Hashimoto’s is more than just hypothyroidism.
It is a complex autoimmune condition that affects multiple systems and processes within the body.
Hashimoto’s develops when an imbalanced immune system leads an attack on the thyroid gland, resulting in hypo- and hyperthyroid symptoms.
Over the course of seven years, I experienced thyroid-related symptoms such as cold intolerance (even when living in Southern California!), acid reflux, and extreme fatigue (I needed 12 hours of sleep to function like my usual self), without knowing what was going on within my body.
Every visit to the doctor was the same: they told me my thyroid levels were normal. It was only years later, when my TSH levels skyrocketed to 8 μIU/mL (back then, the normal levels were 0.4-4.0 μIU/mL), that I was finally referred to an endocrine specialist… and diagnosed with Hashimoto’s.
My experience was not unusual. In certain cases, it can take years before the destruction of the thyroid is reflected in lab results. This is because Hashimoto’s develops through a cascade of events (which we call the “autoimmune cascade”) that take a long time to develop and manifest.
The development of Hashimoto’s arises when root cause triggers such as genetic predispositions, lifestyle predispositions, and other factors interact with one another to promote an inflammatory state. They create the “perfect storm,” or more accurately, perfect circumstances, for autoimmunity to occur.
In this article, I’ll delve into these factors and discuss:
- The three-legged stool of autoimmunity
- The genetic and lifestyle triggers associated with Hashimoto’s
- The six most common root causes of Hashimoto’s
- How the thyroid gland is affected by the autoimmune cascade
- Healing Hashimoto’s
Understanding the Thyroid Gland and Thyroid Hormone Production
Before we delve into the development of Hashimoto’s, let’s discuss how the thyroid functions in the body.
The thyroid gland is a butterfly-shaped organ that is located on the anterior (front) side of the neck. It is connected to our brain through the hypothalamic-pituitary-thyroid (HPT) axis.
The thyroid gland has several functions, including:
- Regulating metabolism, growth, and development
- Modulating body temperature
- Regulating mood (along with the endocrine and nervous systems)
In a healthy individual, the pituitary gland (in the brain) releases thyroid stimulating hormone, or TSH, to signal the thyroid to produce adequate amounts of thyroid hormones.
Within the small cavities (follicles) of the thyroid, tyrosine (an amino acid that serves as the building block for thyroid hormone production) combines with iodide through a process called iodination, to create several thyroid hormones: T1, T2, T3, T4. (Of these four hormones, only T3 and T4 are biologically active, with T3 being the main biologically active form.)
Other organs also play a role in thyroid hormone production. For instance, the liver converts T4 to T3, and provides most of the T3 in the body.
When there are unusually high levels of T3 and T4, this essentially sends a message to the brain to reduce the production of TSH to help all thyroid hormones stay within their optimal ranges.
However, these processes are disrupted when the autoimmune cascade is triggered and the thyroid is attacked.
The Three-Legged Stool of Autoimmunity
Our bodies are smart and are constantly adapting to help us survive. When the body doesn’t feel safe, it tries to adapt, and this can trigger the development of autoimmune conditions such as Hashimoto’s, to survive. (You can read more about this in my article on the Izabella Wentz Safety Theory.)
So, what might cause the body to feel unsafe enough to launch an attack against its own thyroid? According to Dr. Fasano, a world-renowned gastroenterologist, in order for autoimmunity to be triggered, three factors must be present (this is referred to as the three-legged stool of autoimmunity): [1]
- A genetic predisposition
- Intestinal permeability/leaky gut
- A triggering event or root cause factor
Each of these three “legs” or factors plays its own role in triggering autoimmunity (explained throughout this article). When one of the “legs” is removed, the stool cannot stand and the autoimmune condition goes into remission.
A Genetic Predisposition
Specific genes can make an individual more predisposed or susceptible to developing Hashimoto’s.
The more well known and researched ones are: [2]
- HLA-DR3, associated with thyroid gland atrophy
- HLA-DR5, associated with an enlarged thyroid gland
These immune regulatory genes are closely associated with the autoimmune process of Hashimoto’s.
In addition, there are other thyroid-specific genes that play a role in the development of Hashimoto’s. (I wrote this article on genes linked to Hashimoto’s if you would like to learn more.)
Because there is such a strong genetic component in the development of Hashimoto’s, this autoimmune condition is often thought to be hereditary. But, genes alone are not enough to trigger it. If a condition was 100 percent genetic, there would be a concordance rate of 100 percent in identical twins. Because identical twins share the same genes, this means that if one twin had Hashimoto’s, there would be a 100 percent certainty that the other twin would also have Hashimoto’s. However, this is not the case.
The concordance rate for Hashimoto’s disease is 55 percent in identical twins (and 30-35 percent for Graves’, while thyroid antibodies have an 80 percent rate). [3] As identical twins not only share genes, but often environments, the scientist in me wonders if the concordance rates in twins that were separated at birth would be lower.
(Of course, my mama heart doesn’t ever want any twins to be separated at birth, but twin and separated twin studies are always so interesting! :-))
A genetic predisposition can make a person more susceptible to autoimmune conditions. But lifestyle factors (discussed below) can act on genetic predispositions to trigger the autoimmune cascade.
This is another reason why related individuals are both likely to develop thyroid conditions…
When living together, individuals often share similar diet and lifestyle habits (or are exposed to shared environmental triggers such as mold toxicity) — and if these factors are detrimental to thyroid health, both individuals are vulnerable to the autoimmune cascade.
Intestinal Permeability
The second factor that needs to be present, is intestinal permeability, or a leaky gut. Intestinal permeability occurs when “holes” develop in the intestinal barrier, often due to damage caused by:
- Adrenal fatigue
- Alcohol
- Capsaicin (in “spicy” peppers)
- Dental infections
- Dysbiosis
- Enzyme deficiencies
- Food sensitivities
- Gluten
- Gut infections
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Nutrient depletions
- Psychological stress
- Small intestinal bacterial overgrowth (SIBO)
- Sinus infections
- Strenuous exercise
- Stress
- Surgery or trauma
- Toxins
These holes in the intestinal lining allow for toxins and food particles to “leak” into the bloodstream, and the body labels these molecules as foreign invaders. The body may then launch an attack on these “foreign” molecules, and eventually, autoimmunity can develop.
Triggers of Autoimmunity
Of course, the last “leg” in the three-legged stool of autoimmunity involves a triggering event or root cause factor.
The graphic below depicts how specific triggers can lead to certain clinical manifestations, symptoms, and ultimately, autoimmunity. Let’s walk through the chain of events in this graphic to help you understand what’s really going on with Hashimoto’s.
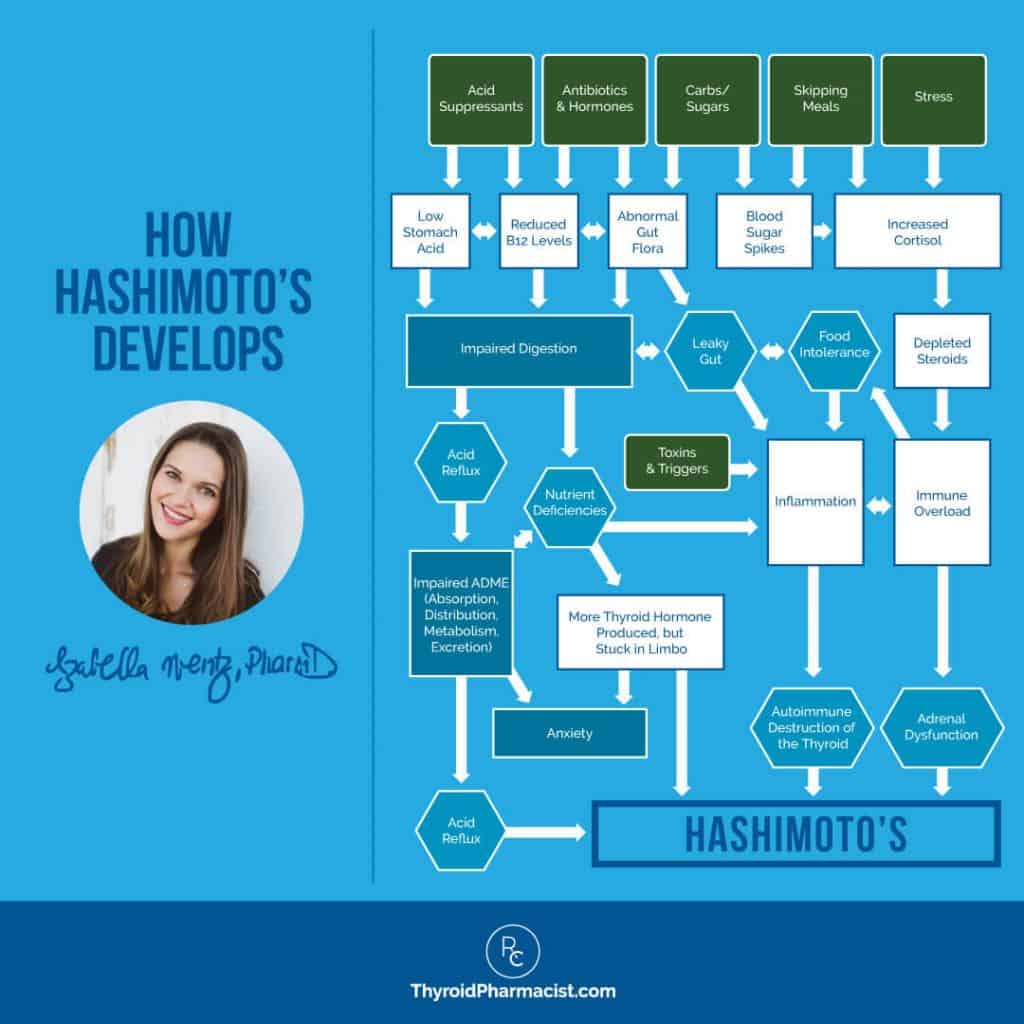
These triggers can create a “cascade” that both represents and results in clinical manifestations and symptoms. This is the autoimmune cascade.
Lifestyle Predispositions
In the graphic above, the green boxes represent some of the most common lifestyle factors that can predispose a person to develop Hashimoto’s. Let’s dive into each of them.
Acid Suppressants
Acid suppressants are usually taken when someone has symptoms of acid reflux (potentially due to pathogens or food sensitivities). Acid suppressants can reduce acidity in the small intestine and the stomach, both of which are naturally acidic environments (needed for these organs to function properly). Reducing acidity can lead to low stomach acid, as well as an overgrowth of pathogens in the stomach and small intestine.
Antibiotics/Hormones
Antibiotics are commonly known (and well researched) disruptors of gut flora. Many antibiotics act against a wide spectrum of flora and have the potential to wipe out both “bad” and “good” bacteria (protective flora).
Similarly, hormone-containing medications (such as steroids and oral contraceptives) can create imbalances in the gut flora.
Carbs/Sugars
Meals containing high levels of carbohydrates and/or sugars can lead to abnormal gut flora by encouraging the growth of certain pathogens such as Candida.
Skipping Meals
If high-carb meals are accompanied by irregular meal times, or if meals are often skipped, blood sugar levels may become imbalanced, resulting in blood sugar spikes and crashes. Skipping meals sends “starvation” signals to the body, which will also negatively impact blood sugar signals.
Stress
Stress plays a crucial role in the development of Hashimoto’s. In my survey of over 2000 individuals with Hashimoto’s, 70 percent said they experienced a lot of stress in their life before they started feeling unwell and experiencing thyroid symptoms.
Stress can stem from:
- Infections
- Changing jobs
- Changing homes
- The death of a loved one
- A stressful job
- Having a baby
A high-stress lifestyle or intense event can interact with other lifestyle factors and contribute to the cascade of autoimmunity.
Toxins and Triggers
Toxins and triggers are other lifestyle factors that may trigger the autoimmune cascade.
We can be exposed to toxins through poor air quality, conventional beauty products and procedures, low-quality produce and meats, and exposure to molds. Consistent exposure to toxins can lead to a liver backlog (a buildup of toxins that may be difficult for the liver to clear out), which can create inflammation and immune system imbalances.
Remember how I mentioned that genetic and lifestyle predispositions and triggers create the perfect storm that leads to autoimmunity? This is when that “perfect storm” starts to develop.
These lifestyle predispositions can create an environment that allows for certain root cause factors to develop, which begins the self-perpetuating cycle that is Hashimoto’s.
Clinical Manifestations
If an individual is exposed to or engages in the lifestyle predispositions mentioned above, clinical manifestations (highlighted in the white boxes in the above graphic) may start to unfold.
These clinical manifestations are often overlooked in conventional medicine, as the main treatment for Hashimoto’s is for the person to receive a thyroid hormone prescription. However, many of these manifestations are left when thyroid hormones are given, and can often result in a person feeling sick, even though they are taking medications. I have found that correcting these imbalances one by one, can lead to complete symptom resolution. 🙂
Low Stomach Acid
Low stomach acid can result from consuming acid suppressants, which can then lead to impaired digestion. This is when individuals start to experience gut and digestion-related symptoms such as fat malabsorption, bloating, constipation, and/or diarrhea.
Reduced B12 Levels
Reduced B12 levels can result from low stomach acid, or from the use of antibiotics and hormones. This is because both factors can compromise our body’s ability to extract and absorb nutrients — I’ll talk more about impaired digestion later on.
Reduced B12 levels will also contribute to impaired digestion, as this nutrient plays an important role in optimal gut health.
Abnormal Gut Flora
Abnormal gut flora pertains to an imbalance between the protective, “good” bacteria, and the pathogenic, “bad” bacteria in the gut.
When good bacteria are wiped out by antibiotics, hormones, and/or a high-carb diet, an opportunity is made for other pathogens (including yeasts) to overgrow and exert their harmful effects. They may, for instance, release toxins and create holes in the intestinal wall. Abnormal gut flora may eventually lead to impaired digestion.
Blood Sugar Spikes
Blood sugar spikes and imbalances from high-carb meals and/or irregular meal times, may result in a sudden drop in energy, feeling faint, and/or feeling dizzy. When blood sugar levels are constantly fluctuating, the body reads this as chronic stress, which then leads to increased cortisol levels.
Initial Increased Cortisol, Followed by Depleted Steroids
Chronic stress and blood sugar imbalances both lead the body to produce high levels of the stress hormone cortisol, which may result in us feeling “wired but tired,” and trigger adrenal fatigue.
The adrenal glands use steroids such as cholesterol (which is involved in the production of hormones such as progesterone, estrogen, testosterone, DHEA, and aldosterone) to make hormones. When cortisol levels are consistently and chronically elevated, the body can impair the production of other hormones in order to meet this demand for elevated cortisol. Eventually, the signaling pathway between the brain and the adrenals can become impaired, and the person will underproduce cortisol.
Inflammation
Inflammation within the body can result from abnormal or imbalanced gut flora, a leaky gut, exposure to toxins, an overloaded immune system, and stress. A pro-inflammatory state is created within the body through the stimulation of cytokines (pro-inflammatory molecules). This pro-inflammatory state can lead to the creation of antibodies, which may eventually launch an attack against the thyroid.
Immune Overload
Inflammation and immune overload go hand-in-hand. The Th1 branch of the immune system creates both the pro-inflammatory state mentioned previously, and cytokines (pro-inflammatory proteins). This results in an overloaded immune system and a heightened immune response. Along with launching an autoimmune attack on the thyroid, an overloaded immune system can overwhelm the adrenal glands, leading to eventual adrenal dysfunction.
More Thyroid Hormones are Produced, but the Body is Still “Stuck in Limbo”
As the body launches an attack on the thyroid gland, the gland will (initially) respond by creating more thyroid hormones to overcompensate for the attack, affecting hormone production.
However, the thyroid hormones will be released into the bloodstream, leading to an individual experiencing a variety of symptoms (including anxiety, as detailed below). The body will then be stuck in limbo (overcompensating by producing more thyroid hormones), yet will still not be able to achieve healthy thyroid function because of the imbalances created by the attack.
Further Manifestations
If the clinical manifestations mentioned above are left unaddressed, they may evolve into further issues (as noted as dark blue boxes in the above graphic).
Impaired Digestion
The overuse of antibiotics, low stomach acid, low B12 levels, and abnormal gut flora, can lead to impaired gut function, which then leads to impaired digestion. Impaired digestion results in the start or worsening of gastrointestinal symptoms such as bloating, constipation, and/or diarrhea.
Impaired Absorption, Distribution, Metabolism, and Excretion of Nutrients and Other Substances
Impaired digestion can lead to impaired ADME (absorption, distribution, metabolism, and excretion of nutrients), and acid reflux, as the digestive tract no longer becomes able to optimally carry out its functions.
This affects how nutrients from food are digested (food molecules start leaking into the bloodstream instead of being absorbed and utilized for physiological processes), and can lead to the development of nutrient deficiencies.
Nutrient deficiencies can lead to a host of other symptoms and can cause us to react to benign substances like foods, medications, personal care products, and supplements. This is because many nutrients are required for proper digestion, metabolism, and excretion of various substances.
Anxiety
Anxiety is a common symptom experienced by people with Hashimoto’s. Many doctors and mental health practitioners often prescribe antidepressants without exploring thyroid health as a potential root cause.
In many cases, anxiety is a result of the autoimmune cascade seen in Hashimoto’s. Anxiety has been linked to elevated thyroid antibody levels. [4] It can be caused by nutrient deficiencies and impaired ADME, which can both result in low selenium levels and higher thyroid antibody levels. Anxiety may also be caused by a thyroid that is “stuck in limbo” between hypo- and hyperthyroid symptoms due to intense thyroid hormone fluctuations.
Possible Symptoms Resulting from the Cascade of Autoimmunity
Leaky Gut
Not only does abnormal gut flora (which may result from high-carb meals, the use of antibiotics, etc.) add to impaired digestion, it also makes an individual more susceptible to intestinal permeability. The increased susceptibility of developing intestinal permeability or leaky gut is due to certain pathogens such as Candida having the ability to create holes in the intestinal wall. As mentioned earlier, intestinal permeability is a factor required for autoimmunity to occur.
Food Intolerance(s)
With leaky gut, food molecules can leak out of the gut and into the bloodstream, where they’re not supposed to be. This can lead to food intolerances. Gluten, dairy, egg, and soy intolerances are common in those with Hashimoto’s. However, each individual is different and some individuals may be sensitive to additional foods, particularly those that are frequently consumed. Food intolerances can create inflammation in the gut.
Acid Reflux
Acid reflux is a symptom that can arise from impaired digestion. (It can also be a symptom of food sensitivities and/or a sign of low stomach acid.) I experienced acid reflux for nearly three years… it started with a chronic cough, pain, and a burning sensation.
Nutrient Deficiencies
When one’s digestion is impaired, the body isn’t able to absorb and utilize all nutrients needed for optimal thyroid function and overall well-being. One common nutrient deficiency mentioned previously is B12 deficiency. Other nutrients commonly deficient in people with Hashimoto’s include:
As these nutrients are important for healthy thyroid hormone production and many of them act as anti-inflammatory molecules, being nutrient deficient can result in inflammation and contribute to the “stuck in limbo” phase. [5]
Adrenal Dysfunction
Adrenal dysfunction (also known as adrenal fatigue) can result from an overloaded immune system (as explained in the Immune Overload section above), as well as from imbalances in cortisol production and steroid levels. Individuals may experience symptoms such as fatigue (often manifesting as that all too familiar “tired but wired” feeling), poor quality sleep, as well as a poor ability to handle stress. This adrenal dysfunction can directly promote autoimmunity by further stimulating the production of pro-inflammatory molecules.
Autoimmune Destruction of the Thyroid
As the body continues the attack on the thyroid (via inflammation and an overloaded immune system), the thyroid gland is slowly destroyed (referred to as “atrophied”). Eventually, the thyroid gland will no longer be able to overcompensate for the attack (that is, it will lose the ability to maintain optimal thyroid hormone production) and will slowly lose its function.
Through this cascade, it becomes apparent how the seemingly random symptoms experienced by those with Hashimoto’s are actually not random at all. Quite the opposite — these symptoms are all interconnected. When these symptoms start to manifest themselves, and once the autoimmune destruction of the thyroid begins, the more classic hypo- and hyperthyroid symptoms experienced by those with Hashimoto’s, will begin to present themselves.
How Triggers Can Encourage an Autoimmune Attack on the Thyroid Gland
As I mentioned earlier, Hashimoto’s is more directly linked to immune system function rather than the thyroid gland itself. When a trigger or root cause factor, such as a toxin or infection, permeates through a leaky gut and attacks the thyroid cells, the thyroid will respond by sending out a stress signal.
This stress signal alerts the immune system, which then attacks the thyroid instead of saving it (as described above). The destruction of the thyroid hormones (along with the gland) affects the negative feedback loop to the brain, resulting in increased TSH. The thyroid gland will try to overcompensate and produce more thyroid hormones (T3 and T4) to keep the levels “normal” even as the gland and the hormones themselves are being destroyed. This is when the individual may start to experience (or already has been experiencing) symptoms of both hypo- and hyperthyroidism.
However, at some point, the thyroid will run out of resources to overcompensate for this destruction, which will lead to a deficiency in thyroid hormones, or hypothyroidism.
Additionally, due to the autoimmune attack and destruction of the thyroid, self-reactive antibodies such as thyroid peroxidase (TPOAb) and thyroglobulin antibodies (TgAb) become elevated and contribute to these symptoms.
Many people will finally be diagnosed with Hashimoto’s at this point, but their Hashimoto’s symptoms may be in more advanced stages, as it may have taken years before abnormal thyroid antibody and thyroid hormone levels appear in lab results.
You can learn more about the 5 stages of Hashimoto’s here.
Healing Hashimoto’s
Due to the complexity of this condition, most patients with Hashimoto’s will present with many of the following symptoms:
- Acid reflux
- Nutrient deficiencies
- Anemia
- Intestinal permeability
- Food sensitivities
- Hypoglycemia
These symptoms are in addition to “typical” hypothyroid symptoms like weight gain, cold intolerance, hair loss, fatigue, and constipation (remember, they’re all connected!).
The body becomes stuck in a chronic state of immune system overload, adrenal insufficiency, gut dysbiosis, impaired digestion, inflammation, and thyroid hormone release abnormalities.
This cycle is interconnected and reinforces itself through a positive feedback loop, meaning the cycle is self-sustaining and will continue causing more and more symptoms until an external factor (like a Root Cause Rebel such as yourself!) intervenes and breaks the cycle.
Treating a complex autoimmune condition such as Hashimoto’s requires a detailed and well-thought-out protocol. In my experience, simply adding thyroid medications to the mix does not often result in a full recovery. Additionally, supporting just the thyroid may weaken the adrenals and immune balance, which will, in turn, perpetuate the vicious cycle.
To successfully reverse Hashimoto’s, one has to understand how multiple factors create a vicious cycle that keeps people in an autoimmune state.
I recommend that everyone begin their journey to healing by getting the right diagnosis, adjusting their medication, and using food to heal.
I initially came up with this process map in 2012. Since that time, and after many years of working with clients, I have found that picking low-hanging fruit, chopping branches, and digging for the root cause is the most effective approach. 🙂
By picking the low hanging fruit, we focus on addressing the manifestations that are almost always present in Hashimoto’s and relatively easy to correct with simple, yet targeted changes.
These include:
- Elimination diets to remove the inflammatory foods (most often gluten, dairy, and soy).
- Testing for three common nutrient deficiencies: vitamin D, vitamin B12, and ferritin (the iron storage protein), and addressing them accordingly.
- Adding nutrients that support proper absorption, distribution/digestion, metabolism and elimination (ADME), and thyroid function, such as magnesium, selenium, thiamine, and zinc.
- Removing the obvious things that interfere with proper digestion (like acid-suppressing medications), and adding digestive support, if appropriate.
- Focusing on eating a diet that keeps your blood sugar balanced.
To chop off the branches, I have found that supporting three body systems that are affected in Hashimoto’s with targeted protocols, can make a world of a difference. I call these protocols my “Fundamental Protocols”, and they focus on supporting the liver, addressing adrenal health, and reducing inflammation in the gut.
Picking the low-hanging fruit and chopping the branches produces incredible results for most people. My clients and readers report vanishing symptoms, labs that improve, and most importantly, feeling like themselves again, after doing so.
In some cases, further work needs to happen to find and address the root cause(s) that are contributing to the condition, such as infections, traumatic stress, and toxins. You can dive deeper into these steps and learn how to implement them to heal your own root causes in my book, Hashimoto’s Protocol.
Takeaway
Hashimoto’s is more than just hypothyroidism; it is a complex condition that arises when certain genetic predispositions, as well as leaky gut and one or more root cause factors, trigger an autoimmune cascade.
Once started, the cascade becomes a vicious cycle that is self-sustaining unless an external factor intervenes to break the cycle. The first step to breaking this vicious cycle is identifying and eliminating the triggers that perpetuate this cycle, using a Root Cause approach. Because this process is complex, I wrote my book Hashimoto’s: The Root Cause to help my Root Cause Rebels identify and eliminate their own unique triggers (because everyone is different :-)).
You can also check out my About Hashimoto’s page for an overview of the protocols I recommend for healing Hashimoto’s.
Although the journey to reversing Hashimoto’s can be a long one, it is possible (and rewarding)! I wholeheartedly believe you can heal your Hashimoto’s and thrive as your healthiest self.
P.S. You can also download a free Thyroid Diet Guide, 10 thyroid-friendly recipes, and the Nutrient Depletions and Digestion chapter of my first book for free, by signing up for my weekly newsletter. You will also receive occasional updates about new research, resources, giveaways, and helpful information.
For future updates, make sure to follow me on Facebook, and Instagram, TikTok, and Pinterest!
References
[1] Fasano A. Leaky gut and autoimmune diseases. Clin Rev Allergy Immunol. 2012;42(1):71-78. doi:10.1007/s12016-011-8291-x
[2] Davies TF, Latif R, Yin X. New genetic insights from autoimmune thyroid disease. J Thyroid Res. 2012;2012:623852. doi:10.1155/2012/623852
[3] Zaletel K, Gaberšček S. Hashimoto’s Thyroiditis: From Genes to the Disease. Curr Genomics. 2011;12(8):576-588. doi:10.2174/138920211798120763
[4] Carta MG, Loviselli A, Hardoy MC, et al. The link between thyroid autoimmunity (antithyroid peroxidase autoantibodies) with anxiety and mood disorders in the community: a field of interest for public health in the future. BMC Psychiatry. 2004;4:25. Published 2004 Aug 18. doi:10.1186/1471-244X-4-25
[5] Danailova Y, Velikova T, Nikolaev G, et al. Nutritional Management of Thyroiditis of Hashimoto. Int J Mol Sci. 2022;23(9):5144. Published 2022 May 5. doi:10.3390/ijms23095144
Note: Originally published in February 2015, this article has been revised and updated for accuracy and thoroughness.


 Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Rhonda- Did you know that reactive foods trigger an inflammatory response in the GI tract, leading to malabsorption of nutrients (gluten sensitivity in particular has been implicated in causing a Selenium deficiency, a well known risk factor for Hashimoto’s), and can also produce intestinal permeability whenever they are eaten?
Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
DianesDetox- Did you know that reactive foods trigger an inflammatory response in the GI tract, leading to malabsorption of nutrients (gluten sensitivity in particular has been implicated in causing a Selenium deficiency, a well known risk factor for Hashimoto’s), and can also produce intestinal permeability whenever they are eaten?
Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
Marlo- When it comes to weight gain these are a couple of things to think about.
1) What was your recent TSH, Free T3 and Free T4? Sometimes when those numbers are on the outskirts of normal, your metabolic rate may still be impaired making it more difficult for you to burn calories. Most people report feeling well with a TSH between 0.5-2.
2) What type of medication are you on? Some report more weight loss with T4/T3 combinations (Armour, Nature-Throid, compounded medications) versus T4 medications (Synthroid, Levoxyl, Tirosint) alone. T4 is a precursor to T3, but some individuals do not convert T4 to T3 properly, and the T3 component is the metabolically active one.
3) What type of diet are you eating? Some report more weight loss with T4/T3 combination vs T4 alone. Some do not convert T4 properly.The Standard American Diet (S.A.D.) full of sugar and simple carbohydrates is perfectly designed to cause us to gain weight year after year. Even yogurts that are marketed as “healthy” contain the equivalent of 16 teaspoons of sugar. Divorcing the S.A.D. is often a step that many of us must take to not just lose weight, but to also feel better. Some diets that have been helpful include the Body Ecology Diet, the Paleo Diet, the Virgin Diet, Autoimmune Paleo Diet, GAPS diet, SCD diet, Weston A. Price Diet, or the Mediterranean Diet. You may need to modify these diets to your own individuality.
BEST DIET FOR HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/best-diet-for-hashimotos-hypothyroidism
HOW TO LOSE WEIGHT WITH HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/how-to-lose-weight-with-hashimotos
An Alternative doctor or Naturopath that works with a doctor so they can give perscriptions may help. Thyro-gold on internet is also available. Celiac may cause low thyroid and Type 2 Diabetes and ear infections and low immune system. Gluten makes antibodies to the thyroid. Gluten is wheat/barley/rye…oats may act like gluten. GMO corn/soy/canola oil may also hurt.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg.
Hidden gluten can be in nuts not in the shell/meat basting/lotions/pans/air/cutting boards/certified gluten free food may have 20 ppm of gluten and also GMO in it/make up/medicines/vitamins may have hidden gluten.
The Celiac diet may help thyroid/depression/moods and the rest you list. This diet may help more nutrients to absorb…then cells are made right to work right and are higher in oxygen which may help depression go away fast. Hernias maybe due to low B vitamins which are water soluble and rinse out of the body. 5000mcg of biotin and B complex help me. Vit B12 methylcobalamin may help stress/sleep/depression and much more. Best wishes.
Shasha- Thank you so much for sharing! Here is an article you may find interesting as well! 🙂
IS YOUR MEDICATION GLUTEN FREE?
https://thyroidpharmacist.com/articles/is-your-medication-gluten-free/
Carol- Thank you so much for sharing. I am so sorry to hear that she had to go through all that. I hope she is doing better now, and I look forward to hearing her progress. Here is an article you may find interesting as well! 🙂
GOT ACID REFLUX?
https://thyroidpharmacist.com/articles/got-acid-reflux
Lorraine- Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year/
Karen- Fatigue was the most debilitating symptom I experienced with Hashimoto’s. It actually started 8 years before I was finally diagnosed in 2009, after I got Mono (Epstein-Barr Virus) in college. I needed to sleep for 12 hours each night to be able to function, and by “function” I mean after hitting the snooze button on my alarm clock for two hours (ask my poor husband), I would drag myself out of bed and then had to drink 4-6 cups of caffeine everyday to keep myself awake. I often had Red Bull and Pepsi for breakfast, and was the epitome of “wired but tired”. I hope my articles help you get started 🙂
OVERCOMING THYROID FATIGUE
https://thyroidpharmacist.com/articles/top-10-tips-for-overcoming-hashimotos-fatigue
THIAMINE AND THYROID FATIGUE
https://thyroidpharmacist.com/articles/thiamine-and-thyroid-fatigue
Kristen- Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year/
Lara- Some people with Hashimoto’s test negative for thyroid antibodies because their overall immune health is so weak they do not produce enough antibodies. I’ve tested negative for antibodies several times. Now I’ve insisted on a thyroid ultrasound. Given that Hashimoto’s is one of the leading causes of hypothyroidism worldwide, I wouldn’t stop until I know one way or another.
These are the recommended labs from my book, page 32.
RECOMMENDED THYROID FUNCTION TESTS
TSH
TPO Antibodies
Thyroglobulin Antibodies
Free T4
Free T3
Reverse T3 (Optional)
Have you read my book, Hashimoto’s The Root Cause? Here’s the link in case you’re interested.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20

HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications
Betsy- I am so sorry to hear that. Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year/
Peaches- Did you know that reactive foods trigger an inflammatory response in the GI tract, leading to malabsorption of nutrients (gluten sensitivity in particular has been implicated in causing a Selenium deficiency, a well known risk factor for Hashimoto’s), and can also produce intestinal permeability whenever they are eaten?
Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
ms_mom- Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
DAIRY AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/got-hashimotos-you-may-want-to-reconsider-dairy
GOING DAIRY FREE TO REVERSE HASHIMOTOS
https://thyroidpharmacist.com/articles/going-dairy-free-to-reverse-hashimotos
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
thank you so much for that invaluable info about the anti-body tests you advise.i would love to hear more. am only aware of TPO. WHAT ABOUT IGg and IgA ? those are food sensitivities? not the same bag?
Lara- When I was first diagnosed with Hashimoto’s, I felt so alone. My doctor didn’t think it was a big deal, and none of my friends or co-workers had it. It wasn’t until I started to research online that I found others who were going through the same thing.
A couple of years after my diagnosis, I found Hashimoto’s 411, a closed Facebook group run by Alice Berry McDonnell. This group is amazing! It is comprised of an army of highly motivated, smart, supportive women and men (now 45,000+ strong), and each of them sharing ideas of what worked for them, things they were planning to try, and offering support to one another. The comfort I received from knowing that there were others going through the same challenges as I, was enormous.
https://www.facebook.com/groups/hashimotos411/
Ask questions. Post your thoughts. Scan the files. It is an absolutely amazing resource. Best of all it’s kept private from spammers.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg.
Hidden gluten can be in nuts not in the shell/meat basting/lotions/pans/air/cutting boards/certified gluten free food may have 20 ppm of gluten and also GMO in it/make up/medicines/vitamins may have hidden gluten.
The Celiac diet may help thyroid/depression/moods and the rest you list. This diet may help more nutrients to absorb…then cells are made right to work right and are higher in oxygen which may help depression go away fast. Hernias maybe due to low B vitamins which are water soluble and rinse out of the body. 5000mcg of biotin and B complex help me. Vit B12 methylcobalamin may help stress/sleep/depression and much more. Best wishes.
Paula- These are the recommended labs from my book, page 32.
RECOMMENDED THYROID FUNCTION TESTS
TSH
TPO Antibodies
Thyroglobulin Antibodies
Free T4
Free T3
Reverse T3 (Optional)
Have you read my book, Hashimoto’s The Root Cause? Here’s the link in case you’re interested.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20

HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications
roller coaster doc calls me a rapid cycler so no meds 7plus years … I recently have gone cold turkey gluten free 2 weeks ago due to them saying something is wrong w gallbladder noone believes me that something is upseting the gallbladder and the thyroid … thyroid also have 4 nodules … lots of other symptoms … in AZ and I NEED a doc tht will help thyroid not test after test lije a guineapig
Amy- Did you know that reactive foods trigger an inflammatory response in the GI tract, leading to malabsorption of nutrients (gluten sensitivity in particular has been implicated in causing a Selenium deficiency, a well known risk factor for Hashimoto’s), and can also produce intestinal permeability whenever they are eaten?
Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
Food intolerances can trigger many of these symptoms as well so I think you are on the right path with changing his diet. I would have your doc recheck his antibodies in 3 months of the dietary changes. It takes that long to see an effect.
Unfortunately, not everyone will get better with the same interventions.
I was actually, gluten, dairy, soy free for over a year without an improvement in my Hashi’s antibodies. I had to continue to dig at my root cause…among other things I took on an elimination diet and found out that I was sensitive to eggs and a few other things I was having daily.
I will be posting about additional interventions in the near future. You can sign up for my Facebook or blog to receive updates.
Hope that helps
http://www.thyroidrootcause.org/1/post/2013/06/got-hashimotos-you-may-want-to-reconsider-milk.html
Juliana- You may be interested in checking out the Root Cause Recipe Portal. It is full of autoimmune paleo and paleo recipes. You’re able to organize weekly shopping lists, meal planning, etc. Hope you check it out.
http://rootcauserecipes.com/
Adria- Here is The Thyroid Bundle Cookbook which contains over 100 delicious gluten, dairy and soy-free recipes from me and my favorite thyroid and nutrition experts – available here:
THYROID BUNDLE FREE COOKBOOK
http://thyroidbundle.com/
Also, you may be interested in checking out the Root Cause Recipe Portal. It is full of autoimmune paleo and paleo recipes. You’re able to organize weekly shopping lists, meal planning, etc. Hope you check it out.
ROOT CAUSE RECIPE PORTAL
http://rootcauserecipes.com/
Cynthia- You may find this article helpful! 🙂
ELIMINATION DIET FOR HASHIMOTO’S
https://thyroidpharmacist.com/articles/elimination-diet-for-hashimotos
Carm- Thank you so much for your support. I’m looking forward to hearing your progress on this page. Make sure to take the book slow, take notes, highlight, and establish a baseline when making changes. Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
I was ill for about 20 years after a severe illness aged 9. Finally about 10 years ago, I was diagnosed with Hashimotos, and put on Levothyroxin. Surprise, surprise I felt no better. But the doctors decided I was well.
About 7 years ago, I met Dr Barry Peatfield, and had treatment for adrenal fatigue. This made a dramatic improvement to my health. My body temperature and energy levels are still low, and recently I am experiencing increased memory loss, but basically in comparison to 10 years ago I am a whole new girl.
Anyway, last summer I decided it was stupid to carry on taking T4 given that I couldn’t see it was making the slightest bit of difference. After my next blood test (we get tested regularly here in the UK) I was pulled in by the GP as my TSH was over 100. I decided to go back to the medication simply because he couldn’t/ wouldn’t offer anything else.
Over the last year I have been thinking about this a lot, and it’s great to stumble across a pharmacist who is thinking creatively and constructively. My basic theory is this.
The T4 goes into the system.
The pituitary notices the T4 and reduces TSH production.
These 2 occurrences are entirely unrelated to any usage of the T4 in the cells.
It is therefore possible to input T4 to one body which is very ready and able to use it, and therefore to see improvement, and to put it into another body, which has no ability whatsoever to use it, and therefore if anything to see worsening of symptoms (because the body is no longer producing TSH and therefore not producing any thyroid hormones it is able to produce).
So all the TSH test is doing is testing whether you get an output from an input; a bit like whether urine changes colour when taking B vitamins, rather than giving any indication at all as to whether the input is useful.
The TSH test should therefore be banned as not only useless, but also smoke and mirrors which distort and confuse.
I’d be really interested to hear what you think of this and if you agree that there’s any possibility of me being on to something, whether you have any idea what to do with it!
thanks so much
Kathy Whitaker
You are absolutely right. TSH is a pituitary hormone, and not a true indicator of what is happening at the cell level with the active thyroid hormone. Synthroid contains T4, a pro-hormone, that is not very active in the body. It needs to be converted to T3. This conversion takes place in the gut and liver. Gut function and liver function are often compromised in those in Hashimoto’s. The adrenals come into play as well, when they are compromised, you make reverse T3, which is an inactive version of T3 that takes us space, so that’s why it helped to get your adrenals better. Combination T3/T4 meds, and addressing your adrenals, gut and liver is the way to go. I have 4 chapters relevant to this information in the book; chapter on medications, chapter on the gut, on the liver/detoxification and on the adrenals.
Sherry- Thank you so much for sharing! You may be interested in checking out the Root Cause Recipe Portal. It is full of autoimmune paleo and paleo recipes. You’re able to organize weekly shopping lists, meal planning, etc. Hope you check it out.
http://rootcauserecipes.com/
Thank you!
Kristy- Here is an article you may find interesting! 🙂
ARE YOUR ADRENALS SABOTAGING YOUR HEALTH?
https://thyroidpharmacist.com/articles/are-your-adrenals-sabotaging-your-health
Kathy- Here is an article you may find interesting! 🙂
IS YOUR MEDICATION GLUTEN FREE?
https://thyroidpharmacist.com/articles/is-your-medication-gluten-free/
Becky- Without going into too much detail, the first of the crucial defining moments in my disease development may have started during my undergraduate studies at the University of Illinois. Due to the communal living setting of dormitories (and less than stellar hygiene habits of most college students) I had recurrent strep throat infections and even contracted mononucleosis, a viral infection caused by the Epstein-Barr Virus (EBV), which is implicated in triggering many autoimmune conditions. I received multiple courses of antibiotics as well as flu shots (which may be associated with EBV infections), and started birth control for menstrual cramps.
It is my belief that this combination had a profound impact on my gut flora, and thus my immune system.
Epstein-Barr is a virus that causes mononucleosis (commonly called “Mono”) , a debilitating viral infection that is common among college students, and is also known as the “kissing disease,” because individuals are exposed to the virus through saliva of those who are infected.
Specific immune cells known as CD8+ T cells are needed to fight off the Epstein-Barr virus, however, some individuals may have a low baseline level of these types of immune cells. (CD8+ T cells decrease with age, are lower in women, and in the presence of low vitamin D intake). When these fighter cells are low, the Epstein-Barr virus may take up residence in our organs (such as the thyroid) and essentially hijack the organ to help the virus hide and multiply.
The timing of infection may also matter as well, for example, children in developing countries usually contract the Epstein-Barr Virus when they are under the age of 10. This usually results in an asymptomatic infection—one that does not cause them symptoms. In contrast, in developed countries, where individuals are not usually exposed to the virus until they are in high school or college, the infection is symptomatic in 50% of the older kids affected. This is because by the time we reach college age, CD8+ T cells, the ones that fight EBV, have declined by threefold compared with the number of cells we had in childhood.
Additionally, animal fat and broths, soups and stews support the body’s ability to suppress the viruses. Monolaurin/lauric acid, one of the components of coconut oil, has been found to be active against the Epstein-Barr virus. Replication of many viruses including Epstein-Barr is inhibited by glycyrrhizic acid, an active component of licorice root. Quercetin, Co-Enzyme Q10, N-Acetylcysteine, and glutathione were also reported to be helpful in chronic fatigue syndrome because of their anti-viral properties.
EPSTEIN-BARR VIRUS AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/epstein-barr-virus-and-hashimotos
Myra- Thank you so much for sharing! Here is an article you may find interesting! 🙂
DAVE’S HASHIMOTO’S ROOT CAUSE: MOLD!
https://thyroidpharmacist.com/articles/daves-hashimotos-root-cause-mold
Eating no gluten/dairy/soy/sugar/GMO…taking vitamins/good oil,LDN to help block hidden gluten and detoxing help me. UK is low sunlight…far from equator which makes Celiac. 5000IU of Vit D3/walking in the sunlight and more helps me. 2000mg of fish oil/Mg citrate/Vit C, zinc, Nature’s plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind and more help me. Best wishes.
Beverly- I strongly encourage you to keep looking until you find a skilled practitioner who can help you with Hashimoto’s, they are out there. Here is an article I wrote about my challenges finding Dr. Right.
MY RECENT CHALLENGES AND FINDING DR. RIGHT
https://thyroidpharmacist.com/articles/my-challenges-and-finding-dr-right
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten maybe hidden in nuts not in the shell/meat basting/some spices or lotions/pans/cutting boards/Certified gluten free food may have 20 ppm and any food in a box/bag etc may be contaminated with gluten. A Chinese restaurant cooks special for me…veg/rice/tea/mushrooms. The Woks my have gluten/MSG in them so no meat there. Other restaurants may say they offer gluten free, but it maybe contaminated. I eat mostly veg/rice/tea/low sugar fruit/organic potatoes/raw walnuts (open shells to avoid gluten)/antibiotic organic eggs and more. Gluten can cause low thyroid. Best wishes.
Jeni- I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Sonia- There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Best wishes.
Steph- Thyroid tissue can regenerate, but the rate at which it does is not always predictable. Thus, some are able to stop the autoimmune attack on their thyroid and regain normal thyroid function. Others can reduce the dose of medications, and others will need to stay on the medications indefinitely. I’m currently working on some protocols to help with tissue regeneration.
Reversing Hashimoto’s means different things to different people. For some, it means a reduction in symptoms and for others it means a reduction in your antibodies. I had both. Here a few articles that might be helpful for you 🙂
HASHIMOTO’S SELF CARE, GETTING AND STAYING IN REMISSION
https://thyroidpharmacist.com/articles/hashimotos-self-care
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
Betsy- There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
People need thyroid medicine for life usually.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg.
Hidden gluten maybe in nuts not in shell/meat basting/some spices/boxed food/restaurants even if they say gluten free and certified gluten free food has 20ppm of gluten…..lotion/make up and more may have hidden gluten.
Asian diet…meat/veg/rice etc but made at home with no soy etc is what I do. Best wishes.
Andrea- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
IS HASHIMOTO’S A SURGICAL DISEASE
https://thyroidpharmacist.com/articles/is-hashimotos-a-surgical-disease
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. This diet may prevent cancer and other brain/body health issues. Hidden gluten may happen…nuts not in shell/meat basting/some spices and more. Best wishes.
Arlene- I am so glad to hear that! I look forward to hearing more of your progress on this page! Here is an article you may find interesting as well! 🙂
HASHIMOTO’S SELF CARE, GETTING AND STAYING IN REMISSION
https://thyroidpharmacist.com/articles/hashimotos-self-care
Tracy- Thyroid tissue can regenerate, but the rate at which it does is not always predictable. Thus, some are able to stop the autoimmune attack on their thyroid and regain normal thyroid function. Others can reduce the dose of medications, and others will need to stay on the medications indefinitely. I’m currently working on some protocols to help with tissue regeneration.
Reversing Hashimoto’s means different things to different people. For some, it means a reduction in symptoms and for others it means a reduction in your antibodies. I had both. Here a few articles that might be helpful for you 🙂
HASHIMOTO’S SELF CARE, GETTING AND STAYING IN REMISSION
https://thyroidpharmacist.com/articles/hashimotos-self-care
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
Sue- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
IS HASHIMOTO’S A SURGICAL DISEASE
https://thyroidpharmacist.com/articles/is-hashimotos-a-surgical-disease
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. This diet may prevent cancer and other brain/body health issues. Hidden gluten may happen…nuts not in shell/meat basting/some spices and more. Best wishes.
Garry- Do you have Hashimoto’s or a thyroid condition?
Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year/
Mela- Do you have Hashimoto’s or a thyroid condition?
Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year/
my name is Manesa . I am 20 years old and from india. I have been diagnosed with hype thyroidism since 2007 and taking presently thyronom 50mg daily.
recently I read the web page of hope for Hashimotos and the author prescribed your book which I bought and read.
it is really amazing to read your life journey and how you have overcome the Hashimottos.
during 2011 nov when I checked my anti bodies my tpo antibodies was some 1800 and the endoctronist just asked my to continue with thyronorm.
I have been having problems with my periods and hair loss .
my father is a psoriatic patient for over 30 years but has been able to bring it under control with diet modifications and with no medicine.
after reading your book my father could connect his conditions with my conditions and told me to avoid gluten. milk and sugar.
I should say I have been sincere for about 95% of the time. I also went for acupuncture for a bout a three month- once a week.
when I last tested my TPO anti bodies it was less than 50 and my Tg(Ab) is ls around 20.
my free T3 is 2.72.
I have started taking selenium 200 mcg and vitamin E 400 mcg from 1st aug.
I take my thronorm 50 mcg before break fast and my selenium and vit E after lunch.
your book recommends selenium and vit E to be taken in empty stomach.
kindly tell me if it is ok to take thyroid medications and supplements.
if so how and when to take the thyroid medication and when to take the supplement.
I have ordered zinc. cu also from US and once I get them I will start taking 37 mg of Zn and 3 mg of Cu.
I also want to know if I have to add any more supplements.
my father is in US -Orlando right now and will be there till 6th aug.
is it possible if he can talk to you over phone and if so kindly let me know a time window when he can speak with you.
thanks
regards
Manes
Manes- I do provide a limited number of consultations, however, my consultative schedule is all full at the moment. I have a 12 week online program called Hacking Hashimoto’s that covers all of the strategies that I go through with my one-on-one clients, in a self-paced format, so that participants have access to all of the things I’ve learned about Hashimoto’s without having to schedule costly consults with me or another practitioner. There are a few requirements that you should pay attention to, such as my book is a required read.
HACKING HASHIMOTOS
http://hackinghashimotos.com/
In addition, any person that goes through the program will have the opportunity for a follow up consultation with one of my thyroid pharmacist consulting members.
Lastly, here’s the link to the book in case you have not read it already.
AMAZON
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Yes…father/you/whole family tree may not be able to eat gluten/dairy/soy/sugar/GMO. GMO maybe corn/soy/canola oil and more. Gluten is wheat/barley/rye..oats may act like gluten. Hidden gluten can be in medicine and meat basting/nuts not in the shell/some spices/boxed food/lotion/make up etc.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Best wishes.
Stacey- When it comes to weight gain these are a couple of things to think about.
1) What was your recent TSH, Free T3 and Free T4? Sometimes when those numbers are on the outskirts of normal, your metabolic rate may still be impaired making it more difficult for you to burn calories. Most people report feeling well with a TSH between 0.5-2.
2) What type of medication are you on? Some report more weight loss with T4/T3 combinations (Armour, Nature-Throid, compounded medications) versus T4 medications (Synthroid, Levoxyl, Tirosint) alone. T4 is a precursor to T3, but some individuals do not convert T4 to T3 properly, and the T3 component is the metabolically active one.
3) What type of diet are you eating? Some report more weight loss with T4/T3 combination vs T4 alone. Some do not convert T4 properly.The Standard American Diet (S.A.D.) full of sugar and simple carbohydrates is perfectly designed to cause us to gain weight year after year. Even yogurts that are marketed as “healthy” contain the equivalent of 16 teaspoons of sugar. Divorcing the S.A.D. is often a step that many of us must take to not just lose weight, but to also feel better. Some diets that have been helpful include the Body Ecology Diet, the Paleo Diet, the Virgin Diet, Autoimmune Paleo Diet, GAPS diet, SCD diet, Weston A. Price Diet, or the Mediterranean Diet. You may need to modify these diets to your own individuality.
BEST DIET FOR HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/best-diet-for-hashimotos-hypothyroidism
HOW TO LOSE WEIGHT WITH HASHIMOTO’S AND HYPOTHYROIDISM
https://thyroidpharmacist.com/articles/how-to-lose-weight-with-hashimotos
Carol- There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. This diet may prevent cancer and other brain/body health issues. Hidden gluten may happen…nuts not in shell/meat basting/some spices and more.
Vit C, zinc, fish oil, Mg citrate, dairy free probiotic, HCl and enzymes with meals, Vit B12 methylcobalamin shot/spray/under the tongue kind…no hidden gluten in nuts/meat basting/some spices/boxed food or certified gluten free food which may have 20 ppm of gluten etc may help. Nature’s plus- Source of life multiple may help and more. T4 need to convert to T3 with zinc/Se/enough iron with meals anddiary free probiotic taken far from stomach acid. Best wishes.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is from Alternative doctor usually.
Nuts not in the shell/meat basting/some spices/certified gluten free food may have 20 ppm of food…food in a box or restaurant..lotions etc may have hidden gluten. Best wishes.
Angela- Thank you so much for sharing! I also have a list here of doctors that other patients recommend on this list: Hope you take a look! You can also add names to the list! 🙂
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
Mary Ann- You may also like to check out the doctors that other patients recommend on this list: : )
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
Rita- Here is an article you may find interesting! 🙂
LOW DOSE NALTREXONE
https://thyroidpharmacist.com/articles/low-dose-naltrexone-and-hashimotos
Molly- These are the recommended labs from my book, page 32.
RECOMMENDED THYROID FUNCTION TESTS
TSH
TPO Antibodies
Thyroglobulin Antibodies
Free T4
Free T3
Reverse T3 (Optional)
Have you read my book, Hashimoto’s The Root Cause? Here’s the link in case you’re interested.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20

HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications
Peach- Thank you so much for sharing! Do you have Hashimoto’s or a thyroid condition?
Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year/
Synthroid is T4 only which may not help unless you have Zinc/Se/enough iron/dairy free probiotic to help convert it to T3. Amour thyroid has some T3 already, but still needs the Zn etc to convert the rest. Synthroid has gluten in it..
People need thyroid medicine for life usually.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Best wishes.
Sandy- Here is an article you may find interesting! 🙂
DAVE’S HASHIMOTO’S ROOT CAUSE: MOLD!
https://thyroidpharmacist.com/articles/daves-hashimotos-root-cause-mold
Thyroid Peroxidase Antibodies*333.7 IU/mL 0 – 34
Above are my results from a private blood test, when taken to the doctors he said he would do his own test, when I went for results from his tests he told me they were in range but would not tell me the results, he also told me I no longer needed my b12 injections as I’m now level 159 (last test was 1,500) I had to fight to stay on iron tablets with a ferritin level of 9, your blog is very interesting and I shall purchase your book for further reading
Sandra- Thank you so much for your support. I’m looking forward to hearing your progress on this page. Make sure to take the book slow, take notes, highlight, and establish a baseline when making changes. 🙂
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Celiac people may need thyroid and Vit B12 shots for life..not stop. Best wishes.
Milena- I can’t make any direct medical recommendations to any single person for legal reasons but I would highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Zn/Se/enough iron/dairy free probiotic may help T4 convert to T3. LDN may help block hidden gluten. Best wishes.
Milena- Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year/
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Zeolites may help detox or organic sulfur or 600mg of cilantro late at night with no food in body, but lots of good water. Best wishes.
Would love more info on diet, how often scans of your goiter should be taken, and more natural health maintenance. It’s so confusing when so many products or OTC items say DO NOT TAKE if Thyroid disease. Even certain teas are contraindicated. But no one tells you why or what will happen. Will it render your Synthoid meds inactive? Will it cause a Thyroid crisis? Or can it simply be eaten at a different time.
I know I’ve mentioned quite I bit and don’t know how much you can comment on. But any would be a service not only to me but others inflicted.
There is much education on diagnosis with cholesterol issues & diabetes. Yet with Hashimotos we are just handed a Rx. And time for next lab appt.
Thanks for listening
JoAnn- Fatigue was the most debilitating symptom I experienced with Hashimoto’s. It actually started 8 years before I was finally diagnosed in 2009, after I got Mono (Epstein-Barr Virus) in college. I needed to sleep for 12 hours each night to be able to function, and by “function” I mean after hitting the snooze button on my alarm clock for two hours (ask my poor husband), I would drag myself out of bed and then had to drink 4-6 cups of caffeine everyday to keep myself awake. I often had Red Bull and Pepsi for breakfast, and was the epitome of “wired but tired”. I hope my articles help you get started 🙂
OVERCOMING THYROID FATIGUE
https://thyroidpharmacist.com/articles/top-10-tips-for-overcoming-hashimotos-fatigue
THIAMINE AND THYROID FATIGUE
https://thyroidpharmacist.com/articles/thiamine-and-thyroid-fatigue
o gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help cysts. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Leslie- I look forward to hearing your progress on this page! Here is an article you may find interesting as well! 🙂
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help cysts. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
John
John- Going gluten free is always the first step that I recommend. I’ve found through my page that a good percentage feel better off of gluten. About 20% will actually go into remission by doing so. Some researchers have found that three to six months on a gluten-free diet can eliminate organ-specific antibodies.
10 MOST HELPFUL DIY INTERVENTIONS FOR HASHIMOTO’S
https://thyroidpharmacist.com/articles/10-most-helpful-diy-interventions-for-hashimotosaccording-to-my-clients
TOP 9 TAKEAWAYS FROM 2232 PEOPLE WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/top-9-takeaways-from-2232-people-with-hashimotos/
We have done a lot of research to get him off of pharmaceuticals and onto a natural desiccated thyroid. He has also removed gluten from his diet and is working on removing diary. He has ok days and some really tired days still but no worse than when on Synthroids. A website with a lot of info is Stop The Thyroid Madness.com. Also Dr. Tom O’Bryan is a gluten free genius and has you tube videos and an online website with tons of info and lab tests you can order to see which foods are causing elevated antibodies. Check out his free online videos- so much helpful information!
It is a slow process and takes a lot of trial and error. The best I can say is listen to your body when adding supplements and try to find a good holistic Dr. in your area. If you can find one that does bio-feedback that would be awesome. Some supplements we are trying are selenium, magnesium, and digestive enzymes. Best of luck in your health journey! -Meg
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Viki- Here are a couple of articles you may find interesting! 🙂
GUT, BRAIN, AND AUTOIMMUNE DISORDERS: THE ROLE OF FOOD
https://thyroidpharmacist.com/articles/gut-brain-and-autoimmune-disorders
HASHIMOTO’S AND THE GUT
https://thyroidpharmacist.com/articles/hashimotos-and-the-gut
THE GUT AND AUTOIMMUNE THYROID CONNECTION
https://thyroidpharmacist.com/articles/the-gut-and-autoimmune-thyroid-connection
Kathryn- Thank you so much for sharing! Here is an article you may find interesting as well! 🙂
HASHIMOTO’S SELF CARE, GETTING AND STAYING IN REMISSION
https://thyroidpharmacist.com/articles/hashimotos-self-care
All you mention can be due to Celiac. Tests may not work to diagnose Celiac. I take Osteoprocare instead of dairy. I eat meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more. Organic vegetables etc may help. Gluten can hurt intestines and cause leaky gut and food allergies and weak bones since less nutrients are absorbing in intestines.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Caryn- Thank you so much for your support. I’m looking forward to hearing your progress on this page. Make sure to take the book slow, take notes, highlight, and establish a baseline when making changes. Here is an article you may find interesting as well! 🙂
LOW DOSE NALTREXONE
https://thyroidpharmacist.com/articles/low-dose-naltrexone-and-hashimotos
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Pari- Did you know that if you live in the United States, the UK, Australia, Europe and most developed countries that add iodine to the salt supply and take thyroid medications, there’s a higher probability that you do have Hashimoto’s?
Depending on the source, estimates are that between 90-95% of those with hypothyroidism have Hashimoto’s.
But most doctors will never tell people that they have Hashimoto’s, or that their own immune system is attacking their thyroid. People are told that their “thyroid is sluggish”, and that these things happen with age and “Just take this pill, you’ll be fine.” Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year/
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
January blood test showed I had elevated Anti-TPO antibodies at 41 but these dropped a couple of months later and were tested to be found in negative range. Thyroid function tests recently done now show my TSH is now 5.01 (0.2-4.2) but my FT4 is up at 19.3! (10-22) FT3 looks good too at 5.2 (3.1-6.8-) This is all so confusing and my doctors don’t seem to be giving me a straight answer.
Ellie- I’m sorry to hear that you are struggling with so many symptoms. I’m afraid I can’t comment on your lab results due to liability. I can tell you that while reference ranges of what’s “normal” may vary depending on the lab that produces the test reports, most thyroid patients feel best with a TSH between 0.5-2, and with Free T3 and Free T4 in the top half of the reference range. You may like to check out the doctors that other patients recommend on this list:
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Gluten may hurt all glands …thyroid/pituitary/pancreas etc..
This diet may stop body/brain/thyroid health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Thanks!
Debbie- People with Hashimoto’s may experience BOTH hypothyroid and hyperthyroid symptoms because as the thyroid cells are destroyed, stored hormones are released into the circulation causing a toxic level of thyroid hormone in the body, also known as thyrotoxicosis or Hashitoxicosis. Eventually, the stored thyroid may become depleted and due to thyroid cell damage, the person is no longer able to produce enough hormones. At this time, hypothyroidism develops.
THE MANY FACES OF HASHIMOTO’S
https://thyroidpharmacist.com/articles/the-many-faces-of-hashimotos/
Gluten may hurt all glands …thyroid/pituitary/pancreas etc..
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Pamela- You may like to check out the doctors that other patients recommend on this list: 🙂
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
Gluten may hurt all glands …thyroid/pituitary/pancreas etc..
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
I got the same response: “there’s nothing we can do, it’s an autoimmune disorder that will destroy the thyroid, check the TSH twice a year and when it’s out of the range, come to me and I’ll prescribe artificial hormones. Once a year do an echo and avoid iodine (salt with iodine and nuts).”
I started reading your book and I found a lot of very useful information.
The first part of your timeline caught my attention immediately (Cernobil related). I was born in March 31, 1986 in the west part of Romania, Europe. When I was a month or so, I was given iodine because of the Cernobil disaster.
In 2010-2011 I found out I had Helicobater-Pylori and only after taking a treatment with antibiotics in 2012 (about 3 grames/per day – 10 days), I got rid of it.
I had mercury dental fillings for 10-15 years and I replaced them at the beginning of this year.
All these can be part of the root cause and I’m sure I’ll find out more while I read more on Hashimoto.
When I saw the Cernobil connection, I just wanted to write something and to thank you for what you do and for providing all this information to people. I’m sure I’ll find out more and hopefully I’ll find a functional doctor that can help me with this journey.
Daniela- Thank you so much for your support! I look forward to hearing your progress on this page! I know it’s a lot to ask, but if you haven’t already, would you mind leaving a review on Amazon? 🙂
http://www.amazon.com/Hashimotos-Thyroiditis-Lifestyle-Interventions-Treating/dp/0615825796/ref=cm_cr_pr_product_top?ie=UTF8
Gluten may hurt all glands …thyroid/pituitary/pancreas etc..
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Maresa- Anxiety symptoms are very common in people with thyroid disorders.
HASHIMOTO’S AND ANXIETY
https://thyroidpharmacist.com/articles/hashimotos-and-anxiety/
AUTOIMMUNE THYROID DISEASE AND ANXIETY
https://thyroidpharmacist.com/articles/autoimmune-thyroid-disease-and-anxiety
ARE YOU GOING CRAZY OR IS IT JUST YOUR THYROID
https://thyroidpharmacist.com/articles/are-you-going-crazy-or-is-it-just-your-thyroid
Gluten may hurt all glands …thyroid/pituitary/pancreas etc..
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Mary- Graves and Hashimoto’s are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto’s, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people)-Hashimoto’s results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually people with Graves have hyperthyroidism and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research in journey for overcoming my autoimmune thyroid condition.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Gluten may hurt all glands …thyroid/pituitary/pancreas etc..
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
My thoughts and prayers for all who suffer from Hashimoto’s.
Mickie- Thyroid tissue can regenerate, but the rate at which it does is not always predictable. Thus, some are able to stop the autoimmune attack on their thyroid and regain normal thyroid function. Others can reduce the dose of medications, and others will need to stay on the medications indefinitely. I’m currently working on some protocols to help with tissue regeneration.
Reversing Hashimoto’s means different things to different people. For some, it means a reduction in symptoms and for others it means a reduction in your antibodies. I had both. Here a few articles that might be helpful for you 🙂
IS IT POSSIBLE TO RECOVER THYROID FUNCTION IN HASHIMOTO’S
https://thyroidpharmacist.com/articles/is-it-possible-to-recover-thyroid-function-in-hashimotos
REVERSING AUTOIMMUNITY? AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
HASHIMOTO’S SELF CARE, GETTING AND STAYING IN REMISSION
https://thyroidpharmacist.com/articles/hashimotos-self-care
Gluten may hurt all glands …thyroid/pituitary/pancreas etc..
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
I don’t over eat(mostly):) I do try to watch my
calorie intake/exercise.I take 200 mcg of
Levothroxin every morning,which is doing nothing for me.Could I possibly have has humorous?Idk about anything anymore! Ear infections,tiredness,hair loss,weight gain,
constipation etc.The list just keeps growing!!
What do I need to do besides find Another doctor! Thanks
Nikki- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Gluten may hurt all glands …thyroid/pituitary/pancreas etc..
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Kelly- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Gluten may hurt all glands …thyroid/pituitary/pancreas etc..
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Tessie- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Gluten may hurt all glands …thyroid/pituitary/pancreas etc..
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Chris- Here is an article you may find helpful! 🙂
GOT ACID REFLUX?
https://thyroidpharmacist.com/articles/got-acid-reflux
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Betty- There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Anne- That is great! Thank you so much for your support! I hope you also check out my book! Here’s the link in case you’re interested.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
Virginia – Most conventional physicians use the TSH test to determine if one has a thyroid disorder and to dose thyroid medications.
However, this test can often times be misleading, as levels of circulating hormones may fluctuate at different times, such as in Hashimoto’s, the person affected may fluctuate between highs and lows.
Additionally, when scientists first set the “normal” ranges of TSH for healthy individuals, they inadvertently included elderly patients and others with compromised thyroid function in the calculations leading to an overly lax reference range.
This resulted in people with underactive thyroid hormones being told that their thyroid tests were “normal,” based on this skewed reference range. Most people with Hashimoto’s will experience weight gain, and so of course that’s what gets the most focus, but some people actually experience weight loss, or they can’t keep their weight on.
This is especially problematic when a person has multiple food sensitivities and needs to adhere to an autoimmune diet that restricts foods.
Here are a few tips to keep in mind:
1) Get a calorie counting app like My Fitness Pal on your phone, to help you keep track of your daily calories. Eating real food can be more filling than eating simple carbohydrates and you may not be getting enough calories. Use the app to figure out your target weight and the number of calories per day you need to get there.
2) Supplement after dinner with The Root Cause Building Smoothie: 1 avocado (300 calories), 1 cup coconut milk (150 calories), 1 banana (100 calories), 2 egg yolks (100 calories, if tolerated), 1 scoop of protein of beef/pea protein(60 calories) – You can also add cooked sweet potatoes if you need more carbs.
3) Get tested for gut infections. Gut infections can prevent the digestion and assimilation of foods, leaving you underweight and malnourished. The 401H test or GI Effects test are my go to tests.
4) Get your adrenals tested with an adrenal saliva tests. In some, stressed adrenals may actually lead to poor absorption of foods.
5) Be sure that you are not over medicated.
6) Work on reducing your antibodies with a selenium supplement
7) Stress reduction, when we’re stressed we don’t digest.
8) Add coconut oil in your beverages, this can add extra calories in your day
9) Avoid caffeine, it can make you less hungry and stress out your adrenals.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
This diet may stop body/brain health issues fast.
No gluten/dairy/soy/sugar/GMO….taking vitamins/good oils, LDN, Vit D3, Vit C, zinc, fish oil, Mg citrate, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic at night, Vit B12 methylcobalamin shot/spray/under the tongue kind, MTHF and more may help. LDN is awesome..helps to block hidden gluten. An Alternative doctor may help with LDN 3mg. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO maybe corn/soy/canola oil. I eat Asian style..meat/veg/rice/nuts (open shells to avoid hidden gluten and freeze) and more.
Hidden gluten may be in nuts not in shell/meat basting/some spices…boxed food/certified gluten free food/restaurants/pans/air/lotions/Synthroid etc.
Iodine/iodide with Se may help…but not too much. Zinc/Se/enough iron/dairy free probiotic may help T4 go to T3. Amour thyroid may help more. Best wishes.
michele- Fatigue was the most debilitating symptom I experienced with Hashimoto’s. It actually started 8 years before I was finally diagnosed in 2009, after I got Mono (Epstein-Barr Virus) in college. I needed to sleep for 12 hours each night to be able to function, and by “function” I mean after hitting the snooze button on my alarm clock for two hours (ask my poor husband), I would drag myself out of bed and then had to drink 4-6 cups of caffeine everyday to keep myself awake. I often had Red Bull and Pepsi for breakfast, and was the epitome of “wired but tired”. I hope my articles help you get started 🙂
OVERCOMING THYROID FATIGUE
https://thyroidpharmacist.com/articles/top-10-tips-for-overcoming-hashimotos-fatigue
THIAMINE AND THYROID FATIGUE
https://thyroidpharmacist.com/articles/thiamine-and-thyroid-fatigue
Amour thyroid right dose may help the immune system. Gluten can make antibodies to the thyroid. Hidden gluten in nuts not in shell/meat basting/some spices/lotions/medicine/air/cutting boards/food in a box/certified gluten free food may have 20 ppm of gluten may lower the immune system. LDN may help block hidden gluten. Synthroid may have gluten in it’s filler.
Zinc/Se/enough iron/dairy free probiotic may help T4 in thyroid medicine to change to T3 and give energy to cells and help. Best wishes.
Jeni- You may like to check out the doctors that other patients recommend on this list:
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
Gluten may cause low thyroid in 97% of people as it makes antibodies to it and causes low nutrients absorbed in intestines. Synthroid may have gluten in it’s filler and is T4 only. To convert T4 to T3 that cells can use…zinc/Se/dairy free probiotic/enough iron may help tired feeling. When I took zinc I felt 5X more energy. Gentle iron (Iron bisglycinate) may cause less constipation. Hair tests show good mineral and heavy metal levels. Heavy metals may block thyroid. Detoxing heavy metals with 600mg of cilantro or zeolites or EDTA/DMPS IV chelations m(from Alternative doctor) may help the thyroid work better.
Acid reflux medicine may lower Vit B12 and stop stomach acid so food is not digested and nutrients don’t come out of the food.
Celiac diet may help weight be normal and health issues go away fast. Antidepression medicine may have Fluorine which can block thyroid and lower oxygen in the brain causing more depression/suicidal thoughts. Depression/anxiety/panic/suicidal thoughts/obsessing/no sleep can be due to low oxygen in the brain due to cells not being made right to work reight due to not absorbing nutrients due to gluten hurting the intestines so they don’t absorb. Amour thyroid may help more than Synthroid unless you take the supplements to help convert T4 to T3.
Endocrinologists may not help. They go only by blood tests which don’t say if you are full of heavy metals or low in nutrients to convert T4 to T3 and TSH may not help since you can make antibodies to the pituitary also which makes TSH.
Dr. Mercola in Chicago or another Alternative doctor may help you fast and then you may thrive/feel terrific. See Mercola site articles/blog on thyroid etc. Yes you may have to pay out of pocket…take loan maybe or ask for payment plan perhaps. .
Hashimotos…most people are. They can measure antibodies to the thyroid if you are still eating gluten. LDN helps to block gluten and helps heal the gut lining. It gives energy.
Try Jose Araujo in Racine WI. 1- 414-305-4046. Amour thyroid twice day and LDN 3mg (take at night or morning if you have too much energy) may help. Thyroid medicine…no food for 1 hour before or 2 hours after is best so it can absorb.
Sunlight/exercise…swim/walk/eating nothing in a box/bag label/premade since it may have gluten contamination/eating organic/cooking pure foods by scratch may help. Nuts sold without the shell may have gluten contamination on them and meat basting or some spices.
Chiropractors may also help nutrition and Thyro-gold may help.
Best wishes.
Gretchen- You may also like to check out the doctors that other patients recommend on this list:
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
http://drknews.com/hashimotos-hypothyroidism-immune-basics/
Synthroid may have gluten in it. LDN may help block hidden gluten…from an Alternative doctor usually. Best wishes.
Amanda- Here is an article you may find interesting! 🙂
ELIMINATION DIET FOR HASHIMOTO’S
https://thyroidpharmacist.com/articles/elimination-diet-for-hashimotos
sypmtoms: weight gain, loss of memory, brittle hair/nails, joint pain, exhaustion, insomnia, dry skin,
Am taking 1mg Eltroxin, sometimes reducing to half every few days
Sharon- Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead’, or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
IS HASHIMOTO’S A SURGICAL DISEASE
https://thyroidpharmacist.com/articles/is-hashimotos-a-surgical-disease
No gluten/dairy/soy/sugar/GMO and vitamins/good oils, LDN and detoxing help me. Vit D3 5000IU, zinc 50mg, fish oil 2000mg, 20000mg of evening primrose oil. 2000mg of lecithin, krill oil, coenzyme Q10, rhodiola, Mg citrate 4000mg, Vit C, 5000mcg of biotin, Nature’s Plus- Source of life multiple, HCl and enzymes with meals, dairy free probiotic, Vit B12 methylcobalamin shot/spray/under the tongue kind/intrinsic factor kind, MTHF folate, coenyzme Q10, rhodiola, may help brain/body/depression and more health issues. Gluten is wheat/barley/rye..oats may act like gluten with avenin. GMO corn/soy/canola oil may hurt. Amour thyroid maybe needed since gluten may made antibodies to the thyroid.
Sunlight (helps the immune system and helps to heal the gut lining),exercise, organic food, good water..not tap water, cooking by scratch pure food, no food in a box/bag/premade/label/restaurant which may help avoid hidden gluten. Nuts not sold in the shell/meat basting/some spices may have hidden gluten and lotion/make up etc. One restaurant cooks special for me…rice/veg/tea/extra mushrooms (no meat since the woks may have MSG/gluten in them).
EDTA/DMPS IV chelations from an Alternative doctor, 600mg of cilantro, zeolites, organic sulfur, Now brand- Detox support and more may help detox. Hair tests show good minerals and heavy metals. Heavy metals can block thyroid and other chemical reactions in the body/brain.
LDN may help block hidden gluten, but the Celiac diet is still needed. 100% no gluten may help.
This is the short version. My longer version is on Mercola site profile. Ask a Health food store for the name of an Alternative doctor who may help you with better thyroid and supplements and Celiac diet. Best wishes.
Jill- Vertigo can be a common symptom seen in people with thyroid disease. In one research study, 52% of Hashimoto’s patients showed an alteration of vestibular function, which can affect balance and lead to vertigo and nausea. Getting your thyroid antibodies down will of course help vertigo, but in the meantime, I wanted to share a new advance in medicine.
http://denver.cbslocal.com/2012/04/23/colorado-doctor-finds-way-to-treat-common-vertigo/
pandanotorious- I know how overwhelming it can be. Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year/
Alina- You may like to check out the doctors that other patients recommend on this list:
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Rit- I do provide a limited number of consultations, however, my consultative schedule is all full at the moment. I have a 12 week online program called Hacking Hashimoto’s that covers all of the strategies that I go through with my one-on-one clients, in a self-paced format, so that participants have access to all of the things I’ve learned about Hashimoto’s without having to schedule costly consults with me or another practitioner. There are a few requirements that you should pay attention to, such as my book is a required read.
HACKING HASHIMOTOS
http://hackinghashimotos.com/
In addition, any person that goes through the program will have the opportunity for a follow up consultation with one of my thyroid pharmacist consulting members.
Lastly, here’s the link to the book in case you have not read it already.
AMAZON
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Linda- Here is some information you may find interesting.
Three things MUST be present in order for autoimmunity to occur…
1. Genetic predisposition
2. Environmental triggers
3. Intestinal permeability (leaky gut)
Developing autoimmunity is like a three-legged stool, all of these factors must be present for autoimmunity to occur! When you remove one of these, you can prevent or stop autoimmune disease. While we can’t change genes, if we know the trigger, we can remove it and we can heal the gut.
REVERSING AUTOIMMUNITY AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
IS HASHIMOTO’S HYPOTHYROIDISM GENETIC
https://thyroidpharmacist.com/articles/is-hashimotos-genetic
EHS- There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
Lisa- There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
Anna- These are the recommended labs from my book, page 32.
RECOMMENDED THYROID FUNCTION TESTS
TSH
TPO Antibodies
Thyroglobulin Antibodies
Free T4
Free T3
Reverse T3 (Optional)
Have you read my book, Hashimoto’s The Root Cause? Here’s the link in case you’re interested.
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20

HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications
Kimberly- Most people will see a dramatic reduction in gut symptoms, brain symptoms, skin breakouts and pain by eliminating the foods they are sensitive to. Some will also see a significant reduction in thyroid antibodies! An additional subset of people, will actually be able to get their Hashimoto’s into complete remission just by getting off the foods they react to, normalizing their thyroid antibodies, and some even normalizing their thyroid function! Here are a couple of articles you may find helpful.
FOOD SENSITIVITIES AND HASHIMOTO’S
https://thyroidpharmacist.com/articles/food-sensitivities-and-hashimotos
AUTOIMMUNE PALEO DIET
https://thyroidpharmacist.com/articles/autoimmune-paleo-diet
I have Hashimoto’s, Rheumatoid Arthritis, Antiphospholipid Syndrome, Sjogren’s Syndrome and Autoimmune Neutropenia. How do these other autoimmune diseases impact healing my hashimoto’s?
Sarah- Thank you so much for following this page! Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. Here is an article you may find interesting as well! 🙂
REVERSING AUTOIMMUNITY AND THE PERFECT STORM
https://thyroidpharmacist.com/articles/reversing-autoimmunity-and-the-perfect-storm/
HASHIMOTO’S ROOT CAUSE BOOK
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
I’m Mrs. Molina Chatterjee from Mumbai, India. I’ve been hypothyroid for the last 20 years and according to the doctor my lab results are normal but my symptoms are abnormal. I was put on thyronorm 75mcg. My latest lab results are also normal as below :
ferritin 19.00
Free t3 2.45
Free t4 1.22
TPO <20
T3 0.79
T4 7.00
TSH 2.34
R/T3 Unheard of in India
I would like your opinion on further treatment as my GP is of no help. Even the Endo has told me to live with my miseries as my lab reports seem normal.
Molina- I’m afraid I can’t comment on your lab results due to liability. I can tell you that while reference ranges of what’s “normal” may vary depending on the lab that produces the test reports, most thyroid patients feel best with a TSH between 0.5-2, and with Free T3 and Free T4 in the top half of the reference range. Hashimoto’s is a complicated condition with many layers that need to be unraveled. While conventional medicine only looks at each body system as a separate category, and is only concerned with the thyroid’s ability to produce thyroid hormone, Hashimoto’s is more than just hypothyroidism. I wanted to pass along these articles that I wrote. I hope they help 🙂
WHERE DO I START WITH HASHIMOTO’S
https://thyroidpharmacist.com/articles/where-do-i-start-with-hashimotos/
OVERCOMING HASHIMOTO’S
https://thyroidpharmacist.com/articles/overcoming-hashimotos-in-the-new-year/
I receive your emails and read and love your Root Cause book. From your “What’s Really Going On With Hashimoto’s” article I am trying to access your free gifts–free chapter, Thyroid Guide, and Recipes, but there seems to be no link for them. Help?
Karen- Here is the link below!
Free Chapter on Depletions and Digestion, Thyroid Diet Quick Start Guide and 10 Nutrient Dense Gluten Free recipes:
https://thyroidpharmacist.com/gift
I am not cold but extremely and I mean extremely hot when no one else around me is. My body hurts when barely any pressure is put on it – almost every where but especially near joints. In fact, it hurts when I get a pedicure and they massage my calves. Lost my taste for most foods, most everything upsets my stomach for a while after eating, I am very careful what I eat so that I won’t gain anymore weight. I am 5′ tall and weigh about 163 now. I should be more in the 130 range or less. I was on Synthroid for several years to control the growth of the nodules in my thyroid but a doctor took me off of it later. No problems while I was on it as long as the dosage wasn’t too large. Regardless of belonging to a gym, being at the gym several hours 5 days a week, no weight loss. I am 74 years old. My eyebrows became very thing especially on the outer edges a number of years ago now. I have been fighting the weight gain for probably 10 years now. Doctors just saying your tests, the typical ones, are “in the range”. That’s the end of that. I sleep poorly as well. I have anxiety attacks without my medicine, some depression (it was worse but not as bad now), tire easily, etc.
Judy – thank you for following this page. My heart goes out to you. <3
I highly recommend that you work with a functional medicine clinician. It’s a whole medical specialty dedicated to finding and treating underlying causes and prevention of serious chronic disease rather than disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
WHAT TYPE OF DOCTOR SHOULD YOU SEE IF YOU HAVE HASHIMOTO’S
https://thyroidpharmacist.com/articles/what-type-of-doctor-should-you-see-if-you-have-hashimotos
10 THINGS I WISH MY ENDOCRINOLOGIST WOULD HAVE TOLD ME
https://thyroidpharmacist.com/articles/10-things-i-wish-my-endocrinologist-would-have-told-me
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
Hi There,
I am on synthroid – 50mg. A year ago my hair was shedding excessively (TE) I went on Eltroxin 25mg and it was worse than ever, switched to Synthroid 50mg and the rapid loss has stopped (10 months on) this was in April. It’s now July and my crown and part are getting thinner. In 10 months my hair has now started miniturising – the doc has now suggested androgenic alopecia has kicked in. I have no family history, low testosterone and previously no hair issues. I am 39. While I have read synthroid can cause hair loss those comments don’t go into detail. I just have a feeling thyroid and T4 meds are to blame not my hormones and DHT. Do you have any advice. I am thinking of trialling a natural thyroid replacement but don’t want to trigger more hair loss!! It’s a terrifying cycle.
Thanks so much.
Minnie – thank you so much for following this page.
There are quite a few options for thyroid medications. In my experience, what works for one person may not work for another. If your doctor will not prescribe the medication which you are looking for, ask your local pharmacist for doctors in your area who prescribe the medication you are looking to try. Have you read these articles?
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
HOW THE DOSE OF YOUR THYROID MEDICATION CAN UNCOVER YOUR ROOT CAUSE
https://thyroidpharmacist.com/articles/the-dose-of-your-thyroid-medication-can-uncover-your-root-cause/
HOW TO GET ACCURATE LAB TESTING WHEN TAKING MEDICATIONS
https://thyroidpharmacist.com/articles/how-to-get-accurate-lab-tests-when-taking-thyroid-medications/
This book will help you understand your thyroid lab results and how to optimize your thyroid hormones!!
https://thyroidpharmacist.com/checkout/?product_id=4702
hello Dr.izabella wentz
could you help me please, i have hair loss for 3 years, i took some multi vitamins but my hair fall did not stop. sometimes it decrease and then back! i think also my energy is low in day.
i am so upset for my hair loss, please tell me what should i do? may i have hashimoto?
my doctor said every thing is normal but i does not feel good…my blood test is:
tsh: 1.9
ferretin: 70.8
VIT. D: 38.4
prolactin: 13.4
testostrone: 0.31
estradiol: 230 (i was in luteal)
progestrone: 7.3
iron: 149
zinc: 94
selenium: 115
Sara – thank you for reaching out. I am so sorry to hear you are struggling with hair loss. <3 Hair loss is a distressing symptom experienced by women with Hashimoto’s. For women,
our hair represents our femininity, and losing our hair is a constant reminder that something is off and that we are not well.
Here are some articles which might help:
HASHIMOTO'S AND GETTING YOUR HAIR BACK
https://thyroidpharmacist.com/articles/hashimotos-and-getting-your-hair-back/
HAIR LOSS AND YOUR THYROID
https://thyroidpharmacist.com/articles/hair-loss-and-thyroid
Hi. I have Hashimoto hypothyroidism and so does my sister and so does my mom. My kids ages 16 (girl) and 13 (boy) have TSH and T4 levels that are within range an negative TPOAb tests but their TGAb is very high (over 400 for my daughter and about 200 for my son). What would be good options to try and see if we can get their TGAb levels down? Or to prevent bigger issues in the future? They do take vitamin D supplements and I am thinking about trying selenium and Wobenzym. Anything else? Not so sure about Betaine with Pepsin because I read it upsets the stomach of some people.
Thanks for any suggestions.
Elisa – thank you for sharing. ❤️ For children, teens, (and adults), I always recommend starting with the diet. Are they gluten, dairy, corn and soy free? Are they eating a nutrient dense diet with fermented foods? Implementing those changes can help. Most of the interventions recommended in my book can be done with children, with the exception of the dosing of supplements. I do suggest that you work with a functional medicine doctor that is familiar in working with children (I only work with adults). I hope this helps!
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117