A Hashimoto’s Guide
Over the last several years, I’ve worked with many people with Hashimoto’s, and it’s disheartening to hear about the misinformation they are given at the time that they are diagnosed.
Some people are told that they would always be tired and that they would always struggle with their weight. Nothing could be done—they would just need to accept this as fact! This is, of course, completely untrue, as many people with Hashimoto’s can make a full recovery and live symptom-free (an unconventional root cause approach will be needed to reverse the condition, but some can eliminate virtually all of their symptoms with just the right medications).
Others were told that thyroid disease is easy to treat and that they had nothing to worry about. However, they often found this was the furthest thing from the truth, as they continued to deal with numerous symptoms and bounce from doctor to doctor only to be told that “it’s all in their heads.”
If you’ve been following me for a while, you likely know much of this information… but if you’re struggling with symptoms or have a newly diagnosed friend, please read on. I hope this article gives you some reassurance and/or a starting point for a conversation with a newly diagnosed friend or family member. Please send them this article to shorten their learning curve.
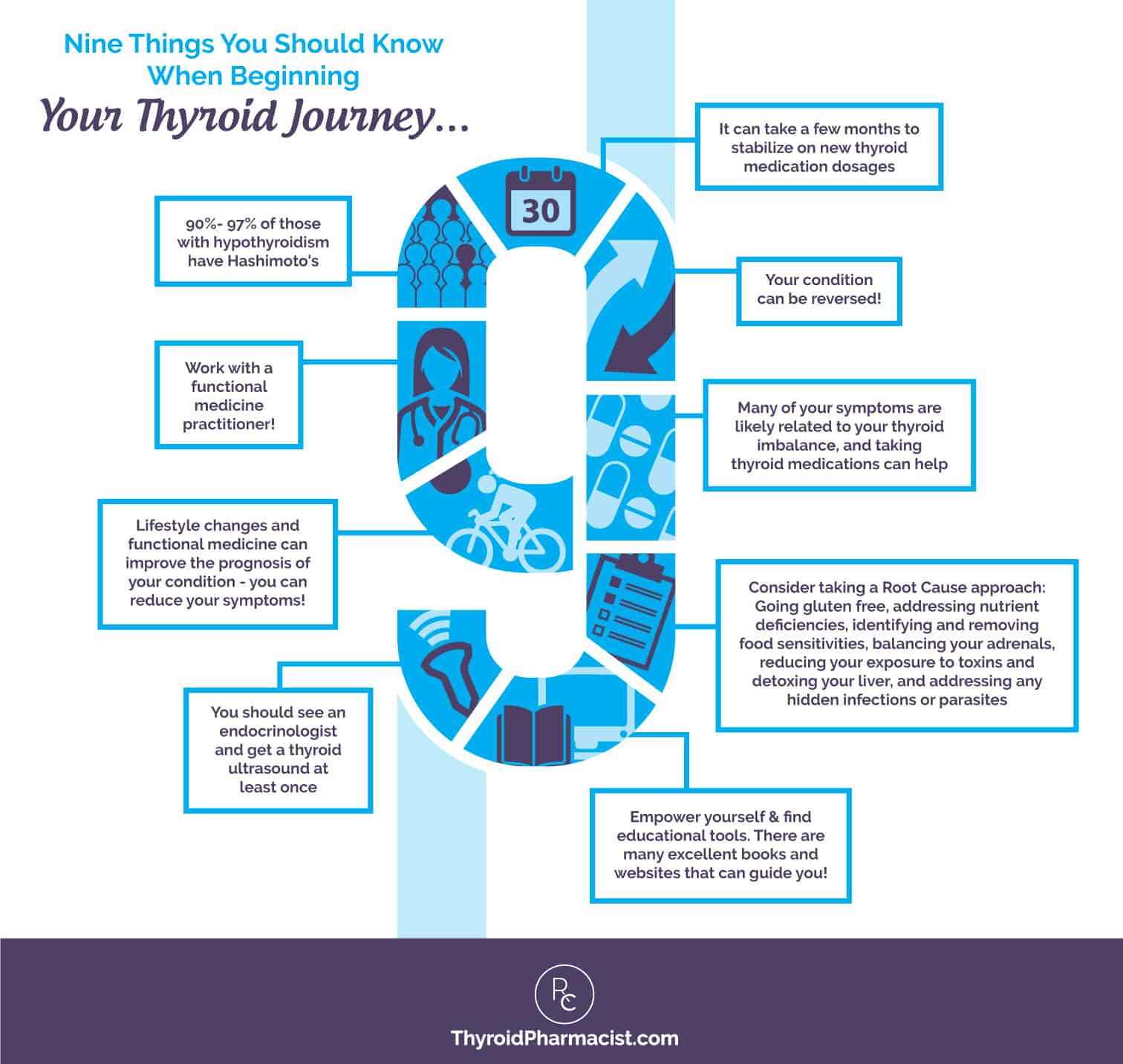
Here are some of the top things I’d say to a newly diagnosed friend with Hashimoto’s:
1. Hashimoto’s is the #1 cause of an underactive thyroid, accounting for 90%- 97% of cases of hypothyroidism.
Hashimoto’s is an autoimmune condition that results in the immune system attacking the thyroid gland. This attack causes damage to the thyroid, eventually resulting in the gland, causing it to lose its ability to make thyroid hormones. Hashimoto’s, and the autoimmune process, likely developed 5-10 years prior to the time you were diagnosed. In the early stages, the TSH screening test for Hashimoto’s often comes up normal. In the later stages of Hashimoto’s, the TSH will become elevated, allowing doctors to make a diagnosis of hypothyroidism. Testing for thyroid antibodies can help a person determine that they have Hashimoto’s and can uncover the condition many years before there is a change in TSH.
Detecting and addressing thyroid antibodies early on, before a change in TSH is seen, can increase the likelihood of improving symptoms and minimizing damage to the thyroid gland. The most common Hashimoto’s antibodies are Thyroid peroxidase (TPO antibodies) and thyroglobulin (TG antibodies). These are standard tests that you can ask your practitioner to order for you. I’ve also set up a portal where you can self-order these labs, if you are unable to get them through a practitioner or have a high deductible.
2. Many of the things you’ve been going through, like fatigue, anxiety, weight gain, menstrual irregularities, and hair loss, are likely related to your thyroid imbalance.
Thyroid hormone receptors are present in virtually every cell in your body. Here’s an article about the most common symptoms experienced with Hashimoto’s. Taking thyroid medications can make a dramatic change in how you feel. The key is to follow what I like to call the five R’s of thyroid medication: The right person, the right, drug, the right dose, the right time and the right way.
Right Person. One of the most common questions I get from readers in the early stages of Hashimoto’s is, “Should I (or when should I) start taking thyroid medications?”
While there is no single right answer to this question for everyone, I encourage you to consider thyroid medications as one of many tools, to give yourself energy and give your thyroid gland a break, so you can focus your resources on healing.
Taking thyroid hormone replacement can be beneficial in all of the following scenarios:
- If your labs are outside of the functional range
- If you have thyroid symptoms
- If you have thyroid antibodies
- If you’ve had your thyroid gland surgically removed
- If your thyroid gland has ever been given a radioactive iodine treatment
Right Drug. Synthroid is the most commonly used medication for hypothyroidism. It was the most commonly prescribed medication in the United States multiple times over the last few years! Synthroid is a synthetic version of one of the main thyroid hormones produced by the thyroid gland. This medication is the treatment of choice for most endocrinologists and conventionally trained MDs. Generic versions include levothyroxine, Levoxyl, and Levothroid.
Synthroid, and other synthetic medications, contain the thyroid hormone T4. The body needs to convert this hormone to T3, a more usable form. In theory, this conversion should happen in the bodies of most people. However, some people do not convert T4 to T3 properly, leading to thyroid symptoms despite taking T4. These people will feel much better (weight, energy, hair) on a medication regimen that contains both T3 and T4. This can be done by adding T3 to the regimen or by taking a T4/T3 combination medication such as the porcine thyroid-derived medications Armour, Nature-Throid, and WP Thyroid. Compounded pharmacists can also make synthetic T4/T3. Here’s a post about thyroid medication options.
Right Dose. Most people who take thyroid medications feel best when they are dosed to a TSH between 0.5-2 mIU/mL. This is close to the “normal” range of TSH for a healthy person without thyroid disease. However, when you get your TSH tested through a medical lab, the medical labs may use outdated reference ranges. Always ask for a copy of your lab tests to make sure you are in a good TSH range for you! Here’s a post about the TSH test and the best TSH range (a printable letter for your doctor is included).
Right Time. For most people, the best time to take thyroid hormone is first thing in the morning 30 minutes before eating, drinking, or taking other medications. Some people may advocate for taking T4 medications at bedtime, however, with T3 medications, this may lead to insomnia.
Right Way. Thyroid hormones interact with a variety of substances including other medications, supplements, food, and even coffee, and thus, are best absorbed when taken on an empty stomach with water, apart from other medications, foods or drinks. Calcium supplements, magnesium, and iron specifically, need to be spaced out by four hours. Of course, I recommend talking to your pharmacist to determine the best way to take thyroid medications for you.
3. It may take a few months to stabilize on thyroid medications.
You are started off at a low dose (too much can be a big shock to a system that’s been deficient), and lab tests are used to determine if the dose needs to increase. After first starting a medication, retest your thyroid function tests within 4-8 weeks. Always request a copy of your lab tests and become familiar with the most important thyroid tests.
4. You should see an endocrinologist at least once.
It is important to get a thyroid ultrasound, which can give you a baseline of the condition of your thyroid and help determine if you have any nodules or tumors in the thyroid gland. However, don’t expect to get the whole story about how to treat your condition. There are many things I wish my endocrinologist would’ve told me, so I’ve put together a top 10 list for you.
5. Hashimoto’s doesn’t have to be a lifelong, progressive condition.
If you’re working with a conventionally trained doctor, he/she likely told you that Hashimoto’s is a lifelong, progressive condition that will require you to take medications for the rest of your life. You might also hear that having Hashimoto’s puts you at a greater risk for additional autoimmune conditions.
This is true if you only take thyroid medications and don’t implement lifestyle changes. However, lifestyle changes and functional medicine can improve the prognosis of your condition. Many of my clients have reported a reduction of their symptoms and their antibodies after implementing changes to their diet and lifestyle. (Some people can even reverse Hashimoto’s completely through these means.)
6. The condition can be reversed.
Conventional medical doctors and endocrinologists will usually only prescribe T4 containing medications and, due to their conventional training in medical school, do not believe the condition can be reversed or improved by any means. But the truth is, the autoimmune process can be stopped and reversed when the root cause is identified and triggers are eliminated. It’s up to you to seek helpful complementary and innovative treatments to help you reach your goal; conventional physicians will not guide you towards them.
With a supportive health care team and thyroid knowledge, some of my readers have been able to stop the autoimmune attack on their thyroid, regain normal thyroid function, and reduce their dose of medications. You could be one of them!
7. Lifestyle interventions and a Root Cause approach can work.
Patients diagnosed with Hashimoto’s, as well as progressive practitioners, have found that lifestyle interventions and a root cause approach (trigger identification and removal) can dramatically improve the way a person feels and may, in some cases, reverse the condition.
Taking selenium as a supplement and reducing stress are two things you can do to start feeling better right away.
Adopting a gluten free diet is another thing you can do right away. Hashimoto’s, like celiac disease, is an autoimmune condition. People with Hashimoto’s are more likely to have celiac disease, which causes the immune system to react to the gluten protein in food. Both autoimmune diseases have been found to respond positively to going gluten free. In fact, 88% of my readers with Hashimoto’s reported that they feel better after eliminating gluten from their diets!
Other lifestyle interventions include addressing nutrient deficiencies, identifying and removing food sensitivities from your diet to help heal your gut, balancing your adrenals, reducing your exposure to toxins and detoxing your liver, and addressing any hidden infections or parasites you may have. Further guidance can be found in my articles Where Do I Start With Hashimoto’s and The Experience from 2232 People with Hashimoto’s.
8. Work with a functional medicine trained practitioner!
If you are hoping to improve the way you feel, slow down the progression of the condition, or reverse the condition, your best bet is to work with a functional medicine trained practitioner, such as an integrative medical doctor/PA/nurse practitioner, chiropractor, naturopathic doctor, functional nutritionist, functional pharmacist, or health coach. You can read more about the growing field of functional medicine that focuses on finding the root cause of immune system imbalances, here.
Practitioners of functional medicine can help you with implementing lifestyle interventions, as well as with finding hidden triggers that may be contributing to the development of your condition. They focus on new research that is not mainstream yet. I know it can be a challenge to find a clinician who understands and practices the root cause approach, so I’ve put together a Recommended Thyroid Practitioners Guide, to help you find these types of professionals with greater ease. (Please note: they were submitted by other thyroid patients).
9. Educate and empower yourself!
Thyroid patients can be misunderstood and mistreated. Some doctors will tell you that all of your symptoms are in your head and that there’s nothing you can do but take antidepressants. Don’t believe them. Listen to your body—you know it best. If you feel that something is wrong, don’t let another person stand in the way of you fixing it. You will need to advocate for yourself. The people with the best outcomes are educated and engaged patients.
There are many excellent books and websites that can guide you! I developed the Thyroid Pharmacist website and blog and wrote my books, Hashimoto’s the Root Cause and Hashimoto’s Protocol, as a way for you to get a deeper understanding of what’s going on in Hashimoto’s, become empowered, and get to the root cause of your condition. I have a few success stories on my website to give you an idea of the improvements you can see by incorporating strategies from my books. I hope they will encourage you to take the first step towards recovering your thyroid health!
P.S. Be sure to sign up to my email list and subscribe to my weekly newsletter to get a free book chapter, recipes, a Thyroid Diet start guide and notifications about upcoming events!
References
- Wang C, Crapo L. The Epidemiology of Thyroid Disease and Implications for Screening. Endocrinology and Metabolism Clinics of North America. 1997;26(1):189-218. doi:10.1016/s0889-8529(05)70240-1.
- Balázs C, Kaczur V. Effect of Selenium on HLA-DR Expression of Thyrocytes. Autoimmune Diseases. 2012;2012:1-5. doi:10.1155/2012/374635.
- Gärtner R, Gasnier B, Dietrich J, Krebs B, Angstwurm M. Selenium Supplementation in Patients with Autoimmune Thyroiditis Decreases Thyroid Peroxidase Antibodies Concentrations. The Journal of Clinical Endocrinology & Metabolism. 2002;87(4):1687-1691. doi:10.1210/jcem.87.4.8421.
- Negro R. Selenium and thyroid autoimmunity. Biologics: Targets & Therapy. 2008:265. doi:10.2147/btt.s2746.
- Xu J, Liu X, Yang X, Guo H, Zhao L, Sun X. Supplemental Selenium Alleviates the Toxic Effects of Excessive Iodine on Thyroid. Biological Trace Element Research. 2010;141(1-3):110-118. doi:10.1007/s12011-010-8728-8.
- Carta M, Loviselli A, Hardoy M et al. The link between thyroid autoimmunity (antithyroid peroxidase autoantibodies) with anxiety and mood disorders in the community: a field of interest for public health in the future. BMC Psychiatry. 2004;4(1). doi:10.1186/1471-244x-4-25.
- Hoang T, Olsen C, Mai V, Clyde P, Shakir M. Desiccated Thyroid Extract Compared With Levothyroxine in the Treatment of Hypothyroidism: A Randomized, Double-Blind, Crossover Study. The Journal of Clinical Endocrinology & Metabolism. 2013;98(5):1982-1990. doi:10.1210/jc.2012-4107.
- Wentz D. Top 9 Takeaways From 2232 People With Hashimoto’s Disease. DR IZABELLA WENTZ, PHARM D. 2017. Available at: https://thyroidpharmacist.com/articles/top-9-takeaways-from-2232-people-with-hashimotos/. Accessed July 20, 2017.
- Sategna-Guidetti C, Volta U, Ciacci C et al. Prevalence of thyroid disorders in untreated adult celiac disease patients and effect of gluten withdrawal: an Italian multicenter study. The American Journal of Gastroenterology. 2001;96(3):751-757. doi:10.1111/j.1572-0241.2001.03617.x.
Note: Originally published in August 2015, this article has been revised and updated for accuracy and thoroughness.




 Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
Disclosure: As an Amazon Associate I earn from qualifying purchases. We are a professional review site that receives compensation from the companies whose products we review. We test each product thoroughly and give high marks to only the very best. We are independently owned and the opinions expressed here are our own.
This is my exact situation, as I am only now have gained weight but before struggles to do so. I have yet to receive the diagnosis but I do show antibodies on my blood tests. I am 19y/o
Abegail – thank you so much for sharing your journey. I understand how hard this is. <3 Most people with Hashimoto’s will experience weight gain, and so, of course, that’s what gets the most focus, but some people actually experience weight loss, or they can’t keep their weight on. This is especially problematic when a person has multiple food sensitivities and needs to adhere to an autoimmune diet that restricts foods. Here are a few tips to keep in mind:
1. Get a calorie counting app like My Fitness Pal on your phone, to help you keep track of your daily calories. Eating real food can be more filling than eating simple carbohydrates and you may not be getting enough calories. Use the app to figure out your target weight and the number of calories per day you need to get there.
2. Supplement after dinner with The Root Cause Building Smoothie: 1 avocado (300 calories), 1 cup coconut milk (150 calories), 1 banana (100 calories), 2 egg yolks (100 calories, if tolerated), 1 scoop of protein of beef/pea protein (60 calories) – You can also add cooked sweet potatoes if you need more carbs.
3. Get tested for gut infections. Gut infections can prevent the digestion and assimilation of foods, leaving you underweight and malnourished. The 401H test or GI Effects test are my go-to tests.
4.
Get your adrenals tested with an adrenal saliva tests. In some, stressed adrenals may actually lead to poor absorption of foods.
5. Be sure that you are not over medicated.
6. Work on reducing your antibodies with a selenium supplement
7. Stress reduction, when we’re stressed we don’t digest.
8. Add coconut oil in your beverages, this can add extra calories in your day
9. Avoid caffeine, it can make you less hungry and stress out your adrenals.
In case you would like to read more, here are the links to my books:
Hashimoto’s Root Cause
http://amzn.to/2DoeC80
Hashimoto’s Protocol
http://amzn.to/2B5J1mq
Hashimoto’s Food Pharmacology
https://www.amazon.com/Hashimotos-Food-Pharmacology-Nutrition-Protocols/dp/0062571591?tag=thyroipharma-20
I’ve had my thyroid removed my Dr said it was as hard as a rock after surgery my calcium bottomed out and had to stay 3 days on calcium drip they never told me to watch my calcium I had thyroid out about 20 years ago my calcium has been low ever since about 7.3 to 7.8 cant seem to get bbn it up have now been using calcitrol and tums do u think I’ll be able to ever get off leverthoroxide
Colleen – thank you for reaching out. I’m so sorry to hear you are struggling with this. Did you know vitamin D affects about 3,000–30,000 genes in our bodies? It’s necessary for helping our body to absorb calcium and strengthen our bones, but it also plays an important role in our immune system health. Many diseases have also been connected to low Vitamin D levels, including heart disease, autoimmune disease, depression, and recently, thyroid conditions and Hashimoto’s. There are also quite a few options for thyroid medications. In my experience, what works for one person may not work for another. I hope you find these article helpful:
Get Some Sunshine for your Thyroid
https://thyroidpharmacist.com/articles/get-some-sunshine-for-your-thyroid/
WHICH THYROID MEDICATION IS BEST?
https://thyroidpharmacist.com/articles/which-thyroid-medication-is-best/
TOP 11 THINGS YOU NEED TO KNOW ABOUT THYROID MEDICATIONS
https://thyroidpharmacist.com/articles/top-11-things-you-need-to-know-about-thyroid-medications/
Dr Izabella,
I am so happy to inform you that just by following your diet and consuming the supplements like selenium, V D 5000 in one month, I could reduce my medication from 75 mgr to 50 mgr. I am very thankful of your effort to help us and would like to encourage every one who is suffering from Hashi’s. Please stay persistent.
Hey Dr Izabella,
ever since I found your book in 2013 my world, life and health have never been the same again. You’re like the Google of Hashimoto, meaning that there is so much noise and info out there, that it becomes really hard to know what and who to follow.
But you had already done the work, you had paved a path through the jungle. Thank you so much for sharing your insights and for this post as well. This post makes the jungle a bit less scary.
Geert
Geert – thank you for your kind words and support! <3
Many of us have had our thyroid killed off with radioactive Iodine. Can you give us more specific information on what applies to people with no thyroid at all and having taken radioactive iodine, does that always completely kill the thyroid or does the thyroid still function in some cases. Is there a test or something that tells us if the thyroid still has some function on its own.
Robert – thank you for reaching out. Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically, is ‘dead,’ or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target. We need to re-balance the immune system to prevent this (sometimes the autoimmunity can be reversed as well). The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition.
Hashimoto’s Root Cause
http://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
Would you recommend taking a “pre”biotic as well as a probiotic? along with all the supplements you list in your Root Cause book.
Kristin – thank you for following this page. For questions pertaining to the supplements please contact my team at info@thyroidpharmacist.com and they will be happy to help you. <3
Hello Dr. Izabella,
Thank you so much for the helpful information! I have been diagnosed with Hypothroid and Rheumatoid Arthritis. Thyroid issues runs in my family and I had to insist on extensive testing as I have been so fatigued I knew something was wrong. My Thryoid Peroxidase AB are at 59, would Hasimoto’s set off RA results? I’ve been given a low dose of synthroid, although I’d prefer armour and a natural substance. I am already feeling better, week 2. I’m going to a GP, I’m thinking of looking for a good endocronologist instead. I’ll be getting your book to help educate myself! Be Well
Elaine – thank you for reaching out. I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
http://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
Dr Izabella,
Thank you for this article!! I have recently been diagnosed with hyperthyroidism and hashimotos. I do not have any symptoms and my endocrinologist is just watching it. My tsh was .03 but everything else shows normal. He did an iodine uptake and he said that was normal too. I have cut out gluten, diary, sugar and caffeine. I do feel like I have more energy. What do I need to so I won’t get symptoms. Thank you again for all your research!
Leslie – thank you for following this page. Graves and Hashimoto’s are both autoimmune conditions that affect the thyroid. They are thought to be closely related. Sometimes one turns into the other. The difference is the site of the antibody attack. In Hashimoto’s, the antibodies are found to thyroglobulin (in 80%) and thyroid peroxidase (TPO) enzyme (in 95% of people)-Hashimoto’s results in hypothyroidism and is usually treated with Synthroid and replacement hormone.
The same antibodies may be present in a smaller percentage of people who have Graves, but the main antibody is to the TSH Receptor (TSHR-Ab). Usually, people with Graves have hyperthyroidism, and they are treated conventionally with thyroid suppressing drugs (methimazole) or radioactive iodine to destroy the thyroid. At that point, the thyroid will no longer produce hormones on its own, and these people end up on Synthroid as well.
Most thyroid conditions result from the immune system attacking the thyroid because the immune system is out of balance. Even when the thyroid is taken out surgically or treated with radioactive iodine the autoimmunity still persists in most cases. Many people will have their thyroids removed, and will develop new autoimmune disorders such as Lupus, Rheumatoid arthritis, etc. The immune system just finds a different target.
We need to rebalance the immune system to prevent this (sometimes the autoimmunity can be reversed as well! The gut determines your immune system. With the exception of discussing proper thyroid medication dosing, the majority of my website and my book focuses on balancing the immune system. The info I present is based on my own research and journey for overcoming my autoimmune thyroid condition. Here are the links to my books:
Hashimoto’s Root Cause
https://www.amazon.com/gp/product/0615825796?ie=UTF8&camp=1789&creativeASIN=0615825796&linkCode=xm2&tag=thyroipharma-20
Hashimoto’s Protocol
thyroidpharmacist.com/protocol
I recently went to the Doctor for what was turning into debilitating panic attacks and horrible stomach/digestive issues . I was afraid that my job was going to be compromised since the attacks were most always work related and seemed to come on together. My Primary Care Dr. ran blood work and found that my ANA was elevated and I was B12 deficient. She ordered more blood work and gave me the diagnosis of Hashimoto’s since I had an elevated TPO. My TPO was barely elevated (a 12 and test said <9 was normal, all other thyroid tests were normal). I ordered the Root Cause and the AIP meal plan and am on week 3 of the AIP diet. Starting to feel better and anxiety is almost non-existent. My question is, am I jumping the gun with the AIP when my numbers are still so low? I just ordered the Hashimoto's Protocol and trying to get my TPO back in the normal range. I am also curious if Hashimoto's is possibly my second autoimmune and I haven't figured out what was making me so sick since my numbers were so low. Just making sure my OCD isn't getting the best of me. Thank you for all the information! It is truly helpful!
Geena – thank you for following this page. For questions pertaining to the protocols please contact my team at info@thyroidpharmacist.com and they will be happy to help you. <3
So glad to have found you. I am 63 and diagnosed with Hypo and Rheumatoid Arthritis almost 15 years ago. Recently they added Hashimoto’s. I’m on biologics (Cimzia), Methotrexate, and Levothyroxine… is there any hope for me? Can I rescue my gut with probiotics while on immunosuppressants? I truly would like to go into my Golden Years with some hope. Thank you.
p.s. I did order your books! 🙂
India – thank you for following this page. I highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms.
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://www.thyroidpharmacistconsulting.com/clinician-database.html
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
I was recently diagnosed with Hashimoto’s Thyroiditis after routine blood tests for a yearly physical. I’ve been on Synthroid for about 4 1/2 weeks. I have had no symptoms that I’m aware of, but I have had small intestine bacteria overgrowth that I’m now thinking may be connected based on what I’ve read about gut issues and the thyroid. I haven’t been tired or cold, I haven’t gained weight, and I’ve felt very healthy. I’m curious why I can have this disease but have no obvious symptoms. My blood test results were normal a year ago. My TSH was high, so my doctor had me get the TPO Ab test, and that was extremely high, resulting in the diagnosis. I’m confused.
Dianne – thank you for following this page. We know that intestinal permeability (aka leaky gut) is present in every case of autoimmunity and often precedes the development of Hashimoto’s. Symptoms of leaky gut may include bloating, diarrhea, constipation, stomach aches, acid reflux and irritable bowel syndrome. According to the Institute of Functional Medicine, many people develop IBS 5-10 years before an autoimmune diagnosis. I was one of them and didn’t take my gut health as seriously as I should have. Gut problems are often caused by infections like H. pylori, parasites like Blasto, SIBO, an imbalance of bacteria, and enzyme deficiencies or food sensitivities (especially to gluten, dairy, and/or soy). Even stress can be a factor in gut permeability. Here is an article you might find interesting.
6 DIFFERENT ROOT CAUSES
https://thyroidpharmacist.com/articles/6-different-hashimotos-root-causes/
You might also find this article helpful as well:
Top 10 Thyroid Tests and how to Interpret them.
https://thyroidpharmacist.com/articles/top-6-thyroid-tests
Hello,
Your information has been extremely helpful trying to navigate all of what is new to my world. I was recently diagnosed with Hypothyroidism in September 2018. This month I was diagnosed with Hashimoto’s and PCOS. I feel like I am having an issue with my current Endocrinologist not listening to my concerns. I am in the process of trying to get a new referral for a 2nd opinion but I was told I may not get one – that’s apparently up to my GP and not me. I have some underlying issues not being addressed by my Endo that I don’t understand why she is not more helpful. I have chronic joint pain. I barely sleep – hard to fall asleep and stay a sleep – 4AM is my nemesis. Fatigue all the time. Major anxiety. Heart palpitations. And gut issues. I recently had to insist a glucose test to rule it out, since I have never been checked and my father is per-diabetic. She made me feel like I was asking too much. She has only tested my cortisol once. I asked if it needed to be checked again – PM instead of AM. She said no. She doesn’t want to check my T3. She doesn’t address my fatigue, joint pain or gut issues. For those she is referring me to a Rheumatologist. I already saw one 2 years ago and they didn’t do anything for me because my ANA is borderline and I don’t have an inflammatory marker. I don’t know what I’m missing here. Should I even see a Rheumatologist? Am I asking too much? I feel belittled and I don’t know if someone else has had issues like this. It’s extremely frustrating after 5 years to finally be diagnosed but still not have all the answers and to still feel sick. Am I right for asking for a 2nd opinion?
Danielle – thank you so much for reaching out and sharing your journey with me. I am so sorry to hear you are struggling with all of this. I understand how frustrating it can all be. <3 I believe that everyone needs to find a practitioner that will let him/her be a part of the healthcare team. You want someone that can guide you, that will also listen to you and your concerns. You want someone that’s open to thinking outside of the box and who understands that you may not fit in with the standard of care. It's a good idea to ask some standard questions when contacting a new doctor for the first time. Something else to consider is you can work with a functional doctor remotely, via Skype. You could also contact your local pharmacist or compounding pharmacy, who may be able to point you to a local doctor who has a natural functional approach. But I encourage you to keep looking for the right one for you! Here are some resources you might find helpful.
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://ifm.org/find-a-practitioner/
http://www.thyroidpharmacistconsulting.com/recommended-compounding-pharmacies.html
I have stomach swelling and have come off two rounds of two different antibiotics, my stomach still hurts and is swollen
Pauline – thank you for reaching out. <3 'm so sorry you are struggling with all of this. We know that intestinal permeability (aka leaky gut) is present in every case of autoimmunity and often precedes the development of Hashimoto’s. Symptoms of leaky gut may include bloating, diarrhea, constipation, stomach aches, acid reflux and irritable bowel syndrome. According to the Institute of Functional Medicine, many people develop IBS 5-10 years before an autoimmune diagnosis. I was one of them and didn’t take my gut health as seriously as I should have. Gut problems are often caused by infections like H. pylori, parasites like Blasto, SIBO, an imbalance of bacteria, and enzyme deficiencies or food sensitivities (especially to gluten, dairy, and/or soy). Even stress can be a factor in gut permeability. The use of multiple antibiotics has been implicated with dysbiosis and exacerbating gut issues. Saccharomyces boulardii (S. boulardii) is a beneficial yeast that helps to clear out dysbiosis such as the pathogenic bacteria, Candida. Here are some articles you might find interesting.
THE FOUR BEST PROBIOTICS FOR HASHIMOTO'S
https://thyroidpharmacist.com/articles/the-four-best-probiotics-for-hashimotos/
6 DIFFERENT ROOT CAUSES
https://thyroidpharmacist.com/articles/6-different-hashimotos-root-causes/
I was sick for over a year and I knew something was wrong but my regular doctor kept telling me I was just getting older or that my kids were older now and they didn’t need me as much that I needed to take some “me time”. My response to these things was I know I am getting older but this is different and that no one had given my kids the memo that they did not need me as much. I struggled for this time until the day that I cried because I did not even have the energy to pick my arm up and hang clothes in the closet. That is the day I went back to the dr crying begging to be sent to an endocrinologist. I instead was sent to a nurse practitioner two hours away. She as the first person to make me think I was just not going crazy. I had gained weight no matter what, my hair was falling out by the handfuls, (my husband asked one day if I was having chemo and had not told him), I had no desire to get out of bed, my joints swell up and I hurt, bowel problems, sleep problems, my periods have been horrible, intolerant to climate changes, and the list goes on and on. I went to see her and she told me that she was ordering a full thyroid panel, hormone testing and a CBC21. I had to wait two weeks before I could see her to get all the results in. When I went back she told me that I was not crazy that I had several things going on. My B12, D, testosterone, progesterone, and iron had all bottomed out. That I have hashimotos, and gluten intolerant. She decided that my levels were not low enough to be put on thyroid meds yet. I was put on weekly B12 injections and bi-weekly testosterone injections. When I went back in six months to redo my labs the injections were not helping. I was also taking supplements of B12, D, and iron. For some reason my body does not want to absorb the vitamins and hormones. I was also put on progesterone that was formulated specifically for me. I felt a little better for a little bit. I am now worse than I was when I went the first time. I had to go back to the dr about a month ago and I was also told that I have fibromyalgia. I have been steadily gaining weight and I feel worse than ever. I literally sat this past weekend and decided that I probably will not live another 10 years with the way I have been feeling. I cannot think straight. I swear between the exhaustion, brain fog, weight gain and swelling and pain that I just want to lay in bed and cry. I have always been a woman on the go. I have six children of my own and yes a couple have hit the age of being grown (21 & 18) but they still need me and then I still have 17, 15, 12, and 10. I just feel like a failure because I cannot function anymore. I just want help!
Tabitha – thank you so much for reaching out and sharing your journey with me. <3 I'm so sorry you are struggling with all of this! I understand how hard this all is! Hang in there. Hashimoto’s is often a combination of food sensitivities, nutrient deficiencies, adrenal issues, gut issues as well as an impaired ability to get rid of toxins. Any of those things would prevent a person from getting better. Hashimoto's is very much an individual condition. While there are root cause commonalities, each person will have their own or in some cases, more than one root cause. You will have to start with the simplest modifications, by removing triggers, followed by repairing the other broken systems to restore equilibrium, allowing the body to rebuild itself. You will need to dig down to why the immune system is imbalanced in the first place and this will tell you how you begin to finally feel better, reduce your thyroid antibodies and even take your condition into remission.
You will have to create your own health timeline. Look back at your overall history as far back as you can remember. Look for infections, periods of severe stress, the use of medications (especially antibiotics, antacids, and oral contraceptives), accidents, and exposure to toxins. These are events that may have contributed to Hashimoto's. Once you do, you will know what types of changes you need to implement to make yourself feel better.
If you need further support, please check out the list of lab tests inside the “Testing” chapter of my book, Hashimoto’s Root Cause. I also offer a 12-week program, Hashimoto's Self Management Program. Here are some resources I hope you find helpful as well.
BUILDING YOUR OWN HEALTH TIMELINE
https://thyroidpharmacist.com/sample-health-timeline/
Hashimoto’s Self-Management Program
https://thyroidpharmacist.com/enroll-in-hashimotos-self-management/
Support is important as well! <3 When I was first diagnosed with Hashimoto’s, I felt so alone. My doctor didn’t think it was a big deal, and none of my friends or co-workers had it. It wasn’t until I started to research online that I found others who were going through the same thing. I found Hashimoto’s 411, a closed Facebook group run by Alice Berry McDonnell. This group is amazing! It is comprised of an army of highly motivated, smart, supportive women and men (now 45,000+ strong), and each of them sharing ideas of what worked for them, things they were planning to try, and offering support to one another. The comfort I received from knowing that there were others going through the same challenges as I, was enormous. Here is a link so you can check it out as well.
https://www.facebook.com/groups/hashimotos411/
Hello Dr. Isabela,
My daughter who is just 8 was diagnosed yesterday, and it was heartbreaking. She is such a healthy and happy and active girl but have GI issues for awhile. So I do see the connection now and wish I was more persistent in looking for way to help heal her guts before. We are going GF now. This is our step #1.
More resouses for managing (hopefully, reversing!) Hashimoto in kids would be very helpful. Thank you!
Yul- thank you so much for sharing your daughters journey! <3 My heart goes out to your both. For children, teens, (and adults), I always recommend starting with the diet. Are they gluten, dairy, corn and soy free? Are they eating a nutrient dense diet with fermented foods? Implementing those changes can help many symptoms. For example, some cases of anemia can be helped by eating liver, others may resolve by going gluten free. Acid reflux is often caused by food sensitivities. Most of the interventions recommended in my book can be done with children, with the exception of the dosing of supplements. I do suggest that you work with a functional medicine doctor that is familiar in working with children (I only works with adults). I hope this helps!
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
CLINICIAN DATABASE
https://thyroidpharmacist.com/database-recommended-clinicians/
FIND A FUNCTIONAL MEDICINE CLINICIAN
https://www.functionalmedicine.org/practitioner_search.aspx?id=117
My name is Debbie Burrell. I am 67 years old. I have several signs of Hashimoto or thyroid problems. I have gut problems every day. I am so tired all the time and all I want to do is lay around all the time. I have no energy at all. Sometimes it is hard to raise my arms. I have had low vitamin D for years and even the prescribed medicine doesn’t help. My stress level is high and I have been diagnosed with depression and I am currently on medicine. I continuly gain weight everyday. I have a lot of stress in my life. My husband is very sick and I try very hard to take care of him. My daughter passed away several years ago and I still struggle with that everyday. I am so tired all the time. My doctor has never said anything about my thyroid. I am sure he has checked it when I have blood work. My mother had thyroid problems and was on medication. I also have COPD and have a very hard time breathing. When I had a breathing test they told me that my shortness of breath was due to me being overweight. What can I do
Debbie – thank you so much for sharing your journey with me. <3 I'm so sorry to hear you are struggling with all of this. My heart goes out to you. Did you know that if you live in the United States, Australia, Europe and most developed countries that add iodine to the salt supply and take thyroid medications, there’s a higher probability that you do have Hashimoto’s? Depending on the source, estimates are that between 90-95% of those with hypothyroidism have Hashimoto’s. But most doctors will never tell people that they have Hashimoto’s, or that their own immune system is attacking their thyroid. People are told that their “thyroid is sluggish,” and that these things happen with age and “Just take this pill, you’ll be fine.” I also highly recommend that you work with a functional medicine clinician to be a part of your own health care team. It’s an entire medical specialty dedicated to finding and treating underlying root causes and prevent serious chronic disease rather than treating individual disease symptoms. I hope you check out these articles that I wrote.
ARE YOU DOING EVERYTHING FOR YOUR THYROID BUT NOT YET WELL?
https://thyroidpharmacist.com/articles/are-you-doing-everything-for-your-thyroid-but-not-yet-well/
DO YOU HAVE HYPOTHYROIDISM OR HASHIMOTO’S OR BOTH?
https://thyroidpharmacist.com/articles/do-you-have-hypothyroidism-or-hashimotos-or-both/
FUNCTIONAL MEDICINE APPROACH TO THE THYROID
https://thyroidpharmacist.com/articles/functional-medicine-approach-to-the-thyroid
Here are the tests you need for diagnosis. Most endocrinologists don’t run them all, so you will have to request them. Make sure to request a copy of your labs as well.
TOP 10 THYROID TESTS FOR DIAGNOSIS
https://thyroidpharmacist.com/articles/top-6-thyroid-tests/