyroid-medication-can-uncover-your-root-cause/
HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications/
Thank to your book, I started to look for the root cause of my Hashimoto’s. I found a functional Dr in my area, adjusted my diet (gluten-free), started taking supplements, fish oil, iron, D, etc. My main concern was hair loss, after 8-9 months, my hair is not any better, in fact it is worse, I don’t have much of it left and it is so disheartening to watch if fall during washing or brushing. Because of your article on hair loss, dr put me on a “natural T3” GTA 90. After 5-6 weeks of taking it, my levels are all out of wack – TSH went from 3 to 2 to 0.045!!! T4 and T3 went up some. So I went to an endocrinologist, who said exactly what you are saying…, get off all supplements and only take levothyroxin. He may introduce a T3 medication later, but I need to free my system form GTA. So………I am confused, annoyed and lost as to what to do next! Who to trust (endo or functional dr), and how to STOP my hair from falling! Please help!!!!
Natalie – thank you for reaching out. I am so sorry to hear you are struggling with! I understand how frustrating it can be! My heart goes out to you! <3 Sometimes, when your TSH is on the outskirts of the normal range, you can continue to lose hair, and your hair may lack luster and shine. If your hair tangles easily, this is a sign that you may not be getting enough thyroid hormone. Talk to your doctor. You should see a change within 4-6 weeks.
Consider the type of thyroid medication you are taking. T3, the more active thyroid hormone, is your “beautiful hair” hormone that helps you grow your hair and prevents it from falling out. Synthroid, Levoxyl, and Tirosint only contain T4, the less active hormone. T4 should be converted to T3 in the body…except this doesn’t always happen. Sometimes an addition of Cytomel**may be cross-contaminated with gluten*** (a T3 medication) or a switch to a medication that contains a combination of T3/T4 such as Armour, Nature-Throid or compounded T4/T3 may result in a return of your hair’s luster and shine.
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
Here is a research article which might help further:
TOP 10 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/
I was diagnosed with Hashimoto’s by an Endo in KC but then again in my town I am seen as I have Hypothyroidism, the thing is that I live in rural Kansas and I am not sure where to start looking for a doctor that really knows what Hashimoto’s is or how to treat it, I am not currently taking medication because doctors are not on the same page on my diagnosis. I feel like the environment here makes it worse for me there is a lot of feed yard’s and I believe that the contamination of cow fecal matter in the air is a contaminant that may create toxins in my body but I am not expert that is just my thought. I would appreciate some feedback on where to start.
Karina – thank you for reaching out and sharing your journey! I understand hard this can be. <3 The most common triggers in Hashimoto's are: nutrient deficiencies, food sensitivities, intestinal permeability (leaky gut), stress, an impaired ability to get rid of toxins and in some cases, infections. Optimizing your health starts with food. Figuring out which foods nourish you, and which ones cause you harm is the single most important thing you can learn in your health journey.
I've found that recognizing and eliminating reactive foods can be a life-changer for most people with Hashimoto's.
Reactive foods trigger an inflammatory response in the GI tract, leading to malabsorption of nutrients (gluten sensitivity in particular has been implicated in causing a Selenium deficiency, a well known risk factor for Hashimoto's), and can also produce intestinal permeability whenever they are eaten.
Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods that they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people will actually be able to get their Hashimoto's into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are some articles which I wrote:
BEST DIET FOR HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/best-diet-for-hashimotos-hypothyroidism
TAILORING YOUR THYROID DIET
https://thyroidpharmacist.com/articles/tailoring-your-thyroid-diet-to-your-needs
DAIRY AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/got-hashimotos-you-may-want-to-reconsider-dairy
I have just ben successfully treated for Hashimoto’s encephalopathy. Diagnosed with Hashi’s 22 years.ago, spent over a decade on T4 only and kept getting worse. Finally switched to alternative practitioner who put me on NDT seven years ago (first Armour, later switched to WP, 3 grains daily). I have been told by neurologist that NDT most likely caused HE and that, in order to avoid a relapse, I need to go back on
T4 only (an additional problem was my TSH which is fully suppressed on NDT despite in-range FTs).
Would you agree with neurologist? It took almost two years before I was diagnosed with HE; I was first misdiagnosed with epilepsy and suffered through hell on three different AEDs so I want to minimize the risk of a relapse if at all possible…
Cathy – thank you for reaching out and sharing your journey. Please, understand that it would not be legal or appropriate for me to give any type of medical advice, but I highly recommend that you work with a functional medicine clinician. It’s an entire medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms. Here are some links which might help:
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
MY RECENT CHALLENGES AND FINDING DR. RIGHT
https://thyroidpharmacist.com/articles/my-challenges-and-finding-dr-right/
hello,
I am suffering from sleep problem and major acidity issue i am on sleeping pills now i have hypo thyroid with positive anti tpo i went to many doctors but no use i have 9 months old baby, i have got thyroid past 6 months ago please suggest
Heena – thank you for reaching out. I am so sorry you are struggling with acid reflux. Low stomach acid is very common in Hashimoto’s. Signs and symptoms that would leave me to believe that a person with Hashimoto’s had low stomach acid include: acid reflux symptom (this condition that is conventionally treated with acid suppressants can actually be caused by low stomach acid), low B12, ferritin, or iron levels, fatigue despite thyroid medications and constipation/diarrhea. Here is an article that might be helpful as well.
https://thyroidpharmacist.com/articles/using-enzymes-to-overcome-hashimotos/
Hi, I suspect having a candida infection. Despite following a clean (elimination) diet, de stressed routine, probiotics, i still feel lethargic and my skin has breakouts. I feel I am suffering from fungal acne, more so because last when I had a visible skin infection my doctor prescribed an antifungal medication, I had noticed a 85-90% reduction in the remaining symptoms as well. When I visited my endocrinologist and my gynaecologist for a suspected vaginal yeast infection my doctors refused to give me tests to check Candida. I live in India and I am clueless about what tests are done here to check candida. Can a candida infection be checked through blood samples? Also can you please suggest antifungal medicines that would be easily available in India.
Pooja – thank you for reaching out and sharing your journey. I am sorry to hear you are struggling with this. Yeast is an opportunistic organism that acts up when your overall health is impaired or when your immune system is compromised. Most people with Hashimoto’s will have a high degree of yeast overgrowth, especially of the Candida genus. Treating this overgrowth can be very helpful in restoring health. A note about Candida: Candida can be a primary or a secondary root cause. While conventional medicine underdiagnoses issues related to yeast overgrowth, natural medicine practitioners seem to overdiagnose yeast and may say Candida is a root cause for all ailments. I recommend a Candida protocol for most people with Hashimoto’s. I talk more about this in my book Hashimoto’s Protocol I hope you check it out.
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hello,
I’m 23 years old and have been diagnosed with hashimotos a year ago. I have a whole list of symptoms affecting my everyday life while being on Armour thyroid. I just purchased your books and I’m working toward finding the root cause and curing myself. I had mono when I was 17. Is getting tested for that infection still relevant for me even though it has been years since I was sick with it?
Thank you!
Madeline – thank you so much for reaching out and sharing your journey. <3 The Epstein Barr virus creates a latent infection in the body, where it lies dormant until the right time when it reactivates and awakens. The reactivated virus has the potential to induce the production of thyroid antibodies and has been implicated in many debilitating autoimmune symptoms. Testing for viral reactivation may be done through your doctor. You need to be sure to ask for the Epstein Barr Virus Early Antigen test, as this is a test that will let us know if the virus is actively replicating. Without going into too much detail, the first of the crucial defining moments in my disease development may have started during my undergraduate studies at the University of Illinois. Due to the communal living setting of dormitories (and less than stellar hygiene habits of most college students), I had recurrent strep throat infections and even contracted mononucleosis, a viral infection caused by the Epstein-Barr Virus (EBV), which is implicated in triggering many autoimmune conditions. I received multiple courses of antibiotics as well as flu shots (which may be associated with EBV infections) and started birth control for menstrual cramps.Animal fats, broths, soups, and stews support the body’s ability to suppress the viruses. Monolaurin or lauric acid, one of the components of coconut oil, has been found to be active against the Epstein-Barr virus. Replication of any viruses including Epstein Barr is inhibited by glycyrrhizic acid, an active component of licorice root. Quercetin, Co-Enzyme Q10, N-Acetylcysteine, and glutathione were also reported to be helpful in chronic fatigue syndrome because of their anti-viral properties. It is my belief that this combination had a profound impact on my gut flora, and thus my immune system. Here is an article which you might find interesting:
EPSTEIN-BARR VIRUS AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/epstein-barr-virus-and-hashimotos
I would love to find a doctor in my area that doesn’t require hundreds and hundreds of dollars to see. That does all required tests,doses to symptoms and optimal levels. I’m in the east of Toronto area, but would travel to Toronto to find what I need. Even an endocrinologist,who listens,will do T4 or equivalent and T3 or equivalent if needed,near area. Any recommendation would be great too,I’m on a hunt.
Sandra – thank you so much for reaching out! <3 I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It's a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
COMPOUNDING PHARMACIES
http://www.thyroidpharmacistconsulting.com/recommended-compounding-pharmacies.html
I live in Upland California is there a good thyroid doctor here or close by
Cathleen – thank you for reaching out. I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It’s a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
COMPOUNDING PHARMACIES
https://thyroidpharmacist.com/database-recommended-compounding-pharmacies/
Hello, my Mother has Hashimotos and is looking to get gashtric bypass. Could this cause anything bad or do anything bad to her?
Daphne – thank you so much for following this page. <3 I am not able to advise your mom on this procedure. I recommend that she discuss this with her personal doctor. I highly recommend that she work with a functional medicine clinician to be a part of her own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms. Here are some resources I hope you and your mom find helpful.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
http://www.thyroidpharmacistconsulting.com/recommended-compounding-pharmacies.html
I wish that you would add to your physician’s list a group of GI doctors that are familiar with Hashimoto’s
Robyn – thank you so much for sharing! Our database is a list of doctors recommended by patients. I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms. Here are some resources you might find helpful:
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Hi Isabella
Do you know any great Hasimoto’s advisers / experts in London or the UK?
My girlfriend has seen GPs and endocrinologists, but not to her liking for the reasons you’ve talked about here.
Any pointers would be appreciated!
thanks
Owen
Owen – thank you for reaching out! I understand how hard it can be to find the right practitioner. <3 I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It's a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
COMPOUNDING PHARMACIES
https://thyroidpharmacist.com/database-recommended-compounding-pharmacies/
Hi there 24yrs ago I was diagnosed with fibromyalgia and then 5 years ago I was diagnosed with Hashimotos. I’m having trouble with my thyroid being enlarged and had an ultrasound done finding out that my thyroid is enlarged and I have a 5mm nodule on one side and a 4 mm nodule on the other side. I went to see the endocrinologist that first diagnosed me only to be told to ” suck it up and just take ibuprofen”. Needless to say I wasn’t impressed. So my faith in the medical profession has dwindle. So my goal for now on is to heal myself. I’ll still take my thyroxine while I’m on this journey.
Samantha – thank you so much for reaching out and sharing your journey. <3 I understand how frustrating this is! Nodules and goiters are often the result of toxicity and/or the autoimmune process. So, doing interventions to reduce the autoimmune attack on the thyroid, and toxicity, can be helpful to reduce them. Here is an article you may find helpful.
THYROID NODULES
https://thyroidpharmacist.com/articles/hashimotos-and-thyroid-nodules/
Oftentimes Hashimoto’s patients will have additional autoimmune conditions. Most autoimmune conditions have common root causes, and a lot of times the things that are recommended for one autoimmune condition will help with others. Conditions that I have found to respond really well to the Hashimoto’s protocols have been rheumatoid arthritis, lupus, Celiac disease, irritable bowel syndrome, eczema, asthma, Graves’, premature ovarian failure, psoriasis, Alopecia Areata, and Sjogrens. I have also seen the protocols help with Fibromyalgia, chronic fatigue syndrome, PCOS, as well as Type 2 diabetes, Crohn’s, and Ulcerative colitis. We need to rebalance the immune system. Sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. Here are links to my book so you can check them out!
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
My father aged 84 years – suddenly behaved abnormally in Nov 2015 – physician diagnosed that he had septicaemia – but after that we found his irrelevant taking frequently – we met physiatrist & neurophysician – they diagnosed that my father has dementia & delirium – for last four years he is being treated on that line but day by day his mental health is down – now I came to know by one neurophysician that my father has Hashimoto decease. Now is it possible to cure him after four years?
Shailesh – thank you for reaching out and sharing your father’s journey. My heart goes out to both of you. <3 Thyroid tissue can regenerate, but the rate at which it does is not always predictable. Thus, some are able to stop the autoimmune attack on their thyroid and regain normal thyroid function. Others can reduce the dose of medications, and others will need to stay on the medications indefinitely. Reversing Hashimoto's means different things to different people. For some, it means a reduction in symptoms, and for others, it means a reduction in your antibodies. I had both. Here a few articles that might be helpful for you:
IS IT POSSIBLE TO RECOVER THYROID FUNCTION IN HASHIMOTO'S
https://thyroidpharmacist.com/articles/is-it-possible-to-recover-thyroid-function-in-hashimotos
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
No, Doctor I Don’t need Antidepressants
https://thyroidpharmacist.com/articles/doctor-dont-need-antidepressants/
Help.. I have been on levo for the last 9 years for hypothyroidism. I recently went in for my routine labs- I requested they check antibodies- I have struggled to lose weight, get frequent cold sores, tired a lot, constipation, amongst a host of other issues. I called about a week after my labs were drawn to see the results. I was told everything looks normal. A week after I checked my patient portal and actually viewed my labs for myself. My TSH was 2.940, and my TPO was 1300. My dose of levo was just lowered to 125mcg from 150mcg- they didn’t post the lab results from which they based this decision. They are now referring me to an endocrinologist. I’m not sure if that’s where I should go, or if functional medicine is where I need to be. I would appreciate any recommendation you have to offer.
DeAnna – thank you for reaching out. <3 I'm so sorry to hear you are struggling with all of this. I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms. I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It's a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
COMPOUNDING PHARMACIES
https://thyroidpharmacist.com/database-recommended-compounding-pharmacies/
Hi there,
Been on a thyroid journey for the last 13 years. My life is 100% better than it was when I was 17 however, despite numerous doctors I’ve seen for my thyroid, no one ever looks deep into the root cause. I’d like to be off thyroid medication or at least at a lower dose. I’ve seen almost all the decent doctors in my area. Is there someone else or could recommend that would be worth traveling to see?
Amanda – thank you for reaching out. <3 Thyroid tissue can regenerate, but the rate at which it does is not always predictable. Thus, some are able to stop the autoimmune attack on their thyroid and regain normal thyroid function. Others can reduce the dose of medications, and others will need to stay on the medications indefinitely. Reversing Hashimoto's means different things to different people. For some, it means a reduction in symptoms, and for others, it means a reduction in your antibodies.
I understand how hard it is to find the right practitioiner. I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It's a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
Here a few articles that might be helpful for you:
IS IT POSSIBLE TO RECOVER THYROID FUNCTION IN HASHIMOTO'S
https://thyroidpharmacist.com/articles/is-it-possible-to-recover-thyroid-function-in-hashimotos
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Wow, I really appreciate your reply. I recently read your book and I’m now starting on the liver protocol. After reading your book, I finally felt a little glimmer of hope. Thank you for your knowledge and sharing your experience!
Amanda – you are very welcome! Please feel free to email my team at info@thyroidpharmacist.com if you have any questions about the protocols! <3
The issue that I have had with a lot of functional medicine professionals is that they can’t prescribe thyroid medication so that puts the patient in a tough spot. Now, I need to go find someone that can prescribe the medication and try to convince them that they need to prescribe a certain dose of thyroid medication. This part is so frustrating.
Chris, thank you so much for sharing. I understand how frustrating this is. It does depend on the type of practitoiner you are working with and sometimes even the state regulations as well. I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It’s a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
COMPOUNDING PHARMACIES
https://thyroidpharmacist.com/database-recommended-compounding-pharmacies/
Wow, I never realized how extensive Hashimoto’s was. I went to an urgent care doctor when experiencing some symptoms, but it looks like most of these can only be treated with a specialist. Is that correct?
Eve – thank you for reaching out. <3 I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms. I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It's a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
COMPOUNDING PHARMACIES
https://thyroidpharmacist.com/database-recommended-compounding-pharmacies/
Hi Izabella,
Since women menstrual problems are rarely discussed as part of thyroid issues, I wanted to check in with you. I have had a recent diagnosis of Hashimoto’s with hypothyroidism TSH=7.7, T4=0.63, T3=2.6, TPO=1100, TG=1300. I heard Royal maca from Whole World botanicals has helped people get free of hypothyroidism, so tried 1/3 tsp for few days. Unfortunately, it messed up my cycles I had 2 bleeding cycles in 1 month and after the day one of second bleed, it’s been 11 days since but I have had no period. Until these last 2 cycles, I have had regular cycles like clockwork. I have stopped maca immediately and would like to know how long will it take for my menstrual cycles to get back to normal. Will thyroid medication alone help or do I need extra medications to bring back my periods? Please advise.
Hi Fran, I am so sorry to hear that your periods are irregular at the moment. ❤️ I recommend discussing this with your doctor as well as about possibly ordering a Dutch Test. The Dutch Test can give you a full picture of all your hormones and this can give you and your doctor a better idea of what might be going on. Here is a link to the testing so you can check it out: https://dutchtest.com/patients/
Here is an article you might find helpful as well:
ESTROGEN DOMINANCE AS A HASHIMOTO’S TRIGGER
https://thyroidpharmacist.com/articles/estrogen-dominance-as-a-hashimotos-trigger/
Hello Dr. Wentz
My question is I had blood work done and my thyroid levels were a little over 5. My doctor wanted to up my thyroid medication but I told him I feel good and not having any symptoms. So he tested me again after 3 months and my levels were just over 3. But he increased my medicine. After a week taking the higher dose I got symptoms of to much hormone. So I went back to my old dose I feel better but now I have bad acid reflux. Just wondering if it will go away are did I cause more harm to my thyroid. I am taking NP thyroid 60mg and my doctor up it to 75mg. But I went back to the 60mg. I only took the 75mg for a week but day 2 of taking the 75mg I started getting acid reflux and 4 weeks later I still have it. Just wondering if it will eventually go away from taking to much thyroid medication. Thank you, Jamie
Jamie – thank you for reaching out.❤️ It’s hard to say, without a comprehensive health assessment. I recommend that you discuss this with your personal doctor. That said, Acid Reflux is a very common symptom that occurs in people with Hashimoto’s. Studies have shown that most people with Hashimoto’s either have very low stomach acid or produce no stomach acid at all. The person who does not have enough stomach acid will have the same symptoms as a person with an overabundance of stomach acid. There aren’t too many tell-tale signs of low stomach acid, other than perhaps feeling full and tired after meals as well as experiencing acid reflux-like symptoms. Other symptoms may include: low B12, low ferritin or iron levels, fatigue despite thyroid medications, and constipation/diarrhea. Here is an article you might find helpful as well:
HASHIMOTOS AND LOW STOMACH ACID
https://thyroidpharmacist.com/articles/hashimotos-and-low-stomach-acid
My partner has suffering from hashimotos for three years now and in the last year has also been diagnosed with ibs,indometriosus and depression, all which need treatment and all treatments clash which is hard to find a way to treat them all at the same time and has been a massive struggle for her which is effecting her mentally more and more every day and she feels like there isn’t a way out of this so I’m asking can you please please please help us.
If you could please email me I would be so grateful !
Mark – thank you so much for reaching out for your partner. I’m so sorry she is struggling. Unfortunately, at present time I am not accepting new clients. I do offer a 12 week online program called Hashimoto’s Self-Management Program, that covers all of the strategies that I go through with my one-on-one clients, in a self-paced format, so that participants have access to all of the things I’ve learned about Hashimoto’s without having to schedule costly consults with me or another practitioner. Here is the link to the program if you are interested in checking it out:
Hashimoto’s Self-Management Program
https://thyroidpharmacist.com/enroll-in-hashimotos-program/
Please feel free to email my team at info@thyroidpharmacist.com if you have any questions regarding the protocols as well!
If you would like to be notified of any future consulting opportunities and educational events, you can sign up for my waiting list: https://thyroidpharmacist.com/dr-izabella-wentzs-waiting-list/
Please can you recommend a functional practioner in kzn south africa to assist with hoshimoto
Libby – thank you for following. Here are a couple of resources that I hope are helpful:
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Hi Dr,Izabella
This is Samara from Australia , I really need a good doctor /Practitioner to walk me through from Hashimoto’s Dilemma ,I took few notes from your book , articles about what’s the blood test /screening we need to know to understand our Root cause for our Autoimmune diseases /ongoing Hypothyroidism’s symptoms .
But to be honest with you , I need an experience practitioner to be with me step by step and inform me from where to start and what to change .
I actually started changing my diet by elimination of sensetive food , de -stressing
I starts feeling improvement , but I need more , I need to work with experience practitioner who has a good knowledge of your protocols .
so , can I ask you if you are able to help me remotely ?
Hi Samara, I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and preventing serious chronic disease rather than treating individual disease symptoms. Check out this article:
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/