The gut–thyroid connection has been near and dear to me for a long time.
Long before I was diagnosed with Hashimoto’s, I was diagnosed with irritable bowel syndrome (IBS). At the time, it felt like an isolated issue. In hindsight, it was the biggest clue to the root cause of my Hashimoto’s – and the many symptoms that followed.
At the time, I didn’t really know about the root cause approach to healing, so I just adjusted my life to my symptoms. I never left home without diarrhea medicine and an extra pair of pants.
A few years later, I was diagnosed with Hashimoto’s.
In order for autoimmune disease to manifest, we need three things to be present: a genetic predisposition, a trigger, and intestinal permeability – also known as “leaky gut.”
Many people with leaky gut don’t realize they have it, as it can often be asymptomatic. But for others, digestive symptoms like diarrhea, constipation, bloating, and cramping (often labeled as IBS) are the body’s early warning signs that the gut barrier is compromised.
In my experience, I have seen that symptoms like those seen in IBS often appear 5-15 years before an autoimmune diagnosis.
This timeline is eerily accurate to my own, and I’ve heard thousands of similar stories from my clients and readers.
When I dug deeper into my health, I came to realize that the key to reversing Hashimoto’s was in solving my digestive issues, and this is actually a big part of my approach to Hashimoto’s.
This is because untreated digestive issues leave a person with lingering intestinal permeability – a precursor to autoimmunity. Some people talk about eliminating foods or drinking bone broth to heal the gut, but this approach often falls short.
Even if you’ve been told that your digestive symptoms are “just IBS” and you can’t really do anything about it, I want you to know that your symptoms may be caused by a medically identifiable, treatable, and often testable condition, such as celiac disease, small intestinal bacterial overgrowth (SIBO), or a protozoal infection, just to name a few. When these root causes are addressed, we see a real shift in symptoms and long-lasting healing.
In the first part of this article, I explored the extensive connection between the gut and the thyroid, and how shared root causes can trigger both IBS and Hashimoto’s. In this follow-up article, I share more about these root causes and how to start addressing them, plus a general, easy-to-follow protocol for IBS.
In this article, you will discover:
- What is considered IBS
- The gut-thyroid connection
- Why the conventional approach to IBS falls short
- The root cause approach to IBS
- A general IBS protocol you can start following
What is IBS vs. Healthy Digestion?
Many of us live with digestive symptoms for so long that they start to feel normal. Bloating after meals, alternating constipation and diarrhea, cramping that comes and goes, and fatigue you can’t quite explain. But I can assure you that this is not normal!
In general, healthy digestion means you can eat most foods without pain or bloating, and you have regular, predictable bowel movements that pass easily – typically anywhere from one to three times per day (or at least several times per week), without straining, urgency, or discomfort. Stool should be soft, formed, and easy to pass.
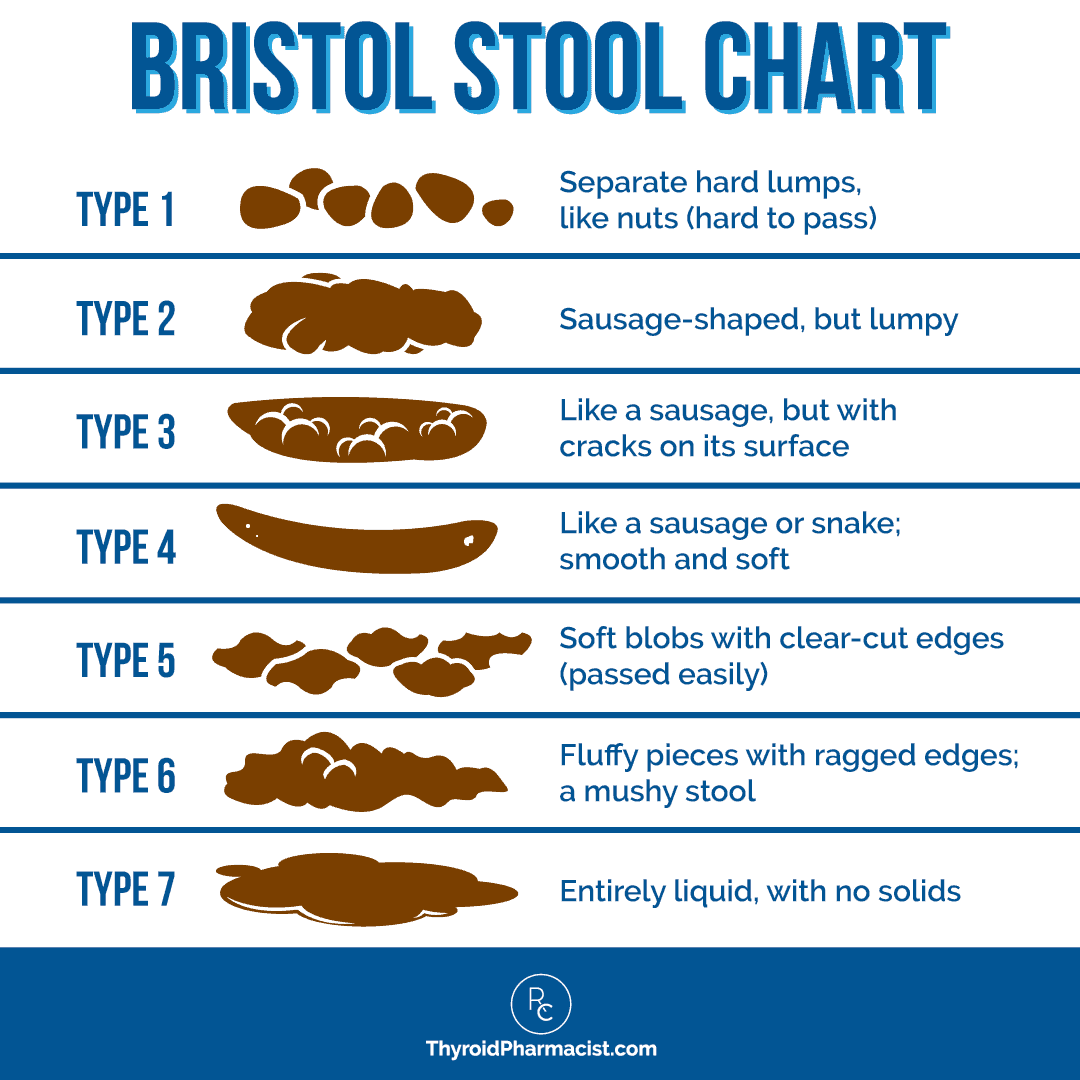
When that’s not happening, many people receive a diagnosis of IBS. IBS is considered a “functional” digestive disorder, meaning symptoms are present, but standard testing doesn’t reveal a clear structural problem. It’s typically diagnosed based on recurrent abdominal pain along with changes in stool frequency or appearance, often after other conditions have been ruled out.
Symptoms can include abdominal pain, cramping, bloating, diarrhea, constipation (or both), mucus in the stool, and a sense of incomplete elimination. [1] Some people experience flares and remission, while others live with ongoing daily symptoms.
IBS is categorized into four distinct diagnostic types: constipation-predominant (IBS-C), diarrhea-predominant (IBS-D), mixed (IBS-M), or unclassified (IBS-U), depending on bowel patterns.
The challenge is that IBS is largely a symptom-based diagnosis. Once the label is applied, many people are told their condition is something they simply have to “manage,” rather than investigate more deeply.
For more on symptoms, testing, other conditions that may be confused with IBS, and risk factors for IBS, refer to the first part of this article.
I personally believe that people struggling with IBS symptoms deserve a thorough investigation, which is what inspired my latest book, IBS: Finding and Treating the Root Cause of Irritable Bowel Syndrome. It released on March 17th and is currently available for order.
The Thyroid and IBS Connection
Thyroid dysfunction and IBS often go hand in hand. I frequently see digestive symptoms appear years before a thyroid diagnosis, and this is what happened to me personally.
It’s my educated guess that IBS-D often develops first, and over time, ongoing gut dysfunction can impair the absorption of nutrients essential for thyroid hormone production and conversion. As thyroid function declines, metabolism and digestion slow, eventually leading to constipation.
This progression makes sense when you understand the role of thyroid hormones. They regulate virtually every metabolic process in the body, including gut motility, enzyme production, and bile flow. [2]
When thyroid hormone levels are low, digestion slows. Reduced stomach acid, digestive enzymes, and bile can impair proper breakdown and absorption of food. Over time, this can contribute to dysbiosis, food sensitivities, and intestinal permeability, further fueling immune activation.
Interestingly, thyroid disorders and IBS have many overlapping features and root causes:
- Disrupted Motility: Transit time (the rate at which food moves through the digestive system) is also regulated by thyroid hormones and will slow down when thyroid hormones are low, which can contribute to constipation (which is the most common GI symptom in hypothyroidism and a top complaint of my clients with Hashimoto’s).
- Imbalance of Gut Bacteria: Slowed motility can then lead to imbalances in the microbiome, also known as dysbiosis. Research has found that hypothyroidism is associated with changes in gut microbial composition, and a comparable pattern of reduced beneficial bacteria alongside an overgrowth of pathogenic species is commonly observed in IBS. [3]
- Intestinal Permeability: Leaky gut is a hallmark feature in autoimmune diseases such as Hashimoto’s. [4] Though not everyone with IBS will have it, studies have found that people with IBS are more likely to have increased intestinal permeability. [5]
- Infections: Chronic infections caused by certain bacteria, protozoa/parasites, and fungi/yeast are common in those with Hashimoto’s (some studies indicate SIBO may be present in as many as 50 percent of people with hypothyroidism), and they can lead to diarrhea. [6] For some people with IBS, infections can be a trigger for their symptoms.
- Stress: Another common thread between Hashimoto’s and IBS is stress! Periods of stress often precede the onset of autoimmune conditions – in fact, in my survey of over 2,000 readers with Hashimoto’s, 69 percent reported a lot of stress in their lives before they began to feel unwell. [7] Adverse childhood experiences (ACEs) are associated with an increased risk of both IBS and autoimmune disease, and research has found that people with IBS are more likely to have experienced trauma of any kind than people without IBS. [8]
Symptoms of hypothyroidism and IBS resemble each other so closely that many people with thyroid dysfunction are diagnosed with IBS prior to getting their thyroid adequately tested. An interesting report from Nepal found that 18.5 percent of people who have IBS actually have thyroid dysfunction, most of them subclinical hypothyroidism (the early stages). [9]
The Conventional Approach to IBS
Much like with Hashimoto’s, the conventional medicine approach to IBS focuses primarily on lessening and managing symptoms, rather than searching for a root cause.
Depending on the type of IBS someone has and the symptoms they are experiencing, they may be told to try an OTC or prescription medication intended to treat their symptoms. Some doctors may also recommend diet and lifestyle changes, and stress management strategies, but those are, of course, few and far between.
It’s no surprise that without tailoring treatments to a cause, symptom relief following conventional treatment for IBS is incredibly poor, with one study finding that less than 25 percent of people gained complete relief from any given symptom. [10] Current conventional management therapies for patients with IBS result in up to 50 percent of patients remaining significantly symptomatic as much as six years after diagnosis. [11]
The good news is, whether you’ve just been diagnosed with IBS or have been struggling with symptoms for years, finding and addressing your unique root cause(s) can help significantly!
The Root Cause Approach to IBS
In functional medicine, we focus on the underlying causes for individual IBS symptoms, and we recognize this may require peeling back multiple layers of root causes as well. In my clinical experience, about 80 percent of people with “IBS” will find a resolution to their symptoms by following the root cause approach.
Let’s look at some of the most common root causes for IBS symptoms. Please keep in mind that while these are the most common root causes and the ones I most frequently see in my clients, these aren’t the only potential root causes.
Dietary Triggers
My work with Hashimoto’s really opened my eyes to the impact of dietary triggers on overall health and disease development, as well as the profound effect these can have on digestive symptoms. Studies have found that 50 to 80 percent of IBS patients identify a particular food as a possible trigger for their IBS symptoms, and up to 25 percent of people with an IBS diagnosis may actually have celiac disease. [12]
There are a number of different diets that can help you uncover your personal dietary triggers of IBS symptoms, including the gluten-free diet, the dairy-free diet, the soy-free diet, the low FODMAP diet, the additive-free diet, grain-free diets (like Paleo or Autoimmune Paleo), the low-nickel diet, the low-histamine diet, the low-oxalate diet, and the low-salicylate diet.
Where to start: I suggest starting with a simple elimination diet that focuses on eliminating the most common reactive foods, including gluten, dairy, soy, corn, sugar, spicy foods, alcohol, and caffeine. I’ve found that over the course of three to four weeks, this diet helps 70 to 80 percent of people with their digestive symptoms. If this doesn’t fully resolve symptoms, there are more advanced protocols. Interestingly, raw fruits and vegetables such as lettuce and blueberries can be a trigger for some with IBS.
Testing: While the elimination diet can help you identify your personal triggers, some people find food sensitivity testing helpful. I recommend Alletess food sensitivity testing. There are two options to test for the most commonly eaten foods:
- The 96 Food Panel test checks for IgG (a branch of the immune system that mediates food sensitivities as well as Hashimoto’s) reactions to 96 common foods. You can order this test through my Rupa Health or MyMedLab.
- The 184 Food Panel test checks for IgG (a branch of the immune system that mediates food sensitivities as well as Hashimoto’s) reactions to 184 common foods. You can order this test through my Rupa Health or MyMedLab.
Digestive Enzyme Deficiencies
IBS-like symptoms can occur due to a person’s inability to digest various food components, including protein, fat, and starches. This can often be corrected by taking the right digestive enzyme in the correct dose. Some enzyme deficiencies can be uncovered by comprehensive testing, while others are best trialed if symptoms suggest a deficiency. Some people may benefit from broad-spectrum enzymes, while others may benefit from very targeted enzymes.
Where to start: To support digestion and your body’s own production of digestive enzymes, there are a few things you can try:
- Relax while you eat: Eating while we’re relaxed supports optimal digestion. Taking a few deep breaths or a moment to calm yourself if you are feeling emotional, hurried, angry, or upset before starting a meal can make a huge difference.
- Chew your food: Chewing kicks off the digestive process, and the more you chew, the more thoroughly your food will be broken down, lowering the risk of gas, bloating, constipation, indigestion, and other digestive issues.
- Drink hot lemon water: Drinking the juice of one lemon in a cup of hot water first thing in the morning can help boost the secretion of stomach acid. (Do not use if you have an ulcer or gastritis.)
In some cases, you may need more targeted support, including digestive enzymes. I cover the different types of digestive enzymes, which enzymes you might be deficient in, recommended products, and recommended dosages in my book, IBS: Finding and Treating the Root Cause of Irritable Bowel Syndrome.
Testing: While a comprehensive stool analysis like the GI-MAP may give you insight into certain enzyme deficiencies, your symptoms and digestive patterns can often point to which enzymes we may be deficient in, and a trial of supplemental enzymes can help determine whether you have a particular deficiency.
Bile Acid Malabsorption
Bile helps to break down fat in the small intestine. If it’s inadequately reabsorbed after doing its work, bile can make its way into the colon and trigger diarrhea. Treating bile acid malabsorption (BAM) may help clear up diarrhea in 30 percent of cases of IBS-D. [13] Normally, bile is reabsorbed after doing its job in digestion, but when this doesn’t happen, excess bile moves into the colon, causing watery diarrhea.
Where to start: While using bile acid sequestrants for BAM is the best-studied approach to relieve symptoms (which you would get from your doctor), there are a few lifestyle approaches that may help. Dietary fiber can bind to secondary bile acids and aid their elimination, while resistant starch found in foods like cooked-then-cooled rice, green bananas, and potatoes can support proper bile acid metabolism and rebalance the gut flora. Certain vegetables are also helpful for binding bile, including beets, okra, and asparagus. In those lacking pancreatic enzymes, supplementing with them can help with BAM. Rootcology Pancreatic Enzymes is a high-quality option.
Testing: Testing is available, though not always widely accessible, with fecal bile acid excretion and serum 7𝛼C4 tests being the most common. In many cases, doctors may recommend a therapeutic trial with bile sequestrant medications like cholestyramine or colesevelam to manage symptoms and confirm BAM.
Nutrient Depletions
Whether you have diarrhea or constipation, nutrient deficiencies can be a very important root cause of IBS symptoms and can be a stand-alone cause of IBS or a consequence of enzyme deficiencies, SIBO, and other causes.
Deficiencies in a few key nutrients related to gut health, such as glutamine, vitamin D, thiamine, carnitine, vitamin A, zinc, and others, may contribute to IBS symptoms.
Where to start: If you’re experiencing diarrhea, glutamine, zinc, and vitamin A can be helpful, and are often well-tolerated and generally safe to supplement without testing. For those with constipation, omega-3 fatty acids, thiamine, magnesium, and vitamin C may be helpful. Staying hydrated with electrolytes is also helpful for constipation.
Testing: While some nutrients are safe to supplement with, even in higher doses, there are some nutrients that can build up in the body and become toxic to us. I always suggest testing these nutrients before supplementing:
Refer to my articles on vitamin B12, iron/ferritin, and vitamin D for more information on optimal ranges and how to boost levels.
Deficiency of Beneficial Bacteria with Excess Pathogenic Bacteria
A 2020 meta-analysis found that people with IBS often have a microbiome pattern characterized by not enough “good” bacteria and too much “bad” bacteria and/or yeast in the microbiome, otherwise known as dysbiosis. [14] This is similar to findings in those with Hashimoto’s.
When the microbiome is out of balance, so is everything else! Restoring balance can not only significantly help resolve IBS-associated symptoms, but may also improve or prevent autoimmune issues, hormonal imbalances, and even help us reach a healthier weight.
Where to start: Generally, the treatment for dysbiosis is focused on increasing the number of beneficial bacteria through probiotic supplements. Lactobacillus-based probiotics are the most widely researched and commonly used, and can be very helpful in rebalancing gut dysbiosis, relieving IBS symptoms, and assisting with fiber digestion. [15] Rootcology ProB50 or Pure Encapsulations Probiotic 50B are high-quality options (available via Fullscript, if you don’t have a Fullscript account, you can sign up with my credentials here). Please note that if you have SIBO, Lactobacillus-based probiotics may make you feel worse. Consider using SIBO-safe probiotics, such as Saccharomyces boulardii.
Testing: Various comprehensive stool analysis tests, such as the GI-MAP or Gut Zoomer, can identify a lack of beneficial bacteria, an overgrowth of opportunistic bacteria, and potentially pathogenic bacteria. I’ve also become very interested in using some newer targeted microbiome tests that analyze the microbiome and provide personalized recommendations for foods, prebiotics, and probiotics. I cover them more extensively in my IBS book.
Intestinal Permeability
Studies have found that people with IBS are likely to have increased intestinal permeability, though not everyone with IBS will have it.[16] As we know, those with Hashimoto’s nearly always have some level of intestinal permeability.
Intestinal permeability, sometimes called “leaky gut,” can show up in many different ways, and in some cases, it doesn’t produce obvious symptoms at all. For many people, the first clues are digestive problems such as bloating, diarrhea, constipation, abdominal pain, and acid reflux/GERD. Others may notice they’ve developed new food sensitivities.
Many things can influence the permeability of the gut, including certain medications, digestive enzyme and nutrient deficiencies, various infections, yeast overgrowths, foods we are reactive to, stress, and environmental toxins.
Where to start: In integrative functional medicine, we use the 5R framework to heal and support intestinal permeability. This protocol is focused on removing reactive foods and infections, replacing digestive enzymes, reinoculating the gut flora with beneficial microbes, rebalancing the lifestyle, and using repairing protocols to help with healing and sealing the intestinal lining. You can learn more about this approach and a full protocol in my IBS book.
Testing: Intestinal permeability can be measured via testing. Zonulin is a protein that acts as a gatekeeper, helping to maintain the integrity of the gut barrier by modulating the tight junctions between cells in the gut lining. When zonulin levels increase, this signals the tight junctions to relax, allowing larger molecules and potentially harmful substances to pass through the intestinal barrier into the bloodstream. Zonulin levels can be measured as part of various comprehensive stool analysis tests on the market, such as the Gut Zoomer or GI Effects, or as an add-on to the GI-MAP. Genova Diagnostics offers an Intestinal Permeability Assessment that measures the ability of two sugar molecules to pass through the lining of your small intestine.
Intestinal Overgrowth of Bacteria or Yeast
Research has found that one-third of IBS patients tested positive for small intestinal bacterial overgrowth, or SIBO. An overgrowth of Candida in the small intestine has been found in about 25 percent of people with previously unexplained GI symptoms, like those associated with IBS.
SIBO is caused by abnormally high levels of bacteria in the small intestine (a place bacteria do not belong), and this has become increasingly recognized as a potential root cause for IBS. If fibrous foods, fermented foods, histamine-containing foods, prebiotics, cruciferous veggies, and/or the use of probiotics seem to cause a flare-up in your digestive symptoms, there’s a good chance you have an overgrowth of bacteria in your small intestine.
Candida, a yeast naturally found in the gut, typically stays in balance without causing issues. However, when the gut’s “good” bacteria are compromised, Candida can become opportunistic and overgrow, leading to symptoms such as food sensitivities, bloating, gas, diarrhea, and constipation.
Where to start: Specific diets can help alleviate symptoms of both SIBO and Candida, but diet alone rarely eradicates the overgrowths. Targeted protocols, either pharmaceutical, herbal, or a mix of both, will likely need to be implemented for long-term resolution. My IBS book contains treatment options and protocols for both, and you can also see my articles on SIBO and Candida for an overview.
Testing: SIBO can be tested with an at-home breath test kit such as Genova Diagnostics SIBO 3-Hour Kit.
For Candida, I’ve found the Organic Acids Test (OAT) to be the most effective at detecting Candida because it not only tests for Candida overgrowth in the colon (as stool tests do), but also detects Candida metabolites in the body.
Infections
Chronic infections are an overlooked source of leaky gut and IBS-like symptoms, yet identifying and treating them correctly can have a tremendous impact on how you feel. I’ve spoken at length about Blastocystis hominis being one of the most prevalent triggering infections in Hashimoto’s. It also happens to be a known trigger for IBS and chronic hives, so if you have all three, I am willing to bet some hard cash that you probably have this infection and that treating it will result in a remission of all three conditions. But there are many other infections that have been tied to IBS, including viral infections, bacterial infections, and parasitic infections, and testing is key to finding out which infection you might have.
Where to start: Treatment options will depend on the type of infection you have. I recommend working with an experienced practitioner, and you can also refer to IBS: Finding and Treating the Root Cause of Irritable Bowel Syndrome for treatment suggestions and protocols.
Testing: Testing will depend on what type of infection you suspect you have:
- Bacterial infections that cause foodborne illness can be triggers for ongoing IBS symptoms. I suggest seeing your practitioner and requesting a stool test for bacterial infections.
- Another very important and potential bacterial trigger of IBS and IBD is Borrelia burgdorferi, the bacteria that causes Lyme disease. Options for testing include: IGeneX Lyme ImmunoBlot IgG, Vibrant Wellness Tickborne Disease Panel, or IGeneX Tick Borne Disease Panel 7 (TBD7).
- For pylori and other potential gut infections, I suggest a comprehensive stool test such as the GI-MAP, Gut Zoomer, or the GI Effects 3-day + H. Pylori.
- For detecting parasites, the Gut Zoomer seems to be the most helpful, but you may also want to consider a specialized test such as the ParaWellness Research Comprehensive Parasite Test.
Alterations in Stress Hormones
Stress can disrupt gut function in many ways. It affects gut motility, increases gut sensitivity, alters secretions like stomach acid and bile, and raises intestinal permeability. Stress also reduces mucosal blood flow, weakens the gut’s ability to repair its lining, weakens the gut’s internal defenses, and negatively impacts gut bacteria. A 2008 study highlighted that stress reduces beneficial bacteria in the gut and allows pathogenic bacteria to proliferate. [17]
Over time, prolonged stress can deplete cortisol, leaving the body less able to manage inflammation and stress. Low cortisol is linked to increased gut permeability, inflammation, and worsened IBS symptoms, as well as mood disorders like anxiety and depression. [18]
Where to start: Many experts view mind-body practices such as yoga, meditation, and breathwork as a cornerstone of IBS management. Research shows these techniques can significantly reduce symptoms by activating the parasympathetic (rest-and-digest) nervous system. [19] For other stress management strategies, see my article for a brief overview, and my book Adrenal Transformation Protocol for a deeper understanding of how to navigate chronic stress.
Testing: I’ve found symptom self-assessments are excellent indicators of an impaired stress response and provide the information we need to start providing the body with the right kind of support. However, testing may help with determining other potential interventions more specific to your individualized hormone levels and patterns. Consider the Precision Analytical DUTCH Complete to assess adrenal function through urine testing, or the ZRT Laboratory Adrenal Stress Test Kit to measure four cortisol readings throughout the day, cortisol sum, and DHEA.
Thyroid Hormones and Autoimmunity
A dysregulation of thyroid hormones in itself can lead to digestive distress and is a very common finding in IBS. Hypothyroidism causes a slowing down in the digestive process, while hyperthyroidism (having an overactive thyroid gland) can lead to diarrhea. With Hashimoto’s, there is an autoimmune attack against the thyroid, resulting in fluctuating thyroid hormone levels. Some people may initially experience a surge in thyroid hormone levels during the early stages of the autoimmune attack, followed by low levels of thyroid hormone, resulting in fluctuating GI symptoms.
Where to start: As the Thyroid Pharmacist, I have plenty of resources for this. 😉 If your thyroid is in fact out of balance, thyroid medications can be a very helpful first step, while you work to dig for your root cause. You may find my books Hashimoto’s Protocol and Hashimoto’s: The Root Cause helpful.
Testing: A full thyroid panel would be the best place to start with testing. You can get one through your doctor or self-order one here. Read more about thyroid testing and how to interpret results here.
Inflammatory Bowel Disease
IBS and IBD share several of the same symptoms, and there are many instances when IBD is missed. According to some studies, as many as 10 percent of people with IBD may be misdiagnosed with IBS, and IBD patients are three times more likely to have a previous diagnosis of IBS. [20] While there are heavy-duty drugs for IBD, there are also lifestyle changes that are (in my humble opinion) much safer and often more effective.
Where to start: Due to my husband’s own experience with IBD, I have extensive personal experience in putting IBD into remission. I wrote about multiple strategies to induce remission of IBD in IBS: Finding and Treating the Root Cause of Irritable Bowel Syndrome, where there is an entire chapter dedicated to IBD with a full protocol.
Testing: Proper diagnosis of IBD typically requires consultation with a gastroenterologist, and may include testing such as a colonoscopy, X-rays, CT scans, and MRIs. Crohn’s disease is associated with anti-Saccharomyces cerevisiae antibodies (ASCAs), so testing for ASCAs through a blood test or a stool test can be useful in diagnosing Crohn’s disease. Fecal calprotectin is a protein that may indicate inflammation in the gut and can be measured on comprehensive stool tests, but keep in mind that this could also come from food reactions, celiac disease, cancer, NSAIDs, poor blood supply, or infections.
Toxins and Chemical Triggers
We are exposed to countless toxic substances on a daily basis through the foods we eat, the air we breathe, and the products we apply to our skin. These various toxins and chemicals, in addition to mold toxins, heavy metals (with nickel being the most widely studied), breast implants, and toxic estrogen metabolites, can all influence gut health.
All of these toxins can disrupt the gut microbiome, lead to inflammation, and aggravate IBS symptoms, making detoxification one of the essential strategies for managing IBS. [21]
Where to start: While narrowing down any specific toxins you may be exposed to can inform a more targeted treatment plan, a general liver support protocol is a great place to start for most people. See my article on liver support for gentle detoxification strategies. I outline more targeted support, depending on the toxin, in my IBS book.
Testing: Testing can help you determine more specifically which toxins you might have been exposed to. Here are some of the most helpful tests:
- For general screening, consider the TOXDetect Profile by Mosaic Diagnostics. This test assesses your exposure to common environmental chemicals. The Vibrant Wellness Toxin Zoomer test is another very comprehensive option, testing for toxic load from metals, mold toxins, chemicals, and PFAS.
- For mold, there are a few tests that can be helpful. The Organic Acids Test (OAT) checks for mold metabolites and oxalate metabolites that may indicate mold colonization in the body. Other tests, such as the Mosaic Diagnostics MycoTOX Profile or the Real-Time Laboratories MycoToxin Panel, can help reveal which types of mold mycotoxins are present in the body.
- For estrogen and other hormone levels, consider the DUTCH Complete Urine Test.
- For glyphosate (a common pesticide) specifically, consider the Mosaic Diagnostics Glyphosate
While it may take some time and experimentation to get to the root of your digestive issues, it is possible. I have seen this approach help so many people take back their health and transform their lives. I wholeheartedly believe it can do the same for you!

This is exactly what inspired my upcoming book, IBS: Finding and Treating the Root Cause of Irritable Bowel Syndrome. Inside, you’ll discover much deeper dives on all the potential root causes I’ve listed in this article, plus you’ll learn about how digestive symptoms often show up 5 to 15 years before an autoimmune diagnosis, how to utilize targeted nutrition strategies, how to restore microbial balance, and how to heal intestinal permeability.
General IBS Protocol
While figuring out your personal root causes and targeting treatment will be the most helpful approach to IBS, I also wanted to offer you a general IBS protocol that can help ease symptoms fast, so you have more energy to dig into the deeper root causes.
Diet
Many different dietary protocols can be helpful for IBS, but a good starting point would be to eliminate the most common reactive foods – gluten, dairy, and soy. Eliminate these foods completely for at least three weeks to see if there is an improvement in symptoms. If you’re feeling up to it, consider also eliminating corn, sugar, spicy foods, alcohol, and caffeine – other common triggers of IBS.
Support Digestion
Try these three things to support optimal digestion at each meal. They seem simple, but they have a big impact for many people!
- Slow down around meals and eat in a relaxed state. The body does not prioritize digestion when it’s in a stressed state. Try taking a few deep breaths before eating, and minimize distractions like watching TV or scrolling while eating.
- Chew your food. Again, this seems too simple, but many of us don’t actually chew our food that well! This leaves a lot of work for our digestive system. Chew your food thoroughly, until it is well broken down before swallowing (10 to 20 times depending on the food). Many people are surprised to find how much this can prevent bloating.
- Sip on lemon juice or apple cider vinegar in water before meals. Drinking the juice of one lemon in warm water in the morning can help stimulate our body’s own digestive juices. You can also have one teaspoon of apple cider vinegar in water before meals, and this will help support digestion as well. (Do not use if you have an ulcer or gastritis.)
Address Your Stress
Stress disrupts gut function in many ways, from affecting gut motility to reducing beneficial bacteria to affecting stomach acid and digestive enzyme production. It can also increase gut sensitivity and pain. Addressing your stress response will be incredibly helpful in shifting you into the parasympathetic rest and digest state. You can start with some simple strategies such as practicing yoga, meditation, or breathing exercises. I also suggest cultivating a support system, whether that be friends, family, or a good therapist.
These strategies are a good starting point for anyone with IBS or ongoing digestive issues, and there are many more advanced protocols based on your root causes, which I cover in depth in my upcoming book, IBS: Finding and Treating the Root Cause of Irritable Bowel Syndrome.
This book has been over a decade in the making, and it’s now available for order!

Inside, you’ll discover much deeper dives on all the potential root causes I’ve listed in this article, plus you’ll learn about how digestive symptoms often show up 5 to 15 years before an autoimmune diagnosis, how to utilize targeted nutrition strategies, how to restore microbial balance, and how to heal intestinal permeability.
Whether you’ve been struggling with Hashimoto’s for many years or you were just diagnosed (and even perhaps received an IBS label), I hope my comprehensive guide to figuring out the root causes of gut issues will help you heal!
Takeaway
There is a complex, bidirectional relationship between the thyroid and IBS, and in many cases, these conditions do not occur in isolation. They may share underlying root causes such as chronic inflammation, gut dysbiosis, nutrient deficiencies, infections, or stress.
If you’re feeling hopeless about ongoing digestive symptoms or frustrated that conventional treatments haven’t provided you with lasting relief, it may be time to dig deeper.
Identifying and addressing your unique root cause can help you achieve more meaningful and sustainable healing, rather than simply managing symptoms.
If this sounds like you, I highly suggest ordering IBS: Finding and Treating the Root Cause of Irritable Bowel Syndrome. Whether you’re newly diagnosed or have been struggling for years, this book will walk you through the exact steps to identify what’s driving your symptoms and how to address those root causes with confidence. You’ll learn how to work smarter, not harder, using the latest research and real-world strategies that actually make a difference.
Have you ever been diagnosed with IBS? Were digestive symptoms part of your Hashimoto’s experience? I’d love to hear your story in the comments!
P.S. You can download a free Thyroid Diet Guide, 10 thyroid-friendly recipes, and the Nutrient Depletions and Digestion chapter of my first book for free by signing up for my newsletter. You will also receive occasional updates about new research, resources, giveaways, and helpful information.
For future updates, make sure to follow me on Facebook, Instagram, TikTok, and Pinterest!
References
[1] Saha L. Irritable bowel syndrome: pathogenesis, diagnosis, treatment, and evidence-based medicine. World J Gastroenterol. 2014;20(22):6759-6773. doi:10.3748/wjg.v20.i22.6759; Palsson O, Whitehead W. IBS – beyond the Bowel: The Meaning of Co-Existing Medical Problems. UNC Center for Functional GI & Motility Disorders Accessed December 10, 2025. https://www.med.unc.edu/ibs/wp-content/uploads/sites/450/2017/10/IBS-Beyond-the-Bowel.pdf
[2] Daher R, Yazbeck T, Jaoude JB, Abboud B. Consequences of dysthyroidism on the digestive tract and viscera. World J Gastroenterol. 2009;15(23):2834-2838. doi:10.3748/wjg.15.2834
[3] Menees S, Chey W. The gut microbiome and irritable bowel syndrome. F1000Res. 2018;7:F1000 Faculty Rev-1029. Published 2018 Jul 9. doi:10.12688/f1000research.14592.1; Shan Y, Lee M, Chang EB. The Gut Microbiome and Inflammatory Bowel Diseases. Annu Rev Med. 2022;73:455-468. doi:10.1146/annurev-med-042320-021020; Fasano A. Leaky gut and autoimmune diseases. Clin Rev Allergy Immunol. 2012;42(1):71-78. doi:10.1007/s12016-011-8291-x
[4] Fasano A. Leaky gut and autoimmune diseases. Clin Rev Allergy Immunol. 2012;42(1):71-78. doi:10.1007/s12016-011-8291-x
[5] Hanning N, Edwinson AL, Ceuleers H, et al. Intestinal barrier dysfunction in irritable bowel syndrome: a systematic review. Therap Adv Gastroenterol. 2021;14:1756284821993586. Published 2021 Feb 24. doi:10.1177/1756284821993586
[6] Patil AD. Link between hypothyroidism and small intestinal bacterial overgrowth. Indian J Endocrinol Metab. 2014;18(3):307-309. doi:10.4103/2230-8210.131155
[7] Stojanovich L, Marisavljevich D. Stress as a trigger of autoimmune disease. Autoimmun Rev. 2008;7(3):209-213. doi:10.1016/j.autrev.2007.11.007
[8] Park SH, Videlock EJ, Shih W, Presson AP, Mayer EA, Chang L. Adverse childhood experiences are associated with irritable bowel syndrome and gastrointestinal symptom severity. Neurogastroenterol Motil. 2016;28(8):1252-1260. doi:10.1111/nmo.12826; Köhler-Forsberg O, Ge F, Aspelund T, et al. Adverse childhood experiences, mental distress, and autoimmune disease in adult women: findings from two large cohort studies. Psychol Med. 2025;55:e36. Published 2025 Feb 11. doi:10.1017/S0033291724003544
[9] Khadka M, Kafle B, Khadga PK, Sharma S. Prevalence of Thyroid Dysfunction in Irritable Bowel Syndrome. ResearchGate. January 2018. Accessed December 17, 2025. https://www.researchgate.net/publication/322946988_Prevalence_of_Thyroid_Dysfunction_in_Irritable_Bowel_Syndrome.
[10] Brown B. Does Irritable Bowel Syndrome Exist? Identifiable and Treatable Causes of Associated Symptoms Suggest It May Not. ResearchGate. July 2019. Accessed December 17, 2025. https://www.researchgate.net/publication/334545135_Does_Irritable_Bowel_Syndrome_Exist_Identifiable_and_Treatable_Causes_of_Associated_Symptoms_Suggest_It_May_Not.
[11] Poon D, Law GR, Major G, Andreyev HJN. A systematic review and meta-analysis on the prevalence of non-malignant, organic gastrointestinal disorders misdiagnosed as irritable bowel syndrome. Sci Rep. 2022;12(1):1949. Published 2022 Feb 4. doi:10.1038/s41598-022-05933-1
[12] Borghini R, Donato G, Alvaro D, Picarelli A. New insights in IBS-like disorders: Pandora’s box has been opened; a review. Gastroenterol Hepatol Bed Bench. 2017;10(2):79-89.; Mansueto P, D’Alcamo A, Seidita A, Carroccio A. Food allergy in irritable bowel syndrome: The case of non-celiac wheat sensitivity. World J Gastroenterol. 2015;21(23):7089-7109. doi:10.3748/wjg.v21.i23.7089; Domżał-Magrowska D, Kowalski MK, Szcześniak P, Bulska M, Orszulak-Michalak D, Małecka-Panas E. The prevalence of celiac disease in patients with irritable bowel syndrome and its subtypes. Prz Gastroenterol. 2016;11(4):276-281. doi:10.5114/pg.2016.57941
[13] Farrugia A, Arasaradnam R. Bile acid diarrhoea: pathophysiology, diagnosis and management. Frontline Gastroenterol. 2020;12(6):500-507. Published 2020 Sep 22. doi:10.1136/flgastro-2020-101436
[14] Wang L, Alammar N, Singh R, et al. Gut Microbial Dysbiosis in the Irritable Bowel Syndrome: A Systematic Review and Meta-Analysis of Case-Control Studies. J Acad Nutr Diet. 2020;120(4):565-586. doi:10.1016/j.jand.2019.05.015
[15] Ceccherini C, Daniotti S, Bearzi C, Re I. Evaluating the Efficacy of Probiotics in IBS Treatment Using a Systematic Review of Clinical Trials and Multi-Criteria Decision Analysis. Nutrients. 2022 Jun 28;14(13):2689. doi: 10.3390/nu14132689. PMID: 35807868; PMCID: PMC9268703.
[16] Camilleri M, Gorman H. Intestinal permeability and irritable bowel syndrome. Neurogastroenterol Motil. 2007;19(7):545-552. doi:10.1111/j.1365-2982.2007.00925.x
[17] Lutgendorff F, Akkermans LM, Söderholm JD. The role of microbiota and probiotics in stress-induced gastro-intestinal damage. Curr Mol Med. 2008;8(4):282-298. doi:10.2174/156652408784533779
[18] Madison AA, Bailey MT. Stressed to the Core: Inflammation and Intestinal Permeability Link Stress-Related Gut Microbiota Shifts to Mental Health Outcomes. Biol Psychiatry. 2024 Feb 15;95(4):339-347. doi: 10.1016/j.biopsych.2023.10.014. Epub 2023 Oct 29. PMID: 38353184; PMCID: PMC10867428.;Dziurkowska E, Wesolowski M. Cortisol as a Biomarker of Mental Disorder Severity. J Clin Med. 2021 Nov 8;10(21):5204. doi: 10.3390/jcm10215204. PMID: 34768724; PMCID: PMC8584322.
[19] Schumann D, Anheyer D, Lauche R, Dobos G, Langhorst J, Cramer H. Effect of Yoga in the Therapy of Irritable Bowel Syndrome: A Systematic Review. Clin Gastroenterol Hepatol. 2016 Dec;14(12):1720-1731. doi: 10.1016/j.cgh.2016.04.026. Epub 2016 Apr 22. PMID: 27112106.
[20] Card TR, Siffledeen J, Fleming KM. Are IBD patients more likely to have a prior diagnosis of irritable bowel syndrome? Report of a case-control study in the Generinflammationinflammationinfluence,al Practice Research Database. United European Gastroenterol J. 2014;2(6):505-512. doi:10.1177/2050640614554217
[21] Kish L, Hotte N, Kaplan GG, et al. Environmental particulate matter induces murine intestinal inflammatory responses and alters the gut microbiome. PLoS One. 2013;8(4):e62220. Published 2013 Apr 24. doi:10.1371/journal.pone.0062220; Choi JJ, Eum SY,influence Rampersaud E, Daunert S, Abreu MT, Toborek M. Exercise attenuates PCB-induced changes in the mouse gut microbiome. Environ Health Perspect. 2013;121(6):725-730. doi:10.1289/ehp.1306534


 Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Leave a Reply